Lithium Disilicate: Advancing Dentistry
Durable, esthetic alternative to porcelain-fused-to-metal restorations.
Restorative dentistry has certainly benefited from the availability of advanced materials, such as lithium disilicate (IPS e.max®, Ivoclar Vivadent Inc., www.ivoclarvivadent.us). Despite this material’s excellent strength, esthetics, marginal integrity, durability, and biocompatibility, however, the applicability of lithium disilicate has been largely underestimated by many general dentists, who continue to rely on conventional materials, such as porcelain-fused-to-metal (PFM) restorations. Materials such as lithium disilicate may provide a variety of advantages over PFM restorations and other restorative materials.
Lithium disilicate is an advanced glass ceramic produced using a constantly optimized process to prevent the formation of defects (eg, pores, pigments). Pressable lithium disilicate (IPS e.max® Press, Ivoclar Vivadent Inc.) owes its esthetic characteristics in part to polyvalent ions that dissolve in the glass and provide the desired color. These color-releasing ions are distributed homogeneously to prevent pigment imperfections. Machinable lithium disilicate CAD/CAM (IPS e.max® CAD, Ivoclar Vivadent Inc.) blocks are colored using coloring ions, but achieve their desired shade and opacity during the post-milling firing process.1
Lithium disilicate provides esthetic advantages, including its ability to replicate the light transmission seen in natural teeth, as ingots are manufactured to exhibit varied optical properties.2,3 Because the material can be used to fabricate a variety and combination of restorations for the same clinical case, shade and color matching achieves a seamless smile design.4 According to cytotoxicity tests conducted by various institutes, lithium disilicate showed no cytotoxicity, mutagenicity, or in vivo toxicity, and safely interacted with its surroundings without causing adverse biologic reactions.5 Additionally, lithium disilicate is less cytotoxic than several commonly used composite materials, its cytotoxicity being comparable with that of several alloys and glass ionomers.6
Lithium disilicate has been shown to be superior to other all-ceramic materials with regard to abrasion. When processed correctly, abrasion of glass-ceramic crowns is sufficiently minimal, such that the material’s advantages over metal and metal-ceramic restorations prevail.7,8 Lithium disilicate also provides dentists with an option of minimally invasive tooth preparation for thin veneers (as thin as 0.3 mm) and other esthetic restorations, while simultaneously ensuring material/restoration strength and a conservative preparation design.1 Pressed lithium disilicate restorations demonstrate flexural strength values of 400 MPa in their final anatomic shaped form. Machinable lithium disilicate in full contour restorations demonstrates 360 MPa of monolithic flexural strength throughout the entire restoration.1 Restorations fabricated from lithium disilicate can be either conventionally cemented or adhesively bonded, providing that a proper retention form demonstrating a taper of 4° to 6° is achieved. Several studies have shown that lithium disilicate restorations demonstrate clinical efficiency with both adhesive and conventional cementation.9-11
Several clinical and laboratory studies have contributed to a growing body of research supporting the use of pressable and machineable lithium disilicate, as well as their accompanying nano-fluorapatite veneering glass ceramic, as alternatives to PFM restorations. In particular, several studies have examined the survival rates of pressable lithium disilicate and other studies have examined the survival rates of machineable lithium disilicate.7-11 Both the material characteristics and success of lithium disilicate have been evaluated and monitored by the scientific community since the product’s inception. Numerous in vitro and in vivo studies confirm its distinction.
Case Study
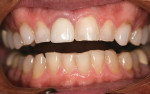
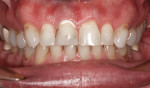
A male patient, who also happened to be a dentist, presented with a fracture to tooth No. 8, which had been previously treated with a root canal and crown (Figure 1). The patient had an implant placed and then presented to the authors for restorations on teeth No. 5 to No. 7 and on teeth No. 9 to No. 14 (Figure 2).
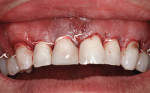
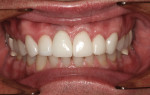
IPS e.max was chosen for fabrication of the required pre-molar and anterior restorations. An implant-supported provisional restoration was seated (Figure 3) and crown lengthening was performed (Figure 4). Given the complexity of the restoration type required, and because lithium disilicate was used to fabricate all restorations (Figure 5), this case demonstrates the versatility and esthetic capabilities of this material (Figure 6 and Figure 7).
The authors found the biocompatible and esthetic characteristics of lithium disilicate ideal because of the demanding esthetic requirements and high expectations of this specific case. In addition, not only was lithium disilicate the material of choice in this case, but, based on the outstanding success achieved in his restoration, it is now the treatment material of choice in the patient’s own practice.
Conclusion
Between providing superlative dentistry and running a practice, it is difficult for today’s dentists to stay abreast of the continual development of advanced materials, procedures, and technologies. The more that lithium disilicate is used in everyday dentistry, the more it will be relied on as an efficacious, esthetic, and durable alternative to PFM restorations.
References
1. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3):112-113.
2. McLaren EA, Phong TC. Ceramics in dentistry—part I: classes of materials. Inside Dent. 2009;5(9):94-103.
3. Culp L, McLaren EA. Lithium disilicate: the restorative material of multiple options. Compend Contin Educ Dent. 2010;31(9):716-720, 722, 724-725.
4. Cardoso JA, Almeida PJ, Fernandes S, et al. Co-existence of crowns and veneers in the anterior dentition: case report. Eur J Esthet Dent. 2009;4(1):12-26.
5. IPS e.max Scientific Report. Amherst, NY; Ivoclar Vivadent; 2011.
6. Brackett MG, Lockwood PE, Messer RL, et al. In vitro cytotoxic response to lithium disilicate dental ceramics. Dent Mater. 2008;24(4):450-456.
7. Etman MK, Watson TF, Woolford M. Early clinical wear of Procera-Allceram restorations and an experimental ceramic. J Dent Res. 2001;80:642.
8. Etman MK, Woolford MJ. Three-year clinical evaluation of two ceramic crown systems: a preliminary study. J Prosthet Dent. 2010;103(2):80-90.
9. Wolfart S, Eschbach S, Scherrer S, Kern M. Clinical outcome of three-unit lithium-disilicate glass-ceramic fixed dental prostheses: up to 8 years results. Dent Mater. 2009;25(9):e63-e71.
10. Gehrt MA, Rafai N, Reich S, et al. Outcome of lithium-disilicate crowns after 8 years [abstract 656]. Poster presented at: 88th International Association for Dental Research General Session; July 14-17, 2010; Barcelona, Spain.
11. Guess PC, Strub JR, Steinhart N, et al. All-ceramic partial coverage restorations—midterm results of a 5-year prospective clinical splitmouth study. J Dent. 2009;37(8):627-637.
Gerard Kugel, DMD, PhD
Dean for Research
Department of Prosthodontics and Operative Dentistry
Tufts University School of Dental Medicine
Boston, Massachusetts
Hans-Peter Weber, DMD, Dr med dent
Professor and Chair
Department of Prosthodontics and Operative Dentistry
Tufts University School of Dental Medicine
Boston, Massachusetts