Ensuring Success in Porcelain Repair
Repairs will adhere as long as the basic principles of adhesive dentistry are followed.
Because more tooth-colored restorations are being done in ever-stronger ceramics, the ability to repair porcelain and lithium disilicate has become an important skill. These repairs will adhere to the restoration as long as the clinician adheres to the basic principles of adhesive dentistry. If these principles are not followed, the repair will need to be redone every few months, until the dentist gives up or the patient gives up on the dentist. Every clinician should know the limitations of ceramic repairs in order to know when to attempt it, and when to say “no.”
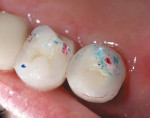
A repaired crown can never be as strong as the original lab-fired unit. Composite repair of porcelain in the mouth or on the bench will restore the tooth to esthetic but not occlusal function. If you cannot figure out why the original crown broke, it will break again. Know the answer before you promise the patient that it can be fixed. The prognosis is much better from accidental trauma, like biting once on a hard object (Figure 1). If the fracture was a result of clenching or bruxism, it is better to remake the crown.
Roughen the fracture with an abrasive air-blaster using aluminum oxide. Do not use a diamond, no matter the grit. Diamond-abraded metal may appear rough to the naked eye, but a microscope would reveal that diamonds do not roughen the surface; they smooth it.
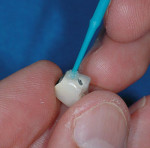
Know what type of metal the crown will be bonded to. Base metals oxidize, which creates strong bonds to resin cements, such as Parkell’s C&B-Metabond®. However, noble or high-noble alloys do not oxidize, so they require tin plating or special noble-metal primers to maximize the bond to the repair resin. Parkell’s MTL-V Primer™ has a long clinical and research history of forming stable bonds to precious and noble alloys. A single generous coat of “V-Primer” on the exposed metal (not the porcelain) is all that is needed; multiple coats may actually reduce the bond. If you are not sure if the alloy is noble, use the V-Primer, as it will not hurt base-metal bonds (Figure 2).
Virtually all ceramic-adhesive systems on the market involve silane, a chemical that bonds porcelain to composite resin, in one form or another. It comes in single- or double-bottle sets, in versions that require acid pretreatment, or do not. Single-bottle silanes contain both water and silane in a single mixture, and tend to react in the bottle, yielding a shorter shelf life. Double-bottle systems keep the water separate from the silane until the two components are mixed before application, so there is much less degradation in the bottle, and a much longer shelf-life.
With most regular silanes, the fractured ceramic surface needs to be etched first. For a predictable etch, manufacturers recommend hydrofluoric acid. However, using hydrofluoric acid intraorally remains controversial, as it can cause serious damage if it contacts soft tissue, including severe superficial and deep tissue injury, or even systemic toxicity. Although many dentists have used it for years without a problem, extreme care must be taken to protect the patient.
For dentists who prefer not to use hydrofluoric acid for etching, Parkell and Sun Medical Corp. created Etch-Free™, a safer, longer-lasting, two-bottle alternative that does not use the dangerous acid. Etch-Free permits resin cements like C&B-Metabond to form strong bonds to ceramic surfaces. The formula contains silane, and includes water, methyl methacrylate, and 4-META, a proven penetrating agent. The system has a well-documented 20-year clinical and research history.
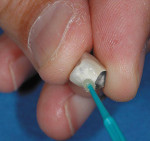
Warm the primed surfaces with a hot air dryer to speed up the drying of the Etch-Free and significantly improve the bond to the porcelain. After priming, brush a thin coat of Parkell’s C&B-Metabond Adhesive Resin Cement over the repair (Figure 3). It acts as both a masking and a bonding layer, holding the overlying composite on tenaciously. The C&B-Metabond powders come in two shades: radiopaque white to hide the metal, and translucent to coat porcelain. It is possible to mix powders, for less masking and more translucence.
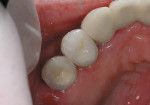
Wait for the C&B-Metabond to set hard, and then apply the matching composite resin. Adjust the repair out of occlusion and contour and polish the restoration. The final result (Figure 4) should look like new—but it is certainly not as strong as new. The patient needs to understand this. Discuss the importance of using proper caution when eating, and wearing their nightguard when sleeping.
Are all of these steps necessary? Maybe not, but if the repair fails, at least the clinician has done everything possible to make it a success. If the surface was not sandblasted, or the Etch-Free was not warmed, or the noble-metal V-Primer was not used, it might make the difference between success and failure. When your patient’s expectations are high, and your clinical reputation is on the line, take the extra time and do the procedure right.
Acknowledgment
The author would like to thank Dr. Gary Alex of Huntington, New York, for his photography of the case.
This article was written by Rich Goldman, DDS, vice president—clinical products for Parkell, Inc.
For more information, contact:
Parkell, Inc.
Phone: 800-243-7446
Web: www.parkell.com
Disclaimer
The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dentistry.