Narrow-Diameter Implants with LOCATOR® Attachments for Denture Stabilization
Hitting the target with careful treatment planning and optimal outcomes
Howard Hill may be the greatest archer to ever live. Newsreels from a time long forgotten capture Hill taking down some of the world’s most dangerous game using nothing but a bow and arrow. He could hit the center of the bulls-eye from nearly any distance and then split the arrow on his next shot. A winner of 196 consecutive archery tournaments, Hill was such a presence that other archers refused to compete against him, no one wanting to settle for no better than second.
I contend that any one of us could hit the center of the target better than Howard Hill could on the best day of his career, provided of course that he was first blindfolded and spun around a few times before he drew aim. You might find this scenario ridiculous, asking yourself, “How can someone hit a target they cannot see?” Here is a better question: “How can you hit a target that you do not have?”
In the ever-changing flux of treatment planning, identifying a targeted end result is the key to successful and desired outcomes. The best treatment outcomes happen when the patient’s needs and wants are met. Although this seems simple, it continues to be an ongoing challenge for most dentists. Our aging patients present unique needs that require us to treatment plan accordingly. In the case review described below, successful treatment was not just defined as treating the needs of an elderly woman, but listening to the desires of her family as well.
Case Presentation
An 88-year-old woman presented with a chief complaint that her dentures fit terribly and she could not eat well. She admitted that several years earlier she had declined implant treatment due to cost but had recently become aware of alternatives such as “mini-implants.” Her family was interested to know if she was a candidate for “mini-implants” because the patient was in early stages of Alzheimer’s disease and was becoming increasing forgetful of where she left her lower denture. In addition, the family had heard that implants also preserved bone. A clinical examination was performed that included taking standard and panoramic x-rays. A treatment plan was made with the patient’s fundamental desires and financial situation in mind. The plan was reviewed with the patient and her family and it was universally agreed upon that the best plan of action was denture stabilization using narrow-diameter implants.
Having identified the desired outcome, proper selection of an implant system became crucial to the overall design elements for the case. Historically, clinician’s choices were limited when employing the use of narrow-diameter implants to o-ball attachments. Although o-ball attachment style implants are functional systems, they have limitations. A few of the drawbacks are the need for constant changing of the o-ring, vertical height clearance requirements, and posterior lifting of the denture base.
The ZEST Anchors LOCATOR Overdenture Implant (LODI) System (www.zestanchors.com) was selected for three key reasons: thread design similar to standard implants, proven LOCATOR Attachment benefits, and ability to immediately load the implant with variable retention. In addition, the surgical kit is thoughtfully designed.
The most intimidating function of preparing any osteotomy is over-drilling. The LODI System provides the clinician with drill stop collars that slide over osteotomy burs, precisely limiting the depth to the desired length. This is a key feature. In my clinical experience, drill stops minimize fear and guesswork during the bone preparation of the osteotomy.
The patient presented with a narrow or knife-edged ridge. Standard protocols would require the surgeon to reflect an entire flap with vertical releasing incisions to flatten the ridge and create a more ideal ridge anatomy for implant placement. In the aging patient population, reducing morbidity is essential for two key reasons: less chance of infection and more patient comfort and acceptance. It is well documented that aging patients have a reduction in manual dexterity. Couple this normative age change with any presentation of Alzheimer’s disease and it becomes clear that conventional methods of surgery may expose the patient to a much greater risk of implant loss or infection. Provided there is an adequate zone of keratinized tissue, a closed reduction alveoloplasty of the ridge, specific for the sites of implant placement, is preferred and described below.
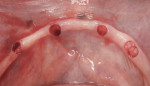
Larger than normal tissue punches were created for improved bone visualization using a 3-mm tissue punch (Figure 1). A ceramic round burr, size #6 (Komet, www.kometusa.com), was used with a surgical handpiece at 800 rpm. The widow’s peak of bone was flattened to create tabletop profile of the ridge and a more favorable shape. Subsequently, the initial form drill with drill-stop was used to prepare the osteotomies and the drill sequence was followed according to the manufacturer’s instructions.
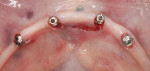
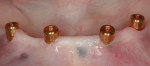
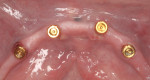
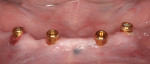
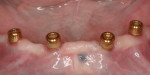
To maximize anteroposterior spread and retention, implants were placed in the cuspid and premolar positions bilaterally, along the lower arch (Figure 2). Care was taken to avoid any anatomical landmarks, staying at least 2 mm away from structures. In addition, each implant was placed ensuring there was 1 mm of bone facial-lingually around the implants for long-term viability. Each implant was inserted and the final placement torque measured at least 35 Ncm for all implants. Care was taken to be certain that each implant achieved excellent primary stability, as it is the key prerequisite of osseointegration. Furthermore, achieving robust primary stability is the determining factor in whether or not loading of the implants will take place at the initial placement appointment.
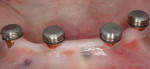
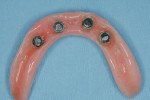
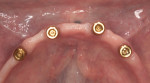
With all implants achieving torque values greater than 35 Ncm, the decision was made to pick up the LOCATOR Denture Caps into the denture base at the initial visit (Figure 3 through Figure 6). Care was taken to be sure of passive fit of the housings into the denture base prior to pick-up. This step was verified using a quick-set polyvinyl siloxane. Once passive fit was verified, the housings were cured in using a pink bisacrylic material. Adjustments were made after fit checking with pressure-indicating paste to relieve any pressure spots. Standard postoperative care instructions were reviewed and postoperative and recall appointments were scheduled.
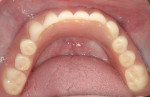
At 24-hour recall, the patient reported no pain or swelling (Figure 7 and Figure 8). Further follow-up at 2 months showed excellent stability of the implants and retention of the lower overdenture (Figure 9 and Figure 10). The patient and her family were thrilled with the life-changing results of a well thought-out and executed treatment plan.
Final Thought
The Greek biographer Plutarch stated, “What we achieve inwardly will change outer reality.” Identifying our target goals in treatment and having thoughtful and well-intentioned plans, coupled with utilizing proper tools and techniques, not only allows us to “hit the mark” in servicing our patients more consistently, but it allows us to change the outer reality of the world we exist in and improve our patients’ lives and well-being.
For more information, contact:
ZEST Anchors, LLC
800-262-2310
www.zestanchors.com
About the Author
Timothy M. Bizga, DDS
Private Practice
Parma, Ohio