Principles of Smile Design
Documentation, assessment, and communication are key
Dentists are challenged to improve the smiles of patients who present with a multitude of variations in facial, labial, and dental characteristics. To best ascertain a treatment plan that will restore a smile to its ideal form for each individual, the principles of smile design are evaluated independently and together. Dentists are expected to present treatment options and verbalize potential compromises, ultimately providing sound dentistry and improving smiles.
Patients present with their own personal goals for their teeth and facial esthetics, as well as their own dental concerns, making proper treatment planning even more challenging.1 The prosthetic implications of smile design principles are numerous and vary depending on each unique situation. Techniques can be implemented to reduce the risk of unexpected outcomes.2,3 If more time is spent by the dentist on analysis of smile principles during treatment planning, the risk of encountering unexpected outcomes is minimized for the dentist and patient.
Smile Design Protocol
New Patient Interview
New patient interviews are the dentist’s opportunity to get acquainted with the patients’ medical and dental histories, as well as acquire more details about the desire for a new smile.4 Care can be taken to ask meaningful questions that encourage patients to reflect on the reason for making the dental appointment.
During this first appointment, patients may seem to be or may express being nervous about seeking treatment; patients may have dental fears, may have multiple concerns about the well-being of their mouths, or may have concerns regarding the cost of potential treatment. It is important not to speed through any conversation, nor begin evaluating the mouth too soon. Much can be learned about patients and their smiles by simply watching them speak and observing their mannerisms.
It is important that patients be aware of and comfortable with their reasons for being in the office. The decision to have a smile improved is an emotional one that will have been made by patients before the appointment is scheduled. It is possible to learn more about our patients and create strong emotional connections with them by asking the right questions, which can include “When did you first notice this problem?”; “What were you doing when you noticed this problem?”; or “What made you decide to improve your smile?” The answers are usually emotional, such as “My grandson told me that my teeth looked yellow,” or “Looking at a picture I took with friends who have nice teeth.” To understand patients’ emotionally-based reasons for seeking an improved smile, dental practitioners need to ask emotional follow-up questions, such as “How did that make you feel?” or “How did that affect you?” This can serve as the beginning of a conversation that will reveal more about patients’ desires for a new smile and healthy mouth.5
Pretreatment Photography
After patient interviews, photographs can be taken and shared with patients to help them explain where they would like improvements made and to facilitate communication of smile principles. Using digital images to communicate this information is often more informative and objective than using a hand mirror.
Typical photos taken of a new patient will vary depending on individual concerns, but should always include a headshot, a 1:2 frontal smile, and a 1:2 retracted smile with upper and lower teeth slightly apart, allowing visualization of incisal edges, gingival margins, tooth wear, and/or crowding. Other photos may include occlusal shots, profile, lip at rest and teeth together, or lateral shots. A portrait studio can be used to obtain full-face images to facilitate patient communication, and video can be taken for further study of facial analysis and dentolabial relationships.6 Images must be taken at the proper angles and magnifications to be diagnostic. Photos taken at improper angles to the teeth will provide false information regarding principles such as incisal and occlusal plane, and can negatively affect treatment planning.
Physical Examination
Information gathered during the interview and from photography should be combined with more detailed information collected during a formal examination that includes intra- and extraoral examination, periodontal analysis, oral cancer screening, and temporomandibular joint (TMJ) and occlusal examination.7,8 Diagnostic records that include accurate upper and lower polyvinyl impressions and correct occlusal analysis are combined with a face-bow for mounting models.9,10
When planning esthetic dentistry, it is wise to begin treatment with centric relation bite registrations to idealize the function of the new restorations and to provide the opportunity to correct occlusal disharmony that can lead to early failure of the natural teeth and restorations. The goal is to optimize function, provide muscle comfort, minimize load in the TMJ, and control load in the teeth. The purpose of the face-bow is to correlate the occlusal plane with the upper dental arch in the cranial fixed plane, such that the correlation may be transferred to the articular.9 It is necessary to position a face-bow on a correct occlusal and incisal plane to guide the fabrication of the future restorations and to ensure that an accurate representation of the existing condition of the mouth is obtained.
Communication of Treatment Options
Treatment options should be presented carefully and thoroughly, taking care to fully explain both positive and negative aspects related to potential outcomes. Ultimately, the least amount of dentistry that can be performed to fulfill patients’ expectations for a healthy mouth and improved smile is the best course of action in every situation.11
Any potential compromises to ideal smile situations of perfect symmetry or violations to principles of smile design should be shared with patients. Alternative treatment plans, including involvement of other dental specialties, must also be presented as options for treatment. A consent form must be signed once patients have committed to treatment. Medical and dental records should be reviewed by the dentist so that he or she can fully understand the patient’s individual facial esthetic and dentolabial relationship in the context of dental smile design principles.
Impact of Facial Planes on Smile Design
When evaluating facial esthetics, the horizontal and vertical facial planes should be studied to determine how they influence the design of the smile. It is not uncommon for this evaluation to be limited by the need to use the interpupillary line, which is often not level with the horizon, as a horizontal reference. Before designing the smile, it is necessary to evaluate other horizontal reference planes, as they may impact the treatment plan for an improved result. Other horizontal reference planes include the commissural line and ophraic line. Patients present with a number of facial plane variations, including horizontal planes that are all parallel with the horizon; facial planes that are parallel with each other, but not the horizon; and facial planes that are parallel with neither the horizon nor each other.
The vertical facial plane line is drawn through the glabella, tip of the nose, and center of the chin. The most esthetic line is drawn 90° to horizontal planes that are parallel with the horizon.7 Vertical lines are often seen that are not perpendicular to the horizon; however, with few exceptions, the smile should be planned with the interdental line perpendicular to the horizon, regardless of variations in the patient’s facial vertical plane, for when this is not the case, it is readily noticed as irregular by the casual observer.7
Facial smile design principles can have dramatic implications in case planning, as illustrated by the following case.
Case 1
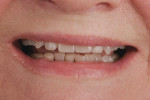
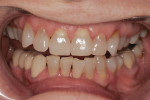
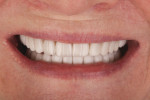
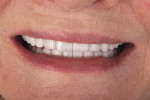
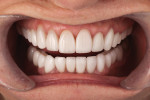
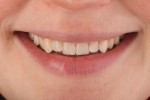
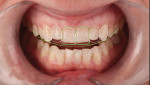
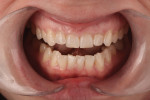
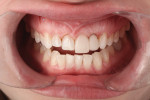
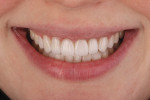
A patient who desired an improved smile presented with an ophraic line, interpupillary line, and commissural line that were parallel with each other; none was parallel with the horizon. The vertical midline was also not perpendicular to the horizon (Figure 1). Her goal was to have a brighter smile and show more teeth when she smiled (Figure 2 and Figure 3). It is not uncommon for patients to present to the dental office with facial variations such as these, and careful planning of the smile design is necessary to achieve facial harmony and patient approval. It is important to fully inform the patient of the variations that are seen in the face and discuss how this will contribute to the overall design of the smile so that all patient concerns may be addressed before the restorations are seated.
In this case, a decision needed to be made whether to follow the canted facial planes for the future smile line or follow the horizon, as is ideal. If a patient presents with several facial deviations from ideal esthetics, the best solution may be to provide a smile line that is parallel with the horizon, and not contribute to the less esthetic existing facial plane variations. In other words, correct smile principles should be applied.
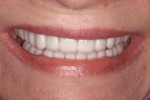
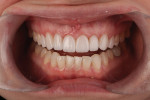
However, in this case, the creation of a smile line that was parallel to the horizon ultimately led to the creation of a facial disharmony that was noticed by the patient. The patient was not properly informed about the existing condition of her facial planes and how their positioning would affect her smile. The finished result revealed a corrected incisal plane, but the patient was displeased with the overall effect of the lengthening of her teeth, and did not like that she was able to see more teeth on the right side of her smile than on the left (Figure 4 and Figure 5). Details are usually worked out in the provisional restorations; however, the operator evaluated the smile design principle in provisionals and determined that the smile was improved from its preoperative condition. The patient did not mention a concern in provisionals. If the design had been more carefully critiqued preoperatively, potential concerns could have been better managed in ceramics.
The solution was to shorten the right side by 1 mm and create a mock-up of left-side teeth No. 10, No. 11, No. 12, and No. 13 that was 1 mm longer than the patient’s teeth (while remaining within functional limitations) using flowable composite; this resulted in less tooth length showing on the right side and more tooth length showing on the left side at full smile (Figure 6). After patient approval, an impression of the intraoral mock-up was created and used as a temporary matrix, and the corresponding IPS e.max® (Ivoclar Vivadent Inc., www.ivoclarvivadent.us) restorations on the left side were cut off and remade at the new lengths. An impression of the provisional restorations was sent to the laboratory with the master impression to assist the laboratory technician in fabricating the new IPS e.max veneers (Gold Dust Dental Lab, www.golddustdental.com). Harmony was restored to the patient’s face, and she was ultimately much happier with her new smile (Figure 7 through Figure 9).
Impact of Dentolabial Relationships
Once facial esthetics are analyzed, the practitioner can evaluate dentolabial relationships. Dentolabial analysis is a dynamic analysis of the way the teeth interact with the lips and face. The parameters of dentolabial analysis include lip at rest, incisal curve versus lower lip, smile line, smile width, labial corridor, upper incisal line versus midline, and occlusal plane versus commissural plane/horizon.7
These parameters are based on lip movements and are easiest to analyze in person and when evaluating video recordings of movement. Frequently, patients who are asked to smile or hold rest positions for photos are providing false information for smile analysis, recorded as a snapshot in time. For example, the author has recordings of patient conversations in which the patient’s natural horizontal head position changes throughout the course of the conversation. Evaluation of movement enables practitioners to watch patients talk and react naturally. These recordings can be paused and evaluated in greater detail. Once information is gathered regarding the relationship between the lips and teeth, the teeth alone can be evaluated.
Tooth and gingival analysis should be performed independently of lip and face analysis, and should include a study of maxillary and mandibular interincisal lines; tooth shapes; micro- and macrotextures; and tooth contours, proportions, and angulations.7 Occlusal relationships should be referenced and incisal and canine guidance determined.10 Maxillary incisal edge positions, as well as tooth width-to-height ratios, are very important to analyze first in smile design. Incisal edge position is analyzed based on esthetic and phonetic parameters. Normal ranges of tooth width-to-height ratios of maxillary central incisors can vary from 75% to 85%. It is the author’s opinion that the two most important characteristics of a beautiful smile are central dominance and radiating symmetry, where the incisal line follows the curve of the lower lip while smiling. Alterations to the form of the maxillary incisors to create length or width changes that are in violation of central dominance will have a negative and unnatural impact on the outcome of the smile. There is greater potential for this to occur when designing smiles in which tooth arrangements are crowded or have excess spacing or the patient has an inadequate arch and/or teeth with nonideal width-to-length ratios; however, this can also occur when making gingival modifications to improve the smile.7 It is important to evaluate all aspects of smile principles, but proper emphasis should be placed on central dominance and radiating symmetry.
Case 2
A patient presented with a main concern of wanting whiter, larger teeth and canines that were less pointy. Evaluation of dentolabial, tooth, and gingival smile design principles revealed that the patient’s smile lacked central dominance and radiating symmetry. Her preoperative central width-to-height ratio was close to 100% and she had a reverse smile (ie, a concave rather than convex smile line that did not follow the lower lip). Some of her teeth where tipped lingually in the arch, creating a deflective smile, which often makes teeth look smaller and darker. Her gingival margins lacked symmetry and gingival heights needed improvement to be closer to ideal form (Figure 10 through Figure 12).
Proper planning for length changes was executed with digital smile design techniques using keynote and constrained proportions to measure actual tooth width-to-height ratios compared with more ideal ratios.12 A final length of central incisor was determined that would result in a change of proportion from 97% to 76% (Figure 13). Although short and worn teeth age and masculinize the smile, teeth that are too long and narrow look unnatural and distract from central dominance.
The final proportion change was used to measure length changes in a gingival and incisal direction. It is critical that this information be gathered before completing gingival length changes, creating an intraoral mock-up and ordering a laboratory wax-up.13 It is beneficial to create intraoral mock-ups before ordering laboratory wax-ups to provide diagnostic information to the laboratory so that the most accurate and useful wax-up can be created. This can be especially important for teeth that are deflective to help with proper positioning of the teeth in a labial-lingual direction (Figure 14). The wax-up assists the dentist with preparation design and enables the most conservative preparation possible for the patient. Use of an accurate wax-up also permits the creation of provisional restorations that require fewer adjustments to achieve dentist and patient satisfaction.
Treatment planning for the case revealed that the gingival margin of the right lateral incisor No. 7 would remain in a slightly apical position compared with the other incisors; however, the gingival and incisal length of the centrals were measured to maintain proper proportions before closed-flap osseous gingival contouring was completed. Had the gingival contour of the other maxillary incisors been raised based on the height of the right lateral incisor without proper treatment planning, a plan would need to have been determined at the end of treatment to create narrow central incisors and lose central dominance, or create a flat smile line. Obtaining this information allowed for a discussion of orthodontics before initiating treatment, giving the patient the opportunity to decline orthodontics as a treatment option.
The results of the case show that careful treatment planning was executed in the provisionals and carried through to the final ceramics. Although incisor No. 7 remained at a slightly apical position to the other maxillary incisors, central dominance and radiating symmetry were restored to the smile (Figure 15 through 17). The smile was functionally finished with application of direct veneer bonding to the lower canines to provide for immediate canine rise in lateral excursions. The bonding procedure was performed with the aid of a matrix fabricated from a laboratory wax-up that required very little adjustment for proper occlusion.
It is important not only to take patient photos before initiating treatment to assist in planning and communication, but also to continue to take photos during the course of treatment and postoperatively. During postoperative appointments, full-face, smile, and intraoral photos can be taken and video can be recorded, which can be used to celebrate the results with the patient and evaluate the results in more detail. In the treatment room, the occlusion can be further refined by recording and adjusting centric and all excursive movements, as well as by using T-Scan® (BioResearch, www.bioresearchinc.com) to balance the bite and ensure that restorations have proper contact forces and timing. Radiographs taken during seating can be further evaluated and photos can be retaken as needed to complete postoperative records.
Final Thought
Proper treatment planning in these cases included careful analysis of several principles of smile design. It is important to review these principles for potential compromises to final results and verbalize these principles to the patient before preparation and provisionalization of the teeth.14 This type of communication allows the dentist to maintain control of the case, prevent costly remakes, and ensure patient satisfaction. Ultimately, a smile that is in harmony with the face may not successfully fulfill every smile design principle, but, with proper treatment planning and patient communication, balance can be achieved in creating a beautiful smile.
References
1. Tripodakis AP. Dental esthetics: oral personality and visual perception. Quintessence Int. 1987;18(6):405-418.
2. Feeley RT. Cosmetics and the esthetic patient and laboratory communication. Oral Health. 1995;85(8):9-12, 14.
3. Kokich VO Jr, Kiyak HA, Shapiro PA. Comparing the perception of dentists and lay people to altered dental esthetics. J Esthet Dent. 1999;11(6):311-324.
4. Silversin J. For better practice relations. Int Dent J. 1987;37(2):123-126.
5. Blatchford WA, Pasley Blatchford C. Blatchford WA, Pasley Blatchford C, eds. Blatchford Blueprints: The Art of Creating Practice Success. Bend, OR: Blatchford Solutions; 2009:197-199.
6. Duchenne GB. The Mechanism of Human Facial Expression. New York, NY: Cambridge University Press; 1990.
7. Fradeani M. Esthetic Rehabilitation in Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 2004. Esthetic Analysis: A Systematic Approach to Prosthetic Treatment; vol 1.
8. Tarnow DP, Chu SJ, Kim J. Aesthetic Restorative Dentistry: Principles and Practice. Mahwah, NJ: Montage Media Corporation; 2008.
9. Fradeani M, Barducci G. Establishing communication with patients. In: Fradeani M, Barducci G, eds. Esthetic Rehabilitation in Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 2008;29-115. Prosthetic Treatment: A Systematic Approach to Esthetic, Biologic, and Functional Integration; vol 2.
10. Dawson PE. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St. Louis, MO: Mosby; 1989.
11. Spear F. Occlusion in the Clinical Practice [CD]. Seattle, WA: Seattle Institute for Advanced Education; 2005.
12. Coachman C, Calamita M. Digital Smile Design: A Tool for Treatment Planning and Communication in Esthetic Dentistry. In: Sillas Jr D, ed. Quintessence of Dental Technology. Chicago: Quintessence; 2012.
13. Magne P, Magne M, Belser U. The diagnostic template: a key element to the comprehensive esthetic treatment concept. Int J Periodontics Restorative Dent. 1996;16(6):560-569.
14. Goldstein RE. Masters of esthetic dentistry. Considerations for smile-generated long-range treatment planning: thoughts and opinions of a master of esthetic dentistry. J Esthet Restor Dent. 1999;11(1):49-53.
About the Author
Jason Olitsky, DMD
Immediate Past President
Florida Academy of Cosmetic Dentistry
Tallahassee, Florida
Director of Esthetics with Clinical Mastery Series
Accredited Member of American Academy of Cosmetic Dentistry