The Mandibular Bar Overdenture
Getting from treatment plan to completion takes careful consideration and planning.
No longer is a complete denture the standard of care in restoring the edentulous mandible.1 The new standard of care is an overdenture that uses implants to help retain and support it. This article is aimed at dentists who are beginning to incorporate implant placement and restoration into their practices.
Bar Overdenture Considerations
A bar overdenture is an excellent prosthetic option that many patients choose over less expensive alternatives for a number of reasons, including:
- having more retention than a conventional denture.
- providing better support than a tissue-supported prosthesis.
- functioning better because it is more stable and moves less.
- being more comfortable to the patient.
Because of the amount and the pattern of resorption of the edentulous mandible, the only area available for implant placement is often the intraforaminal area.2 For the purposes of this article, the author will not discuss short implants or grafting procedures.
Some basic conditions must be present for the patient to be a candidate for a bar overdenture, and a good protocol for examination and treatment planning will determine whether or not these conditions are present.3
First, there must be adequate volume of bone in the intraforaminal area.4 This means having adequate bone in three dimensions—arch length, width, and height.3 (Note that approaches for dealing with inadequate bone volume are beyond the scope of this discussion.) Arch length is not a problem for placing four implants between the mental foramina; adequate bone height should allow a 12-mm or 13-mm implant to be placed without damage to any structures, and width should be approximately 6 mm to allow for placement of the standard 3.7-mm to 4-mm wide implants with 2 mm of bone facial and lingual to them.
There must be an interarch space of about 15 mm, which is not uncommon in the edentulous mandible, but in case there is not enough space, an alveoloplasty would create the space necessary.
Patient Selection
To determine if the patient meets the requirements described, at the initial examination the clinician should take preoperative photographs and impressions for study models and mount them using a facebow record and bite registration in centric relation. In addition, a radiographic survey consisting of a panoramic X-ray and selected periapical films are exposed as needed. As radiographs show only two dimensions, it is necessary to supplement that information with clinical observations or use a cone beam volumetric tomography scan to obtain very accurate cross-sectional measurements.5-7 Once the required information is obtained and a treatment plan is prepared, they are presented as part of informed consent to the patient along with information on all alternative treatment—eg, a fixed prosthesis, a fixed removable (hybrid), an implant-supported prosthesis (bar overdenture), a tissue-supported prosthesis such as an O-ring, a locator- or mini-implant-retained overdenture, or a conventional complete denture.
Case Presentation
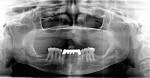
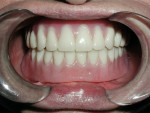
A 50-year-old woman with an unremarkable health history and who wore a maxillary complete denture against a terminal mandibular dentition, chose to have her remaining teeth extracted and replaced with a bar overdenture (Figure 1).
The patient did not want the implants placed on the same day of the extractions, so a new maxillary denture and mandibular immediate denture were fabricated for her. All of her remaining lower teeth were removed, an alveoloplasty was performed, and the dentures were delivered. The patient was allowed to heal for 3 months. Next, the lower immediate denture was duplicated, and the duplicate was used first to hold radiographic markers and later as a surgical guide by placing holes in the selected osteotomy sites.
Surgical Techniques
The letters A through E were assigned by Misch to the recommended osteotomy sites in the intraforaminal region,6 with A and E being the most distally placed osteotomies, and B and D the anterior ones. Undoubtedly, the distal osteotomy sites must be selected carefully to avoid the vital structures associated with the mental foramen and related anterior loops. Several techniques are useful here. The most reliable is gently exposing the mental foramen and placing the implants 6 mm or 7 mm mesial to it. Another technique designed to minimize the surgical flap extension is to use radiographic markers (which are radiopaque objects of known dimensions—eg, a 10-mm long orthodontic wire) attached to the surgical template and expose some films (Figure 2).
The anterior-posterior spread of the implants should be as large as possible to be able to extend a small cantilevered bar distal from the most posterior implants for better support of the overdenture in the posterior region. The literature suggests that the surgeon can cantilever as much as 2.5 times the anterior–posterior spread,8 but the author does not extend more than 10 mm when cantilevering (Figure 3). The sites are selected, and in preparing the osteotomies, the surgeon must take into account the anatomy of the area, which allows a fairly straight up and down angulation in the first premolar region; however, in the anterior region, the osteotomy may need to be angled slightly anteriorly to avoid perforating the lingual plate while proceeding apically, because the bone is more anterior in that area and perforating the lingual plate apically can result in severe bleeding complications.
The surgeon should always try to align the implants parallel to each other, but should not be concerned if they are not perfectly parallel, because the bar makes it possible to correct moderate amounts of divergence in the implants (Figure 4).
One technique that optimizes the surgical placement of the implants uses cone beam computed tomography-based surgical guides.9,10 The surgeon can use the guide to locate the predetermined implant sites and even control angulation and depth to prevent damage to important anatomic structures.
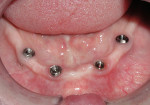
The implants are placed at crestal bone level and will heal submerged for 3 to 4 months to prevent pressure from mastication that may cause their failure to osseointegrate. Next, the implants are exposed, but not with a tissue punch; instead, the surgeon should use a small incision to be able to keep all of the scarce keratinized attached gingiva, which is desirable around the implants (Figure 5).
Seating the Overdenture
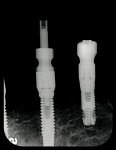
After the gums heal, impression posts are placed and an X-ray is exposed to verify complete seating before taking an impression (Figure 6). The impression posts used are either transfer or pick-up impression copings. Transfer copings require a conventional impression technique and pick-up copings use an open tray and are unscrewed from the implant before removing the impression from the mouth. The open-tray impression posts are necessary when the implants have different angulations; a closed tray could lock the impression in the mouth. The open tray may arguably be a more accurate technique because the impression posts remain inside the impression.
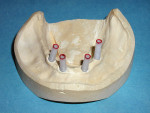
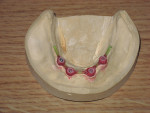
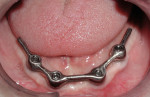
The laboratory pours the impression and the resulting model has the implant analogs replicating the position of the implants. One of the most popular bar designs uses three attachments—one anteriorly and two posteriorly (one on each side)— and these attachments are usually clips. The most common bar patterns are the Dolder Bar (Preat Corporation, www.preat.com), and the Hader Bar® (Sterngold™, www.sterngold.com). The Hader bar, which was used in this case, is fabricated using a plastic pattern and DuraLay™ resin (DuraLay, Reliance Dental, www.reliancedental.net) by casting it in Type 3 or Type 4 noble alloy (Figure 7). The Dolder bar is premade and soldered or welded. Other more expensive options are a milled cast bar and a CAD/CAM overdenture bar, which is computer-designed and milled from a titanium blank.11 This milled bar is stronger and often more accurate than the conventional cast bar. The bar needs to fit passively on the implants, and is verified by placing only one screw and taking X-rays to determine the fit (Figure 8). Once the fit is verified, the bar is placed back on the model and the laboratory can construct the overdenture (Figure 9).
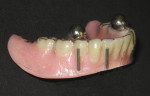
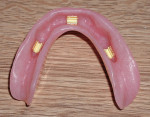
When the overdenture is returned, the bar is placed and torqued to the manufacturer’s specifications, delivered (Figure 10) to the clinician, and checked for fit, extension, balanced contacts, and group function (Figure 11).
Conclusion
In the author’s opinion, the mandibular overdenture is one of the best and most comfortable modalities of treatment for the edentulous patient. The above discussion is meant to provide some useful information to help dentists adequately select, plan, and deliver a bar overdenture to their patients.
References
1. Carlsson GE, www.ncbi.nlm.nih.gov/pubmed?term=%22Omar R%22%5BAuthor%5D">Omar R. The future of complete dentures in oral rehabilitation. A critical review. J Oral Rehabil. 2010;37(2):143-156.
2. Pietrokovski J, Starinsky R, Arensburg B, Kaffe I. Morphologic characteristics of bony edentulous jaws. J Prosthodont. 2007;16(2):141-147.
3. Misch CE. The endentulous mandible: an organized approach to implant-supported overdentures.Contemporary Implant Dentistry. 3rd ed. St. Louis, Mo: Mosby; 2008.
4. Şahin S, Kaya Y, Şençimen M, et al. Retrospective radiographic evaluation of the interforaminal region with spiral computerized tomography: adequacy for dental implant placement related to age and dental status. Gulhane Med J. 2010;52(2):69-75.
5. Worthington P, Rubenstein J, Hatcher DC. The role of cone-beam computed tomography in the planning and placement of implants. J Am Dent Assoc. 2010;141(Suppl 3):19S-24S.
6. Dreiseidler T, Neugebauer J, Ritter L, et al. Accuracy of a newly developed integrated system for dental implant planning. Clin Oral Implants Res. 2009;20(11):1191-1199.
7. Nokar S, Moslehifard E, Bahman T, et al. Accuracy of implant placement using a CAD/CAM surgical guide: an in vitro study. Int J Oral Maxillofac Implants. 2011;26(3):520-526.
8. Misch CE. Preimplant prosthodontics. Dental Implant Prosthetics. St Louis, Mo: Mosby; 2005:178.
9. Al-Harbi SA, Sun AY. Implant placement accuracy when using stereolithographic template as a surgical guide: preliminary results. Implant Dent. 2009;18(1):46-56.
10. Valente F, Schiroli G, Sbrenna A. Accuracy of computer-aided oral implant surgery: a clinical and radiographic study. Int J Oral Maxillofac Implants. 2009;24(2):234-242.
11. Carpentieri JR. Clinical protocol for an overdenture bar prosthesis fabricated with CAD/CAM technology. Pract Proced Aesthet Dent. 2004;16(10):755-757.
For additional content on Removable Prosthodontics, visit: dentalaegis.com/go/id106
For product information on Dentures & Partials, visit: dentalaegis.com/go/id107
About the Author
Carlos Boudet, DDS, DICOI
Private Practice
West Palm Beach, Florida