The Protocols of Biomimetic Restorative Dentistry: 2002 to 2017
Increase the longevity of restorations with the biomimetic approach
David Starr Alleman, DDS | Matthew A. Nejad, DDS | Capt. David Scott Alleman, DMD
During the last 15 years, the restorative approach has steadily evolved, progressing from mechanical retention to advanced adhesion. This transition was fostered by a wealth of scientific publications, improvements in adhesive materials, and most importantly, worldwide dissemination of the science and techniques of advanced adhesion. Collectively, the science, principles, and techniques of advanced adhesive dentistry are known as biomimetic dentistry. At its core, the biomimetic approach respects the simple philosophy that, to adequately restore teeth, we must “mimic life” and understand the natural tooth in its entirety.1-3
Logically, conserving more of the intact tooth is paramount to this approach, which pairs perfectly with adhesion. Similar to the intact natural tooth, an adhesively-restored tooth is better able to handle and manage functional stresses. As a result, the biomimetically-restored tooth eliminates gaps under restorations and cracks into dentin that develop as a result of deformation and stress concentrations, reducing or eliminating postoperative pain and sensitivity and preserving vitality, as bacteria are not able to invade and kill the pulp.4,5 The natural flexibility and fracture resistance of a tooth are also enhanced when it is hydrated by the vital pulp. 4,6
The biomimetic protocols of today are founded on the “silent revolution” of adhesive dentistry that developed during the 80s and 90s.7-9 This revolution was advanced by Japanese researchers who identified two different layers of carious dentin that had two different characteristics of dentin adhesion. These researchers were able to predictably bond to dentin by using the novel technology of a caries detecting dye, which allowed an ideal caries removal end-point to be visualized in the all important “peripheral seal zone.”6 On a dentin surface free of denatured collagen, a bond to dentin could be established using newly developed polymerizable monomers that were both hydrophilic and hydrophobic. With these two technological breakthroughs, Dr. Takao Fusayama and his team of researchers at the Tokyo Medical and Dental University began the quest for conservative, long-lasting adhesive restorations.10 For the next two decades, continued advances in materials and techniques allowed for more extensive dental defects to be restored in both the anterior and posterior regions of the mouth.3,11-13
Fast-forwarding to 2002, a landmark book was published that advanced major concepts in biomimetic dentistry, including new information regarding the properties of natural teeth and their behavior under function, preparation design principles, and the all important foundational biomimetic concept of immediate dentin sealing.1,2 In the same year, a technique to reduce the effects of polymerization shrinkage stress was published, referred to as a stress-reduced direct composite, which allowed a biomimetic approach to a direct composite restoration.14-16 This article outlines the biomimetic paradigms and protocols that are supported by these and other scientific publications and practiced by biomimetic dentists around the world.
Biomimetic Paradigms
Biomimetic restorative dentistry is founded on these four basic paradigms:
1. Maximum bond strength. Reducing polymerization stress to the developing hybrid layer results in a 300% to 400% increase in bond strength.17-20 Dentin bond strengths in the range of 30 MPa to 60 MPa are in the same range as the tensile strengths of enamel, the dentinoenamel junction, and dentin.21 This strong bond allows the biomimetically restored tooth to function and handle functional stresses like an intact natural tooth.
2. Long-term marginal seal. A strong and secure bond allows for a long-term marginal seal to be established and maintained during functional stresses.3,22-25
3. Increased pulp vitality. By maintaining a highly bonded seal, the restoration will provide long-term function without recurrent decay, dental fractures, or pulp deaths.3,16,26,27 A vital tooth is also three times more resistant to fracture.28
4. Decreased residual stress. Residual stress, while hard to visualize, leads to cuspal deformation, debonding, gaps, cracks, pain and sensitivity, and recurrent decay. Reducing residual stress while maintaining the maximum possible bond strength is the ultimate goal of any biomimetic restorative technique.29,30
Biomimetic Protocols
The biomimetic restorative protocols used to produce these results can be divided into two groups: stress-reducing protocols and bond-maximizing protocols.
Stress-Reducing Protocols
The first group includes 10 key stress-reducing protocols, which promote stress reduction to the developing hybrid layer as it is formed and throughout the life of the restoration under function:3,25
1. Use indirect or semi-direct restorations for the occlusal and interproximal enamel replacements. An indirect technique is the most stress-reduced technique. It reduces the volume of shrinking restorative material.3,11,22 This also reduces residual stress.22,29,30
2. Decouple with time. This protocol states that polymerization shrinkage stress to the developing dentin bond of the hybrid layer should be minimized for a certain period of time (ie 5 to 30 minutes) by keeping initial increments to a minimum thickness (ie less than 2mm). This minimal thickness prevents the connection, or “coupling,” of deep dentin to enamel or superficial dentin before the hybrid layer is matured and close to full strength. This procedure neutralizes the “Hierarchy of Bondability,” which states that the shrinkage of composite moves toward (or “flows” toward) the walls of the preparation that are the most mineralized and dry and flows away from the walls of the preparation that are the most moist and organic.20,31-33
3. Restore the dentin with thin horizontal layers of composite that are 1mm or less.14,20 This ensures that decoupling with time is properly achieved and that the flow of the composite is not moving away from the deep dentin during the early stage of horizontal layer development. This is the solution to the problem of a preparation’s complex geometry and the resulting configuration stresses, which are known as “C-Factor” stresses.34,35 Small volume increments are always associated with small ratios of bonded to unbonded surface areas; thus, high C-Factor stresses can be reduced to “micro C-Factor” stresses. This is the basic protocol of the stress-reduced direct composite technique.14,15
4. For large restorations, place fiber inserts on pulpal floor and/or axial walls to minimize stress on the developing bond strength of the hybrid layer.24,36 The fiber nets allow the composite on either side of the net to move in different directions via micro shifting of the woven fibers. The polymer network is still highly connected, but the polymerization shrinkage does not stress the hybrid layer.37
5. Use slow start and/or pulse activation polymerization techniques.14-16,26,38
6. Use dentin replacing composites with shrinkage rates of less than 3% and with a modulus of elasticity between 12 GPa and 20 GPa.1-3,12,38
7. When restoring pulp chambers in non-vital teeth, use dual cure composite with the chemical cure mode active for the first five minutes.39 The volume of composite is not as critical for chemically cured composites because the chemical initiation of the polymerization is very slow (4 minutes to 5 minutes).34,35 This slow polymerization allows sufficient time for the dentin bonding system to mature into a strong hybrid layer.
8. Remove dentin cracks completely within 2mm of the dentinoenamel junction. This area is referred to as the “peripheral seal zone.” Remove all dentin cracks inside of the peripheral seal zone to a depth of 5mm from the occlusal surface and to a depth of 3mm interproximally from the axial wall.6 If cracks into dentin are left under the restoration, micro-movements under function will allow the cracks to get longer (ie crack propagation).4,5,40 Larger cracks propagate with smaller forces than shorter cracks; therefore, it is recommended to remove as much of the cracked dentin as possible without exposing the pulp.
9. Limit onlay cusps to thinner than 2mm after removal of decay and cracked dentin.1-3 This will change the forces on the hybrid layer from predominantly tensile to predominantly compressive, which helps reduce bond fatigue.25,41
10. Verticalize occlusal forces to reduce tensile stress to the restoration and the cervical region of the tooth.41 This can be done by restoring anterior guidance with bonded composite to the lingual surface of maxillary cuspids and/or the facial surfaces of mandibular cuspids.
Bond-Maximizing Protocols
The second group includes eight key bond-maximizing protocols, which, when implemented, can help achieve the maximum possible bond strengths attainable when employing the stress-reducing protocols:
1. Establish a caries-free peripheral seal zone. Achieve a caries-free zone 2mm to 3mm circumferentially around the cavity without exposing the pulp. Inside of the peripheral seal zone, caries excavation should be limited to a depth of 5mm, measured on the long axis from the cavo-occlusal surface. Measuring from the proximal tooth, the depth of excavation should be limited to 3mm from the cavo-proximal surface.6
2. Air abrade surfaces. Air abrade composite surfaces for bonding/cementation. This will increase bond strength to both normal and carious dentin.19,42 It will also change the failure mode to eliminate failures in the hybrid layer.19 When bonding to the composite base of a biomimetic restoration, air abrasion will maximize the composite-to-composite bond.12,43
3. Bevel enamel. Bevel enamel across enamel rods to increase bond strength.44
4. Deactivate matrix metalloproteinases. This prevents 25% to 30% of bond strength from being degraded.45 Deactivation can be achieved by using a 30 second treatment with 2% chlorhexidine (eg Consepsis, Ultradent), benzalkonium chloride (eg Micro-Prime B, Danville or Etch 37, Bisco), or a dentin bonding system with the MDPB monomer (eg SE Protect, Kuraray).6
5. Employ gold standard bonding systems. Use a gold standard dentin bonding system that can achieve a microtensile bond strength of 25 MPa to 35 MPa on enamel and 40 MPa to 60 MPa on flat dentin surfaces. The available data indicates that three-step total etch dentin bonding systems and two-step self-etch dentin bonding systems offer the best clinical performance.19,46
6. Utilize immediate dentin sealing. The application and polymerization of dentin bonding agents at the time of preparation (and before an impression is taken) has numerous advantages and will ultimately increase the microtensile bond strength by 400% when compared to the traditional approach of bonding the dentin at the cementation appointment.17,18 This is fundamental to achieving maximum bond strength.
7. Resin coat the immediate dentin sealing. This can be done with a flowable resin or a lower viscosity restorative composite with a modulus of elasticity of around 12 GPa (ie the same as deep dentin). This ensures that the dentin bonding system is fully polymerized even if the pressure of pulpal fluid transudation (in conjunction with the air-inhibited layer) has made the adhesive too thin to be polymerized due to air-inhibition. Once the dentin bonding system is resin coated and the resin coating is light polymerized, the air inhibition and transudation stop. This step also creates a “secure bond,” which means that if the onlay was ever dislodged from the resin coating, the resin coating would stay bonded to the sealed dentin.13,47-49 A few dentin bonding systems have thicker and highly filled adhesives (ie around 80 microns). These dentin bonding systems can act like a resin coating. Examples include OptiBond FL (Kerr), All Bond 3 (Bisco), and PQ1 (Ultradent).
8. Achieve deep margin elevation. A sub-gingival box margin needs to be bonded and raised to a supra-gingival position to obtain a biomimetic microtensile bond strength greater than 30 MPa. This deep margin elevation, in conjunction with immediate dentin sealing, resin coating, and the composite “dentin replacement,” is referred to as the “bio-base”—a term used by the Academy of Biomimetic Dentistry for the stress-reduced, highly bonded foundation that the indirect or semi-direct inlay or onlay will be bonded to.50,51
Case Presentation
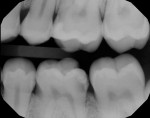
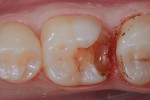
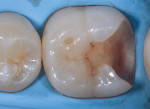
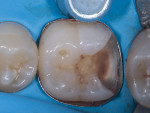
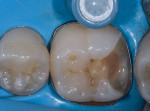
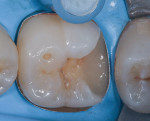
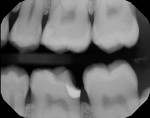
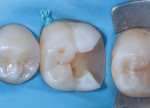
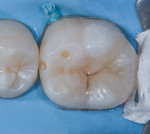
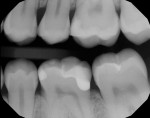
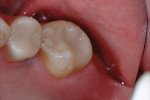
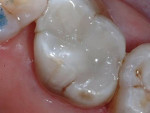
In this case, which would present problems for dentists who perform treatments without biomimetic restorative protocols, the caries are deep and the structure of the tooth is compromised (Figure 1 through Figure 10). For a traditional, full-coverage treatment, much of the intact tooth would have to be sacrificed. However, employing biomimetic restorative protocols can solve many of these problems by conserving tooth structure and promoting healing of the pulp. By combining the stress-reducing and bond-maximizing protocols, biomimetic restorative dentistry is able to reconnect all parts of the tooth with all parts of the restoration while maintaining a lifelike tensile/cohesive strength in the 30 to 50 MPa range.
Lifelike Longevity
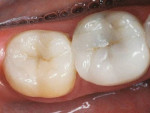
These two semi-direct biomimetic restorations (Figure 11) on teeth #3 DOLF inlay/onlay and #4 full onlay (mirror reversed) are more than 15 years old now. The onlay on the bicuspid and the inlay/onlay on the molar were restored using most of the protocols presented in this article with the exception of fiber placement for stress reduction and deep margin elevation on the bicuspid. There is a slight ditching of the flowable cementing resin on the molar, but no leakage is present. The onlays were fabricated out of Z-100 (3M, St Paul, MN).
This 10-year-old stress-reduced direct composite restoration (Figure 12) included fiber placement for stress relief. Only the cracks into the dentin were removed. The cracks into the enamel were stabilized with biomimetic protocols to re-establish a tensile cohesive strength from side to side, front to back, and top to bottom. As a whole, the tooth is now functioning again like a natural tooth. The occlusal surface was restored with Majesty Posterior (Kuraray, Okayama, Japan).
These Empress inlay and Empress onlay restorations (Figure 13) are 17 years old. Replacing occlusal and interproximal enamel, they are bonded to stress reduced bio-bases consisting of immediate dentin sealing, resin coating, and dentin replacement with a composite (AP-X, Kuraray) with a modulus of elasticity similar to dentin (16.7 GPa). The modulus of elasticity of the ceramic enamel (Empress, Ivoclar) is around 80 GPa. This number is a little higher than the enamel that it replaces, which has a modulus of elasticity of around 60 GPa. Composites with a modulus of elasticity of 20 GPa, such as Z-100 and Majesty Posterior, have also been functioning biomimetically for 10 to 20 years without breaking down.3
Conclusion
When performing a biomimetic restoration, it is vital to visualize the accomplishment of the protocols. Magnification in the 5X to 8X range is highly recommended when performing a biomimetic restoration.6 The use of a surgical microscope or high-powered loupes makes treatment very predictable.
Beyond the biomimetic paradigms, stress reducing protocols, and bond maximizing protocols, there are other principles that are related to biomimetic restorative dentistry. Minimally-invasive dentistry, structural analysis of existing tooth structure, and polymerization dynamics of composites are important topics that fully-trained biomimetic restorative dentists need to understand.34,35,40,52
The purpose of using biomimetic restorative concepts and protocols is to increase the longevity of restorative dental treatments and to reduce or eliminate future cycles of retreatment. In addition, conservation of tooth structure prevents periodontal complications and pulp death.27 Dentists and patients who choose biomimetic dentistry enjoy these benefits every day.
References
1. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing; 2002.
2. Magne P. Esthetic and Biomimetic Restorative Dentistry: Manual for Posterior Esthetic Restorations. Los Angeles, CA: USC School of Dentistry; 2006.
3. Bottacchiari S. Composite Inlays and Onlays: Structural, Periodontal and Endodontic Aspects. Milan, Italy: Quintessenza Edizioni; 2016.
4. Brannstrom M. Dentin and Pulp in Restorative Dentistry. London, UK: Wolfe Medical Publications; 1982.
5. Brannstrom M. The hydrodynamic theory of dentinal pain: sensation in preparations, caries and the dentinal crack syndrome. Journal of Endodontics. 1986;1 2(10):453-457.
6. Alleman D, Magne P. A systematic approach to deep caries removal end-points: The peripheral seal concept in adhesive dentistry. Quint Int. 2012;43(3):197-208.
7. Vanherle G, Smith DC. Posterior Composite Resin Dental Restorative Materials. 3M Co.; 1985.
8. Nakabayashi N, Pashley DH. Hybridization of Dental Hard Tissues. Chicago, IL: Quintessence Publishing; 1998.
9. Roulet J-F, Degrange M. Adhesion: The Silent Revolution in Dentistry. Chicago, IL: Quintessence Publishing; 2000.
10. Fusayama T. New Concepts in Operative Dentistry: Differentiating Two Layers of Carious Dentin and Using an Adhesive Resin. Chicago, IL: Quintessence Publishing; 1980.
11. Dietschi D, Spreafico R. Adhesive Metal Free Restoration. Chicago, IL: Quintessence Publishing; 1997.
12. Dietschi D, Spreafico R. Current clinical concepts for adhesive cementation of tooth-colored posterior restorations. PPAD. 1998;10(1):47-54.
13. Rocca GT, Krejci I. Bonded indirect restorations for posterior teeth: from cavity preparation to provisionalization. Quint Int. 2007;38(5):371-379.
14. Deliperi S, Bardwell D. An alternative method to reduce polymerization shrinkage [stress] in direct posterior composite restorations. J Amer Dent Assoc. 2002; 133(10)1387-1398.
15. Deliperi S, Alleman D. Stress-reducing protocol for direct composite restorations in minimally invasive cavity preparations. PPAD. 2009;21(2):E1-E6.
16. Deliperi S, Bardwell D, Alleman D. Clinical evaluation of stress-reducing direct composite restorations in structurally compromised molars: a 2-year report. Oper Dent. 2012;37(2):109-116.
17. Bertschinger C, Paul SJ, Luthy H, Scharer P. Dual application of dentin bonding agents: effect on bond strength. Am J Dent. 1996;9(3):115-119.
18. Magne P, Kim TH, Cassione D, Donovan TE. Immediate dentin sealing improves bond strengths of indirect restorations. J Prosthet Dent. 2005;94(6):511-519.
19. Van Meerbeek B, DeMunck J, Mattar D, Van Landuyt K, Lambrechts P. Microtensile bond strengths of an etch and rinse and self-etch adhesive to enamel and dentin as a function of surface treatment. Oper Dent. 2003;28(5):647-66
20. Nikolaenko SA, Lohbauer U, Roggendorf M, Petschelt A, Dasch W, Franenberberger R. Influence of C-Factor and layering technique on microtensile bond strength to dentin. Dental Mater. 2004;20(6):579-585.
21. Urabe I, Nakajima M, Sano H, Tagami J. Physical properties of the dentin-enamel junction region. Am J Dent. 2000;13(3):129-135.
22. Ida K, Inokoshi S, Kurosaki N. Interfacial gaps following ceramic inlay cementation vs. direct composites. Oper Dent. 2003;28(4):445-452.
23. Dietschi D. Evaluation of Marginal and Internal Adaptation of Adhesive Class II Restoration: In Vitro Fatigue Tests [PhD Thesis]. Amsterdam: Academic Center for Dentistry of the University of Amsterdam and the Vrije University; 2003.
24. Belli S, Orucoglu H, Yildirim C, Eskitascioglu G. The Effect of Fiber Placement or Flowable Resin Lining on Microleakage in Class II Adhesive Restorations. J Adhes Dent. 2007;9(2):175-181.
25. Nikaido T, Kunzelmann K-H, Chen H, et al. Evaluation of thermal cycling and mechanical loading on bond strength of a self-etching primer system to dentin. Dent Mater. 2002;18(3):269-275.
26. Deliperi S, Bardwell D. Clinical Evaluation of Direct Cuspal Coverage with Posterior Composite Resin Restorations. J Esthet Rest Dent. 2006;18(5):256-267.
27. Zollner A, Gaengler P. Pulp reactions to different preparation techniques on teeth exhibiting periodontal disease. J Oral Rehabil. 2000;27(2):93-102.
28. Kishen A, Vedantam. Hydrodynamics in dentine: Role of dentinal tubules and hydrostatic pressure on mechanical stress-strain distribution. Dental Mater. 2007;23(10):1296-1306.
29. Versluis A, Tantbirojn D, Pintado M, De Long R, Douglas WH. Residual shrinkage stress distributions in molars after composite restoration. Dental Mater. 2004;20(6):554-564.
30. Bicalho AA, Pereira RD, Zanatta RF, Franco SD, Tantbirojn D, Versluis A, Soares CJ. Incremental filling technique and composite material-part 1: Cuspal Deformation, Bond Strength and Physical Properties. Oper Dent. 2014;39(2):E71-E72.
31. Wilson NHF, Cowan AJ, Unterbrink G, Wilson MA, Crisp RJ. A clinical evaluation of class II composites placed using a decoupling technique. J Adhesive Dent. 2000;2(4):319-329.
32. Versluis A, Tantbirojn D, Douglas WH. Do dental composites always shrink toward the light? J Dent Res. 1998; 77(6):1435-1445.
33. Irie M, Suzuki K, Watts DC. Marginal gap formation of light-activated restorative material: effects of immediate setting shrinkage and bond strength. Dental Mater. 2002;18(3):203-210.
34. Davidson CL, de Gee AJ. Relaxation of polymerization contraction stresses by flow in dental composites. J Dent Res. 1984;63(2):146-148.
35. Feilzer AJ, De Gee AJ, Davidson CL. Setting stress in composite resin in relation to configuration of the restoration. J Dent Res. 1987;66(11):1636-1639.
36. El-Mowafy O, El-Badrawy W, Eltanty A, Abbasi K, Habib N. Gingival microleakage of class II resin composite restorations with fiber inserts. Oper Dent. 2007; 32(3):298-305.
37. Erkut S, Gulsahi K, Imirzahoglu P, Caglar A, Karbhari VM, Ozmen I. Microleakage in over flared root canals restored with different fiber reinforced dowels. Oper Dent. 2008;33(1):96-105.
38. Charton C, Colon P, Pla F. Shrinkage stress in light-cured composite resins: Influence of material and photoactivation mode. Dental Mater. 2007;23 (8):911-920.
39. Kuroe T, Tachibana K, Tanino Y,Satoh N, Ohata N, Sano H, Inoue N, Caputo AA. Contraction stress of composite resin build-up procedures for pulpless molars. J Adhes Dent. 2003;5(1):71-77.
40. Milicich G, Rainey JT. Clinical presentations of stress distribution in teeth and their significance in operative dentistry. Pract Periodontics Aesthet Dent. 2000; 12(7):695-700.
41. Magne P, Belser U. Rationalization of shape and related stress distribution in posterior teeth: a finite element study using nonlinear contact analysis. Int J Periodontics Restorative Dent. 2002; 22(5):425-433.
42. Sattabanasuk V, Burrow MF, Shimada Y, Tagami J. Resin adhesion to caries-affected dentine after different removal methods. Aust Dent J. 2006;51(2):162-169.
43. Papacchini F, Dall’Oca S, Cheffi N, Goracci C, Sadek FT, Suh BI, Tay FR, Ferrari M. Composite-to-composite microtensile bond strength in the repair of a microfilled hybrid resin: effect of surface treatment and oxygen inhibition. J Ades Dent. 2007;9(1):25-31.
44. Opdam N, Roeters JJ, Kuis R, Burgersdijk RCW. Necessity of bevels for box only class II composite restorations. J Prosthet Dent. 1998;80(3):274-279.
45. Pashley D, Tay F, Yui C, Hashimoto M, Breschi L, Carvalho R, Ito S. Collagen degradation by host-derived enzymes during aging. J Dent Res. 2004;83(3): 216-221.
46. De Munck J, Mine A, Poitevin A, Van Ende A, Cardoso MV, Van Landuyt KL, Peumans M, Van Meerbeek B. Meta-analytical review of parameters involved in dentin bonding. J Dent Res. 2012;91(4):351-357.
47. Krejci I, Stavridakis M. New perspectives on dentin adhesion—differing methods of bonding. Pract Periodontics Aesthet Dent. 2000;12(8):727-732.
48. Jayoosariya PR, Pereira PNR, Nikaido T, Tagami J. Efficacy of a resin coating on bond strengths of resin cement to dentin. J Esthet Restor Dent. 2003;15(2):105-113.
49. Belli S, Inokoshi S, Ozer F, Pereira PNR, Ogata M, Tagami J. The effect of additional enamel etching and a flowable composite to the interfacial integrity of class II adhesive composite restorations. Oper Dent. 2001;26 (1):70-75.
50. Magne P, Spreafico R. Deep margin elevation: a paradigm shift. Amer J of Estht Dent. 2012;2(2):86-96.
51. Frese C, Wolff D, Staehle HJ. Proximal box elevation with resin composite and the dogma of biological width: clinical R2-technique and critical review. Oper Dent. 2014:39(1):22-31.
52. Bazos P, Magne P. Bio-emulation: biomimetically emulating nature utilizing a histo-anatomical approach; structural analysis. Eur J of Esthet Dent. 2011;6(1):8-19.
About the Authors
David Starr Alleman, DDS
Co-Director
Alleman-Deliperi Centers for Biomimetic Dentistry
South Jordan, Utah and Cagliari, Sardinia, Italy
Co-Director
Biomimetic Dentistry CE
Beverly Hills, CA
Matthew A. Nejad, DDS
Co-Director
Biomimetic Dentistry CE
Beverly Hills, CA
Adjunct faculty
Herman Ostrow School of Dentistry
University of Southern California
Los Angeles, California
Capt. David Scott Alleman, DMD
Instructor
Alleman-Deliperi Centers for Biomimetic Dentistry
South Jordan, Utah and Cagliari, Sardinia, Italy
US Army Dental Corps
Seoul, Republic of Korea