Strengthening the Communicative Bond between Clinician and Ceramist
This dentist worked with his ceramist using IPS e.max lithium disilicate to replace worn anterior restorations.
The success of cases requiring indirect restorations from a laboratory depends on collaborative and ongoing communication between the dentist and ceramist. Both parties must share a mutual understanding and agreement of the patient’s condition and expectations for treatment in order to form a treatment plan that is minimally invasive regarding esthetic considerations, preparation design, clinical parameters, and material selections. Using diagnostic models, photographs, detailed impressions, and other tools is instrumental in the collaborative process. Sharing information regarding color matching, length and size ratio, and patient history enables ceramists to create restorations that meet desired criteria and dramatically simplify the restorative process.
Understandably, however, not all ceramists possess the same experience level, but must nonetheless develop the artistic and technical skills required to consistently produce high-quality restorations. Materials such as pressed ceramics allow laboratories to easily produce restorations using familiar hot-wax techniques, esthetic cut-back and layering techniques, and also ensure conservative preparations. Additionally, when the material is lithium disilicate (IPS e.max, Ivoclar Vivadent, www.ivoclarvivadent.com), ceramists can work with a user-friendly medium that demonstrates enhanced fitting properties, as well as a flexural strength that results in long-lasting, highly durable restorations.1,2
By combining detailed communication with an easy-to-use, predictable material, the author and his family-owned laboratory were able to work through a highly esthetic case that simultaneously served as a learning experience for the ceramist—his brother. A first-time lithium disilicate user well versed in fabricating posterior restorations, the ceramist had only recently begun fabricating single-unit anterior restorations. The case described here presented the opportunity for the ceramist to gain experience working on a larger, multi-unit treatment involving smile design and anterior esthetics.
Case Presentation
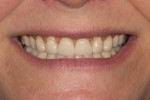
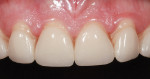
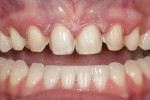
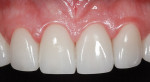
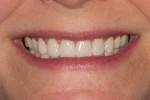
A 40-year-old woman presented with worn anterior porcelain veneers on teeth Nos. 6 through 11, which had been veneered with feldspathic porcelain when she was in high school. The veneers were over-contoured, and her gums had receded 3 mm, exposing the margins and dark roots (Figure 1 and Figure 2). She was aware of the esthetic problems but was hesitant to replace them because of financial concerns; with three children, this was not a priority. When Ivoclar Vivadent sponsored the materials and the author and ceramist donated their time for the treatment, she agreed.
A treatment plan to replace the existing porcelain veneers with IPS e.max lithium-disilicate veneers fabricated with an esthetic layering technique was decided upon. However, the patient also had congenitally missing lateral incisors, leaving her canines in the lateral incisor position and her first premolars in the canine position. This made obtaining the proper esthetic proportions and visible anatomy challenging.
Treatment Planning
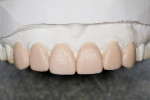
A comprehensive examination and esthetic consultation was performed. Study models and photographs were taken to demonstrate how her existing porcelain veneers were prepared and what would be different this time. Imaging software was used to depict the patient’s preexisting condition and the anticipated final outcome. The patient’s bite was evaluated, and a bite registration helped diagnose an absence of free space. For adequate evaluation of treatment goals and to ease the patient’s anxiety, wax-ups were created. The diagnostic wax-up illustrated the new height-to-width ratio and shape of the porcelain veneers (Figure 3). Because the existing veneers were worn down from the enamel on the opposing arch, necessitating additional room for the jaw to move without causing further wear, 0.5 mm of length was added to the incisal edges. The remaining length would be gained from a new gingival margin.
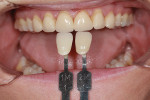
A shade guide was used to match the new veneers to the patient’s teeth (Figure 4). The patient’s worn anterior veneers were removed (Figure 5). A lingual silicone-putty matrix made from the diagnostic wax-up and filled with temporary crown resin was placed over the patient’s existing anterior dentition to create a trial smile. This provided a visual and physical representation of the final outcome for the patient. The original treatment plan included teeth Nos. 5 and 12 for a more overall esthetic appearance. However, the patient was unsettled with compromising healthy teeth because she could not comprehend that there would be a size discrepancy and did not want to reduce healthy tooth structure, so they were not included.
Preparation
Before the preparation appointment, the patient used at-home bleaching trays with 9% hydrogen peroxide for a few weeks. Subsequently, minimal soft-tissue contouring was performed on the laterals to create a more harmonious tissue zenith. Preparations were kept conservative, with refinement consisting of interproximally wrapping the margins to conceal the cement line. Typically, a lingual chamfer for added retention would be created, but in this case was unnecessary due to limited space with the opposing arch. Direct contact on the porcelain in centric relation would be avoided. To maintain all centric occlusion on the natural tooth and not on the porcelain, caution was taken to not break the contact points on the preparation.
The provisional restorations were placed, and a final impression and a length wax-up of the provisional restorations were taken and sent to the laboratory.
Laboratory Protocol
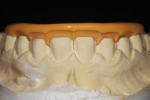
The anterior restorations were waxed on the master cast (Figure 6). The ceramist took a silicone impression of the white wax mock-up and injected molten pressable ceramic wax. This transferred the exact form defined by the white wax mock-up to the new wax patterns to be pressed. The margins were sealed with margin wax.
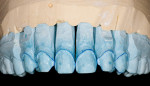
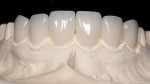
Managing contact points on the stone models was a tedious but necessary process (Figure 7). The completed wax-ups were sprued, invested, burned-out, and pressed using the IPS e.max ingot in shade IV-1. The single-unit anteriors were cut from sprues and ready for layering with the IPS e.max Ceramic veneering powder. The wax patterns were cut back, and translucent enamels were layered to create a life-like translucency at the incisal edge and labial surface. This was a joint process between the dentist and the ceramist. While the ceramist was responsible for the majority of the work, the dentist was also working in the laboratory, assisting with the final contours and textures of the restorations (Figure 8 and Figure 9). In this case, the color matching was straightforward because the patient did not have much incisal translucency or characterization.
Cementation
Proper fit and color of the ceramic veneers was ensured during the cementation appointment. The veneers received a final polish (Figure 10). Hydrofluoric acid was used in conjunction with Variolink Veneer resin cement (Ivoclar Vivadent) for bonding. The patient was given a week to wear and test-drive the veneers before returning to the dental office for a check-up appointment.
When the patient returned, an occlusal adjustment was performed to relieve high spots in excursive movements. Previously in centric relation, the patient was only touching natural enamel, so her bite never changed. A few weeks later, the incisal edges on all veneers were shortened by 0.5 mm to blend the smile line. This occurred because the length of the premolars appeared too short compared to the front six.
It was after the final restorations were placed that the patient understood why teeth Nos. 5 and 12 were originally included in the treatment plan. She was happy with the results (Figure 11 and Figure 12). An occlusal guard was constructed for the patient to wear at night to protect her new smile.
Conclusion
The patient was grateful for the assistance of Ivoclar Vivadent and the dental office for helping her regain confidence in her smile. The ceramist was appreciative for the opportunity to work on this case and gain a boost in self-confidence with his newfound knowledge and experience in working with smile designs and the IPS e.max system.
Advanced materials such as IPS e.max lithium disilicate allow dentists to perform more minimally invasive procedures that require less trauma to the patient’s natural dentition. The enhanced strength and optical properties satisfy the need for highly esthetic restorations while concurrently fulfilling clinical and functional requirements. Further contributing to the predictable results in this case were communication and collaboration between the dentist and ceramist. Predictable treatment outcomes are more likely to occur when diagnostic and treatment planning tools are integrated into the communication process.
Acknowledgment
The author would like to thank Craig Brown of Brown Dental Lab in Issaquah, Washington, for his ceramic work on this case.
References
1. McLaren EA, Phong TC. Ceramics in dentistry, part 1: Classes of materials. Inside Dentistry. 2009;5(9):94-103.
2. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dentistry Today. 2009;28(3):112-13.
About the Author
Kevin Brown, DDS
Private Practice,
Bellevue, Washington