Handpiece and Diamond Selection
Careful consideration of this component of the armamentarium is critical for optimal results in restorative dentistry.
By Alan M. Atlas, DMD
The development of the dental handpiece is considered one of the most important advancements in dentistry. Since 1868, when Green and, a few years later, Morrison in 1871, introduced the air-driven handpiece that transformed the dental profession, technology, especially over the past 50 years, continues to improve the speed and efficiency of tooth preparation and increase handpiece performance and longevity.1
The air-turbine high-speed handpiece continues to be the most popular type of high-speed handpiece due to its reasonable cost for purchase and repair, ability to rapidly remove tooth structure, excellent ergonomic weight and size, and reduced risk of pulpal damage when used properly.2 The high-speed electric handpiece was introduced as an alternative option to the air-driven device but has been unable to achieve a significant market share in America.3 These handpieces are considered more costly to purchase and repair, have larger contra-angle heads, and are heavier in weight, which may cause problems with ergonomics and reduced visual access. Advantages of the electric version are reported to be improved precision, torque, and cutting efficiency.
The goal for any operative dental procedure is to achieve conservative, atraumatic, and precise preparations for optimal long-term outcomes. Kenyon and colleagues evaluated the quality of dental preparations performed by dental students comparing the air-driven and the electric handpiece. The results indicated that differences in preparation and refinement scores between the two handpieces was not statistically significant.2
Clinicians have the opportunity to perform precision dentistry using state-of-the-art armamentarium. Recent advancements in handpiece technology now offer an air-powered adaptive air and electric control in one system (eg, Midwest® Stylus™ ATC, DENTSPLY Professional, www.professional.dentsply.com) enabling the power and efficiency of electric without the added size and weight. This type of handpiece can deliver constant torque at high speeds, enabling superior preparation.
With the advent of contemporary dental adhesive technology, the proper selection of a dental handpiece and accompanying diamond or bur selection becomes even more critical for optimal outcomes. The preparation of tooth structure for removal of a carious lesion or defect creates the substrate for the final restoration. During this preparation, enamel and dentin surface characteristics that make up the cavity walls and margins are affected differently depending on the size and shape of the instrumentation.
In 1962, Kasloff et al4 showed that upon preparation with different handpieces, fewer enamel cracks and microfractures occurred when diamond points were used instead of carbide burs. Another study demonstrated that the degree of enamel damage is influenced by the diamond grit size and type of bur.5 Fine-grit and superfine-grit diamond burs produce less marginal enamel cracks than regular-grid diamond burs and six-bladed carbide burs as well as improve the marginal adaptation of the adhesively placed composite resin to the cavity wall.6 A smooth cavosurface and proximal margin will reduce enamel irregularities and cracking resulting from the polymerization stress of light-curing and finishing, and allow for a more intimate contact between enamel and composite if the bonding agent is carefully placed without excess. The net clinical outcome will be enhanced marginal integrity of the restoration and improved long-term outcomes.
A diversity of scientific opinion has evolved about the effect of diamonds on bond strengths to dentin depending on the strategy employed for adhesion. The result of dentin preparation is a smear layer consisting of ground-up dentin, bacteria, collagen, and hydroxyapatite not tightly attached to the dentin substrate. This layer is considered a barrier to resin-monomer infiltration and must be treated before resin is applied. The two approaches used today are phosphoric acid in a total-etch or an etch-and-rinse system, which completely removes the smear layer, or the self-etch system that uses acidic monomers to simultaneously demineralize and infiltrate the smear layer, incorporating it within the resin–dentin bond. Ermis et al7 concluded that for the etch-and-rinse and strong, highly acidic self-etch adhesive systems, the bonding effectiveness is unaffected by diamond or bur type, while for ultra-mild, less-acidic self-etch adhesives, bond strengths can be significantly improved by finishing the cavity preparation with fine-grit diamond burs. Marques et al8 had a similar conclusion in their study, stating that a course-cut carbide bur should be avoided prior to using a mild self-etch adhesive, while a fine-cut carbide bur provided the best bond strength.
Studies9,10 have demonstrated that rounded internal line angles produced by appropriately shaped diamonds lead to a reduction of stress along the adhesive interface between the tooth and composite restoration. In addition, tooth preparations for indirect restorations refined with finishing burs or super-fine diamonds may favor the placement of restorations with the smallest marginal discrepancies, regardless of the type of cement used.11 This is best achieved with specifically shaped, modified shoulder and feather-edge diamond burs (eg, 836 KR F, 845 KR F, 847 KR F, and 888 EF; Midwest Diamonds, DENTSPLY Professional) with fine and superfine grits used on enamel and dentin rather than carbides, as well as an innovative handpiece that allows precise preparation as described in the following case study.
Case Study
This case study will describe the placement of a direct posterior composite restoration using a state-of-the-art dental handpiece, specifically shaped and grit diamonds, a sectional matrix system for proper contacts, and exceptional resin composite materials placed incrementally using careful and controlled placement to minimize finishing of the restoration.
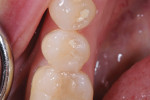
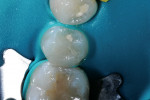
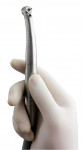
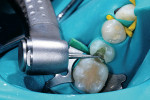
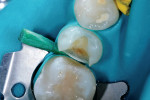
The patient presented with a defective composite restoration due to recurrent caries at the distal–gingival margin (Figure 1). After rubber-dam placement to control potential contamination of the operative field (Figure 2), initial preparation commenced using the Midwest® Stylus™ ATC dental handpiece (Figure 3). The unique features of this handpiece are the speed-sensing intelligence that uses a sensor to maintain speed and torque while under the load of tooth preparation. In addition, this handpiece offers superior turbine suspension to deliver exceptional control, precision, and accuracy.
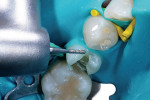
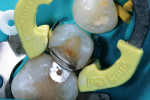
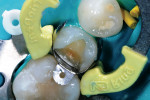
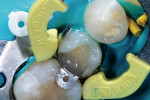
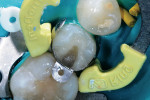
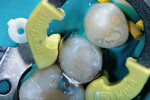
The rationale for diamond selection has been described above (Midwest Diamonds, DENTSPLY Professional). The 836 KR medium-grit diamond created a conservative, rounded internal line-angle cavity shape, and dentin preparation was finished with the 836 KR extrafine diamond for an ideal substrate surface for the adhesive system selected (Figure 4). The enamel cavosurface margin and interproximal walls were finished with the 888 extrafine diamond to create smooth, aprismatic enamel surfaces for optimal placement of the restoration (Figure 5). The final preparation had the correct finish lines for the best adaptation of the sectional matrix, adhesive bonding agent, and composite resin material (Figure 6).
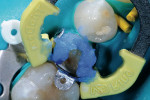
The V3 sectional matrix band and separation ring (Triodent, www.triodent.com) was placed to achieve the correct convex contours for proper tooth contacts (Figure 7). Prior to the self-etch bonding system application, a selective enamel etch was incorporated in the technique to maximize the bond strength to the enamel cavosurface margins only (Figure 8).12 The viscous 37% phosphoric etch was not applied to the gingival box enamel, if it were present, to avoid placement on dentin when using a self-etch adhesive system. The etchant was placed for 15 seconds, rinsed well for 10 seconds, and the tooth adequately dried. The self-etch adhesive system used, Xeno IV® (DENTSPLY Caulk, www.caulk.com), was agitated on dentin, carefully applied to the enamel surfaces, and the excess was picked up using a microbrush (Figure 9). It was then air-dried and light-cured for 10 seconds using an LED curing light (Smartlite® Max, DENTSPLY Caulk).
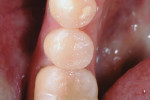
The composite resin was placed incrementally in an open-sandwich technique where all layers of composite would be exposed to the oral environment when the matrix band was removed. The first horizontal increment of resin composite was Surefil® SDR™ flow (DENTSPLY Caulk) (Figure 10). This unique composite features low viscosity, self-leveling, low shrinkage, and low contraction-stress properties that enable exceptional marginal adaptation at gingival box areas.13 The first vertical increment of a micro-nanohybrid composite (Esthet-X HD®, DENTSPLY Caulk) was placed in a technique described as controlled placement,14 where the material was positioned only against the walls of the entire cavity, leaving space internally to allow the composite to flow and obtain maximum adaptation with minimal strain or stress as it underwent light polymerization and transformed from monomer paste to a rigid polymer (Figure 11).15 The last vertical increment was the most confined and stressful to the cavity, but it was placed against the first horizontal and vertical composite increments and did not touch any tooth surface (Figure 12). The separation ring was removed from the tooth and the matrix band was opened to allow for inspection of margins and additional light-curing for complete conversion and polymerization (Figure 13). Due to the controlled placement of the composite resin, the final restoration was finished minimally with finishing diamonds, preserving sound healthy enamel and polished well with a one-step polishing system (POGO® Diamond Micro Polishing System, DENTSPLY Caulk) (Figure 14).
Conclusion
Precision dentistry using a state-of-the-art dental handpiece, specifically shaped and grit diamonds, sectional matrix systems, and carefully placed, exceptional bonding agents and resin composite materials will ensure extraordinary long-term outcomes.
References
1. Choi C, Driscoll CF, Romberg E. Comparison of cutting efficiencies between electric and air-turbine dental handpieces. J Prosthet Dent. 2010;103(2):101-107.
2. Kenyon BJ, van Zyl I, Louie KG. Comparison of cavity preparation quality using an electric motor handpiece and an air turbine dental handpiece. J Am Dent Assoc. 2005;136(8):1101-1105.
3. Christensen GJ. Are electric handpieces an improvement? J Am Dent Assoc. 2002;133(10):1433-1434.
4. Kasloff Z, Swartz ML, Phillips RW. An in vitro method for demonstrating the effects of various cutting instruments on tooth structure. J Prosthet Dent. 1962;12(6):1166-1175.
5. Xu HHK, Kelly JK, Jahanmir S, et al. Enamel subsurface damage due to tooth preparation with diamonds. J Dent Res. 1997;76(10):1698-1708.
6. Nishimura K, Ikeda M, Yoshikowa T, et al. Effect of various grit burs on marginal integrity of resin composite restorations. J Med Dent Sci. 2005;52(1):9-15.
7. Ermis RB, De Munck J, Van Meerbeek B, et al. Bond strength of self-etch adhesives to dentin prepared with three different diamond burs. Dent Mater. 2008;24(7):978-985.
8. Marques MM, Kenshima S, Muench A et al. Effect of c-factor and dentin preparation methods in bond strength of a mild self-etch adhesive. Oper Dent. 2009;34(4):452-459.
9. Hubsch P, Middleton J, Knox J. The influence of cavity shape on stresses in composite dental restorations: a finite study. Comput Methods Biomech Biomed Engin. 2002;5(5):343-349.
10. Kinomoto Y, Torii M, Takeshige F, et al. Polymerization contraction stresses of resin-based composite restorations within beveled cavity preparations of class I restorations. Am J Dent. 2003;16(2):139-143.
11. Ayad MF. Effects of tooth preparation burs and luting cement types on the marginal fit of extracoronal restorations. J Prosthodont. 2009;18(2):145-151.
12. Van Meerbeek B, Yoshihara K, Yoshida Y, et al. State of the art self-etch adhesives. Dent Mater. 2011;27(1):17-28.
13. Ilie N, Hickel R. Investigation on a methacrylate- based flowable composite based on the SDR™ technology. Dent Mater. 2011;27(4):348-355.
14. Atlas AM. The controlled placement and delayed polymerization technique for the direct class 2 posterior composite restoration. Compend Contin Educ Dent. 2005;26(11):812-818.
15. Ferracane JL. Buonocore Lecture. Placing dental composites-a stressful experience. Oper Dent. 2008;33(3):247-257.
About the Author
Alan M. Atlas, DMD
Clinical Associate Professor
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Private Practice
Philadelphia, Pennsylvania