Restoring Implant Single Units: CAD/CAM Options
Technology creates more options for clinicians and labs alike
Traditional methods for the restoration of implants have been increasingly displaced by CAD/CAM technology with respect to abutments and crowns. In the past, with regard to both cemented or screw-retained implant restorations, a UCLA abutment was waxed to replicate a custom abutment or the screw-retained substructure and then cast. A traditional crown—typically porcelain fused to metal (PFM)—was fabricated; a coping was waxed and cast, and porcelain stacked and fired to complete the crown. When the screw-retained option was selected, the cast substructure would have porcelain fused to it to complete the restoration.
The first evolutionary step to marry CAD/CAM technology to implant restorations was virtual design of the abutment head, which was then milled from titanium. This provided a stronger, better fitting restoration to the implant and helped overcome some issues with cast abutments. Because they were fabricated from a gold-containing metal that had a lower melting point then the gold UCLA, cast abutments could fracture under load from the gold base below if the casting was too thin. As the milled titanium abutment is a single piece, there are no parts that can separate under loading. Additionally, titanium is a stronger metal than the gold-containing metals used for casting, which had the potential for deformation under load.
As the technology progressed in the realm of standard crown and bridge, various avenues were developed to scan either the prepared tooth in the mouth or the die fabricated from an impression. The first CAD/CAM-milled crowns were all ceramic, and eventually milling progressed to fabrication of milled metal copings, onto which porcelain would be applied. These metal copings were milled from either titanium or chrome cobalt, both of which can accept porcelain application. The CAD/CAM applications using ceramics provided a full milled crown, which was either fabricated from a ceramic that only required polishing and glazing or from a green (non-sintered) state that required firing to achieve the final strengths. As an alternative option, copings could also be milled and overlayed with porcelain.
In recent years, there has been a blending of these technology applications, wherein abutments can be CAD/CAM milled and crowns CAD/CAM fabricated to fit the custom abutment. This allows an abutment choice of titanium or zirconia as well as multiple options for the crowns that will sit on these abutments. These crown options include porcelain fused to titanium, porcelain fused to zirconia, and monolithic zirconia. Those practitioners who prefer screw-retained restorations have available several options, which include zirconia monolithic crown with a metal connector to the implant or porcelain fused to a milled zirconia or titanium substructure.
This article will review the different options available with regard to CAD/CAM for restoration of non-splinted implants in a single patient.
All-Ceramic Restorations
Ceramic restorations are being used more frequently than those with metal substructures due to the perceived esthetic benefits. Zirconia is quickly eclipsing metal as the preferred crown material due to the rising costs of gold; most labs report their numbers of zirconia restorations are increasing with a corresponding decrease in PFM restorations. We are also seeing increasing demand for zirconia abutments, which have esthetic benefits in the anterior, especially in those patients with thin biotypes where graying of the soft tissue may be noted, affecting esthetics. In the posterior, especially considering the higher loads due to mastication on the molars, zirconia abutments’ esthetic benefits may not outweigh the lower strengths seen at the connector. Additionally, due to the differences in material, a true frictional fit is not possible with a zirconia connector in a titanium implant and fretting wear may be observed at the mated surfaces. Fretting wear is defined as the micro-wear that occurs between two dissimilar materials under function. As zirconia is harder then titanium, after a period of loading, small black specks can be observed on the zirconia connector when the parts are separated, demonstrating wear of the titanium surface. Over time, this will lead to increasing micro-motion, a sloppier fit, and potentially a loose restoration. For this reason, if a zirconia abutment is planned, it is recommended that a titanium insert be the mating surface with the implant connector, to which the zirconia abutment is then luted. This applies to both abutments that will accept a cemented crown and also screw-retained restorations.
The all-ceramic options available include a zirconia abutment with a cemented all-ceramic crown, a titanium milled abutment with a luted ceramic crown, a zirconia substructure upon which porcelain has been layered, and a monolithic screw-retained zirconia restoration.
Currently, the all-zirconia restorations available are well suited to the posterior but due to their higher opacity compared to layered ceramics with a zirconia substructure/coping, they may not be suitable in the anterior where higher esthetics are demanded. Clinicians often have to weigh esthetics with load handling, especially in patients who may be bruxers or have other parafunctional habits. After milling, monolithic zirconia in the green state is stained and tinted prior to firing, which helps it achieve its final high strength. The tinting (coloration) can be applied to either the zirconia abutment or to the crown itself to allow better natural blending.
Green state zirconia is formed into disks that can be used in a CNC milling machine and are manufactured by using a spray-dried zirconia powder that is then isostatically pressed and incompletely sintered. CAD/CAM milling is then performed. This green state material remains softer than the sintered zirconia and is easier and faster to mill. After milling is completed, the green state zirconia is then sintered completely in a furnace at l,350°C to 1,500°C to achieve its final shape, strength, and physical properties. Because sintered zirconia is so hard, trimming and contouring after sintering should be kept to a minimum, though occlusal adjustments can be made.1
The flexural strength of zirconia oxide materials is reported to range from 900 to 1,100 MPa, which is approximately twice as strong as other ceramics such as alumina oxide and five times greater than standard glass ceramics.2 Fracture toughness of zirconia is between 8 and 10 MPa, which is twice that of aluminum oxide ceramics.3,4 These properties provide a durable tooth-colored material that functions well as an abutment, screw retained or cemented restoration, or coping for porcelain application.
In clinical situations where esthetics is more critical, porcelain can be layered onto the zirconia. As porcelain does not “fuse” to the underlying zirconia, since the melting point of zirconia is considerably higher than porcelain, it is micromechanically bonded to the zirconia. With this in mind, restorations can be designed wherein the porcelain overlay is only in the esthetically visible areas and occlusal contacts may be placed on zirconia only. This may be considered in situations where clearance is insufficient for full porcelain overlay or the patient has parafunctional habits that may lead to fracture of overlaying porcelain.
Ceramics 2in1 (Biodenta, www.biodenta.com) is a unique, a low-melting porcelain that can be used for ceramic veneering and characterization of framework materials of sintered zirconia, titanium, and titanium alloys. This leucite-free dental ceramic is characterized by a very high stability of thermal expansion coefficient. Resulting from the lack of leucite crystals, the stable thermal expansion coefficient allows for stability even after multiple firings and ensures stabilized processing on both titanium and zirconia substructures. This layering ceramic also shows very good chemical resistance and thus high biocompatibility.
One difficulty with fusing porcelain to titanium is graying. An oxide layer forms on the metal surface and darkens when placed in the oven prior to application of a ceramic. The unique microstructure of a titanium opaquer, however, causes a sealing of the titanium surface, prevents ceramic graying, and establishes a reliable bond between metal and ceramics. The use of an additional bonder can be omitted.
PFM Restorations
Traditionally, PFM restorations involved waxing and casting of a nonprecious, semi-precious, or precious metal coping, upon which ceramics were then layered and fired. These provided reasonable esthetics in the anterior when sufficient reduction was performed on the prepared tooth to allow the lab technician to layer porcelain over the coping. Final esthetics depended upon the skill and technique of the lab, and generally involved building in nuances with 2 to 3 different shades of porcelain and finishing with surface stain to achieve more natural esthetics. Restoration of implants followed the same techniques, but due to concerns about dissimilar metals being used for the restorations coping/abutment and the implant, attempts were made to cast titanium copings. This was fraught with two main issues: difficulty in casting titanium and the previously mentioned graying that occurs when porcelain is layered over titanium. Besides the esthetic issues, the oxide layer produced on titanium is considered to have a potentially adverse effect on titanium-porcelain bonding.5 This has been addressed with newer porcelain formulations and surface materials, which prevent oxide formation by locking out the oxygen that reacts with the titanium’s surface. Additionally, bonding liquids have shown to improve bond strength of the porcelain to the titanium, yielding a stronger more durable restoration.6,7 Titanium (unalloyed) differs in two aspects from those metals used in casting, as it has a phase transformation at 882°C that changes its properties and has a thermal expansion coefficient that lies between that of the porcelain types available on the market. Due to the difficulty of casting titanium, alternative methods of shaping the metal, such as milling, spark erosion, and laser welding, were introduced. This was to avoid the phase transformation seen during casting.
Using three-point bending tests, bond strengths between different porcelains and metal alloys/titanium have been compared by examining different brands, types of processing of the titanium surface, different compositions of the porcelain, and different firing conditions. Generally it was found that the bond strength between porcelain and titanium was lower than with alloys.8
CAD/CAM milling has permitted the technician to bypass the issues found with casting titanium. As previously discussed, this permits fabrication of custom metal abutments as well as copings or screw-retained substructures for porcelain application (Figure 1). As with milling zirconia, multiple restorations are simultaneously milled from a block, with the individual restorations “nested” in the block to maximize usage of the entire block.
Single Fixture Prosthetic Options
Cementable Options
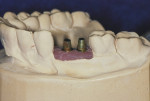
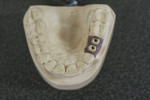
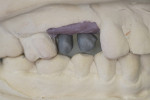
Those practitioners who prefer cemented restorations have multiple options available today. Stock abutments (prefabricated) may be placed into the implants intraorally or on a soft tissue model fabricated from an impression of the implants intraorally (Figure 2). These can be modified either at the lab or, if necessary, intraorally by the practitioner, and then either a monolithic zirconia, porcelain-fused-to-zirconia, or PFM crown can be fabricated to fit the abutment.
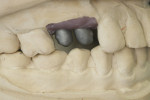
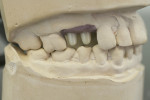
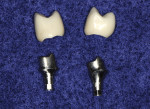
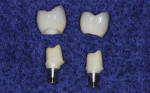
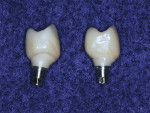
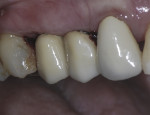
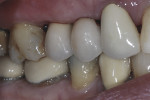
In certain clinical situations, or at the preference of the practitioner, a CAD/CAM-milled custom abutment can be fabricated. If esthetics is not critical and an all-ceramic restoration is desired, a monolithic zirconia crown can be milled to fit the abutment. When an improved esthetic is desired, a coping can be milled to fit the CAD/CAM-milled abutment and a porcelain overlay can be layered to develop the esthetics and contours needed (Figure 3 through Figure 6).
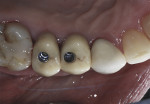
When restoring a case with high occlusal loading, CAD/CAM-milled abutments are selected when there is concern that a zirconia abutment may not withstand parafunction. These abutments may receive an all-ceramic crown (Figure 7) or a PFM depending on the practitioners’ preferences.
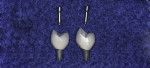
Some clinical situations may require the use of a non-metallic abutment due to thin gingival tissue and the resulting graying that may occur with metal abutments in those cases (Figure 8). The crown option in those situations, where esthetics is critical, would be a CAD/CAM-milled zirconia coping to which porcelain would be fused for development of contour and esthetics (Figure 9 and Figure 10). As previously discussed with regard to all-ceramic options, monolithic zirconia or a zirconia coping with layered porcelain may be selected. Monolithic zirconia by its nature tends to be more opaque then layered porcelain and may not be suitable in all situations.
Screw-Retained Options
With monolithic zirconia single-unit crowns, a titanium metal connector is used between the implant fixture and restoration to eliminate the potential for fretting wear. These monolithic zirconia restorations are very durable and have no overlaying ceramic that could potentially chip under function. Yet they tend to be more visually opaque than a layered all-ceramic restoration and may not be suitable in the anterior or for very esthetically conscious patients (Figure 11 and Figure 12).
The standard prosthetic option with screw-retained implant restorations still remains a metal substructure with overlaying porcelain. As discussed, the substructure may be milled from titanium and shaped to best support the overlaying ceramic (Figure 13 and Figure 14) and porcelain is then layered to full contour. The resulting restoration allows easy retrieval if required and provides natural-looking esthetics (Figure 15 through Figure 17).
Conclusion
Multiple options exist when restoring single implant fixtures that utilize CAD/CAM technology. This technology allows fabrication of a zirconia or titanium abutment and a cemented crown with monolithic zirconia or a coping milled from zirconia or titanium with overlayering of porcelain. When a screw-retained option is desired, one can mill a monolithic zirconia crown or a zirconia or titanium substructure upon which porcelain can be layered for improved esthetics. The options for improved form and function are limitless with the benefits of CAD/CAM milling.
Disclosure
The author received an honorarium from Biodenta; laboratory work presented in this article was fabricated by Biodenta using their CAD/CAM CNC machines and material.
References
1. Parker, RM. Use of zirconia in restorative dentistry. Dent Today. 2007;26(3):114-119.
2. White SN, Miklus VG, McLaren EA, et al. Flexural strength of a layered zirconia and porcelain dental all-ceramic system. J Prosthet Dent. 2005;94(2):125-131.
3. Evans AG. Perspective on the development high-toughness ceramics. J Am Gerem Soc. 1990;73:
187-206.
4. Mclaren EA, Giordano RA II. Zirconiabased ceramics: material properties, esthetics, and layering of a new veneering porcelain, VM9. Quintessence. 2005;28:99-111.
5. Atsü S, Berksun S. Bond strength of three porcelains to two forms of titanium using two firing atmospheres. J Prosthet Dent. 2000;84(5):567-574.
6. Gilbert JL, Covey DA, Lautenschlager EP. Bond characteristics of porcelain fused to milled titanium. Dent Mater. 1994;10(2):134-140.
7. Haag P, Nilner K. Bonding between titanium and dental porcelain: a systematic review. Acta Odontol Scand. 2010;68(3):154-164.
8. Haag P. Porcelain veneering of titanium--clinical and technical aspects. Swed Dent J Suppl. 2011;(217):11-75.
About the Author
Gregori M. Kurtzman, DDS, MAGD, FACD, DICOI
Private Practice
Silver Spring, Maryland