Long-Term Stabilization and Retention of Mandibular Dentures
A simple approach for placing one-piece narrow-body implants
In 2002, a symposium held at McGill University in Montreal, Canada, used expert testimony, scientific evidence, and personal experience to affirm use of two implants in the anterior mandible to secure a complete denture.1 In 2009, a follow-up symposium in York, United Kingdom, reaffirmed the two-implant overdenture as the minimum standard for most people, taking into account performance, patient satisfaction, cost, and clinical time.2 The McGill review did not consider implants smaller than 3 mm in diameter because one-piece, narrow-body (“mini”) implants were indicated for provisional use only in 2002. Subsequent changes in design and prosthetic connection options expanded the use of one-piece, narrow-body implants for overdentures. Still, available data remained insufficient for consensus regarding minimum implant length and diameter for stabilizing and retaining a mandibular overdenture.
What had become clear is that flapless placement of narrow-body implants (1.8 to 2.8 mm diameter) in the anterior mandible simplifies placement for patients who are not candidates for traditional dental implant surgery.3,4 Traditional dental implants may not be an option for patients who lack sufficient ridge width to accommodate standard implants, those with compromised health that precludes more extensive surgical treatment, or those with financial limitations that prevents grafting and other procedures that would allow the use of standard implants.
Narrow-body implants are well suited for placement beneath mandibular dentures, as their axial form and one-piece design allow centering over the ridge crest between the mental foramina. One-piece construction assures adequate strength with a variety of prosthetic heads. Design criteria for the heads include wrench-lock placement and prosthetic attachment features. By 2004, at least three one-piece, small-diameter implant brands/styles were on the market. Manufacturers of all systems recommended four implants in the anterior mandible. The author purchased, completed hands-on training, and began using the following systems when patients were not candidates for traditional implants: ERA®/Micro (Sterngold, www.sterngold.com), IMTEC (now 3M ESPE, www.3mespe.com), and Atlas® (Dentatus, www.dentatususa.com).
Small-Diameter Protocol
Case selection and restorative protocol for denture stabilization using narrow-body Atlas implants has been described by Carpentieri and Tarnow.3 Facial-lingual ridge widths 4 mm or greater indicate flapless placement. After the mental foramina are identified, the most distal implant is positioned at least 7 mm anterior to each foramen to accommodate for the anterior loop of the mental nerve in some patients. Spaced entry sites should allow 4 to 5 mm between implants.
Each implant site is infiltrated with a small amount of local anesthetic before pilot openings are drilled with copious irrigation. Alignment of each osteotomy is confirmed, followed by implant placement with the manual driver. Finger pressure on either side of the ridge (Figure 1) is used to detect vibration suggesting close proximity or perforation of bone facially and lingually. Use of a finger on each side of the ridge also assists the practitioner in visualizing the trajectory of the mandible at the site being prepared. Final seating of the implant is completed slowly, turning the ratchet not more than one-quarter turn, waiting for bone expansion before continuing.
Because of its low prosthetic profile and simplified surgical placement, Atlas implants quickly emerged as the author’s preferred system. Requiring no metal housings, Atlas’s Tuf-Link retention silicone can be placed chairside or indirectly using analogs. The service life of Tuf-Link in the author’s practice has been 18 to 24 months, about the same as IMTEC’s O-rings, and at least twice as long as Micro ERA® retention elements. It’s arguably easier to replace O-rings and retention elements when a metal housing is present, although housings consume precious space and, in this author’s experience, weaken the denture base.
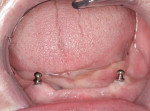
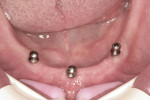
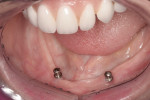
Although manufacturers advocate placement of four implants to secure mandibular dentures, that’s not always possible given recommended spacing intervals. With clinicians deviating from each manufacturer’s recommendations with increasing frequency, it was established that three, or even two, Atlas implants adequately support and retain mandibular dentures (Figure 2 and Figure 3). Clinical studies now support using two narrow-body implants beneath mandibular overdentures.5,6 Although one study suggests splinting when only two narrow-body implants are used, another study found no difference in bone level following integration with sustained function.6 Splinting is now an option with Anew® narrow-body implants using removable Elypse® prosthetic platforms (Dentatus), which include the option to transition from a removable to fixed restoration on the same implants.
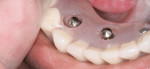
In the 10 years since the author’s first experience with Atlas implants, his preference is to place two or three implants flaplessly with copious irrigation during pilot drilling. Consistent with the McGill and York consensus statements, two narrow-body implants can reliably support and retain a mandibular denture to patient satisfaction.5-7 When the arch form of the mandible affords the possibility of an anterior-posterior spread, placement of three implants offers improved stability with better load distribution, although supporting evidence is anecdotal. Figures 4 through 6 show results observed 2 to 3 years after placement.
Final Thought
In conclusion, Atlas Implants—with Tuf-Link silicone hermetically sealed within the denture base without adhesives or bonding agents—provides retention and comfort, thus satisfying unhappy mandibular denture wearers whose initial complaint was denture lift-off or lateral displacement during function. Loading protocols vary according to quality of bone and biting force. When placement torque is below 35 Ncm, or whenever a patient’s musculature suggests parafunctional activity, the author’s preferred protocol includes progressive loading using a denture plastisol lining (COE-SOFT™, GC America, www.gcamerica.com) for 6 weeks, with scheduled replacement every 2 to 3 weeks. Early overload is guarded against by directly viewing each implant with the denture seated to confirm that there is no contact between the implant and acrylic denture base (Figure 7). The viewing windows should be closed with microwave-cured resin when processing the Tuf-Link silicone.
References
1. Feine JS, Carlsson GE, Awad MA, et al. The McGill consensus statement on overdentures. Mandibular two-implant overdentures as first choice standard of care for edentulous patients. Gerodontology. 2002;
19(1):3-4.
2. British Society for the Study of Prosthetic Dentistry. The York consensus on implant-supported overdentures. Eur J Prosthodont Restor Dent. 2009;17(4):164-165.
3. Carpentieri JR, Tarnow DP. Future considerations. In: The Mandibular Two-Implant Overdenture: First Choice Standard of Care for the Edentulous Complete Denture Patient. Mahwah, NJ: Montage Media; 2007:77-80.
4. Alternative techniques. American Academy of Implant Dentistry website. www.aaid-implant.org/dental-implant-options/alternative-techniques. Accessed April 7, 2014.
5. Jofre J, Hamada T, Nishimura M, Klattenhoff C. The effect of maximum bite force on marginal bone loss of mini-implants supporting a mandibular overdenture: a randomized controlled trial. Clin Oral Implants Res. 2010;21(2):243-249.
6. Jofre J, Hamada T, Nishimura M, Klattenhoff C. Effect of splinting mini-implants on marginal bone loss: a biomechanical model and clinical randomized study with mandibular overdentures. Int J Oral Maxillofac Implants. 2010;25(6):1137-1144.
7. Tomasi C (Department of Periodontology, Institute of Odontology, The Sahlgrenska Academy at University of Gothenburg, Gothenburg), Idmyr BO, Wennström JL. Patient satisfaction with mini-implant stabilized full dentures. A 1-year prospective study. J Oral Rehabil. 2013;40(7):526-534.
ABOUT THE AUTHOR
Nels Ewoldsen, DDS, MSD
Private Practice
Waveland, Indiana
For more information, contact:
Dentatus
800-323-3136
www.dentatususa.com