Economy Resin Rehabilitation
Matrix-driven direct resin rehabilitation
Michael J. Bannan, DDS, FAGD, AAACD
In the public health setting and in private practice, patients frequently present after years of neglect and deterioration of their dentition. There may be complex issues that include periodontal disease, caries, and occlusal instability that complicate the treatment-planning process. All too often, financial limitation is a primary obstacle to seeking treatment and limits clinicians’ ability to plan conservative, predictable treatment options.1
Teeth that might be restorable with full-coverage restorations often become default extractions because of cost considerations.2 Unfortunately, patients pay the ultimate price with long-term compromise of function and stability. If some key teeth can be saved and restored, the benefits to the patient in terms of health, function, and self-esteem can be significant. Sometimes, lives are changed and new hope helps people get their lives back on a more positive track. This is where dentistry can really make a difference.
This article describes a relatively low-cost, matrix-driven, direct resin technique3 used to restore two compromised dentitions: one compromised primarily by caries, the other addressing occlusal collapse. These dentitions belong to good people on a limited income who are dependent on government assistance to restore their health, function, and self-esteem.
Restorative Matrix Fabrication
Complex restorative cases require clinical decisions so that the operator can visualize the final positions of the restored teeth. The matrix concept has been used for many years and is based on dentofacial analysis, development of the diagnostic wax-up, fabrication of the matrix, and the subsequent management of the matrix and restorative materials.4-6
After a diagnostic wax-up is developed, it is blocked out with a putty spacer and a vacuum-formed stent is overlaid to develop a clear carrier tray (Figure 1). The tray is trimmed to the desired outline, and the block-out material is completely removed.
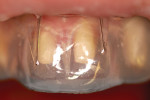
The clear tray is filled with clear polyvinyl siloxane (PVS) impression material and seated over the diagnostic wax-up to create an accurate registration that will serve as the restorative matrix.7 The clear tray/clear PVS combination yields a more rigid, accurate, and optically clear matrix than other techniques used by the author, although the result is more accurately described as translucent rather than clear (Figure 2).
The matrix is further modified in the areas of the teeth to be restored by making an entrance and exit hole to accommodate injection and venting of a flowable restorative material. The injection technique takes advantage of the hydraulic principle to ensure minimal flash at the cervical margin with a void-free fill as trapped air escapes the vent hole, allowing the restorative material to completely fill the matrix.
The injection technique has several advantages over seating a preloaded matrix. Preloading creates hydraulic resistance that can result in inaccurate or incomplete seating. It also results in more excess cervical flash as the restorative material seeks to vent itself apically. Additionally, preloading may cause voids where trapped air prevents material flow to completely fill the desired contours.
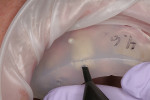
The injection hole should allow for a snug-fitting syringe tip of the restorative material. The author has found that a #6 round bur in a straight handpiece works well. The injection hole should be oriented toward the mesial aspect of the teeth to be restored for convenient delivery. The second vent hole is placed at a distal aspect of the restored segment. The location of the vent is less critical, but should be visualized when excess restorative material is expressed to signify that the injection process is complete (Figure 3).
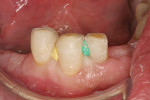
Prior to placement of the matrix, blocking out the open cervical embrasure can facilitate the ease of access for initial finishing and separation. Trimmed-to-fit wooden wedges (Figure 4) or a soft-tissue shield or dental dam can be employed.
Because the prepared teeth will be adhesively bonded, they need to be well isolated from blood and saliva. Preliminary treatment is usually indicated to address hopeless teeth, gingival inflammation, and rampant subgingival caries prior to this final bonded restorative procedure. Lip retractors combined with absorbent pads are very helpful along with adept four-handed suctioning.
Restorative Material Selection
The choice of restorative material is less clear. Ideal characteristics include:
• Low enough viscosity to hydraulically flow into small preparation features and completely fill the matrix without voids
• Ability to be adhesively bonded to tooth structure
• Dual-cure capability to reduce the risk of underpolymerized resin
• Good postoperative physical properties for wear and fracture resistance
• Esthetic optical properties to blend a single shade into an existing dentition
• Good surface polishability
• Resistance to recurrent caries
Traditional flowable resins lack the filler content and physical properties for long-term function. Bis-acryls have auto-cure capabilities, but are brittle and prone to fracture. Hybrid and nano-restorative composites have great esthetic and physical properties, but lack flowability. The author has found that using a composite heater improves flow for single teeth, but the composite cools and stiffens before multiple teeth can be injected.
One laboratory composite, Sinfony™ (3M, www.3m.com), has great flowability, physical properties, and esthetics. The manufacturer cites very high-density cross-linking, resulting in high compressive, flexural, and impact strengths and abrasion resistance.8 However, it lacks dual-cure capability and is designed to be used for indirect restorations, which also entail impressions, provisionals, return appointments, and additional laboratory costs that are not feasible in a low-fee environment. An “off-label” direct application of Sinfony is described in Case 1.
A relatively new “bioactive” direct resin restorative material, ACTIVA™ (Pulpdent, www.pulpdent.com), is, in the author’s opinion, the most ideal material to employ for this technique and is demonstrated in Case 2. The manufacturer reports that this material possesses the previously mentioned desired properties to act as a suitable injectable direct restorative.9-11
Curing and Finishing
Once the matrix is filled, it is held stable for extended intraoral light-curing. A concern with curing through the matrix is the inherent reduction in polymerization energy that reaches the hybrid layer. The matrix is translucent, not clear, filtering out some of the polymerization energy. More importantly, the light source is at an increased distance from the deeper hybridized surfaces, and light energy is reduced proportionally as the inverse of the distance squared.12
To offset this diminished energy, dual chairside LED light sources of approximately 1,500 mW/cm2 were bench tested for extended cure times of approximately 90 seconds per surface, curing from all accessible angles through the matrix. A hardness test on the intaglio surface of the restorative materials yielded sufficiently positive results to support innovative application with the matrix technique.
After maximal curing, the resin sprues from the injection and vent holes are ground down to facilitate matrix removal. The outer carrier tray is removed first, followed by the flexible inner PVS liner.
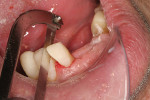
Initial gross finishing and separation of adjacent restorations is accomplished with an interproximal separator (Figure 5), various burs, disks and strips, according to personal preferences. The esthetics are refined and occlusion is adjusted as with any restorative technique.
Case Report 1
This is a case study of a severely damaged, worn occlusion that was restored on a limited budget with direct resin overlays and economy acrylic partial dentures. The restorative approach used matrix-driven direct resin overlays to a predetermined increased occlusal vertical dimension.
Patient History and Complaints
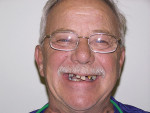
A 58-year-old Caucasian man presented with a chief complaint of “pus and tooth pain on the lower right.” He was very self-conscious about the appearance of his teeth and wanted them to look better and to improve his ability to chew. He stated that he knew his teeth were “jacked up” and wondered if he should just get complete dentures (Figure 6).
He reported that he had not seen a dentist in more than 30 years. He was on disability from chronic back pain, managed by the Veterans Administration Hospital, and had a limited budget, relying on Medicaid coverage to help with his treatment. Although his health history was significant, consultation with his physician indicated no contraindications to routine dental treatment.
Clinical Findings
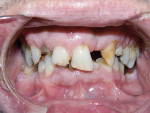
The initial oral and radiographic examination revealed localized periodontal disease, caries, several missing teeth with resultant drifting and three impacted third molars. There was evidence of prior endodontic treatment with poor prognosis, a symptomatic apical abscess on tooth No. 31, occlusal trauma, and severe occlusal mutilation resulting in a collapsed vertical dimension. He was an acknowledged bruxer. The mutilation and loss of vertical support presented a challenge to restore normal form and function (Figure 7).
Treatment Plan and Clinical Procedures
The ultimate decision was to treat the periodontal disease and restore the caries in teeth with favorable pulpal and biomechanical prognosis. Less-critical abutment teeth and those with endodontic or severe compromise (teeth Nos. 7, 23 through 25, and 31) were removed and would be replaced with economy acrylic partial dentures. Informed consent was obtained for the innovative application of a laboratory resin to restore his form and function with direct overlay procedures, and he would follow his treatment with an occlusal guard.
After this initial urgent phase of extractions and nonsurgical periodontal treatment had been completed, occlusal modifications and tooth preparations were accomplished with reference to preparation guides made from the diagnostic wax-up.
Total-etch bonding was completed with Ultra-Etch® (Ultradent, www.ultradent.com) and OptiBond™ Solo Plus (Kerr, www.kerrdental.com), and the restorative matrix was held securely while the restorative resin (Sinfony) was introduced into the injection hole until the excess was visualized from the vent hole. Prolonged light-curing from all angles, as previously discussed, was accomplished. After matrix removal, additional light-curing was completed to achieve the maximum polymerization.
Meticulous equilibration was completed to establish stable bilateral centric stops and limited anterior guidance with posterior disclusion in excursions. The increased vertical dimension and improved occlusal plane was evident in centric occlusion. The patient was then dismissed to “test drive” his new bite and improved smile. He returned approximately 3 weeks later reporting comfortable function and great satisfaction with his improved appearance. Upper and lower economy partial dentures were subsequently completed.
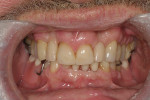
The patient reported that he was delighted with his new smile and was much more confident in his day-to-day social encounters. His biggest appreciation was for his new “bite.” He reported that his bite has never felt as balanced, solid, and comfortable as it did currently (Figure 8 and Figure 9). He declined proceeding with the occlusal guard because of cost. To date, the case has empirically demonstrated clinical success for more than 2 years with no adhesive failures, in spite of addressing adverse occlusal forces on an acknowledged bruxer who is less than ideally compliant.
Case Report 2
This case represents an attempt to help a teenager overcome an environment of neglect, low self-esteem, and drug abuse. A matrix-driven direct resin rehabilitation was undertaken, along with economy acrylic partial dentures.
Patient History and Complaints
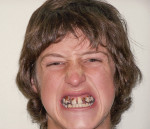
A 17-year-old Caucasian male presented with a chief complaint of generalized cold sensitivity and pain that progressed over the past 3 years. He was extremely self-conscious about the appearance of his teeth and spoke with his head down and his hand in front of his mouth (Figure 10). He had been recently admitted into the custody of a local county drug rehabilitation center for recovery assistance from years of neglect and drug abuse. In full-time custody, he was no longer abusing or currently taking any medication. His general health was not contributory.
Clinical Findings
The initial oral and radiographic examination revealed rampant decay and severe gingivitis. He had a class II malocclusion with severely malposed teeth, missing lower first molars, and resultant drifting and instability of lower second molars. All third molars were present and unerupted.
Treatment Plan and Clinical Procedures
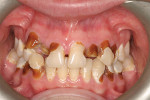
The patient presented as a huge caries control challenge (Figure 11). Many teeth appeared to be “unrestorable” without full-crown restorations. However, his custodial situation and lack of parental support made him reliant on government benefit reimbursement to pay for his dental care, and this would not cover ceramic crowns.
It was decided to initially proceed with caries excavation and placement of glass-ionomer restorative, GC Fuji IX GP® (GC America, www.gcamerica.com). Ultimately, teeth Nos. 2, 6, 7, 10, 15, and 28 were extracted due to biomechanical compromise. Additional caries control measures included patient education, diet counseling and modification, chlorhexidine gluconate 0.12% oral rinse, and a 1.1% sodium fluoride toothpaste, Colgate® PreviDent® 5000 Booster Plus (Colgate Professional, www.colgateprofessional.com).
Three months after the completion of this initial urgent phase of treatment, all deeply decayed teeth remained asymptomatic and tested vital. Laboratory mock-ups and restorative matrices were created to address more definitive function and esthetics.
Previously placed glass ionomers were left as a base and groups of teeth were prepared using the restorative matrix technique. After preparation, total-etch bonding was completed and the restorative matrix was positioned as previously described. The flowable dual-cure restorative (ACTIVA) was injected until it was seen extruding from the vent hole, indicating a complete fill. Prolonged light-curing was completed through the matrix, and the full auto-cure set time was monitored. Individual tooth contours were refined and the occlusion was carefully evaluated and adjusted as previously described.
This protocol was repeated over several subsequent appointments, until all of the required teeth had been restored and the occlusion had been verified. The patient was now very motivated to take good care of his teeth. Upper and lower acrylic partial dentures were fabricated and delivered to replace teeth Nos. 6, 7, 10, 19, 28, and 30.
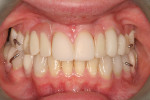
The patient was very pleased with his newly restored smile and indicated much more confidence when meeting and speaking with people. His caseworker reported that his self-esteem had improved immeasurably and he was engaging in conversations without hiding his mouth. The entire staff at the rehabilitation center agreed that he was not the same person he was several months ago (Figure 12 and Figure 13).
Rather than move toward the edentulation of this young man, aggressive caries control combined with appropriate materials and techniques helped get his life back on track. He is a changed individual with the confidence to move forward with his life.
Conclusion
As dental practitioners, we all encounter challenging situations where cost is an obstacle to restoring a debilitated mouth for a person we would really like to help. This article described an innovative restorative matrix technique to cost-effectively restore complex dental dilapidation. While this may not represent an idealized implant and ceramic-driven indirect rehabilitation, it does introduce an option that may allow patients to keep their dentition more intact. It is the author’s hope that these case reports will motivate clinicians to implement this matrix-driven, direct resin injection technique in those cases where it is an appropriate, cost-effective treatment option.
Disclosure
The author has no relevant financial relationships to disclose.
References
1. Oberlander J, White J. Public attitudes toward health care spending aren’t the problem; prices are. Health Aff (Millwood). 2009;28(5):1285-1293.
2. Neuman L. Land of confusion: Standardizing the standard of care. Inside Dentistry. 2008;4(9):126-138.
3. McLaren EA, Schoenbaum TR. The bonded functional esthetic prototype. Part 1. Inside Dentistry. 2013;9(1):70-.74
4. Lodding DW. Long-term esthetic provisional restorations in dentistry. Curr Opin Cosmet Dent. 1997;4:16-21.
5. Kois DE, Schmidt KK, Raigrodski AJ. Esthetic templates for complex restorative cases: rationale and management. J Esthet Restor Dent. 2008;20(4):239-248.
6. Malone M. Smile design and advanced provisional fabrication. Gen Dent. 2008;56(3):238-242.
7. McLaren EA. Bonded functional esthetic prototype: an alternative pre-treatment mock-up technique and cost-effective medium-term esthetic solution. Compend Contin Educ Dent. 2013;34(8):596-607.
8. 3M ESPE. Compilation of clinical studies. Available at: http://multimedia.3m.com/mws/media/131721O/sinfonytm-clinical-studies.pdf. Accessed October 26, 2016.
9. Slowikowski L, John S, Finkelman M, Kugel G. Fluoride ion release and recharge over time in three restoratives. J Dent Res. 2014;93(Spec Iss A):268.
10. Garcia-Godoy F, Morrow BR. Wear resistance of new ACTIVA compared to other restorative materials. J Dent Res. 2015;94(Spec Iss A):3522.
11. Christiansen GJ. When are Dual-Cure Restoratives Clinically Useful for Class I-VI? Clinicians Report. May 2015;8(5):1-4.
12. The inverse square law. Available at: http://physics.stackexchange.com.
About the Author
Michael J. Bannan, DDS, FAGD, AAACD
Private Practice
Raleigh, North Carolina
Wilmington, North Carolina