Full-Coverage All-Ceramic Crowns
Clinical considerations for and management of nonvital teeth
Stephen J. Chu, DMD, MSD, CDT
Practitioners often face clinical decision-making challenges when removing a full-crown restoration. Various strategies and options are available in regard to materials selection and managing such factors as substrate discoloration, tooth preparation design, and depth/reduction. The case report presented here will exemplify the esthetic restorative correction and replacement of an existing full-crown restoration and demonstrate shade management of a discolored substrate of a nonvital maxillary right central incisor tooth. Tooth preparation design will be shown, and diagnostic nonvital bleaching options when restoring discolored substrate preparations will be presented.
The three clinical keys to know are: 1) the tooth preparation design that should be used in treatment; 2) the clinical situations that can be treated with nonvital bleaching techniques and materials; and 3) the type of material that can be used for full-coverage restorations. Esthetic restorative correction of discolored tooth substrate preparations can be clinically managed with an understanding of nonvital bleaching concepts and techniques along with proper restorative materials selection.
Background
Replacement of existing full-crown restorations can be perplexing because it is often difficult to assess what lies underneath. When the clinician is confronted with a discolored tooth preparation stump shade, the decision-making process can become convoluted. The clinical key to success is making the proper diagnosis, which includes tooth preparation design and reduction as well as material selection, to achieve a consistent esthetic restorative outcome.
Nonvital bleaching of a discolored stump shade preparation can lend to consistent treatment outcomes that may not have been fully realized by the clinician otherwise. Etiologies of tooth discoloration stem from two clinical situations: 1) dental trauma causing pulpal necrosis; and 2) microleakage of metallic ions into the dentin tubules. The first condition occurs when hemolysis of red blood cells releases ferric ions that combine with hydrogen sulfide to form ferric sulfide, a black compound responsible for tooth discoloration. The second clinical scenario happens when metallic ions leach into the dentin tubules, causing “tattooing” of the stump preparation of the tooth.1,2
Treatment of these discoloration conditions has been explored extensively in the endodontic literature. The use of sodium perborate (NaBO3) is effective for nonvital bleaching of ferric sulfide ions; this is commonly known as the “mild walking” bleach technique. In addition, the risk of internal/external root resorption is reduced when using NaBO3 and water with nonvital bleaching techniques.3,4
The causative agent for resorption is 30% to 35% hydrogen peroxide, more commonly known as superoxol.5 When using superoxol, an intraradicular glass-ionomer barrier or “plug” at the cementoenamel junction is recommended to occlude any accessory canals, thereby reducing the potential risk of resorption. In-office techniques can be used that employ a superoxol-saturated cotton pellet with heat. Mixing NaBO3 with water instead of superoxol has the same efficacy of bleaching but without the risk, although it does require more clinical appointments and time to achieve the desired results.
The mechanism of action is that oxygen radicals are liberated, which severs the stain molecules, thereby reducing them in size and decreasing the appearance of discoloration. Clinically, once the discolored stump shade preparation is corrected, a tooth-colored core and transparent or semi-transparent restorative material can be used for the definitive crown restoration. Even though nonvital bleaching can remove ferric sulfide ions in the dentin tubules, some authors have reported a recurrence or rebound rate of 20% following such techniques.6-8
Unfortunately, metallic ions bleached in the dentin tubules are resistant to the aforementioned techniques. Consequently, the treatment of nonvital discolored tooth preparation stumps in this type of situation leans toward the use of opaque, masking restorative materials, such as metal-ceramic crowns.
Case Report
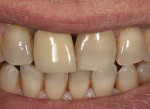
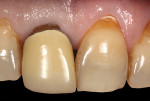
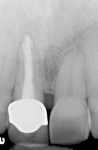
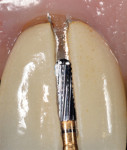
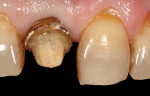
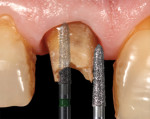
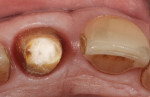
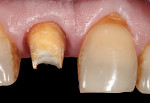
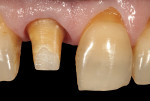
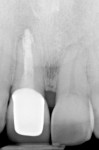
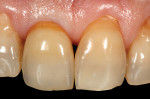
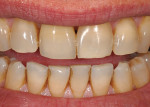
A 59-year-old man presented with an existing full-coverage crown on tooth No. 8 that after three decades of service ceased to match in shade. The crown exhibited midfacial gingival recession with margin exposure and poor marginal integrity (Figure 1 through Figure 3). The existing crown was removed using high-speed rotary instrumentation with diamond and carbide fissure burs (Figure 4). The tooth stump shade was discolored due to the formation of ferric sulfide in the dentin tubules as a result of intrapulpal hemorrhaging (Figure 5).
The tooth preparation was reprepared to create a 135-degree angular shoulder preparation using a K-series diamond (Brasseler USA, www.brasselerusa.com) (Figure 6). Subsequently, a paste-like mixture of sodium perborate and water was placed intracoronally into the pulp chamber to bleach the stump color of tooth No. 8 (Figure 7 through Figure 9). After the desired bleaching was achieved, a tooth-shaded foundation restoration was constructed for tooth No. 8 using a fiber-reinforced post system (D.T. Light-Post®, Bisco, www.bisco.com) and a core build-up material (FluoroCore® 2+, Dentsply Sirona, www.dentsply.com) (Figure 10).
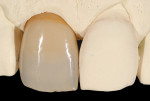
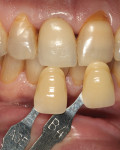
After definitive tooth preparation, final shade information was taken and impression-making was done with a polyvinylsiloxane material (Flexitime®, Heraeus Kulzer, www.heraeus-kulzer.com). A gypsum cast was poured to create a master die model (Figure 11). After two layering firing cycles, the restoration was contoured, textured, and fitted onto the master gypsum cast (Figure 12). The final restoration underwent a first try-in, and photographs with the shade tabs were retaken to reevaluate the shade (Figure 13). After finishing the final zirconia crown, the internal surface was cleaned, coated with a primer (Z-Prime™ Plus, Bisco), and cemented with a dual-cure resin cement (Maxcem Elite™, Kerr Dental, www.kerrdental.com) (Figure 14).
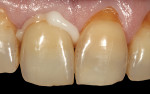
The successful results of the case, including excellent marginal integrity and esthetics, are shown in Figure 15 through Figure 17, as the maxillary right central incisor was restored to a state of functional health. The patient was well satisfied with the outcome.
Conclusion
As demonstrated in this case, the correction of a discolored stump shade preparation of a single central incisor tooth can be a predictable treatment option for restorative dentists using material that affords superb marginal integrity and esthetics.
References
1. Plotino G, Buono L, Grande NM, et al. Nonvital tooth bleaching: a review of the literature and clinical procedures. J Endod. 2008;34(4):394-407.
2. Dahl JE, Pallesen U. Tooth bleaching—a critical review of the biological aspects. Crit Rev Oral Biol Med. 2003;14(4):292-304.
3. Rotstein I, Zalkind M, Mor C, et al. In vitro efficacy of sodium perborate preparations used for intracoronal bleaching of discolored non-vital teeth. Endod Dent Traumatol. 1991;7(4):177-180.
4. Rotstein I, Mor C, Friedman S. Prognosis of intracoronal bleaching with sodium perborate preparation in vitro: 1-year study. J Endod. 1993;19(1): 10-12.
5. Heller D, Skriber J, Lin LM. Effect of intracoronal bleaching on external cervical root resorption. J Endod. 1992;18(4):145-148.
6. Holmstrup G, Palm AM, Lambjerg-Hansen H. Bleaching of discoloured root-filled teeth. Endod Dent Traumatol. 1988;4(5):197-201.
7. Deliperi S. Clinical evaluation of nonvital tooth whitening and composite resin restorations: Five-year results. Eur J Esthet Dent. 2008;3(2): 148-159.
8. Burrows S. A review of the efficacy of tooth bleaching. Dent Update. 2009;36(9):537-548.
About the Author
Stephen J. Chu, DMD, MSD, CDT
Adjunct Clinical Professor
Ashman Department of Periodontology and Implant Dentistry
Department of Prosthodontics
New York University
College of Dentistry
New York, New York