Treating Cracked Teeth
Treating cracked teeth biomimetically can optimize clinical results.
By Randall G. Cohen, DDS | David Rudo, DDS
All-ceramic or ceramo–metal full-coverage crowns are sometimes placed as a preventive treatment for a tooth that is suspected of having a fracture. Full cut-down crowns, however, will not necessarily protect teeth from further cracking; they can instead weaken the remaining tooth structure by compromising the tooth’s elasticity and injuring the dental pulp. Sometimes a cracked tooth restored with a full crown does not resolve the tooth pain, and endodontics is required. Full-coverage porcelain-fused-to-metal crowns can develop a “push-pull” effect where the higher elastic modulus of the casting does not flex along with the underlying dentin, thus rendering it hypofunctional.1
The gingival margin is the point of maximum flexure and the region with the greatest stress concentrations. This occurs because of the abrupt geometric discontinuances and changes in shape at the butt margin.2 The maximum flexure and the great stress concentrations often lead to the breakdown of the cement seal sometimes resulting in microleakage, recurrent caries at the crown–tooth interface, pulpal pathology, tooth fracture, and catastrophic failure. Full-crown restorations have been described as the least desirable treatment option3 and should be avoided unless re-treatment of an already-crowned tooth is required.
Traditional G.V. Black amalgam cavity preparation designs involve the removal of a significant amount of tooth structure and the creation of sharp internal line angles. The sharp line angles act as stress concentrators, leading to the initiation and propagation of cracks, which, ultimately, will cause restoration failure.2 Because of the mechanical retention and dissimilarity of performance characteristics of the amalgam and the tooth, the components of this tooth–restoration complex conflict with one another rather than flexing and functioning harmoniously and biomimetically.
A preferred treatment is one that attempts to replicate the stress distribution, energy absorption, and other characteristics of the intact natural tooth. These performance characteristics contribute to the “fail safe” mode of intact natural teeth.4 Accordingly, this type of treatment option should be considered rather than weakening the remaining tooth with a full-coverage crown. Unlike the full-crown option, biomimetic preparation principles preserve the dentino-enamel junction (DEJ) in the gingival region during tooth preparation, thus maintaining the absorbing capacity of the intact tooth and is, therefore, recommended.5 These “biomimetic” tooth–restorative complexes help prevent cracking, fracture, subsequent pulpal degeneration, and catastrophic failure of the restored tooth.6 In this article, the authors will discuss a method for preventing a tooth from cracking, and an appropriate treatment method should a crack occur.
The Tooth’s Structural Integrity
Understanding the attributes of an intact tooth will help to determine how to replicate its performance characteristics. Natural tooth structure and its external form have evolved to satisfy specific functional requirements. By definition, the DEJ is the developmental and structural center of the tooth, orientated in a specific location within the tooth.7 The DEJ is actually a three-dimensional region composed of a network of collagen fibrils and dentin in one inter-phase united with an inter-phase composed of collagen fibrils and enamel. This three-dimensional network unites the dentin and enamel, which developed from two different embryonic types of cells and have different performance characteristics. The DEJ collagen fibril network forms the junction between the harder and stiffer enamel and the softer and more elastic dentin, permitting the tooth components with different stress/strain responses to function in harmony together. This collagen fibril network also acts as a “fail safe” mechanism that inhibits, stops, and redirects a crack or fissure.6 In vitro studies demonstrated that when teeth were overloaded, the cracks in the enamel did not penetrate into the dentin, rather they actually sheared at the DEJ.4 Other studies have demonstrated the great energy-absorbing ability of enamel8 that can sustain deformation without catastrophic failure.
In contrast to full-coverage crowns, biomimetically restored teeth use adhesive materials and fiber composites with performance characteristics similar to the hard tissues that were lost to caries or fracture. The fiber/resin reinforcement used in this restorative concept is Ribbond® (www.ribbond.com), a fiber reinforcement composed of ultrahigh molecular weight polyethylene in the form of a three-dimensional leno-weaved ribbon. An integral component of this restorative concept involves the creation of a three-dimensional “bio-liner” at the dentin–restorative composite interface that acts as a uniting component. A gap-free secure bond is formed between the dentin walls and the composite restorative material. There are documented outcomes of this “bio-liner” including increased the microtensile bond strength,9 minimized polymerization shrinkage and leakage,10 and the ability to bridge cracks in the pulpal floor.6
When placed parallel to and under the occlusal surface of the composite restoration, the three-dimensional fiber reinforcement ribbon acts as a stress distributor and energy-absorbing mechanism. These protective mechanisms function as an internal “shock-absorbing” system to prevent the build-up of strain energy and stress concentration that might otherwise lead to the initiation and propagation of cracking and even fracture of the dental–restorative complex.11 This concept creates a dental–restorative complex that preserves rather than destroys tooth structure, one in which the performance characteristics of the components of the complex function harmoniously.
Symptomatology
Cracked tooth syndrome can present varied clinical symptoms including pain on chewing, percussion sensitivity, and intermittent cold sensitivity. The cold sensitivity usually abates when the pulpal aspect of the crack remineralizes, and returns when the cracks propagate under occlusal loading. The longer the crack, the longer the patient experiences the sensitivity cycle.12 This may be due to the significant increase in stress concentrations immediately in front of the crack tip and the ensuing strain in the region.2 Cracks that develop in the tooth allow for the colonization of bacteria and caries to develop, putting the health of the pulp at risk, as well as compromising the structural integrity of the tooth.
Clinical Case
History and Findings
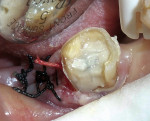
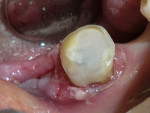
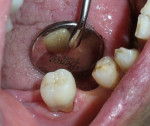
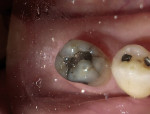
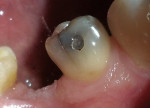
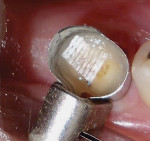
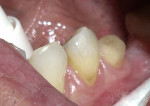
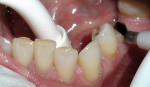
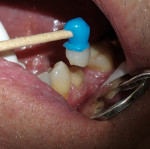
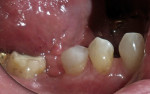
A 62-year-old man presented to the office for routine dentistry with no complaints of sensitivity or other symptoms. Examination revealed that tooth No. 20 was rotated and had drifted distally, leaving an open contact. In addition, tooth No. 20 displayed numerous cracks into the dentin, indicating that the tooth was structurally compromised (Figure 1 and Figure 2). The cracks into dentin were a result of the flexing under function of the tooth that had been weakened by a wide occlusal amalgam. It is appropriate to treat cracked dentin even when the patient has no symptoms because the 50-μm to 100-μm openings allow for bacterial growth and penetration into the dentin. Untreated cases ultimately result in a fractured tooth, requiring endodontics, periodontics, crown treatment, or possibly extraction. A similar condition existed for tooth No. 18; tooth No. 19, according to the patient, had been missing for more than 40 years. Restoration of teeth Nos. 18 and 20 was indicated; however, replacement of tooth No. 19 with a conventional fixed bridge was ruled out because of the thin root on tooth No. 20, the highly weakened tooth structure, and the narrowed edentulous space. The patient had been functioning satisfactorily for 40 years and did not want a replacement.
Removal of Structurally Compromised Dentin
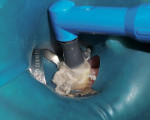
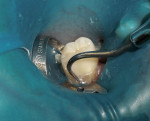
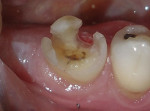
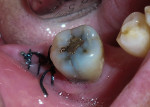
After satisfactory local anesthesia had been achieved, the tooth was isolated using a dental dam and the existing amalgam was removed with a 330-carbide bur. Inspection of the dentin revealed numerous multidirectional and deep cracks that extended far beyond the original amalgam. Only the fragile remnants of cusps remained after the removal of the cracks with a flat-ended diamond (Figure 3), so the cusps were removed as well using a flat-ended diamond with the handpiece turned to the side. The dental dam was removed to facilitate easier application of the matrix retainer.
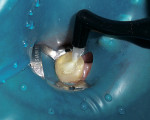
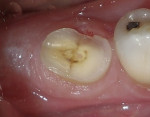
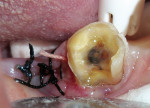
A crack persisted at the floor of the preparation. It was apparent that further penetration into the floor of the preparation would have resulted in a pulpal exposure, so the remnant of the crack was allowed to remain (Figure 4).
Creating a Predictable Resin-Dentin Bond
The bonding agent selected was Clearfil SE Protect (Kuraray Dental, www.kuraraydental.com) a sixth-generation, self-etch adhesive system that contains an antibacterial component in Bottle 1 (primer) and a fluoride component in the microfilled resin (Bottle 2.) A single drop of primer was dispensed into the mixing well, and was applied to the cut tooth surface with a disposable brush. The primer was allowed to reside on the preparation for 20 seconds by the clock. Then, the preparation was dried very thoroughly (10 seconds) using an air syringe. Next, one drop from Bottle 2 (resin) was applied to the preparation, lightly air-dried, then light-cured with a standard curing light for 20 seconds.
Bridging the Crack with a Fiber-Reinforced Liner
Further reduction in polymerization contraction stress was accomplished by lining the dentin with Ribbond®, a high molecular weight, leno-weaved fiber, although this was less necessary in this very flat, low-stress preparation. However, the Ribbond®/Majesty Flow lining also serves to re-create the intact dentin’s energy-absorbing capability by redirecting forces laterally. By adapting the Ribbond® closely to the dentin substrate, the clinician can increase the fracture toughness of the tooth and prevent the existing dentin crack from propagating and causing failure. The multidirectional Ribbond fibers bridging the crack act like stitches and transfer the stresses to regions of greater structural integrity.6
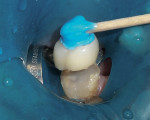
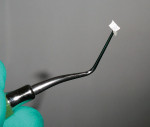
A tiny amount of Ribbond® Securing Composite was applied to the floor of the preparation, and a small amount was also applied to the end of an endodontic plugger. The end of the plugger was used to pick up a piece of Ribbond (Figure 5) to enable its transfer to the preparation and the plugger was then used to press the fiber into place. The field was then light-cured for 20 seconds to secure the Ribbond® to the dentin floor (Figure 6).
Building the “Biobase”
A thin layer of a heavily filled, flowable composite (Clearfil Majesty Flow, Kuraray Dental) was then applied and cured for 20 seconds to completely cover the dentin surface. The “biobase” was built up further by adding a 2-mm layer of Clearfil AP-X (Kuraray Dental). This greatly simplified final preparation technique was completed by creating an enamel bevel and a smooth, gradually sloping “bathtub” design with a finish line several millimeters above the tissue margin. Perfectly flat preparations should be avoided because they create difficulties in lining up the casting for easy seating. Accordingly, the preparation required no retraction cord to make an accurate impression using a vinyl polysiloxane material. The patient was dismissed with no provisionalization required (Figure 7).
Bonding the Indirect Restoration
The dental laboratory fabricated a custom-shaded onlay made from Estenia™ (Kuraray Dental), a ceramic-filled, heat-cured composite that has the same hardness and flexural modulus as tooth enamel. On the insertion visit, the preparation was cleaned with a slurry of coarse pumice, rinsed, and isolated with cotton rolls.
The intaglio of the restoration was etched (K-Etchant Gel, Kuraray Dental) and rinsed. Next, a single drop of Clearfil Ceramic Primer (Kuraray Dental) was applied to the internal aspect of the casting and dried thoroughly. The case was placed onto the die model, and an applicator stick was created with Delar blue wax melted onto a cotton-tipped applicator. The blue wax was softened in a flame and attached to the case so that the stick was oriented over the canine on the same side of the arch.
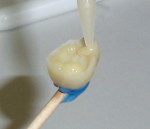
The adhesive was a dual-cured, universal bonding agent (Clearfil DC Bond, Kuraray Dental). One drop from Bottle A and one drop from Bottle B were combined in a mixing well and stirred for 5 seconds with the applicator brush. The mixture was applied generously to the dentin substrate (Figure 8) and allowed to stay for 20 seconds. The surface was lightly dried and light-cured. The restoration was loaded with adhesive cement (Clearfil Esthetic Cement, Kuraray Dental) through its automix syringe, and brought to the tooth using the applicator stick (Figure 9).
The gross excess of cement was first removed with the end of a cotton roll with digital pressure from the restoration down to the tooth. Then, while maintaining constant apical pressure on the restorations, a 5-second “wave-cure” with the standard curing light was performed to bring the unset cement to the gel point. At this point, with the assistant maintaining apical pressure on the casting, the excess interproximal cement was removed with floss. After using a scaler on the accessible surfaces, the final cure of the cement was accomplished with two circuits of a 10-second light burst on each of the facial, occlusal, and lingual aspects of the restoration. Lastly, a brief polish with coarse pumice on a prophy cup imparted a smooth finish to the tooth/restoration (Figure 10). Proximal and occlusal adjustments in biomimetic restorations are rare because complete seating is easily attainable and verifiable.
Clinical Case 2
A 91-year-old man in good general health elected to have tooth No. 31 restored once he had experienced a fracture on tooth No. 32 that required surgical removal (Figure 11). The patient was a vibrant person, physically active and mentally sharp, who liked to take vacations with his wife to Disney World and really enjoyed dining out. The cracks into the dentin allowed tooth decay to develop (1-μm of bacteria can easily penetrate 50-μm to 100-μm cracks). When his functioning third molar split the week prior to this appointment and required removal, he wanted to make sure he could still chew on his right side. The preoperative view showed occlusal-effect caries and cracks into dentin in tooth No. 31, which substantially undermined the coronal tooth structure. Dentin cracks were removed with the exception of the deepest part of the buccal crack that was encroaching on the pulp. Once debridement of the carious dentin had been completed, a coarse flat-ended diamond was used to flatten the remaining tooth structure (Figure 12). Isolation was accomplished with retraction cord soaked in astringent (Hemodent™, Premier Dental, www.premusa.com.)
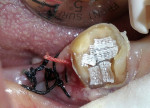
The “soft zone” of the tooth, corresponding to the DEJ, was created by applying a thickened flowable composite (Ribbond® Securing Composite) to the dentin walls and floor and adapting multiple overlapping Ribbond® squares (Figure 13). The bioliner was completed by adding a heavily filled, low-shrinking flowable composite (Clearfil Majesty Flow) and light-cured 20 seconds (Figure 14). The bulk of the biobase was then built up with a light-cured composite (Clearfil AP-X.) The biobase was contoured axially using a flat-ended diamond to create a smooth transition between tooth structure and composite in the furcation area. Once the biomimetic onlay preparation was completed, an impression of the case was made and the patient was dismissed (Figure 15).
When the casting was returned from the laboratory, the preparation was isolated by applying the rubber dam, then cleaned of salivary proteins and debris using coarse pumice (Figure 16). One drop from each of the two bottles of bonding resin (Figure 17) were combined in a single mixing well, then brushed onto the preparation (Figure 18). Simultaneously, the assistant applied an etch (K-Etchant Gel, Kuraray Dental) to the interior of the casting, then rinsed and dried it. One drop of silanating agent (Clearfil Ceramic Primer) was applied to the interior of the case and dried. A wax stick applicator was attached to the onlay, and the casting was loaded (Figure 19) with resin cement (Clearfil Esthetic Cement, Universal shade) and seated onto the preparation (Figure 20). A one-third piece of cotton roll on a mosquito hemostat was used to remove excess cement while continual downward pressure was exerted on the case to avoid dislodgment. The cement was brought to its gel state after a wave cure (5 seconds) then the remaining excess was removed with scalers and curettes. After checking the occlusion, the white rubber point and the coarse pumice were used to bring the finished case to a smooth finish (Figure 21 and Figure 22).
Discussion
Cracks that develop in dentin in the months and years after amalgam or composite restorations fail can propagate under occlusal function and lead to caries, pulpal inflammation, pain, and tooth loss.
The biomimetic clinical protocol to treat and prevent dentin cracks by replacing lost tooth structure with materials that will flex along with the tooth has proven to be clinically successful. In addition, biomimetic techniques maximize bond strength and minimize stresses, ultimately resulting in highly esthetic, durable, and maintainable restorations.
Proper restorative material selection is vital to achieving the desired result. In the clinical example presented, an antibacterial self-etch adhesive (Clearfil SE Protect) was chosen because it disinfects the dentin and provides a predictably strong bond to the dentin. Further, this product has low technique sensitivity, which is characteristic of self-etch adhesives. The fluoride contained within the microfilled resin (Bottle 2) has been shown to stabilize the resin–dentin bond over time, avoiding the slow degradation that is associated with some self-etch adhesives.13 Further work has suggested that the fluoride within Clearfil SE Protect will inhibit secondary caries formation. The use of a heavily filled, low-shrinking flowable composite (Clearfil Majesty Flow) as a liner provides excellent dentin surface coverage, strength, and an elastic modulus that approximates human dentin.14
The bulk of the lost tooth structure should also be replaced using a composite material that approximates dentin’s flexibility to lessen the stress at the restoration–tooth interface. The material also should have the same hardness as dentin to facilitate effective cutting during the preparation phase, and must be compatible with the adhesive used. In this clinical example, Clearfil AP-X was selected because of its compatibility with the dentin bonding agent, its simplified light-curing protocol, its physical properties of elasticity and hardness, and its ease of handling.
The final casting of the tooth should be made from a stiffer material than the underlying composite but still flexible so that a “flexibility gradient” is established, similar to what exists in the intact tooth. Suitable materials are cast-ceramic and cast-gold, and a ceramic-filled, heat-cured laboratory composite (Estenia®) as shown in the example.
In both clinical cases, teeth with structural compromises were restored biomimetically rather than using the aggressive crown preparation that has long been part of the routine practice of restorative dentistry. Furthermore, the long-term success in both cases will be extended by not cutting down the two abutment teeth for a fixed bridge.
Conclusion
The biomimetic protocol for preventing and treating cracked teeth is advanced, yet simplified. By keeping cast restorations well above the tissue margin, impression making and cementation in a less-than-ideal field is eliminated. By preserving the DEJ at the tooth’s gingival margin, the clinician maintains the tooth’s flexibility and avoids failure at the tooth’s weakest point. If recurrent caries occurs in a biomimetically restored tooth, it frequently takes place in an accessible, easily repaired part of the restoration, well away from the gingival margin. This is in sharp contrast to a failed full cut-down crown where cement washout leads to submarginal caries and sometimes a non-restorable fracture. Frequently, a replacement crown is needed along with periodontal surgery and endodontics. Indirect biomimetic restorations, therefore, represent an upgrade of the quality of care over the destructive 360º crown preparations that are frequently performed in clinical practice. With reliable bonding technology, no longer are geometric retention forms required for restorative dentistry, and so the clinician can take full advantage of today’s bonding agents, composites, and resin cements to prevent and treat teeth with stress fractures.
Disclosure
Dr. Cohen has received an honorarium from Kuraray Dental for this article.
References
1. Douglas W. In: Magne P, Belser U, eds. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing. 2002;19.
2. Gordon JE. The New Science of Strong Materials. Princeton University Press. 1984.
3. Schmitt J, Robbins W, Schwarz R. The Fundamentals of Operative Dentistry. 2nd ed. Chicago, IL: Quintessence. 2001;vii.
4. Lee JJ, Kwon JY, Chai H, et al. Fracture modes in human teeth. J Dent Res. 2009;88(3):224-228.
5. White SN, Miklus G, Chang PP, et al. Controlled failure mechanisms toughen the dentino-enamel junction zone. J Pros Dent. 2005;94(4):330-335.
6. Belli S, Cobankara FK, Eraslan O, et al. The effect of fiber insertion on fracture resistance of endodontically treated molars with MOD cavity and reattached fractured lingual cusps. J Biomed Mater Res B Appl Biomater. 2006;79(1):35-41.
7. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing. 2002;38-40.
8. Xie Z, Swain MV, Hoffman MJ. Structural integrity of enamel: experimental and modeling. J Dent Res. 2009;88(6):529-533.
9. Belli S, Donmez N, Eskitascioglu G. The effect of c-factor and flowable resin or fiber use at the interface on microtensile bond strength to dentin. J Adhes Dent. 2006;8(4):247-253.
10. Erkut S, Gulsahi K, Caglar A, et al. Microleakage in overflared root canals restored with different fiber reinforced dowels. J Oper Dent. 2008;33(1):96-105.
11. Rudo DN, Karbhari VM. Physical behaviors of fiber reinforcement as applied to tooth stabilization. Dent Clin North Am. 1999;43(1):7-35.
12. Brannstrom M. The hydrodynamic theory of dentinal pain: sensation in preparations, caries, and the dentinal crack syndrome. J Endod. 1986;12(10):453-457.
13. Donmez N, Belli S, Pashley DH, Tay FR. Ultrastructural correlates of in vivo/in vitro bond degradation in self-etch adhesives. J Dent Res. 2005;84(4):355-359.
14. Data on file. Kuraray Dental.
About the Authors
Randall G. Cohen, DDS
Private Practice
Yardley, Pennsylvania
David Rudo, DDS
Developer and President
Ribbond, Inc.
Seattle, Washington



 ® squares." title="Figure 13">
® squares." title="Figure 13">