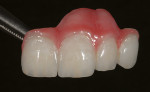
Esthetic Provisionals to Final Restorations
There are three key components for an optimal final restorative solution.
By Peter Pizzi, MDT, CDT, FNGS
In the March issue of Inside Dental Technology, the author demonstrated the importance of creating an esthetic provisional.1 The esthetic provisional plays a critical role in understanding how to achieve all of the details needed to complete a highly esthetic final prosthesis. The three primary purposes of the esthetic provisional are:
• Tooth Position: The provisional restoration should be the key determinate in establishing the incisal edge position, midline, horizontal plane, and starting point for basic tooth shape, ie, morphology, position, embrasure space, and possible rotation.
• Case Acceptance: The provisional is crucial to functional acceptance of the case as it pertains to occlusal vertical dimension (OVD), guidance, phonetics, and a mutually protected occlusion.
• Esthetics: Provisionalization is the trial phase for the case to assess negative space, color transition, and translucency.
These three keys are also critical for creating a blueprint of the final restorative solution and its esthetic outcome. One of the challenges here is our ability to have a role in the provisional process. A common thread of discussion among laboratory technicians both here and abroad is the lack of patient information provided by the clinician. Esthetic cases that do not include preoperative photographs, provisional photographs, and provisional casts limit the ability of the technician to deliver an esthetically challenging case. No matter what our level of expertise, we must accept the fact that we are just not good enough to replace a missing part of the human body without defined parameters as to where it belongs physically, functionally, and esthetically. Referring again to the March article, the wax-up was the author’s interpretation of the restorative solution that he believed to be proper for that particular patient. The fabrication of the provisional restoration became the test-run of that hypothesis and an evaluation of its possible esthetic pros and cons. After placement of the provisional, a photograph and study cast now became the key factors in the design and fabrication of the final restoration.
Case Presentation
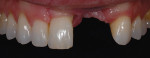
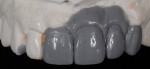
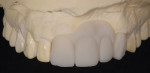
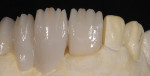
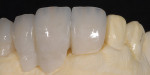
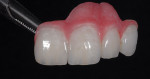
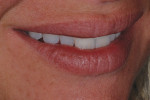
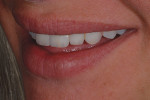
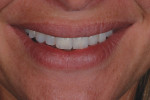
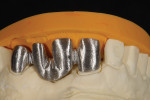
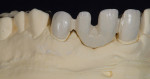
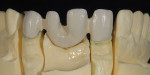
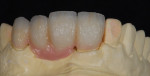
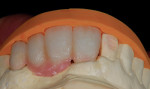
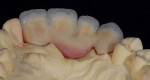
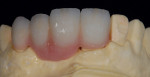
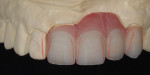
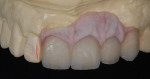
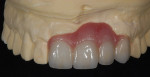
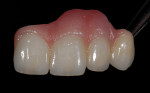
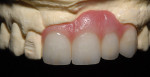
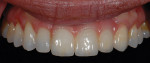
The patient presented with missing teeth Nos. 9 and 10 without the ability to place implants in the edentulous sites (Figure 1). The difficult esthetic challenge faced by the dental team in this case was to recreate the missing teeth, the gingival tissue, and bony arch. The first protocol was to fabricate a diagnostic wax-up. The diagnostic wax-up served as a guide to fill the voids and create the needed tooth height-to-width ratio in comparison to the height of the gingival tissue, as well as the papilla’s relationship to the tooth position. The diagnostic wax-up was then duplicated into an acrylic shell (Figure 2 and Figure 3). The acrylic was cut back, stained, and relayered with enamels and pink composites (Figure 4, Figure 5, Figure 6). The final provisional was placed and photographed for esthetic and functional evaluation (Figure 7, Figure 8, Figure 9). The patient left the practice feeling confident with the esthetic outcome.
Moving Forward
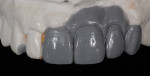
With the parameters of the case established in the provisional, an index of the provisional cast and a photograph of its esthetic outcome can be used to design the final framework (Figure 10). The author opted to fabricate porcelain-fused-to-metal restorations based on the connector size of the framework for anterior esthetics. Compared to a zirconia framework, which needs a larger connector size and possibly limits the proper embrasure spaces in the anterior zone, a metal framework allows for the thinnest connector for the proper embrasure spaces (Figure 11).
Now, a few shortcomings of the provisional, such as the gingival color, can be addressed. In years past when using gingival porcelain, the underlying opaque had been applied in a pink color. Today, we realize that this protocol was not entirely correct. The gingival is opaqued in a “boney” color and then overlaid with a selection of pink material (Figure 12). The ceramic margins were another challenge in this case. Ceramic margins are the author’s comfort zone to fabricate. However, this particular case needed a “pink” material to help finish the gingival portion of the case. A custom-colored marginal material was created to match the patient’s natural gingival tissue (Figure 13).
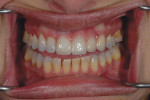
The index again became a guide for the ceramic build-up. After the first bake, a good working canvas for the framework had been created (Figure 14). A second bake of mostly effects and enamels was fired and the contours of the gingival material began to take shape (Figure 15 and Figure 16). After contouring, the author evaluated the esthetics and shape of the final restorations. As with any case, photographs are a good adjunct for case evaluation (Figure 17). An additive glaze bake allowed the author to create the final texture on the facial aspect of the teeth and to contour the gingival portion of the restoration with additional gingival ceramic (Figure 18 and Figure 19). Although the glaze bake created a nice facial surface, the glaze-fired surface did not replicate the patient’s natural tooth surface. The restorations had to be polished to achieve and match the proper luster of the adjacent natural teeth (Figure 20, Figure 21, Figure 22). The final restoration was delivered, seated, and blended fairly well in the oral environment (Figure 23 and Figure 24). The ability to achieve the esthetic realities of the final case was made possible through the proper preliminary clinical preoperative information, the creation of a diagnostic wax-up to serve as a guide, and the fabrication of a provisional restoration that provides the technician direction for the final case outcome and final placement (Figure 25, Figure 26, Figure 27, Figure 28).
Reference
1. Pizzi P. Fabricating esthetic provisionals. Inside Dental Technology. 2011; 2(3):36-39.
About the Author
Peter Pizzi, MDT, CDT, FNGS
Owner and Manager
Pizzi Dental Studio Inc.
Staten Island, New York