Dental Infection Control and Technology
Eve J. Cuny, RDA, MS
The advancement of technology and science in dentistry over the past two decades is astounding. Lasers, microscopes, intraoral imaging, digital radiology, computerized clinic management systems, computer-controlled local anesthetic systems, chairside porcelain milling, and digital impression technologies are just a sampling of the advances realized in recent years. The benefits to patients and the profession from these technological developments are vast.
Infection Control Technology
In the arena of infection control in dentistry, we have seen the development of best practices and regulatory requirements that have solidified the use of heat sterilization as the gold standard for intraoral dental instruments and equipment. A shift away from the use of chemical disinfectants and sterilants to heat sterilization, in combination with the increasing use of barriers and disposable products, places dentistry in the forefront of outpatient healthcare providers in terms of asepsis. In addition, the development of new technologies to improve processes and ensure efficiency and efficacy of infection control practices are helping the profession to maintain these high standards for patient and worker safety.
Instrument Reprocessing
Instrument reprocessing is an important part of the dental office infection control program. Patients expect that the instruments going into their mouths are clean, sterile, and safe to use. Ensuring the safety of the instruments requires a systematic approach that is part technology, part practice, and part adequate knowledge of the mechanics of sterilization and cleaning.
Instrument Cleaning Technologies
Of all the methods available to clean instruments before sterilization, hand scrubbing is the least effective and efficient.1 Additionally, hand scrubbing increases the time the dental healthcare provider (DHCP) must handle contaminated sharp instruments. Increased handling of instruments provides a greater number of opportunities for accidental puncture injury and exposure to blood or other bodily fluids on the contaminated instruments.
Mechanical cleaning is a safe and effective way to prepare dental instruments for the final sterilization process. Cleaning is an essential element of instrument reprocessing. Debris such as tissue, blood, and dental materials left on instruments may hamper the effectiveness of the heat sterilization process. A combination of effective technology with the suitable cleaning agents will ensure that instruments are clean in preparation for the heat sterilization process. The use of inappropriate agents in the ultrasonic or washer/disinfector may damage instruments or hamper the effectiveness of the processes. It is important to follow manufacturer’s recommendations for cleaning agents added to these devices.
Ultrasonic Cleaning
Ultrasonic cleaning baths are not new to dentistry. For more than a generation, DHCPs have relied on these as the primary method of cleaning instruments and other materials in the dental practice. Ultrasonic cleaners use sound waves to create cavitations within the solutions. When these cavitations come into contact with instruments, they remove debris from the instrument surface. If the debris is firmly attached to the instruments, the cleaning process may be incomplete. Precleaning items that are known to be problematic (cements, resin materials, etc) is one way to overcome ineffective cleaning. For items heavily soiled with organic debris (eg, blood and tissue), the use of an enzymatic precleaning (spray or presoak) or enzymatic ultrasonic solution may provide superior cleaning results. In this situation, hand cleaning with a solvent intended for the type of debris is appropriate. Personnel should always wear utility gloves when handling instruments before placing and after removing instruments from the ultrasonic cleaner. Although these instruments are clean, ultrasonic cleaners do not produce germicidal activity, and it is possible that some contamination from instruments placed in the device may still be present after the cleaning process. Using the lid during operation will effectively eliminate any emissions from the ultrasonic during the cleaning process.2
Instrument Washers and Thermal Disinfectors
Large medical facilities and institutional settings have used instrument washers or instrument washers/disinfectors for many years. More recently, the dental manufacturing industry has begun offering these devices that are intended for use in a typical dental practice (Figure 1). Often resembling a household dishwasher, these devices function very differently than dishwashers and, under some circumstances, provide high-level disinfection of instruments during the cleaning process. Household dishwashers are not a suitable alternative to mechanical devices intended for cleaning dental instruments.
Instrument Washers
Devices classified and sold as instrument washers use an automated cycle to clean instruments. Some washers also have the ability to dry instruments before removing them for packaging and sterilization. These devices are an effective means of preparing instruments for sterilization. These devices may not disinfect instruments, and all appropriate personal protective equipment (PPE) is necessary until the instruments are placed in the sterilizer after packaging. PPE should include utility gloves to protect the DHCP’s hands from accidental puncture injury.
Washer/Disinfectors
Similar to instrument washers, washer/disinfectors (sometimes called thermal disinfectors) prepare instruments by removing debris that may interfere with the sterilization process. The major difference between the two types of devices is the ability of the washer/disinfector to perform high-level disinfection of instruments before the sterilization process. This renders the instruments safe for handling during packaging and while loading the sterilizer. Both may use a combination of chemicals and detergents to remove debris from instruments. The washer/disinfector follows the cleaning process with a high temperature water cycle that is a Food and Drug Administration-cleared method of high-level disinfection.
The cleaning agents used in combination with washers and washer/disinfectors often include multiple cycles with different chemicals. A typical washer/disinfector might start with a cycle containing an alkaline detergent, followed by an acid detergent, which acts as a neutralizer, and finally an enzyme wash to remove organic debris. Some may have the option of using a neutral detergent instead of the alkaline. Between washing cycles, there will also be a series of rinse cycles. Creating the right balance of chemicals for use in the automated washers and disinfectors is important because some metals or plastics are sensitive to the alkaline detergent. Manufacturers of dental instruments and the washer or washer/disinfector should be able to provide guidance on the right combination of detergents for the level of soil and types of instruments in a given dental practice.
Infection Control for Treatment Technologies
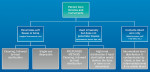
The fast-growing selection of devices and materials in dentistry requires that all of the professionals on the dental team plan for infection control when introducing any new product or material to the clinical care environment. Fortunately, many of the companies developing these new technologies are also providing suggestions or solutions for infection control challenges that may arise because of the introduction of these items to the clinical practice of dentistry. Regardless of the device, equipment, or instrument, the basic rules for determining if an item should be sterilized, disinfected, or barrier-protected applies (Figure 2). If an item contacts oral tissues, heat sterilization is the appropriate method. Only if the item cannot withstand the heat sterilization process should a chemical sterilant/high-level disinfectant process be substituted.3
Because many devices have intraoral components and then extraoral components that may be touched with contaminated gloves, a combination approach to infection control is often indicated. Detachable, reusable parts that go in the patient’s mouth should be heat-sterilized between uses. Barriers must be protected. Barriers must be impervious to fluids and changed between each patient in a manner that does not allow contamination of the device. If the device becomes contaminated, a low- to intermediate-level disinfectant can be used to clean and disinfect the item before returning it to service.
Parts of equipment that are touched with gloved hands during the procedure and cannot be detached for sterilization can be cleaned, followed by disinfection with a low- to intermediate-level disinfectant. Alternatively, barriers may be placed over switches and other areas that require touching and may be sensitive to contact with chemical germicides.
Computerized Systems
Paperless patient records and the need for information management systems in dental practices require the placement of computer components in patient care areas. In dentistry, this can be particularly problematic because dental procedures generate spray and spatter that may contaminate the computer equipment. The touch surfaces of the computer equipment can be a source of cross-contamination. Some viruses, such as hepatitis B virus (HBV), have the ability to survive on surfaces for extended periods if not inactivated by contact with a germicide.4 This may present a risk for patient-to-patient and patient-to-DHCP cross-infection. Simple measures, such as the appropriate use of barriers and low- to intermediate-level disinfectants, are effective in controlling cross-contamination.
Keyboard and Associated Devices
Widely available and inexpensive, sealed keyboards allow disinfection between uses. Some also contain an integrated touch mouse. Barriers are another possibility for providing aseptic use of the computer keyboard; however, plastic barriers slip and can make using the keys difficult. Sealed pointing devices (mouse) are available, as are barrier covers specifically developed for use with a traditional mouse. Signature pads are available as a sealed device that can be disinfected or may be placed in nonclinical areas of the dental facility.
Monitors
Swing arms for monitor screens allow the DHCP to move the monitor out of the zone of spray or spatter when using devices such as handpieces, sonic scalers, etc. This method is preferable to wiping the screen with disinfectants, which may damage the surface of the monitor. Touch-screen monitors present a particular challenge in the dental office setting. Although it may be possible to place a clear barrier over the screen, it may cause distortion or difficulty viewing some of the elements displayed. Ideally, one would avoid touching the screen with gloved hands and move the monitor out of range of spray and spatter during the dental procedure. Each dental practice should evaluate which solution is best suited to its needs and then develop standard operating procedures for the management of infection control with the variety of devices present in the office.
Digital Radiographic Machines
Digital radiographic procedures require a combination of technology that can present challenges for infection control. Computer components, film-positioning devices, sensors, and the x-ray head can all become contaminated during the imaging process. Film positioning devices are usually heat-stable and can be heat-sterilized after they are cleaned and packaged. Digital sensors, which cannot withstand heat sterilization, should be covered with fluid-impervious barriers that are changed between each patient, or they should be cleaned and then disinfected between each patient. Precautions for computerized components described previously in this article are also appropriate for digital x-ray units.
Conclusion
Each dental practice should evaluate which solution is best suited to its needs and then develop standard operating procedures for the management of infection control with the variety of devices present in the office. Creating a simple instruction sheet for infection control when introducing a new device into the practice is a relatively simple means of ensuring all items are handled properly. Attaching instructions to the device if it is portable, or the area of use for the device if it is not, helps to sustain the desired level of knowledge and practice for infection control.
References
1. Cafruny WA, Brunick A, Nelson DM, Nelson RF. Effectiveness of ultrasonic cleaning of dental instruments. Am J Dent. 1995;8 (3):152-156.
2. Bettner MD, Beiswanger MA, Miller CH, Palenik CJ. Effect of ultrasonic cleaning on microorganisms. Am J Dent. 1998;11(4):185-188.
3. Centers for Disease Control and Prevention. Guidelines for infection control in dental health-care settings–2003. MMWR. 2003;52(RR17):1-61.
4. Centers for Disease Control and Prevention. FAQs for Health Professionals. Division of Viral Hepatitis, National Center for HIV/AIDS, Viral Hepatitis, STD and TB Prevention. July 8, 2008. https://www.cdc.gov/hepatitis/HBV/HBVfaq.htm. Accessed December 17, 2008.
About the Author
Eve J. Cuny, RDA, MS
Assistant Professor, Director of Environmental Health and Safety
University of the Pacific, Arthur A. Dugoni School of Dentistry
San Francisco, California