Treating Patients with a User-Friendly Glass Ionomer Restorative
This type of restorative may have potential to restore and prevent future decay in patients with compromised oral health.
David Hyten, DMD; and Debbie Murphy, DA
Prevention of recurrent decay is an important consideration for dentists and assistants as they restore teeth and counsel patients on good oral health habits. While patients are carefully instructed on proper hygiene techniques and necessary lifestyle changes, the fact is that there are some patients for whom proper oral care is always a challenge. This is commonly seen with senior-aged patients or those with physical handicaps. These patients may have systemic health conditions that hinder their natural defenses against decay, as well as their physical ability to care for their teeth.
Restoration of these cases requires special attention to the materials and techniques that can best help these patients. One such restorative material that may be too frequently overlooked is the resin-modified glass ionomer. The first generation of these materials, which were introduced in the 1970s, did not provide the necessary durability and esthetics.1 Later generations also did not adequately improve on these issues, and also had difficult handling and mixing characteristics. As a result, many practitioners have not enthusiastically embraced the glass ionomer category. However, new innovations from 3M ESPE have addressed many of these issues, renewing the potential of these fluoride-releasing materials to help patients with compromised oral health.
What Makes Glass Ionomers Effective?
Glass ionomers are formulated with a combination of water, an acid-functional polymer, and fluoroaluminosilicate glass. As these components react with one another, they create an acid-base material. Because the material is water-based, ions can be exchanged within it, which allows fluoride, calcium, strontium, and phosphate ions to move in and out of the material. This property is what gives glass ionomers their remineralizing capabilities, as the tooth-strengthening ions move out of the material and into the teeth.1 Glass ionomers are also self-adhering, which eliminates the bonding step required with composite restoratives.2
An additional beneficial characteristic of a traditional glass ionomer is its self-curing ability, which can be both a strength and a weakness. Because the self-cure can take up to 1 week, a traditional glass ionomer restoration is subject to water uptake, and may be brittle, which makes it less than ideal for use in load-bearing areas.1
To address some of the issues with the original class of glass ionomer materials, resin-modified glass ionomers were developed. By adding a polymerizable resin to the conventional formula, manufacturers were able to give the materials light-curing capability, improve their esthetics, and increase their dimensional stability and wear resistance.3,4
Overcoming Delivery Challenges
Even after these improvements, resin-modified glass ionomers were not favored at many practices because of their inconvenient delivery systems. Until recently, most of these products came in capsules, which required activation and trituration of the capsule prior to its use. In addition to being time-consuming, this method of delivery also occasionally resulted in “dud” capsules that failed to mix properly, which required that the assistant start the process again from the beginning.
Recently, though, a new delivery system has been introduced that helps prevent this problem. The Quick Mix Capsule for the Ketac™ Nano Light-Curing Glass Ionomer Restorative from 3M ESPE (www.3MESPE.com) is equipped with a tip that mixes the material’s two pastes inside of it, allowing for direct delivery via syringe. With this system, the assistant’s traditional mixing steps are eliminated. The nozzle on the capsule is lifted and inserted into the applier, and the material is ready to be dispensed. Not only is this system more convenient for the assistant, but research has shown that it also results in fewer voids than in restorations created with triturated capsules, making it more clinically reliable.5 It also saves a considerable amount of time for the assistant, thanks to the far fewer steps required for its use.
Technique and Cases
The general technique to create the resin-modified glass ionomer restorative is as follows:
- The patient is anesthetized and the tooth is prepared to remove the decay.
- The cavity is rinsed and slightly dried, but not desiccated.
- If necessary, a retraction cord is placed, such as in the case of a cervical lesion.
- Ketac™ Nano Glass Ionomer Primer is dispensed into a well and applied to the tooth with a fiber tip for 15 seconds.
- The primer is then dried with an air syringe for 10 seconds, but is not rinsed. With correct priming, the surface will remain shiny in appearance after drying.
- The primed surface is then light-cured for 10 seconds. These separate drying and light-curing steps help ensure maximum adhesion of the glass ionomer restorative.
- To apply the restorative, the orange mix tip is flipped open to 180º and the capsule is seated into the applier dispenser. A small amount of material is dispensed onto a cotton pad, after which the material is ready to be slowly syringed into the preparation, with care taken to keep the syringe tip immersed in the material to prevent entrapment of air.
- The material is then shaped and contoured, during which dental instruments can be wetted with additional primer to prevent the restorative from adhering to them.
- The material can then be light-cured for 20 to 30 seconds, depending on the curing light. The authors prefer the Elipar™ S10 LED Curing Light from 3M ESPE because it offers a fast, deep cure. The filling is then trimmed with fluted carbide burs and polished.
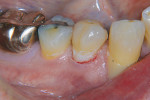
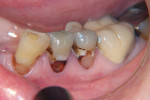
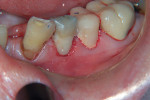
The cases shown here demonstrate the use of a glass ionomer in two instances of cervical decay (Figure 1, Figure 2, Figure 3, Figure 4, Figure 5 and Figure 6) and in one patient with gross decay (Figure 7 and Figure 8).
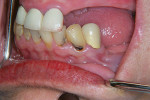
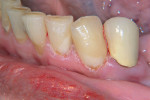
Figure 1 and Figure 2 show a 65-year-old woman with cervical decay on tooth Nos. 22 and 23. The patient was currently taking several prescribed medications that reduced her salivary flow and consequently contributed to the decay. It was hoped that use of the resin-modified glass ionomer, with its ongoing fluoride release, would help prevent recurrent decay.
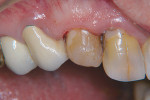
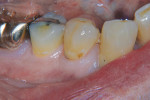
The second patient, seen in Figure 3, Figure 4, Figure 5 and Figure 6, was also a senior-aged patient with cervical decay. This patient, an 84-year-old man, had teeth Nos. 7 and 28 restored with resin-modified glass ionomer in a single visit.
Figure 7 and Figure 8 show a case in which the patient, a 52-year-old woman, suffered from gross decay. The patient was unable to brush properly due to poor dexterity caused by a medical condition. She was also taking prescribed xerostomia-causing medications to manage the medical condition. This combination of poor dexterity and lower salivary flow made the fluoride-releasing properties of the material especially helpful in this patient’s treatment.
Discussion
The technique described above is simple and straightforward, making it easy for both dentists and assistants to do their part in the restorative procedure. The consistent and reliable mix of the Quick Mix Capsule means the assistant does not have to be concerned about “dud” capsules or improper mixing. The time savings enabled by the material helps to keep the process moving efficiently, and, with the elimination of mixing, clean-up time is significantly reduced for the assistant.
For the dental team, a resin-modified glass ionomer restorative presents a number of attractive properties. Unlike composite, no bonding agent is required, and the traditional glass ionomer material also has the ability to self-cure. One notable feature of Ketac Nano Glass Ionomer Restorative is its availability in an A4 shade, which is especially useful in creating natural-looking restorations in senior patients, who tend to have darker teeth. The mix tip can also rotate in the applier dispenser, giving dentists easier access to every area in the patient’s mouth.
The fluoride release of a resin-modified glass ionomer makes it helpful in the treatment of patients who struggle with caries. In addition to the senior-aged and medically compromised patients seen here, these materials can also be useful for pediatric patients. The benefits of fluoride are commonly known among the patient population, so when patients are made aware that the restorative material being used in their treatment releases fluoride, many are very reassured to know that their dental team is doing all they can to help them prevent future decay.
References
1. Mount GJ, Tyas MJ, Ferracane JI, et al. A revised classification for direct tooth-colored restorative materials. Quintessence Int. 2009;40(8):691-697.
2. Data on file, 3M ESPE. Ketac Nano Light Curing Glass Ionomer Restorative Technical Product Profile.
3. Xie D, Brantley WA, Culbertson BM, Wang G. Mechanical properties and microstructures of glass ionomer cements. Dent Mater. 2000;16:129-138.
4. Rios D, Honorio HM, Francisconi LF, et al. In site effect of an erosive challenge on different restorative materials and on enamel adjacent to these materials. J Dent. 2008;3:152-157.
5. Boehm A, Brostrom M, Broyles B, et al. Void-Content and Customer-Satisfaction of Glass Ionomers: Novel Automix versus Triturated Capsules. IADR General Session, Barcelona, Spain. July 15, 2010.
About the Authors
David Hyten, DMD
Private Practice
Edwardsville, Illinois
Debbie Murphy, DA
Private Practice
Edwardsville, Illinois