Sealants and Fluoride Varnishes
Two effective weapons in the fight against caries
Although fluoride in water and toothpaste has dramatically lowered the rate of caries in the United States, the effectiveness of fluoride from those sources in terms of preventing caries is said to be largely limited to interproximal tooth surfaces. A more comprehensive approach to caries prevention may necessitate the additional use of more concentrated, professionally applied fluoride in varnish form. In some cases, sealants will need to be used on the pits and fissures of occlusal and buccal/lingual surfaces, which resist effective hygiene as well as fluoride treatment.
Fluoride Varnishes
Fluoride varnish is cleared for marketing by the U.S. Food and Drug Administration (FDA) for the treatment of dentin hypersensitivity associated with the exposure of root surfaces or as a cavity varnish, but it is not officially cleared for reducing caries. However, in keeping with a growing body of evidence supporting its use for caries prevention, it has been endorsed by the American Dental Association (ADA) for caries prevention.1 In fact, the ADA Council on Scientific Affairs position paper called fluoride varnish “the safest and most efficient fluoride delivery system for children.”1
Fluoride varnishes, which typically contain 5% sodium fluoride, can be applied to the enamel, dentin, or cementum of the tooth as an adjunct to other forms of fluoride treatment. These alcohol- and resin-based preparations, which must be applied by a healthcare professional, are not permanent varnishes, but their adhesive consistency enables them to remain in contact with tooth surfaces for a period of several hours, delivering a highly concentrated temporary dose of fluoride for a longer amount of time than other concentrated fluoride products.2
Varnishes are available in different flavors for young patients and do not have the bitter taste of some fluoride gels; there is no need for the use of fluoride trays, which can induce gagging.
Patients should be made aware that the color and characteristics of the material may temporarily discolor teeth and/or fillings, but will fade as the varnish is gradually removed by eating and brushing.
Application Procedure
Although professional prophylaxis is not necessary prior to application, teeth should be brushed or otherwise cleared of heavy plaque or debris. They should then be lightly dried with air or a cotton gauze and isolated with a dental dam or absorbent material. The varnish—which will set on contact, even in the presence of saliva—should be applied to each tooth surface with a small brush or applicator.
The patient should refrain from eating, drinking, or rinsing for the amount of time specified in manufacturer’s directions. Normal oral hygiene procedures can resume the following day.
Sealants
Dental sealants provide a different form of preventive care. Composed of a plastic material, they are applied to pits and fissures of occlusal and buccal/lingual surfaces of teeth to act as a shield to prevent food from becoming trapped and to arrest demineralization. With proper application, and provided that the sealant stays in tact, it can protect teeth from decay for years.3
The success of this treatment hinges on the correct identification of at-risk teeth as well as achieving long-term retention. Although occlusal surfaces typically retain the properly selected and applied sealant, achieving retention on buccal and lingual pits and fissures of molars is generally more problematic.4 In addition, challenges are posed by how to handle teeth on which it is difficult to achieve good sealant retention, including partially erupted permanent first molars, second molars, and partially erupted premolars.
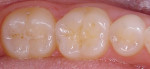
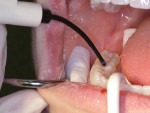
To determine which teeth are appropriate for sealant application, the practitioner should examine the thoroughly dried occlusal surface of permanent molars and premolars using a dental mirror and explorer to confirm the presence of deep occlusal pits and fissures (Figure 1).
Note that although it is possible to unknowingly seal over active or incipient carious lesions on the occlusal surface, there is no evidence to show that this negatively impacts caries progression.
Clinical Technique
If possible, the sealant should be applied before teeth have a chance to decay, using the method described below.5 This technique can be used immediately after the teeth have erupted, which is generally at approximately age 6 years.
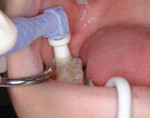
Cleaning—Teeth are first isolated with a dental dam or absorbent and occlusal surfaces are cleaned with a non-fluoride pumice prophylaxis paste or an air abrasion device (Figure 2). Teeth are then thoroughly rinsed with an air-water spray and dried.
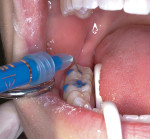
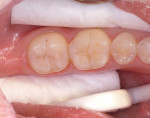
Etching—The tooth is then etched for 15 to 30 seconds with a phosphoric acid etchant (Figure 3). The etchant is thoroughly rinsed with either a water spray or an air-water spray for 10 seconds, after which surfaces are completely dried. The enamel surface will have a dull, frosted appearance (Figure 4).
Application—Using either an applicator tip or a brush type applicator, the sealant is applied to the occlusal surfaces, covering all pits and fissures and extending onto the cusp ridges (Figure 5). The final sealant thickness upon application should be at least 0.3 mm.
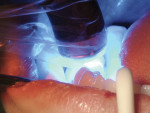
Light Cure—If this method is used, the device must provide enough energy to light cure the resin sealant. To be effective, the light should be 600 mW/cm2 from the tip, held within 1 mm of the occlusal surface, and positioned at right angles to the tooth surface being light cured. The tooth being sealed should be light cured for at least 10 seconds (Figure 6).
Sealant Evaluation—The sealant is evaluated for retention and seal of the occlusal surfaces. Sealants should also be checked at each regular dental appointment and can be reapplied if they are no longer in place.
Sealant Failure
Table 1 lists factors that may lead to early sealant failure, which include issues surrounding application, the appropriateness of the treatment, patient behavior, and more.5 Even under the best of circumstances, a 5% to 10% per year loss of the sealant is to be expected, with a resulting loss of effectiveness.4 It is therefore important to reevaluate teeth with sealants on a periodic basis and to reapply if necessary. Failure to maintain sealants can make previously treated pits and fissures again susceptible to bacterial invasion.
When sealants require repair or reapplication, the technique described for initial sealant placement should be used. It may be necessary to treat at-risk teeth for which sealants are not successful with more invasive preparations or restorations.
Sealants and Varnishes Together
Just as fluoride treatments alone may be unable to protect occlusal surfaces, dental sealants do not eliminate the need for fluoride treatment. Sealants and fluorides can work together to prevent tooth decay.
References
1. American Dental Association Council on Scientific Affairs. Professionally applied topical fluoride: evidence-based clinical recommendations. J Am Dent Assoc. 2006;137(8):1151-1159.
2. Collins FM. The development and utilization of fluoride varnish. www.ineedce.com website. www.ineedce.com/courses/2093/PDF/1106cei_varnish_web4.pdf. Accessed August 23, 2013.
3. American Dental Association. Sealants. Mouth Healthy website. www.mouthhealthy.org/en/az-topics/s/sealants. Accessed August 23, 2013.
4. Feigal RJ. Sealants and preventive restorations: review of effectiveness and clinical changes for improvement. Pediatr Dent. 1998;20(2):85-92.
5. Strassler HE, Grebosky M, Porter J, Arroyo J. Success With Pit and Fissure Sealants. Dentistry Today website. www.dentistrytoday.com/ce-articles/351. Accessed August 24, 2013.