A New Height for Esthetic Creativity in Smile Makeovers
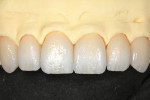
Creating natural-looking high- and low-value zones in specific anterior lithium disilicate tooth restorations
When creating a natural-appearing smile makeover, the author typically uses three different ingots. For this he needs the doctor and patient to allow him to use some “creative license” in designing the maxillary central incisors to be predominant both in value and in position. Likewise, the upper laterals should match the lower laterals’ lesser value, and the upper cuspids also should match the lower cuspids’ high chromatic warmth.
A lesson in value mandates that value not be considered as a gray scale. For oil painters painting on canvas, a gray-scale concept would be appropriate. However, because dental technicians are recreating natural teeth, what they are creating must take on light internally in order to appear like natural dentition. In other words, it must assume the optical qualities of a natural tooth. It is only by understanding this that it is possible to better and more accurately design restorations that demonstrate vitality.1
The area of a tooth that is high value should be considered an area of light reflection. In fact, the light is reflecting so much in some cases that it appears to have its own light source. Therefore, the areas of a tooth that are low value should be considered areas of light absorption. Here, in some cases, the light is absorbed so much that no light is reflected back, as if it is being absorbed like a sponge.1
When a clinician removes 0.6 mm or 0.5 mm of the facial tooth surface of an anterior tooth, he or she has removed mostly enamel.2-4 Why, then, would technicians select an ingot that is more opaque and then cut it back to a thin coping (ie, 0.3 mm) and begin layering it? The answer is that since enamel/dentin tooth structure has been reduced, it makes sense to choose an enamel/dentin ingot (IPS e.max® Impulse ingots, Ivoclar Vivadent, www.ivoclarvivadent.com).
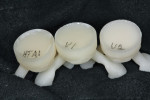
In the case demonstrated here, after the shade comparison photographs were evaluated, the author determined that the patient was basically a B1 shade (ie, IPS e.max Impulse V1), which is a medium translucency B1. This is the shade the author would use for the laterals and posteriors. However, he will typically use one shade lighter or higher in value for the centrals (IPS e.max Impulse V2, 040 medium value). In this case, he selected one shade more chromatic for the cuspids (HTA1).
However, ingot selection is only part of the equation. To understand how to mimic a natural anterior tooth, it also is important to first imagine what a central incisor would look like after 0.5 mm of facial enamel is removed. Ceramists must have an idea of this in order to reproduce or mimic the vitality of a natural tooth.5,6
This is due to the fact that once a full-contoured IPS e.max tooth (ie, core) is created, the 0.5 mm of space that enamel would take up must be removed. Next, the internal effects that mimic a natural tooth must be placed. Lastly, enamel must then be layered back over these internal effects.5,6 In this case, the enamels would be layered again to mimic a natural tooth using Opal Incisal powders.
Case Presentation
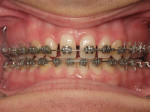
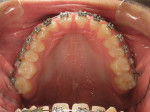
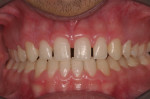
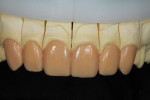
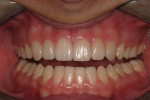
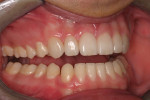
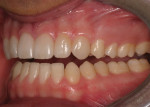
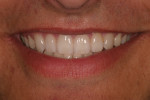
A 17-year-old patient (Figure 1) recently completed orthodontic treatment (Figure 2 and Figure 3) to create room for fuller, more adult-sized teeth in the esthetic zone (Figure 4).
Impressions were taken during the consultation, and a preoperative model was created and mounted with a Kois facebow on a Stratos 200 articulator (Ivoclar Vivadent, www.ivoclarvivadent.com) (Figure 5). When clinicians use an earless facebow record (Kois) combined with an articulator-mounting table, concern about the records being distorted during shipping is eliminated.
After the maxillary preoperative model was mounted, the lower model was mounted using centric occlusion bites. A diagnostic wax-up was then developed and subsequently used to create a Sil-Tech® matrix (Ivoclar Vivadent) for use in fabricating provisional restorations. An eyebrow-to-chin photograph of the patient’s natural smile with the provisionals in place was taken (Figure 6). Based on an analysis of this photograph, the cast of the provisionals was modified for fabricating the definitive restorations.
A new Sil-Tech matrix was made based on the modified provisional cast and formed under 60-psi pressure using a Wiropress SL pressure chamber (BEGO USA, www.begousa.com). This will enable creation of incisal edges and occlusion in exactly the same position as the working, approved provisionals. It also facilitates fabrication of predictable final restorations.
A 1.5-mm hole was drilled from the insides of the matrix in the incisal edge area. Using a jeweler’s wax-injector, Yeti beige wax (Yeti Dental, en.yeti-dental.com) was injected into the matrix and onto the untrimmed, lubricated master dies (Figure 8). The injected wax was left to cool for 5 minutes before the matrix was carefully removed. Excess flash was minimized and removed using a small Hollenbeck wax carver (Pearson Dental, www.pearsondental.com).
The master dies were lubricated but not trimmed for two reasons. First, the injected wax restorations demonstrated an accurate fit to papilla and surrounding gingiva. Secondly, by leaving all the papilla and gingival landmarks the author saves time not second guessing himself in getting the final shape and contour.
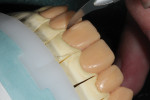
After the wax-up was finalized, the waxed restorations were separated using an ultra-thin knife (Smile Line, www.smilelineusa.com), which facilitated their removal (Figure 9). The master dies’ margins where accurately trimmed under magnification, sealed, re-lubricated, and ready for spruing and investing.
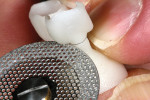
The restorations were pressed from HTA1 ingots for the cuspids, V1 ingots for the laterals, and V2 ingots for the centrals, creating a natural scenario (Figure 10). After pressing and divesting, the sprues were cut and then removed using a Cardinal 932-250-1 rotary instrument ( www.cardinalrotary.com) (Figure 11).
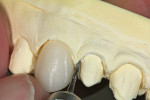
The restorations were carefully fitted to the master dies, after which they were then fitted to a hard-tissue model using a modified high-speed FG-57 burr (Benco Dental, www.benco.com) (Figure 12). It was particularly important to only remove the stone where necessary in order to fully seat the individual restorations. This provided the ceramist with the gingival architectural landmarks while cutting back and layering the restorations (Figure 13).
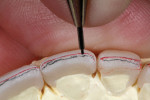
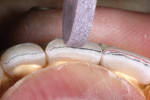
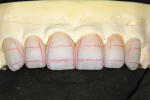
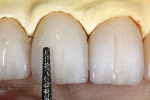
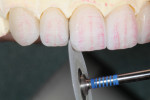
After marking the incisal facial edge with a red pencil, a 0.3-mm Eversharp lead pencil was used to mark the vertical reduction at 0.3 mm below the incisal edge. A Cardinal DB-15M rotary stone was used to carefully remove 0.3 mm of vertical structure from the incisal edge (Figure 14). After using a 0.3-mm Eversharp lead pencil to mark 0.5 mm lingually from the facial red mark, a red pencil was used again to re-mark the newly reduced facial incisal edge (Figure 15). Then, using a Cardinal DB-15M rotary stone, the 0.5 mm of facial core was carefully removed (Figure 16).
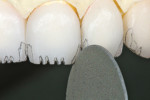
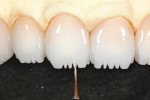
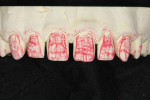
A 0.3-mm Eversharp lead pencil was used to mark the mesial/facial and distal/facial low-value areas found in a natural tooth. Then, the internal lobe details were marked. Cuts then were made using a sharp Cardinal 940 220 (ie, double-sided diamond disk). This was carefully removed to make a trough in the outermost mesial/facial and distal/facial aspects. This troughed out area would be stained to absorb light (ie, low value) and mimic a natural tooth (Figure 17). Vanilla Universal stain was modified with Universal Red to accent a little incisal lobe detail (Figure 18).
Much of the beauty found in natural teeth comes from their ability to act as an optic fiber. As they take on light, it travels apically to illuminate the gingiva from within. Therefore, dental technicians typically see a transference of a pinkish color into the warmer colored cervical of natural teeth, which imparts an orange/pink hue to the neck of a natural tooth.
Therefore, a mixture of Universal Red and Universal 110-120 stain was carefully added to the cervical of the restorations. The troughed areas that need to absorb light (ie, low value) were carefully stained with a mixture of IPS e.max Incisal 2 (violet) and Universal Grey (Ivoclar Vivadent). Care was taken to ensure the grey stain remained inside the trough so it would not negate the interproximal halo effect (Figure 19). A4 Universal stain then was used to imitate the natural color found in the lingual fossa.
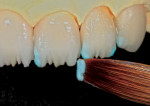
After the internal stain effects were fired, internal powders were selected and mixed on a stay-wet porcelain tray. BL2 dentin was mixed 50/50 with each individual mamelon powder (ie, salmon, yellow-orange, and light) to make three different, smooth, level segments of porcelain (Figure 20). Using a moist culinary sponge, a Tanaka Big Brush ( www.tanaka.de) was formed into a flat blade, with the tip trimmed straight to pick up the mamelon porcelain.
The specially formed big brush tip easily picked up the perfect mamelon piece in its form. The mesial and distal internal lobes were formed from the light mamelon/BL3 dentin 50/50 mixture for all four incisors. This formed mesial mamelon piece was then carefully placed onto the internal surface of the central core (Figure 21).
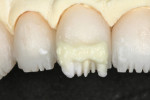
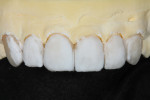
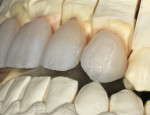
After the internal lobes were added using the mamelon mixtures, a BL3 high-value “bow tie” or band was placed (Figure 22). This was feathered over the mamelons (Figure 23 and Figure 24). Using the formed big brush, an exact piece of OE1 (Opal Clear) was placed in the outermost interproximal incisal trough (Figure 25). TI1 (high-value enamel) was placed in between the lobe details, taking care not to trap air.
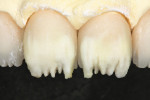
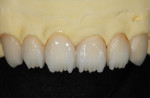
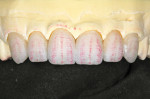
The fired internal effects were evaluated and compared to how a natural tooth would look with its enamel removed (Figure 26). In this case, it was determined that some additional halo effects would be added using the light MM/BL3 mixture. The internal effects of the six anterior restorations were evaluated, after which it was determined that enameling could proceed.
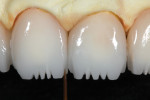
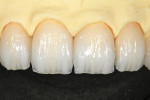
TI1 (high-value enamel) was placed over the effects to full contour (Figure 27), fired, and then evaluated (Figure 28). A Cardinal ZLD8842R-018-1 diamond was used to adjust the enameled surface to the correct thickness (Figure 29).
Using the side of a lead red pencil, the heights of contour were found and marked. These deflective and reflective zones were corrected where necessary to mimic the patient’s preoperative dentition. The preoperative model was used to evaluate and duplicate the patient’s natural tooth surface, including deflective surfaces (Figure 30). The surface lobes of the patient’s preoperative model were carefully copied onto the restorations (Figure 31).
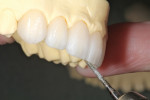
The surface lobes were added using OE1 (Opal Clear) powder. Then, the thicknesses of the powder surface lobes were evaluated by looking from the incisal view. After evaluating the fired surface lobes, it was determined that their thickness required reduction. Using a Cardinal T5856.104.023 (ie, spiral-cut diamond), perikymata was cut into the restorations to mimic the patient’s preoperative tooth surface (Figure 32).
A piece of articulating film was used to mark the surface texture to evaluate the perikymata (Figure 33). The gingival and incisal interproximals were refined using a flexible double-sided diamond disc (ie, Cardinal 918B 220) (Figure 34). The lingual incisal edge bevel was cut using a Cardinal ZLD 850 diamond to duplicate the same edge found on the preoperative model (Figure 35).
Using the Stratos articulator, the left and right cuspid rise were checked and adjusted (Figure 36 and Figure 37). Additionally, using the articulator, the protrusive function of the restorations also could be evaluated (Figure 38). They were then adjusted and smoothed to ensure no anterior interferences.
To glaze the IPS e.max restorations, one-third of a tube of IPS e.max non-fluorescent glaze paste was placed into a small empty mixing jar with one-to-two drops of glaze liquid. This precise measurement of glaze and liquid was thoroughly mixed with a non-metallic spatula to a stringy consistency before applying. With the restorations on the solid model, this glaze mixture was first applied liberally to each restoration (Figure 39). Excess glaze in and around the interproximal areas was removed. Due to the perikymata, it was necessary to clean all excess glaze from these horizontal details. This was accomplished using the glaze brush with horizontal strokes, making sure there was no excess glaze while still seeing the surface gloss back over with each passing horizontal stroke.
The restorations were then fired. The glassy look of the artificial glaze was removed using a white knife-edge rubber wheel (ie, Cardinal G322), paying close attention to maintaining the desired amount of perikymata (Figure 40). It is important to note that the natural surface of a tooth is neither all high-shine nor dull. The lip naturally polishes the top surface of the lobes, while in between these high surfaces, the tooth is usually less polished or dull. To imitate this effect, a large polishing wheel (ie, Cardinal 6625-250-1) was used to highly shine the highest surfaces (Figure 41 and Figure 42).
Conclusion
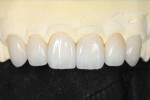
Today’s ceramic materials, such as the IPS e.max lithium disilicate Impulse ingots, enable dental ceramists to take their esthetic creativity to new heights to create truly natural- and vital-looking restorations for the anterior region. Dental professionals can now treat more patients in more satisfactory ways, matching shades not only to adjacent natural teeth, but also as they would progress naturally from anterior to posterior, and from upper to lower. In the case described here, multiple postoperative views confirm the natural esthetics, form, and texture achieved using the selected IPS e.max Impulse ingots and the cutback and layering technique demonstrated (Figure 43 through Figure 51).
Acknowledgements
The author would like to acknowledge Dr. John Workman, Glen Ellyn, Illinois, for his excellence in dentistry. He would also like to thank a few of his mentors—Matt Roberts, Don Cornell, Tom Trinkner, David Hornbrook, and Wayne Payne.
References
1. Sieber C. Voyage: Visions in Color and Form. Chicago, IL: Quintessence Pub.;1994.
2. Rufenacht CR. Fundamentals of Esthetics. Hanover Park: Quintessence; 1990:329-332.
3. Terry DA. Aesthetic & Restorative Dentistry Material Selection & Technique. Houston, TX: Everest Publishing Media; 2009:152-153.
4. Chiche GJ. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, IL: Quintessence; 1994:42-48.
5. Ubassy G. Analysis of anatomic occlusal surface condition. Dent Labor (Munch). 1990;38(4):493-500.
6. Ubassy G. Fabrication and natural stratification of dental ceramics 1. Rev Fr Prothes Dent. 1990;(14):61-70.
About the author
Brad Jones, FAACD
Owner
Smiles, Inc.
Boise, Idaho