Achieving an Esthetic, Additive Full-Mouth Reconstruction
Expand your occlusal knowledge to gain longer-lasting and reliable restorations.
By Brad Jones, FAACD; Brent Engelberg, DDS
Each dental treatment, from single tooth to full-mouth restorations, requires specific material characteristics. Highly regarded for their expertise and artistry, laboratory technicians are relied upon by dentists for their knowledge of physical, esthetic, and material properties for the successful fabrication of highly esthetic and long-lasting restorations. By choosing the least invasive treatment option, the following full-mouth reconstruction was achieved using the additive-reductive model with pressable lithium disilicate as the material of choice for fabricating anterior veneers and posterior crowns.
Dental wear can be divided into three categories: erosion, attrition, and abrasion.1 When tooth wear is due to attrition, the occlusal surfaces are worn down from tooth-to-tooth contact from natural forces such as chewing or pathological friction caused by bruxing.1,2
While it is agreed that emotional stress is often a precursor to bruxing, research indicates that occlusal interferences, however minor, can trigger bruxing, grinding, clenching, or gnashing of teeth.2 Grinding also contracts the elevator muscles, which overloads the teeth, support structures, and the temporomandibular joints (TMJ), and causes pain and tooth wear.
Natural tooth wear is unavoidable with aging. Complications, both structural or involving the surrounding soft tissue, can develop over time. If the masticatory system is kept in equilibrium, teeth should last a lifetime. The combination of enamel and dentin form a network that absorbs forces placed on teeth, enforcing structural integrity. Loss of enamel is also minimized when normal proximal wear is stabilized by occlusal wear. In certain cases, however, natural and/or pathological tooth wear during aging contributes to interproximal deterioration and dentin and enamel wear, eliminating the protective network and leaving teeth vulnerable to defects.3 Wear of the functional dentition can also alter craniofacial structures, including the masticatory stroke, the condyle, occlusal vertical dimension, canine guidance, and the edge-to-edge incisal relationship, resulting in excessive wear and malocclusion.
Occlusal instability can break down restorative dentistry, causing a need to re-cement crowns, re-bond veneers, and repair fillings and broken porcelain restorations.4 Knowledge of occlusal principles and recognizing the symptoms of malocclusion are critical to providing predictable, reliable, and long-lasting restorations.4 The occlusal treatment plan is determined by the patient’s condition and its underlying causes.
Designed to remove occlusal interferences and promote harmonious muscle function, splints or deprogrammers are primarily used to eliminate pain from grinding or TMJ dysfunction. They protect teeth from pathological wear and provide pre- and post-restoration stability. However, when damaged dentition results from malocclusion, restorative dentistry is often required.
To help ensure lasting restorations, occlusal balance must be restored. When the jaw muscles are in harmony and there is no premature contact of teeth, occlusal stability is achieved. Premature contact of teeth can cause overload. Therefore, posterior interferences to centric relation (CR) should be eliminated and anterior guidance established.2
While focusing on the preservation of sound tooth structure, many laboratory ceramists use the additive model as a conservative, less invasive treatment that provides lasting results.5 The importance of choosing an appropriate restorative material for additive treatment cannot be over-emphasized—the restorative material should promote conservative dentistry, provide superior wear resistance, be durable and long-lasting to avoid the need for re-restoration, and provide an esthetically pleasing smile. Various advanced materials allow ceramists to provide long-lasting, esthetic restorations while practicing conservative dentistry. Although some generations of porcelain veneers required invasive procedures, today’s all-ceramic veneers may be placed with minimal preparation.
Case Presentation
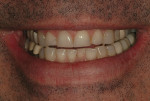
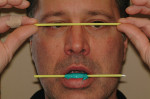
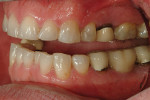
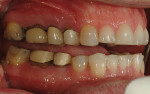
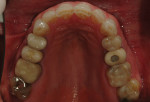
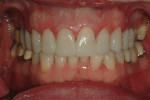
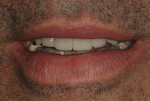
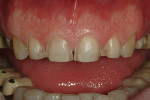
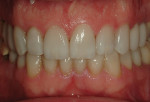
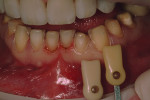
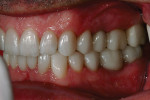
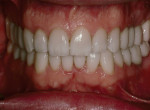
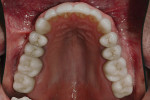
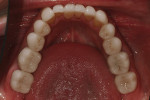
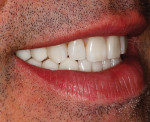
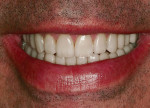
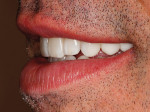
A 50-year-old, highly stressed businessman presented with severe wear on all teeth. The excessive wear developed over time because of a combination of age and malocclusion (Figure 1 and Figure 2). After the initial examination and consultation, the patient agreed to treatment in three phases using lithium-disilicate all-ceramic restorations (IPS e.max® Press, Ivoclar Vivadent, www.ivoclarvivadent.com). The patient was adamant about starting with “just the front upper 10” (ie, teeth Nos. 4 through 13). Restoration of teeth Nos. 20 through 29 was planned as the second stage, and the molars would be treated last.
Veneers were the treatment of choice for the patient’s anterior teeth, and crowns were chosen for the posteriors. The treatment plan involved correcting the occlusion, opening the bite, and providing cosmetic restorations. When the maxillary 10 restorations were seated, it was necessary to equilibrate the opposing mandibular teeth. A root canal also was needed on tooth No. 31 prior to completing the posterior restorations, because it was symptomatic and had a vertical fracture.
To achieve predictable results, dentists and ceramists should be knowledgeable about the patient’s masticatory forces and parafunctional habits.6,7 Joint vibration is a sign of joint dysfunction and/or joint pathology.8 Because of the patient’s unusual request to complete the rehabilitation in three phases and the necessity to open the bite, occlusal stability of the provisionals would be impossible to gauge, as they would never be in place at the same time. Therefore, an evaluation of the joint vibrations was performed to assess the health and function of the TMJ.
A full set of diagnostic photographs and radiographs were taken. A polyvinyl siloxane (PVS) impression material (Imprint™, 3M ESPE, www.3MESPE.com) was chosen for taking upper and lower impressions. The impressions also facilitated creation of a model of the initial and final restorations on the Stratos 200 articulator (Ivoclar Vivadent).
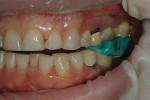
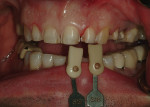
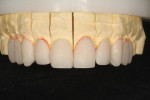
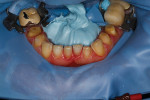
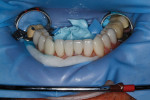
A centric bite registration was taken after the patient had worn an anterior deprogrammer for several days (Figure 3). Proper vertical dimensions were further established using upper and lower incisor cemento-enamel junction (CEJ) to CEJ measurements from digital calipers.9 This information enabled the ceramist to mount the case in centric relation and correct the patient’s vertical dimension. With the addition of clinical photographs, the ceramist produced a precision wax-up (Figure 4).
To meet the requirements of the patient’s form and function, ceramists must have all diagnostic tools necessary to complete the case and should understand that high-quality model work is a bedrock principle for achieving that goal. This foundation is crucial to achieving results synonymous with high-expectation dentistry, especially full-mouth reconstruction. Other diagnostic tools required to reach this level include preoperative, postoperative, and provisional photographs (Figure 5 through Figure 9), master impressions, provisional impressions, a CR bite registration, and a horizontal plane reference (stick bite). It is of the utmost importance to have either an eyebrow-to-chin photograph of the patient—with the stick bite in place on the lower incisors—to communicate the horizontal plane in relation to the patient’s face or an eyebrow-to-chin photograph with a grid overlay.
Additive-Reductive Model
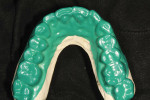
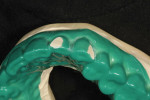
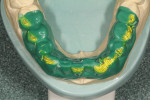
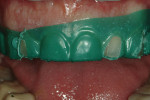
After the diagnostic models were poured and based, they were mounted using CR bites and an earless facebow (Kois Dento-Facial Analyzer, Panadent, www.panadent.com) with the Stratos/Kois mounting table on a Stratos 200 articulator. A green plastic suck-down material (LAK Enterprises, www.lakdental.com) was vacuum-formed over the preoperative model (Figure 10 and Figure 11). Any dentition protruding from the arch form (labially or lingually) was reduced, creating a reduction stent used intraorally so the dentition could conform to the proper arch form. The preparations were completed and the final margin positions were established and smoothed with the KS3SC, KS5SC, KS6SC, and 8856.021 burs (Komet USA, www.kometusa.com).
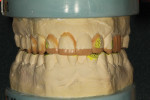
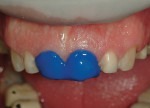
After highlighting these reductions on the preoperative model (Figure 12), wax was then added to both form and function (Figure 13 through Figure 15). This additive-reductive model operated as the essential blueprint for the provisional and ultimately the definitive restorations.
Provisionals
Because the procedure was an additive restorative technique, little tooth structure was removed prior to introducing provisionals (Figure 16 and Figure 17). Impressions were taken using impression trays (3M ESPE) filled with a heavy-body impression material (Imprint™ 3, 3M ESPE).
A “bite-jig” was created from a rigid PVS bite registration material (Mega Bite, Discus Dental, www.discusdental.com) on the articulated wax-up of the molars, and it was used to maintain the correct proposed vertical dimension throughout the procedure. The “bite jig” also was used by the ceramist to mount the upper and lower preparation models to the proper vertical dimension. Stump shades and digital photographs were taken to provide the laboratory with case specifics (Figure 18).
Provisional restorations were created based on the additive-reductive model. Photographs were taken and models of the provisionals were created (Figure 19 through Figure 22). Once the patient was satisfied, all photographs and necessary diagnostic information were forwarded to the laboratory with a prescription for IPS e.max Press restorations (ie, cutback and layered veneers) for the anterior teeth.
Laboratory Protocol
After receiving the provisional records, impressions, and eyebrow-to-chin photographs of the patient smiling with the provisionals in place (fabricated in plastic), a Sil-Tech® (Ivoclar Vivadent) matrix was formed over the cast of the provisionals and placed in a pressure chamber. This matrix then was used as a mold to inject wax onto the treated and lubricated master dies (Figure 24). Through the lost-wax process, the final restorations were produced using IPS e.max Press lithium-disilicate glass-ceramic. Impulse V1 was pressed at a temperature of 915° C (Figure 25 and Figure 26.).
Pressable lithium-disilicate material was chosen due to its superior characteristics and clinical results for posterior inlays and onlays, crowns, and anterior veneers.10 Proven to wear better and longer than other ceramics, it is an optimal material for full-mouth restorations. Because wear is significantly affected by the friction between materials and the material surface roughness, smoother surfaces produce the least amount of resistance and, consequently, result in the least amount of abrasion and wear.
In clinical studies, when finished with fine-grain diamond burs, less antagonist abrasion was generated from IPS e.max Press samples than from other available lithium-disilicate ceramic materials, indicating that IPS e.max press lithium disilicate provides durable and longer-lasting restorations.11 Press technology achieves a highly accurate fit, natural-looking shades, and optimal light transmission that create esthetic, life-like restorations.12-15
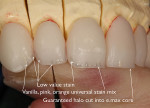
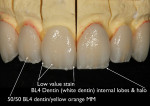
After pressing, divesting, and fitting the IPS e.max restorations, the facial surfaces were cut back 0.5 mm incisally to 0.2 mm cervically. A guaranteed halo was embossed around the outer silhouette of the incisal half, and stains were added to mimic the high and low values of the patient’s natural internal tooth structure (Figure 27.). After the stains were fired, internal effect powders were added to emulate a natural tooth with the enamel removed, then fired (Figure 28.). Next, the restorations were segmentally enameled and fired. Finally, the facial lobes and surface texture characteristics of a natural tooth’s surface were created. The restorations were then glazed, polished, and made ready for delivery (Figure 29.).
Seating the Restorations
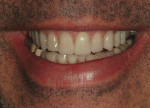
After viewing the final restorations when tried-in intraorally in various lighting conditions, including natural sunlight, the patient was pleased with the results. Proper adhesive protocols were then followed to definitively seat the restorations (Figure 30. through Figure 32.). Bisco adhesive All-Bond 3® (BISCO, www.bisco.com) was used for adhering the restorations, and Variolink® Veneer (Ivoclar Vivadent) cement was used for bonding the teeth. The molars remained out of occlusion at this point because they were included in the planned final treatment stage. The remaining stages of the full-mouth reconstruction (ie, phase 2—teeth Nos. 20 through 29, and phase 3—the molars) were completed according to the same procedures (Figure 33 through Figure 35.). Upon conclusion of the case, the patient, dentist, and ceramist were pleased with the esthetic and functional treatment results (Figure 36. through Figure 44).
Conclusion
When fabricating a full-mouth restoration case, the forces resulting in the wear, breakage, joint dysfunction, or malocclusion should be considered. The goal of occlusal dentistry is to balance the masticatory stresses to prevent uneven and excessive contacts from breaking down dentition.16 Several issues need to be assessed, and resolved if necessary, to restore a stable and balanced occlusion. This includes, but is not limited to, TMJ dysfunction, occlusal vertical dimension, anterior guidance, performance of the masticatory musculature, and condylar function. The type of enamel wear can help determine the underlying causes and the appropriate treatment for any parafunction or pathway-of-destruction issues. Therefore, ceramists fabricating restorations for full-mouth rehabilitations should possess an in-depth knowledge of occlusal principles in order to provide predictable, reliable, and long-lasting restorations.
Acknowledgment
The author would like to thank Gosia Barczak for her involvement throughout the treatment process.
References
1. Bartlett DW. The role of erosion in tooth wear: aetiology, prevention and management. Int. Dent J. 2005;55(4 Suppl 1):277-284.
2. Dawson P. Functional Occlusion From TMJ to Smile Design. Canada: Mosby, Inc.; 2007.
3. Cohen RG, Rudo D. Treating cracked teeth. Inside Dentistry. 2011;7(10):78-84.
4. Hess, LA. The relevance of occlusion in the golden age of esthetics. Inside Dentistry. 2008;4(2):38-44.
5. The glossary of prosthodontic terms. J Prosthet Dent. 1999;81(8):39-110.
6. McIntyre F. Restoring esthetics and anterior guidance in worn anterior teeth. A conservative multidisciplinary approach. J Am Dent Assoc. 2000;131(9):1279-1283.
7. Montgomery MW, Shuman L, Morgan A. Joint vibration analysis in routine restorative dentistry. Dent Today. 2010;29(9):94-97.
8. Li X, Lin X, Wang Y. Temporomandibular joint vibration in bruxers. Cranio. 2009;27(3):167-173.
9. Spear FM. Interdisciplinary esthetic management of anterior gingival embrasures. Inside Dentistry. 2007;3:34-44.
10. McLaren EA, Cao PT. Ceramics in dentistry–part I: classes of materials. Inside Dentistry. 2009;5(9):94-103.
11. IPS e.max press. Scientific Documentation. Schaan, Liechtenstein: Ivoclar Vivadent; 2011:1-40.
12. Sorensen JA, Cruz M, Mito WT, et al. A clinical investigation on three-unit fixed partial dentures fabricated with a lithium disilicate glass-ceramic. Pract Periodontics Aesthet Dent. 1999;11(1):95-106.
13. Höland W, Schweiger M, Frank M, Rhein-berger V. A comparison of the microstructure and properties of the IPS Empress 2 and the IPS Empress glass-ceramics. J Biomed Mater Res. 2000;53(4):297-303.
14. Kheradmandan S, Koutayas SO, Bernhard M, Strub JR. Fracture strength of four different types of anterior 3-unit bridges after thermo-mechanical fatigue in the dual-axis chewing simulator. J Oral Rehabil. 2001;28(4):361-369.
15. Guess PC, Zavanelli RA, Silvia NR, et al. Monolithic CAD/CAM lithium disilicate versus veneered Y-TZP crowns: comparison of failure modes and reliability after fatigue. Int J Prosthodont. 2010;23(5):434-442.
16. DiMatteo, AM. Pounding on the occlusion pulpit. Inside Dentistry. 2008;4(3):102-110.
This article is also presented online as CE at dentalaegis.com/go/idt50
To earn additional CE hours, check out Total Advantage Live, a 4-day course on cosmetic dentistry taught by Brad Jones and Dr. Engelberg. For more information and registration, visit: dentalaegis.com/go/idt46
About the Authors
Brad Jones, FAACD
OwnerSmiles, Inc.
Boise, Idaho
Brent Engelberg, DDS
Private Practice
Arlington Heights, Illinois