Implant Treatment Planning for a Restorative Outcome
Choosing the correct implant for the desired restorative outcome aids achievement of the treatment goals.
While several techniques have claimed successful outcomes using a variety of intra- and supra-osseous fixtures, implant dentistry did not enjoy broad-based appeal until the early 1980s. True acceptance in the dental community did not arrive until commercially pure titanium cylindrical implants were reported as having as high as a 92% success rate, as reported in a 15-year retrospective article.1 With this documented predictability, practitioners have become more comfortable recommending implant-retained prostheses for their patients. Over the past 3 decades, this form of tooth replacement has become the treatment of choice as a result of innovations in esthetics, abutment choice, implant design and materials, surface technology, and bone regeneration. Recent advances in implant dentistry enable clinicians to treatment plan using the restoration as a starting point. This makes it possible for them to better serve their patients and predictably deliver an esthetic prosthesis in a timely fashion.
Today, practitioners have dozens of implant companies from which to choose. Straumann offers a complete portfolio of tissue-level and bone-level implants as well as a complete portfolio of stock and custom abutments. From a clinician’s perspective this offers an appropriate solution for all situations encountered. However, the most compelling research reported in the last few years is that of the SLActive® surface technology (Straumann, www.straumann.us). This third-generation implant surface attracts the blood and bloodborne proteins deep into the roughened titanium surface, which accelerates both bone growth and osseointegration. As a result, the overall stability of the implant in the first 4 weeks does not drop because the secondary (biologic) stability is initiated sooner. Studies show that the 56% reduction in surface carbon on the SLactive (modified SLA) surface enhances the osteogenic properties of the implant, increasing the predictability when implants are at their greatest risk.2,3
The SLActive hydrophilic surface can positively affect the outcome of immediate and early loading of implants, as well as sites requiring bone regeneration. Recent research4,5 has concluded that the surface does in fact support greater bone apposition when compared to a hydrophobic surface. The studies suggest that gap-like lesions < 1 mm may not need to be grafted. This finding gives the clinician confidence in both early and immediate loading4 and immediate placement in an extraction socket, due to the faster healing and, ultimately, osseointegration.5
The Straumann product portfolio enables the case to be designed with the final prosthesis in mind. This concept of treatment planning begins with choosing the appropriate implant for the outcome desired. The tissue-level implant with a 1.8-mm collar has been a favorite for many practitioners due to its simplicity and predictability. In the author’s experience, this is often the implant of choice in more straightforward situations. The tissue-level implant is typically indicated in situations where a solid abutment can be used successfully. However, the decision also has to take into consideration the gingival biotype, restorative materials, emergence profile, intraocclusal distance, and space between teeth. Considering these other parameters, the Regular Neck Straumann Tissue Level implant may not be appropriate. If there is less than 7 mm of space between the adjacent teeth, a bone-level implant would be a better choice, as 1 mm of space is necessary between the collar and the adjacent tooth. The Straumann Bone Level implants offer the flexibility of choosing one of the many stock abutments or a custom-machined titanium or zirconium Straumann CARES® abutment to treat more demanding situations.
Surgeons are frequently faced with situations requiring implant placement in a narrow interdental space or thin alveolar ridge. With the advent of the Straumann Roxolid® implant, a predictable treatment alternative is available. The Roxolid implant is an alloy composed of titanium and zirconium (TiZr) with a SLActive surface. Mechanical tests have demonstrated higher fatigue and tensile strengths when compared to other implants made from Ti Grade IV.6
Case 1
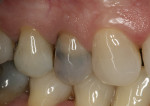
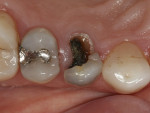
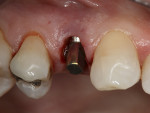
A 47-year-old woman with an unremarkable medical history presented with a nonrestorable upper right first bicuspid (tooth No. 5) (Figure 1 and Figure 2). Her treatment alternatives included strategic extraction with the fabrication of a conventional three-unit bridge or immediate placement of a single dental implant. Preparation of adjacent teeth, which would be required with a fixed removable prosthesis, was rejected in favor of implant placement.
Radiographic analysis revealed that immediate placement and provisionalization would be an option. This fell in line with the patient’s expectations, which included tooth replacement after extraction.
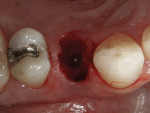
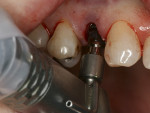
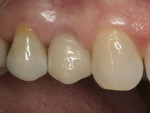
Consent was obtained and the tooth was extracted atraumatically using forceps (Figure 3). The socket was debrided thoroughly and rinsed with 0.12% chlorhexidine gluconate. After careful consideration, the decision was made to use a Straumann Regular Neck Tissue Level implant (Figure 4). This was the treatment of choice due to its simplicity and predictability. Good initial stability was obtained, which enabled immediate provisionalization. A hand-tightened 4-mm solid abutment was placed and temporized at the time of surgery (Figure 5). Healing was unremarkable, and the case was finalized after 10 weeks. The abutment was torqued to 35 Ncm, and the porcelain-fused-to-metal (PFM) crown was permanently cemented (Figure 6).
Case 2
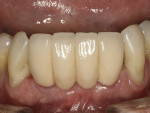
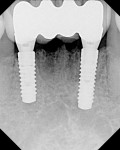
This patient presented with a generalized moderate chronic adult periodontitis. Significant pain was associated with her lower anterior segment due primarily to the pathologic mobility of her lower incisors. Radiographs revealed advanced bone loss, and a decision was made to strategically extract her hopelessly involved symptomatic teeth (Figure 7). Several comprehensive treatment plans were suggested, including mucogingival surgery, orthodontics, and orthognathic surgery. However, for a variety of reasons, she declined the therapy and preferred to have her chief complaint addressed.
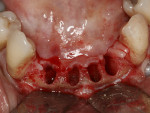
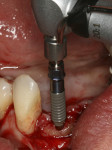
After informed consent was obtained, the area was anesthetized with 2% lidocaine. Teeth Nos. 23, 24, 25, and 26 were carefully extracted with forceps, and a full-thickness flap was elevated from teeth Nos. 22 through 27 (Figure 8). The extraction sockets were rigorously debrided of any soft-tissue remnants and rinsed with chlorhexidine gluconate 0.12%. The choice of placing two 3.3-mm diameter Straumann Bone Level implants was made when the ridge thickness and the clinician’s ability to create an appropriate emergence profile were taken into consideration. The fixture of choice was the SLActive Roxolid implant, as four teeth were replaced with two narrow-diameter implants (Figure 9). The additional fatigue and tensile strength made it unlikely that fixture fracture would be an issue. The additional bone in-growth found with the alloy implants proved advantageous in using narrow-diameter implants.
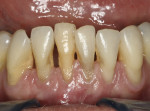
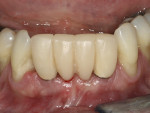
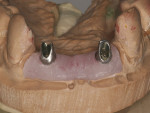
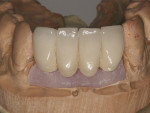
The fixtures had good initial stability enabling immediate provisionalization, which was performed by the patient’s restorative dentist immediately after the surgery (Figure 10). Custom- milled Straumann CARES abutments were fabricated to develop a hygienic emergence profile (Figure 11). The final prosthesis was a PFM bridge fabricated after the tissue had reached maturation (Figure 12, Figure 13, and Figure 14). This is consistent with the rationale to use Roxolid alloy implants. In situations calling for strength and rigidity, materials with the highest fatigue strength and proven longevity are preferred.
Conclusion
Comprehensive implant dentistry requires a complete knowledge of the restorative materials as well as the prosthetic and surgical phases of treatment. It is incumbent upon the members of the team to work together to choose the appropriate materials including the correct implant. The treatment plan should, therefore, not only include the prosthetic design but also an implant that aids achievement of the treatment goals. Straumann Tissue Level, Bone Level, and Roxolid implants with the SLActive surface help practitioners to exceed their patients’ expectations.
References
1. Adell R, Lekholm U, Rockler R, Branemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
2. Zhao G, Schwartz Z, Wieland M, et al. High surface energy enhances cell response to titanium substrate microstructure. J Biomed Mater Res A. 2005;74(1):49-58.
3. Bornstein MM, Valderrama P, Jones AA, Wilson TG, Seibl R, Cochran DL. Bone apposition around two different sandblasted and acid-etched titanium implant surfaces: a histomorphometric study in canine mandibles. Clin Oral Implants Res. 2008;19(3):233-241.
4. Ganeles J, Zöllner A, Jackowski J. Immediate and early loading of Straumann implants with a chemically modified surface (SLActive) in the posterior mandible and maxilla: 1-year results from a prospective multicenter study. Clin Oral Implants Res. 2008;19(11):
1119-1128.
5. Lai HC, Zhuang LF, Zhang ZY, et al. Bone apposition around two different sandblasted, large-grit and acid-etched implant surfaces at sites with coronal circumferential defects: an experimental study in dogs. Clin Oral Implants Res. 2009;20(3):247-53.
6. Gottlow J, Dard M, Kjellson F, et al. Evaluation of a new titanium-zirconium implant: A biomechanical and histological comparative study in mini pigs. Academy of Osseointegration 23rd Meeting, Boston, Massachusetts. February 28-March 1, 2008; Abstract OS-5. Clin Implant Dent Relat Res. 2010 Jun 25. [Epub ahead of print].
About the Author
Robert J. Miller, DMD
Private Practice
Plantation, Florida