Are Standard Precautions Really Universal?
Radiation hygiene is critical to providing patient safety.
You wear gloves, sterilize your instruments, and disinfect your work surfaces and use barrier protection. By practicing these and other universal standards, you assume you are keeping your patients and staff as safe as possible in the practice environment.
But what about radiation safety? You provide aprons with thyroid protection, are judicious about taking radiographs only when diagnostically necessary, and use high-speed film or digital sensors. By practicing these standards, recommended by the ADA,1 CDC, and National Council on Radiation Protection and Measurement (NCRP and state radiation guidelines), again you assume you are doing everything you can to minimize patient and staff exposure to ionizing radiation. However, if you are taking only these steps, you are not doing enough.
Radiation Hygiene
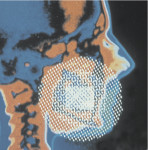
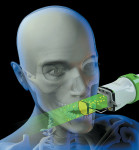
Just as you implement universal standards to prevent the transmission of disease-causing microbes, you need to implement radiation hygiene to minimize the transmission of disease-causing ionizing radiation (Figure 1).
With more and more traditional and social media coverage—from the relatively balanced to the blatantly sensationalist—about radiation exposure in medical and dental x-rays, patients are raising concerns about the safety of standard diagnostic radiography. Therefore, dental assistants need to be prepared not only with answers to patient questions, but with concrete proof that your dental practice is actually taking all of the steps necessary to ensure maximum patient safety.
The ALARA Principle
The core of radiation hygiene is the ALARA principle—As Low As Reasonably Acheivable.2 The point is, you must keep radiation exposure to patients and staff “as low as reasonably achievable,” according to the latest update of the NCRP’s Guidelines for Radiation Protection.
So what is required to comply with the radiation hygiene protocol? The NCRP has some very specific steps, which, fortunately, are all easy to implement. A complete version of the latest Guidelines is available for purchase by visiting https://www.ncrppublications.org.3 The report is very detailed and comprehensive, but the core recommendations are listed below.
Rectangular Collimation
Dentists, hygienists, and assistants have been taught that the only way to guarantee hitting the receptor (whether film, phosphor plate, or sensor) is with a large round cone.
Despite the fact that rectangular collimation is acknowledged to provide better images and to significantly reduce radiation exposure, the dental industry and profession may avoid it because of the high incidence of cone cuts associated with traditional options (Figure 2).
Enter the Tru-Align™ device from Interactive Diagnostic Imaging. This device is a game-changer because it eliminates these noted problems when it is installed on an existing x-ray head. It uses proprietary laser-guided alignment: when its internal LED laser and the positioning ring are precisely aligned, the ring magnetically and firmly snaps into place. As added assurance, green lights and an audible beep indicate the proper alignment as well.
As stated in the NCRP guidelines, rectangular collimation “produces more accurate images in terms of minimizing inaccurate relationships of one structure to another, foreshortening, elongation, distorition, and the overlap of structures such as contact points.”1 So in addition to the reduced radiation scatter, the system further enhances safety by reducing the risk of retakes.
The Tru-Align is compatible with any receptor type (film, phosphor plate, or sensor), as well as with popular positioners and holders. Its fits on all round cones between 2.5 and 3 inches in diameter and installs quickly without tools (Figure 3).
Implement All Recommendations
Included in the executive summary accompanying the NCRP’s Guidelines for Radiation Protection is the following: “Quality practice dictates that none [of the recommendations] be neglected. The technical factors, including office design and shielding, equipment design, clinical techniques, image receptors, darkroom procedures, and quality assurance are essential. However, the professional skill and judgment of the dentist in prescribing radiologic examinations and interpreting the results are paramount. Informed consent requires that dental patients be provided with information as to the benefits and risks of dental procedures, including dental radiography.”1
With the availability of the Tru-Align (Figure 4), dental assistants will have all of the resources to fulfill any part of the radiation hygiene recommendations. Compliance is simple, effective, and economical. Between universal standards and radiation hygiene, you can provide your patients and staff the safest environment and the highest quality of care.
References
1. American Dental Association. The Use of Dental Radiographs: Update and Recommendations. J Am Dent Assoc. 2006;137:1304-1312.
2. Hoos JC, Razzano M. The ALARA principle: Do you know what it is? Are you compliant? Dental Economics. 2010;100(11):128-129.
3. National Council on Radiation Protection and Measurement. Guidelines for Radiation Protection. Available at: https://www.ncrppublications.org/index.cfm?fm=Product.AddToCart&pid=1845765544. Accessed May 23, 2011.
About the Author
Don Cohen, DMD
Private Practice
Highland Mills, New York
For more information, contact:
Interactive Diagnostic Imaging
Phone: 855-idi-xray
Web: www.idixray.com
Disclaimer
The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dental Assisting.