The Benefits of Glass Ionomers in Restorative Dentistry
An innovative cement that imitates some characteristics of natural teeth and provides fluoride-ion benefits
Glass-ionomer cement systems have gained a prominent place in modern clinical dentistry.1 Today, more than 40 states allow dental assistants to use glass ionomers in various capacities. Glass ionomer has become the common term for glass-polyalkenoate cements. These materials are made of calcium alumino-fluoro-silicate glass powder (base) combined with a water-soluble polymer (acid). When mixed together, the glass and acid components undergo a setting reaction involving neutralization of the acid groups by the powdered solid glass base. To curious patients, the authors describe this reaction as the following: The acid solution chemically melts the glass powder and creates a solid glass-like repair material that actually bonds to the enamel and dentin and, in many ways, resembles tooth structure. Significant amounts of fluoride ions are released from the glass powder during this reaction, without diminution of the hardened cement’s physical properties. The first glass-ionomer compound was invented in 1969, and Wilson and Kent2,3 reported about the new dental material concept in the early 1970s.
Regardless of the favorable properties of glass ionomers, the initial materials in the 1970s were quite difficult to use and had distinct disadvantages. They had long hardening times and were very susceptible to breakdown or fracture if they became too wet or too dry during the extended setting reaction. Their important physical properties, once set, were inferior to the resin-based composites, even though the glass ionomers were more compatible with, and comparable to, dentin. As time passed, materials scientists continued to work on developing glass-ionomer systems, realizing their potential and searching for ways to improve the products. Alterations in the glass particle sizes and distributions and types of acid formulations have improved handling and physical properties of the cements.
In the 1980s and 1990s, metal-modified glass ionomers and those containing a light-polymerized liquid resin component were introduced. Resin-modified glass-ionomer cements have significantly enhanced physical properties along with the great advantage of rapid, “on command” hardening by concentrated visible light exposure. Products in this class of glass ionomers have been manufactured and packaged in such ways to enhance handling, delivery of the material in the mouth, overall user convenience, and durability in the mouth.
Since the 1960s when glass-ionomer cements were first developed, the variety of tooth-colored restorative materials has caused confusion among dentists. The resin-based composites and glass-ionomer systems are the two major groups of such materials; however, the many variations and overlaps can make it difficult to sort out the product types. McLean et al4 addressed this issue in 1994, and Mount et al5 provided an update in 2009. A true glass-ionomer cement, whether it be used for tooth repair or luting purposes, has a hardening mechanism that involves a significant acid-base reaction—that is, the acid is a water-soluble polymer and the base is a special glass.4-8
All glass-ionomer systems share certain properties. Along with their chemical bonding to dentin and enamel, good biocompatibility, and easy handling by syringe injection, the hardened cements have coefficients of thermal expansion quite similar to that of tooth structure. That means when cold or hot foods influence expansion and contraction of enamel and dentin, the cement expands and contracts in concert. That property, along with the chemical bond, helps to maintain marginal integrity and facilitates fluoride-ion dynamics.
Glass-ionomer cement systems can be considered “therapeutic” dental materials. Fluoride ions are released by glass ionomers and are taken up by associated enamel and dentin. That tooth structure becomes less susceptible to acid challenge.9-27 In addition, water-based glass-ionomer materials act as fluoride-ion reservoirs by taking in salivary fluoride from dentifrices, mouthwashes, and topical fluoride solutions in the dental office. The fluoride content in true glass-ionomer systems and its ongoing activity is not only beneficial for young patients, but is particularly advantageous for all people with high susceptibilities to dental caries; for example, elderly patients with decreased abilities in personal home care and gingival recession with associated root caries.
Another major development in tooth restoration related to resin-modified glass-ionomer systems is that the light-curing resin component of the glass-ionomer cement chemically combines with resin-based composite material. Because certain glass-ionomer cements are the best direct-application dentin replacement materials presently available and resin-based composites closely simulate enamel, using the two in combination makes for biomimetic “tissue-specific tooth repair.”28,29 The word biomimetic means something imitating nature. This concept has been called layering, the sandwich technique, or stratification.
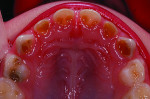
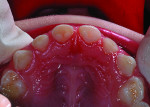
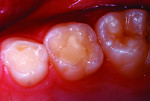
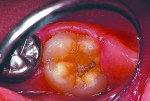
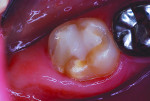
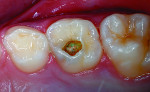
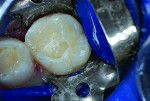
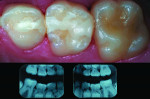
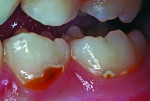
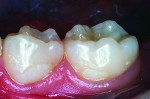
In the past decade, many new glass-ionomer products have been introduced in the dental materials marketplace. These include tooth-repair materials, dentin-replacement liners and bases, and luting cements. Along with their uses in cementing various types of full crowns in both permanent and primary teeth, glass-ionomer luting cements have proven extremely effective in orthodontics. The fluoride content of these cements is helpful to prevent decalcification around bonded brackets and other hardware and stainless steel bands cemented to posterior “anchor” teeth. While certain manufacturers have been the main source of glass-ionomer products and innovations, other dental companies have developed and introduced their own brands of glass-ionomer systems. Figures 1 through 10 demonstrate various uses for glass-ionomer cement systems.
Conclusion
The adhesive dentistry revolution that has propelled clinical dentistry to new heights in the past four decades is not about resin-based composites alone. Even though glass-ionomer systems, including resin-modified glass-ionomers, do not possess certain physical strengths of the resin-based composites, they have other advantages that make them excellent biomimetic materials to replace dentin. Some are good enough to replace both enamel and dentin for use in primary teeth and certain applications in permanent teeth, as well. As materials scientists continue their work, perhaps new direct-application restorative materials will be developed that have the physical properties and handling characteristics of both resin-modified glass-ionomers and resin-based composites.
Authors’ Note
This article is a modified version of Croll TP, Berg JH. Glass-ionomer cement systems. Inside Dentistry. 2010;6(8):82-87.
About the Authors
Theodore P. Croll, DDS
Private practice, pediatric dentistry
Doylestown, Pennsylvania
Affiliate Professor
Department of Pediatric Dentistry
University of Washington School of Dentistry
Seattle, Washington
Adjunct Professor, Pediatric Dentistry
University of Texas Health Science Center at San Antonio (Dental School)
San Antonio, Texas
Joel H. Berg, DDS
Dean
University of Washington School of Dentistry
Seattle, Washington
References
1. Croll TP, Nicholson JW. Glass-ionomer cements: history and current status. Inside Dentistry. 2008;4:76-84.
2. Wilson AD, Kent BE. The glass-ionomer cement: a new translucent dental filling material. J Appl Chem Biotechnol. 1971;21(11):313.
3. Wilson AD, Kent BE. A new translucent cement for dentistry: the glass ionomer cement. Brit Dent J. 1972;132:133-135.
4. McLean JW, Nicholson JW, Wilson AD. Suggested nomenclature for glass-ionomer cements and related materials (editorial). Quintessence Int. 1994;25:587-589.
5. Mount GJ, Tyas MJ, Ferracane JI, et al. A revised classification for direct tooth-colored restorative materials. Quintessence Int. 2009;40:691-697.
6. Nicholson JW, Croll TP. Glass-ionomers in restorative dentistry. Quintessence Int. 1997;28(11):705-714.
7. Nicholson JW. Glass-ionomers in medicine and dentistry. Proc Inst Mech Eng H. 1998;212(2):121-126.
8. Berg JH. The continuum of restorative materials in pediatric dentistry—a review for the clinician. Pediatr Dent. 1998;20(2):93-100.
9. Ewoldsen N, Herwig L. Decay-inhibiting restorative materials: past and present. Compend Cont Educ Dent. 1998;19:981-992.
10. Mitra SB, Creo AL. Fluoride release from light-cure and self-cure glass ionomers. J Dent Res. 1989;68:274[Abstract #739].
11. Tam LE, Chan GP, Yim D. In vitro caries inhibition effects by conventional and resin-modified glass-ionomer restorations. Oper Dent. 1997;22(1):4-14.
12. Scherer W, Lippman N, Kalm J, LoPresti J. Antimicrobial properties of VLC liners. J Esthet Dent. 1990;2(2):31-32.
13. Coogan MM, Creaven PJ. Antimicrobial effects of eight dental cements. Int Endod J. 1993;26(6):355-336.
14. Shelburne CE, Gleason RM, Mitra SB. Measurement of microbial growth inhibition and adherence by glass ionomers. J Dent Res. 1997;76:40 [Abstract 211].
15. Forsten L. Fluoride release from a glass ionomer cement. Scand J Dent Res. 1977;85(6):503-504.
16. Swartz ML, Phillips RW, Clark HE. Long-term F release from glass ionomer cements. J Dent Res. 1984;63(2):158-160.
17. Hicks MJ, Flaitz CM, Silverstone LM. Secondary caries formation in vitro around glass ionomer restorations. Quintessence Int. 1986;17(9):527-532.
18. Tyas MJ. Cariostatic effect of glass ionomer cement: a five-year clinical study. Aust Dent J. 1991;36(3):236-239.
19. Griffin F, Donly KJ, Erickson RC. Caries inhibition of three fluoride-releasing liners. Am J Dent. 1992;5(6):293-295.
20. Donly KJ. Enamel and dentin demineralization inhibition of fluoride-releasing materials. Am J Dent. 1994;7(5):275-278.
21. Souto M, Donly KJ. Caries inhibition of glass ionomers. Am J Dent. 1994;7(2):122-124.
22. Forsten L. Resin-modified glass ionomer cements: fluoride release and uptake. Acta Odontol Scand. 1995;53(4):222-225.
23. Donly KJ, Ingram C. An in vitro caries inhibition of photopolymerized glass ionomer liners. ASDC J Dent Child. 1997;64(2):128-130.
24. Segura A, Donly KJ, Stratmann RG. Enamel remineralization on teeth adjacent to Class II glass ionomer restorations. Am J Dent. 1997;10(5):247-250.
25. Forsten L. Fluoride release and uptake by glass-ionomers and related materials and its clinical effect. Biomaterials. 1998;19(6):503-508.
26. Donly KJ, Segura A, Wefel JS, Hogan MM. Evaluating the effects of fluoride-releasing dental materials on adjacent interproximal caries. J Am Dent Assoc. 1999;130(6):817-825.
27. Jang KT, Garcia-Godoy F, Donly KJ, Segura A. Remineralizing effects of glass ionomer restorations on adjacent interproximal caries. ASDC J Dent Child. 2001;68(2):125-128,142.
28. Croll TP, Cavanaugh RR. Posterior resin-based composite restorations: a second opinion. J Esthet Restor Dent. 2002;14:(5)303-312.
29. Croll TP, Cavanaugh RR. Tissue-specific, direct-application class II tooth repair: a case report. Compend Contin Educ Dent. 2009;30(9):608-614.