Digitizing the Implant Restorative Process
CAD/CAM offers a major leap forward in the fabrication of implant restorations
Tony Prestipino, CDT
Douglas H. Mahn, DDS
Implant abutments must satisfy important biologic, functional, and esthetic demands.1 The materials they are made from, therefore, are critical to their success.2 Abutment emergence profiles with natural contours permit esthetic3,4 peri-implant soft-tissue remolding.
Traditionally, implant-level impressions have been made using an impression coping. This requires removal of the healing abutment. The impression is made, the impression coping is removed, and the healing abutment is replaced.5 Fabrication of a custom abutment typically has involved using a UCLA abutment.6 Quality custom abutments required skilled laboratory technicians and the use of precious metals.7 Prefabricated abutments reduce costs but do not predictably create natural emergence profiles.8
Advances in impression systems and abutment fabrication have revolutionized implant dentistry. Computer-aided design and computer-aided manufacturing (CAD/CAM) technologies enable a sophisticated fabrication of customized implant abutments.9-13 Coded healing abutments can, furthermore, eliminate the need to remove healing abutments during impression taking. The use of virtual imagery allows technicians to design abutments to meet certain specifications and conform to the surrounding dentition. The computer-designed abutments can then be milled from solid blocks of biocompatible material.
This case report illustrates the steps involved in restoring implants using coded implant abutments and CAD/CAM technologies.
Case Report
A 67-year-old patient was seen for evaluation and treatment of her partial edentulism (sites Nos. 28 through 32). After thorough clinical and radiographic evaluation, a treatment plan was developed that called for placement of three implants to support individual porcelain-fused-to-metal (PFM) crowns in site Nos. 28 through 30.
The patient agreed, and 4/3 mm x 11.5 mm Certain PREVAIL Implants (BIOMET 3i, www.biomet3i.com) were placed by the clinician as planned. BellaTek® Encode® Healing Abutments (BIOMET 3i) were placed on the implants. The dimensions of each abutment were 3.4 mm (prosthetic diameter) x 5 mm (abutment profile) x 3 mm (abutment height). The clinician repositioned and secured the gingival flaps using a continuous 4.0 chromic gut suture.
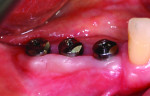
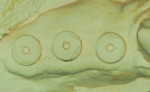
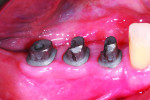
Following three months of healing, all the implants were found to be healing well (Figure 1). At least 1 mm of the abutments were exposed above the gingiva circumferentially. The tightness of the BellaTek Encode Healing Abutments was verified, and radiographs confirmed that the abutments were completely seated (Figure 2). The clinician took full-arch impressions of both arches, using medium-body polyether impression material (Impregum™ F, 3M ESPE, www.3MESPE.com) with a light-body polyether impression material (Permadyne™, 3M ESPE) syringed around the healing abutments. The clinician inspected the impressions for defects in the area of the healing abutments (Figure 3) and used softened wax to make an occlusal registration. These records were sent to the dental laboratory with a completed lab prescription.
The author placed BellaTek Encode Healing Abutments that were the same dimension as those used in the impression on implant analogs. He placed the abutments and analogs in the impression, and injected silicone (Gi-Mask®, COLTENE, www.coltene.com) around them to aid in the fabrication of a soft-tissue model. The author then removed the implant analogs and abutments and poured die stone to complete the master cast, void of any bubbles (Figure 4). The casts were mounted on a Stratos 100™ articulator using Adesso Split Plates (Ivoclar Vivadent, Inc., www.ivoclarvivadent.com). The author filled out a prescription and sent the models without the articulator to the BellaTek® Production Center in Florida.
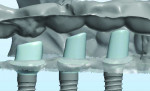
The production center digitally scanned the casts with a D700 3D scanner (3Shape Inc., www.3shape.com). Using the data derived from the BellaTek Encode Healing Abutments and the dental laboratory prescription form, virtual implant abutments were designed using the Abutment Designer™ CAD software (3Shape Inc.). These designs were sent to the dental laboratory (Figure 5 and Figure 7). The author checked and measured the abutments for margin heights. Margin heights are usually 1 mm subgingival on the buccal, ½ mm subgingival on the mesial and distal, and flush with the lingual, axial walls of the abutments parallel to the adjacent teeth. Inter-occlusal space for the definitive restoration and porcelain (usually 2 mm) was also checked and measured. The emergence profile designs were checked to ensure that there would not be any gingival embrasure issues and whether the emergence profiles were concave or convex. Note: Concave emergence profiles are often designed when the implant healing abutment is platform switched due to biologic width concerns.
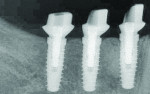
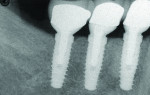
Once the designs were approved, Robocast™ Technology (BIOMET 3i) was used to place implant analogs robotically in the master cast. Custom CAD/CAM abutments were then milled from a titanium alloy blank using a 5-axis industrial milling machine (Figure 8, Figure 9 and Figure 10).
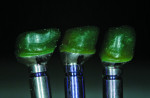
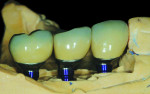
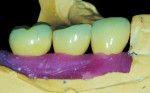
The custom abutments were sent to the author on the Robocast for fabrication of the definitive PFM crowns. The crown wax-up was performed directly on the CAD/CAM abutments (Figure 11). The definitive crowns were placed on the Robocast to confirm proper seating, contours, and contacts (Figure 12 and Figure 13). The abutments and crowns were then sent to the restorative dentist.
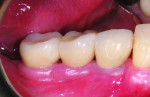
The clinician placed the CAD/CAM abutments on the implants, and prosthetic screws were hand-tightened (Figure 14). Full seating was confirmed radiographically (Figure 15). After proper abutment seating was confirmed, Gold-Tite® Abutment Screws (BIOMET 3i) were torqued to 20 Ncm using a torque driver. The PFM crowns were placed, and radiographs were taken to confirm their full seating (Figure 16). The crowns were cemented in place (RelyX™, 3M ESPE) (Figure 17), and all excess cement was meticulously removed.
Discussion
The use of traditional implant impression copings can be challenging.5 If healing abutment removal and placement of an impression coping is not done quickly, the soft tissue can slump and be pinched. Implant angulation can create situations where impression-coping placement is blocked by the adjacent teeth and/or impression copings. In posterior sites, access to the implant can be difficult. Once the copings are placed, patients cannot fully close their mouths. Finally, placing the impression tray over the coping(s) requires additional clinical skills. This is especially true when an open-tray pick-up impression coping must be positioned within the prepared hole in the tray. Elimination of the need for impression copings by using coded healing abutments that do not need to be removed during the impression process greatly simplifies the impression process and makes it less expensive and confusing.9-13 Only 1 mm of the abutment needs to extend beyond the surrounding gingiva. The ability of a 3-dimensional (3D) scanner to digitize the master cast is integral to this process.
Computer-aided design (CAD) of abutments allows for images of the abutment designs to be reviewed and adjusted prior to definitive abutment fabrication.9-13 Design elements such as the emergence profile and crown margin placement are critical to a properly contoured and natural-appearing restoration. Problems such as inadequate abutment height for a cement-retained crown can be recognized early. Visualizing the virtual abutment prior to its fabrication enabled the author to confirm that the abutment would be made according to the instructions given on the laboratory prescription.
References
1. Heydecke G, Sierraalta M, Razzoog ME. Evolution and use of aluminum oxide single-tooth implant abutments: a short review and presentation of two cases. Int J Prosthodont. 2002;15(5):488-493.
2. Rasperini G, Maglione M, Cocconcelli P, Simion M. In vivo early plaque formation on pure titanium and ceramic abutments: A comparative microbiological and SEM analysis. Clin Oral Implants Res. 1998;9(6):357-364.
3. Rompen E, Raepsaet N, Domken O, et al. Soft tissue stability at the facial aspect of gingivally converging abutments in the esthetic zone. A pilot clinical study. J Prosth Dent. 2007;97(6 suppl):S119-S125.
4. Su H, González-Martin O, Weisgold A, Lee E. Considerations of implant abutment and crown contour: critical contour and subcritical contour. Int J Periodontics Restorative Dent. 2010;30(4):335-343.
5. Wöstmann B, Rehmann P, Balkenhol M. Influence of impression technique and material on the accuracy of multiple implant impressions. Int J Prosthodont. 2008;21(4):299-301.
6. Dario LJ. Implant angulation and position and screw or cement retention: clinical guidelines. Implant Dent. 1996;5(2):101-104.
7. Binon PP. Implants and components: entering the new millennium. Int J Oral Maxillofac Implants. 2000;15(1):76-94.
8. Daftary F. Dentoalveolar morphology: evaluation of natural root form versus cylindrical implant fixtures. Pract Periodontics Aesthet Dent. 1997;9(4):469-477.
9. Priest G. Virtual-designed and computer-milled implant abutments. J Oral Maxillofac Surg. 2005;63(9 suppl 2):22-32.
10. Grossman Y, Pasciuta M, Finger IM. A novel technique using a coded healing abutment for the fabrication of a CAD/CAM titanium abutment for an implant-supported restoration. J Prosthet Dent. 2006;95(3):258-261.
11. Vafiadis DC. Computer-generated abutments using a coded healing abutment: a two-year preliminary report. Pract Proced Aesthet Dent. 2007;19(7):443-448.
12. Kapos T, Ashy LM, Gallucci Go, et al. Computer-aided design and computer-assisted manufacturing in prosthetic implant dentistry. Int J Oral Maxillofac Implants. 2009;24(suppl):110-117.
13. Drago C, O’Connor CG, Peterson T. Robotic analog placement and CAD/CAM abutments. J Dent Tech. 2009;26(7):22-28.
About the Authors
Tony Prestipino, CDT
President
Artifex Dental Laboratories, Inc.
Alexandria, VA
Douglas H. Mahn, DDS
Private Practice
Manassas, VA