Creating a Custom Denture Base Plate
How to provide a more accurate foundation to evaluate the fit and stability of the final product.
By Robert Kreyer, CDT; and Renzo Chiappe
Times have changed, and so have the demographics in the dental laboratory industry and profession. Now more than ever, dental technologists must take on the task of encouraging and inspiring a new generation of laboratory professionals to ensure a bright future for the profession and industry. Though the materials, techniques, and equipment will change, the basic principles of prosthodontics will remain the same. The Internet offers today’s technologists a wide variety of interactive means to communicate with colleagues and other dental professionals and to share information about new developments as well as tried-and-true techniques.
Over the past few years, the number of opportunities for advanced learning has skyrocketed with the increasing amount of online and web-based education available. Those who invest in their future by taking advantage of these vast resources and by attending hands-on courses will benefit greatly, as it will enable them to practice and perfect their prosthetic techniques to reach a higher level of personal and professional proficiency. In his book Outliers: The Story of Success, Malcolm Gladwell says it best: “Practice isn’t the thing you do once you’re good. It’s the thing you do that makes you good.”1
Exposure to the principles of cosmetic dentistry has increased the expectations of today’s denture consumers. Many clinicians are encountering a new aging patient population with very active lifestyles that include travel, recreational sports, and fine dining. These patients are demanding esthetic, functional, and cosmetic outcomes that mimic natural dentition. For clinicians who provide removable prosthetics to this older population, technicians must design and create a complete prosthesis that exceeds the esthetic and functional expectations of both the clinician and the patient. This article details Renzo Chiappe’s approach to removable prosthetics and the techniques he uses to create a custom base plate.
The Prosthetic Approach
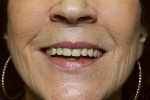
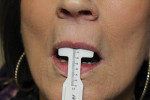
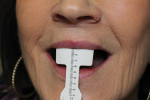
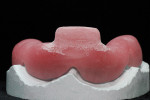
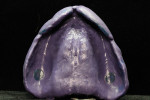
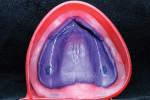
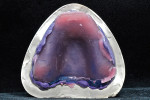
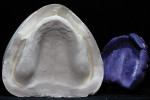
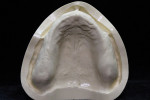
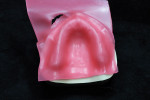
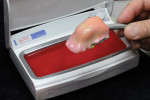
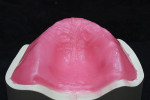
Removable technicians should aim to work alongside the restorative practitioner during every phase of the case. To acquire the information necessary to fulfill both the patient and clinician’s expectations, it is essential that the technician take pictures prior to treatment, listen to the dentist explain the case to the patient, and understand the patient’s desired outcomes (Figure 1). Taking facial measurements with a papillameter (Figure 2 and Figure 3) is key to achieving an esthetic outcome, along with the preliminary impressions the dentist takes and the custom tray that the technician fabricates from them (Figure 4 and Figure 5). The border-molded impression provides a stable and retentive biofunctional processed base (Figure 6 and Figure 7). In order to take advantage of the sediment properties of the model stone, boxing the final impression is very important (Figure 8, Figure 9, and Figure 10).
To ensure that the processed base is anatomically correct, a cast is created that preserves the proper horizontal and vertical extension of the peripheral borders with custom palatal rugae.
If the dentist carefully takes the time to copy every detail of the rugae with the impression, it is imperative for the technician to honor that effort by creating quality model work in the laboratory. Boxing and measuring the die stone to exact factory specifications should be the standard for model creation in order to achieve the best result and to replicate every detail of the impression (Figure 11).
Benefits of a Processed Base Plate
The traditional base plate has many disadvantages and often results in the dentist having to explain to the patient that it does not accurately represent the retention or stability of the final denture. This often makes both the patient and the treating clinician uncomfortable and leaves them with uncertainty about the final delivered prosthesis.
A processed base plate, on the other hand, has many benefits. It provides the clinician and technician with a more accurate foundation to evaluate fit and stability of the final product. Most importantly, a processed base plate is the definitive gingival base for the complete denture. It enables the clinician to evaluate phonetic function and vertical dimension during the try-in appointment and to detect pressure points. A processed base plate allows adjustments to be made to the plate up until the time of delivery and seating appointment, which reduces the frequency and duration of follow-up appointments. Another benefit of the processed base plate is that it enables a better evaluation of the denture stability. If the dentist is not satisfied with the suction achieved in the base plate design, a wash-off impression can be executed after the denture tooth setup to get the patient’s approval for the final processing.
The ability to replicate the rugae in the processed base plate also provides the patient more natural function when eating. The palatal rugae have a passive function in the mastication and swallowing process. The upper part of the tongue presses food up against the hard palate (rugae) to begin the movement of the food back toward the soft palate for swallowing. The palatal rugae provide a static grip surface for the tongue to move food around in the mouth during the chewing and swallowing process. For patients with existing dentures that have a smooth palate, this functional concept may be difficult to understand and challenging for the clinician to explain.
Creating the Processed Base Plate
There are a couple of techniques that technicians can use to fabricate and replicate the palatal rugae. The technique described here is a variation of the standard technique taught in dental technology programs. The first technique involves taking an impression of the master model with light-body impression material and wash putty to transfer the patient’s palatal rugae to the base plate (Figure 12). The second technique is for the technician to take an impression of his own palatal rugae with light-body impression material and wash putty, making sure to keep the thickness of the silicone impression to about 3 mm. When finished, the impression must be cleaned and sterilized. Then a handpiece should be used to remove the impression of the thumbprint made on the opposing side of the impression, ensuring the impression retains a uniform thickness. This is important for the adaptation of the wax rugae to the base plate (Figure 13 and Figure 14) because the shape of the technician’s mouth is not the same shape as the patient’s and because the base plate must be flexible enough to press. To create the custom base plate, the custom rugae should be dipped in liquid wax (Figure 15), and dipping should be repeated until the desired thickness is attained (Figure 16). The technician must carefully control the heat from the opposite side of the rugae because the silicone has the tendency to hold heat (Figure 17). By controlling the heat to facilitate the union of the base plate and custom rugae, the custom rugae will remain intact (Figure 18 and Figure 19). After the two sections are placed together, they should be aligned and held in place then gently cooled (Figure 20). The technician must press the sides of the custom rugae to adapt it to the base plate. Natural separation will indicate when the correct temperature has been reached so that the natural rugae can be gently separated from the silicone (Figure 21).
The mid-line must be marked on the model and the silicone impression of the palatal rugae so it can be aligned correctly (Figure 22). If there are problems with alignment, the impression can be pulled off and re-created. The sides of the rugae should be sealed by pouring hot wax into the separation between the two sections and pressing to hold them together (Figure 23). A heated waxing tool should be used to soften the wax sides of the base plate (Figure 24) and the deeper, retentive areas of the just-transferred natural rugae (Figure 25).
It is important to create custom rugae for every case. If the dentist can successfully explain the functionality of the rugae to the patient, the patient can test the functionality and the technician can make adjustments to smooth it out or remove it if that is the patient’s desire. It is very important when working on base plates with rugae to highly polish the plate to reduce the possibility of tartar build-up on the denture surface. The use of a low-speed handpiece and polishing compound is a must to preserve the integrity of the rugae. One technique is to cut a goat-hair brush in a serrated shape and polish the rugae in different directions at low speed (6,000 rpm). Using first pumice and then high polishing paste, the long goat hairs of the brush can reach and highly polish the recesses of the rugae. Figure 26 and Figure 27 show the finished custom base plate ready for processing.
This article is dedicated to those that have taken their time, energy, and vision to mentor dental technicians in removable prosthodontics.
Reference
1. Gladwell M. Outliers: The Story of Success. New York, NY: Little, Brown and Company; 2008. Robert Kreyer, CDT
About the Authors
Robert Kreyer, CDT
Director of Removable Prosthodontics
Microdental/DTI
Dublin, California
Renzo Chiappe
Owner
Chiappe Dental Lab
Covington, Louisiana