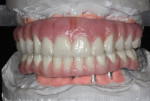
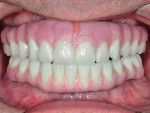
Saving Money and Time with Composites
The next generation of hybrid implant prosthetics.
Over the past decade, dental technologists have seen a rise in the number of prescriptions for implant hybrid prosthetics. It is an area of dental technology that is in constant evolution. The materials currently used in construction of hybrid implant prosthetics are not designed for that specific use. Because of the various issues involved with the use of these dental materials and the general lack of knowledge about these materials, technologists will most certainly encounter problems during the fabrication process. The primary goal in fabricating any prosthetic device should be to provide the patient and the clinician with a highly esthetic, durable prosthesis with longevity in mind. In the vast majority of cases, the clinician’s primary focus is the esthetics, while the experienced technician’s primary concern is merging function with esthetics.
The only viable solution for technologists has been to set the denture teeth in mutually protected articulation to avoid anterior interferences. However, over the long term, the lack of proprioception in combination with excessive wear on the posterior teeth has eventually caused problems.
Today, technologists have new materials that allow the use of various occlusal concepts that eliminate concern about excessive forces being applied to specific areas of the restoration. Conventional denture teeth do not come close to exhibiting the Knoop hardness of natural enamel or porcelain and are not designed to withstand excessive forces in the mouth.1,2 Porcelain is a common material of choice, but repairs can be costly and time-consuming, which is a burden to the patient and the clinician.
Flowable and Paste Composites
Flowable and paste composites are a solution for removable implant technicians, and they possess acrylic-like properties in terms of viscosity and can be injected and pressed using techniques very similar to denture processing. If technicians are willing to extend their technical knowledge and explore various areas of ceramic material science and handling, they will be able to fabricate and provide an alternative solution for patient-specific cases for highly esthetic and functional restorations, but with more speed and efficiency. With the appropriate knowledge of implant bar design, flowable and paste composite usage, and the technical intricacies of injecting and pressing these materials in clear flasks invested with clear silicone, a renewable solution for hybrid implant restorations is available.
The primary concern with any patient fitted with a hybrid implant restoration is the lack of proprioception, which can be a life-long problem. Therefore, the use of materials exhibiting a high MPa hardness is a concern due to the possibility of shearing and fracturing under stress and pressure. Obviously, a lower stiffness value is an advantage. The most important properties to look for in flowable composites are the modulus of elasticity and the bending strength. The composite used to fabricate the restoration presented in this article was a flowable composite with a modulus of elasticity of 6.530 MPa, a bending strength of 140 MPa, and a hardness of 365 MPa. If a conventional acrylic hybrid needs maintenance or repair, it normally discomforts the patient for a day or two. Repairs on a porcelain hybrid can be very time-consuming and costly. In the vast majority of cases, composite restorations can be repaired in the mouth within a very short period of time, saving both the clinician and technologist time and money. If deemed necessary, the technician can incorporate different techniques and materials, such as anaxblend Enamel Paste (anaxdent, www.anaxdent.com), which has a hardness 574 MPa, modulus of elasticity of 10.040 MPa, and a bending strength of 143 MPa, and anaxblend Dentin Paste (anaxdent), which has a hardness 405 MPa, a modulus of elasticity 6.890 MPa, and a bending strength 94 MPa). It is very important to evaluate what the best treatment option is for the patient on a case-by-case basis.
The Case
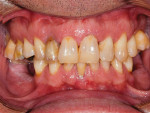
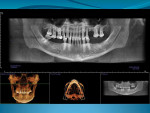
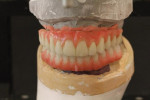
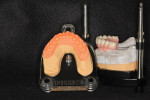
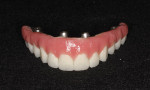
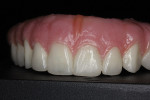
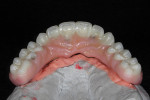
A 46-year-old man presented with oral facial pain associated with chronic advanced generalized periodontitis and dental caries and was referred by his general practitioner to a periodontal specialist (Figure 1 and Figure 2). Objective and subjective clinical data were obtained via a pre-treatment interview and clinical examinations. Panoramic and cone-beam computed tomography (CBCT) examinations were supplemented by extraoral and intraoral photographs for consultation and treatment planning. Based on a review of the clinical data and on informed consents, the prognosis for the existing dentition long-term was deemed very doubtful. Several prosthetic treatment options were discussed with the patient, including: a complete removable denture; a single-arch or complete-arch implant over dentures; or complete-arch, screw-retained, fixed implant prosthetic. After further deliberations with the clinical team, the patient elected the full-mouth rehabilitation with traditional fixed implant technology.
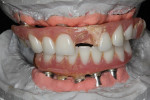
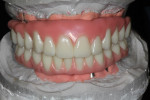
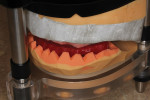
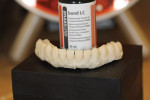
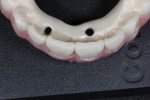
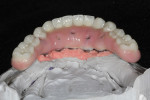
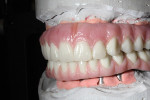
Due to the patient’s frustration with the constant breakage of the current conversion denture (Figure 3), a bite registration was taken and a new wax setup was completed on site to the patient’s specifications (Figure 4). The decision was made by the clinician to manufacture a new reinforced implant provisional out of an injected tooth-colored PMMA New Outline and MatrixForm System (anaxdent), which would be reinforced using E-Fibre (Preat Corporation, www.preat.com). This would allow the clinician to make any necessary occlusal adjustments and any esthetic changes before proceeding to the second stage of the rehabilitation. The advantage of fabricating a temporary implant prosthesis using this method is that it is made out of a homogenous structure, which decreases the chance of the denture teeth debonding and also reduces the chance of fractures.
The denture setup was duplicated using the Big Flask (anaxdent) duplication method. By means of accurate silicones (Figure 6 and Figure 7), the same mold was used to also create a pattern resin duplicate (GC Pattern Resin™ LS, GC America, www.gcamerica.com) of both arches. The resin duplicate was cut back to create the frameworks that were digitized using the NobelProcera™ Scanner (Nobel Biocare, www.nobelbiocare.com) and copy-milled. These molds can always be saved until the case is complete or for future purposes. The reason the author prefers this method is because it constantly provides the technologist with a reduction of processing time to build the pattern resin.
Framework Design
The pattern resin duplication was mounted on the anaxform Verticulator (anaxdent), which is an indispensable tool when fabricating a gingival mask, recording occlusal clearances, and reproducing the occlusal surfaces for the design of the copy-mill pattern framework. In order to gain optimal bonding strength to prevent the composite from fracturing, the pattern must be reduced by only 2 mm. Any reduction exceeding that limit may cause weak areas and the composite to delaminate or fracture. Reducing the occlusal, labial, and lingual surfaces by 2 mm readied the framework for scanning, copy milling, and milling out of titanium (Figure 8 and Figure 9). Use of the Verticulator can eliminate the step of injecting the pattern material by building it up directly on the jig—it is a matter of preference. The author felt that reducing the pattern resin rather than building it up could obtain a
better result.
Investing Process
The working model was invested in the bottom half of the Universal Flask (anaxdent) and 70 Shore clear silicone was injected onto a base of 60 Shore silicone. Any excess silicone was trimmed, undercuts were filled, and an application of Divorce separating medium was used to prevent the two similar silicone products from bonding (Figure 10). The Universal Flask was used due to its optimal size and suitability for larger cases and for its ability to accommodate and process the restoration directly on the master model. This material must be allowed a sufficient amount of time to dry. Injection canals were applied to the denture wax-up, preferably of 1.2-mm diameter (Tri-Wax Sprue System, Ivoclar Vivadent, www.ivoclarvivadent.com) and centered in on the glass upper part of the flask (Figure 11). A two-part clear silicone, Matrix Form Cast Clear (anaxdent) was vacuum-mixed and allowed to flow into the openings. The flask was now placed in a pressure pot and allowed to vulcanize at 2 bars of pressure for 25 minutes until clear (Figure 12 and Figure 13).
Framework Preparation
Once the vulcanization process was complete, the denture setup was removed from the flask, leaving a void for the framework to be placed (Figure 14). Before placing the framework, it had to be removed of all wax, sandblasted with a 110 aluminum oxide grit, steam cleaned, and dried with oil-free compressed air. It was then ready to be conditioned with a metal bonding agent.
A first layer of paste opaque, anaxblend Opaque (anaxdent) was thinly applied with a brush (maximum thickness of 80 um), then polymerized. This procedure was repeated two or three times until the desired opacity was achieved (Figure 15). A layer of composite primer (GC Fuji BOND™ LC, GC America) was added and polymerized for 60 seconds. The framework was placed into the flask and readied for the injection process (Figure 16).
First Injection
The first injection was used with composite preheated at 55 ºC using the Warm-Up composite heater (anaxdent) (Figure 17). Heating the materials decreases the viscosity and provides a better result. Various syringes can be used from a 3-gram dentin flow or a 20-gram Big Block. For this case, the author used a 20-gram syringe. The flask must be held at a 45-degree angle and injected from the last injection canal from the bottom to the first injection hole at the top of the flask. Constant pressure must be applied until the entire void in the flask is filled (Figure 18). After that, the flask may be polymerized. For this case the flask was polymerized for 6 minutes, based on the unit used. Polymerization times may vary.
Cutback
The injection canals were removed and a reduction was made on the dentin body to allow space for the second injection of the incisal material. The dentin body was then cut back to the desired specifications, and extensive composite primer was added to renew the dispersion layer and create more adhesion between the dentin body and the enamel. Because the patient required a bleach shade, the dentin body was not only cut back incisally, but also on the body and the cervical (Figure 19 and Figure 20). The dentin body was also characterized with anaxblend colors (anaxdent), color stains, and effect materials using anaxBlend NT Transpa and CL-O.
Second Injection
The restoration was then repositioned in the flask and the glass top was closed and tightened once again. The heated enamel was injected from the last canal from the bottom, filling the void in the silicone until it reached the top canal (Figure 21). Injecting composites is an advantage for the dental technologist because it can be processed within minutes and repeated if any issues occur. Unlike like other materials, no buildup is necessary.
Gingival Characterization
A composite primer was added to the gingival area and polymerized for 60 seconds. The gingival composite pastes—anaxgum Gingiva and anaxgum Gingiva Flow materials (anaxdent)—were heated. These composite pastes vary in opacities, translucencies, and colors. A base foundation was applied, followed by various colors, which were then built up in stages and polymerized until the desired effects were achieved (Figure 22 through Figure 25).
Final Polymerization and Finishing
Once the gingival buildup was complete, an air barrier medium, Cover Gel (anaxdent), was applied. This seals the restoration to prepare it for polishing. The air barrier was steamed and restorative surfaces were carefully pumiced to remove all residue. A polishing medium, Pasta Grigia I (anaxdent), was used with different varieties of bristle brushes (HATHO, www.hatho.com), along with a leather chamois, felt wheels, and cotton buffs (Renfert, www.renfert.com) (Figure 26 through Figure 30).
Conclusion
Once the restoration was polished, finished, and ready for insertion, a master mold was fabricated. The finished case was screwed on the master model, injection canals were replaced, and a new silicone pour was executed. This procedure allows for rebuilding the occlusion and the repair of potential fractures should they occur in the short-term future. This is a valuable tool for both the clinician and the technologist. Maintenance can be easily accomplished in a very short period of time and also provide long-term client retention for laboratories (Figure 31). The original denture setups still remain intact and can be saved for future use, for either injected or pressing techniques. Unlike an acrylic hybrid, which must be restored, or a ceramic implant bridge that fails and requires multiple appointments to have the restoration remade, a composite hybrid restoration can be rebuilt within minutes.
References
1. Suzuki S. In vitro wear of nano-composite denture teeth. J Prosthodont. 2004;13(4):238-243.
2. Avery J. Oral Development and Histology. New York, NY: Thieme; 2001.Av
About the Author
Robert Sarno, CDT, RDT
Owner
Pinnacle Dental Laboratory
Chesterfield, Missouri