Taking Control of a Difficult Case
How to guide patients to accept treatment that will benefit them most.
Peter Pizzi, CDT, MDT, FNGS
Realistically, the esthetic dentistry boom of the mid-2000s, when elective casework dominated the fixed market, has dried up. In today’s economy, patients are reluctant to accept a more costly esthetic treatment plan, especially when their perception of the treatment solution is a simple repair or crown replacement.
Every member of the dental team can certainly understand a patient’s financial concerns. However, if the treatment solution presented is one that the team believes will give the patient the most esthetic, functional, and predictable outcome, then they must work with the patient to find creative solutions that do not compromise best-practice dentistry. It is the responsibility of the dental team to evaluate all aspects of a case and educate the patient on the best possible and probable outcomes without financial bias to the patient’s concerns.
Informed consent is the profession’s mantra, and everyone knows that the educated consumer is the best customer. Many times situations arise that cause both clinicians and technicians to rethink the proposed treatment protocol or to explain the “whys” and “whats” of a treatment plan. Although this is often a difficult and uncomfortable task, the dental team must adhere to what it believes is best for the patient. It is critical to the team’s confidence in itself and to the patient’s confidence in the team.
The Case
The author recently received a case from a local dentist with whom he frequently works. The patient presented with veneers on teeth Nos. 8 and 9 that had been completed by another dental team. The patient explained that the veneer on tooth No. 9 had debonded on several occasions. He was seeking a new dental team to replace the debonded veneer on tooth No. 9 using materials that would provide a long-term solution.
The Problem
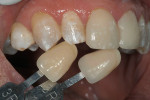
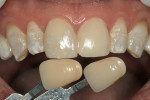
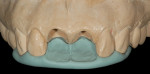
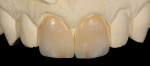
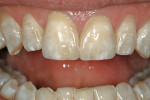
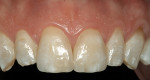
The challenge with this patient was to create a single central incisor to match an existing restoration. For technicians, fabricating a single central incisor restoration to match natural dentition that blends into the oral environment is the most difficult challenge in restorative dentistry (Figure 1 and Figure 2). However, matching a single central incisor restoration to a pre-fabricated restoration is even more difficult. At least when attempting to match a natural tooth, technicians have an understanding of anatomy and a point of reference on how to recreate nature.
When attempting to match a pre-existing ceramic restoration, however, technicians do not know which ceramic material was used or the depth of the enamels, dentin, or effect materials. Nor do technicians know what firing parameters were used both in amount and maturity. Any and all of these parameters greatly affect the final outcome and create an enormous challenge.
Secondly, from an esthetic point of view, replacing only the veneer on tooth No. 9 would be patchwork dentistry at best. And worse, if the technician were to fabricate No. 9, there would be no assurance that the restoration on tooth No. 8 would not exhibit the same debonding problem in the future. So the challenge became how to convince the patient that replacing both veneers would be best-practice dentistry.
The Solution
The patient is paying the full fee for the single veneer he wanted replaced because the author’s dental team was not the originating restorative team. For the dentist, this case appeared quite simple. Tooth No. 9 was already prepared for a veneer. All that was needed was an impression and photographs of the existing veneer in the No. 8 position for the laboratory. As long as the technician could match tooth No. 8, the patient would be satisfied with the final case outcome.
When the author received the case, he found himself in a dilemma. Even if it were possible to match tooth No. 8, he questioned whether the team was really giving this patient its best service. The patient was paying a very high laboratory fee to match a subpar, pre-existing restoration. Morally, the author would much rather fabricate two esthetically pleasing veneers that better matched the oral environment and that would give the patient a more predictable and functional outcome. Exceeding expectations would also ensure that the author’s client dentist retained this patient for future restorative work.
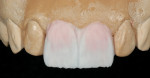
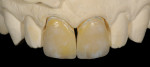
Rather than begin the fabrication process, the author made the dreaded phone call. Fortunately, the restoring dentist agreed with his assessment (Figure 3). The decision was to offer the patient two veneers for the price of one, with only an additional laboratory fee. The dentist’s chairtime would be the same whether it was a one- or two-veneer case. This was a win-win for the restorative team and for the patient. The author’s time was covered, and he was able to improve the esthetic outcome with confidence; the dentist was able to offer a higher level of service; and the patient received the best restorative care.
Communication Protocol
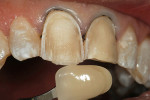
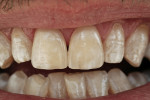
This case represents the good working relationship that can be achieved when the communication lines between team members revolve around what is best for the patient. The dentist re-prepared teeth Nos. 8 and 9 and impressed the case for the author (Figure 4). A mutual understanding of biological width (crest of bone to marginal finish line/contact area) was critical for this particular case to ensure healthy tissue response. Using the impression, the author created a refractory tissue cast (Figure 5). In combination with the finish line of the preparation, it played an important role in determining the contact point of the veneers (Figure 6 and Figure 7). Clinical photography submitted with the case was also critical during the ceramic build-up phase. The challenge for the author was to replicate the calcified look of the patient’s natural teeth. This was achieved by mixing white stains with white enamel (Figure 8). After firing, the veneers were divested and fitted to the original dies with yellow die spacer and checked on the master cast (Figure 9). The completed case was returned to the clinician for insertion (Figure 10 and Figure 11). The dentist/technician team successfully restored the natural smile of the patient (Figure 12 and Figure 13).
Conclusion
It is the responsibility of the dental team to ensure the long-term results of the restorative work it does. The services that dental teams offer their clients must be built on a solid foundation of education and knowledge. Patients need guidance to help lead them in a direction that will benefit them most.
At the same time, dentists and dental technicians cannot lose sight of the fact that they are operating a business; however, it should not be at the expense of the patient. The author believes that making the right choices and helping patients make the right choices is the building block of a good business. Practicing good dentistry creates patient confidence in the profession. What dental teams deliver and how they deliver it is the ultimate in self-promotion and builds the foundation for good business practices.