Achieving an Esthetic Smile with Tissue Management
Combining patient expectations with photographic blueprints and adhering to biologic principles can reap superior cosmetic results.
By Jack D. Griffin, Jr, DMD
The simplicity of closed diode laser gingivoplasty can tempt the practitioner to administer hasty treatment and less-than-ideal planning. In doing smile rehabilitation, it is prudent to stick to biologic width limitations when sculpting tissues, and to use sound tissue preparation procedures to achieve predictable results that deliver superior esthetics, long-term tissue tolerance, and patient satisfaction. Thorough planning with photography, probing, and tissue marking can lead to predictable results, despite slight compromises due to patient demands.
Gingival Enhancement with Laser Treatment
For more than 20 years, bonded porcelain veneers have been placed to meet the esthetic desires of patients. But, in this time of heightened cosmetic awareness and greater desire for more acceptable long-term solutions, gingival enhancement with laser treatment has become an important adjunct.1,2 Creating a highly esthetic smile can only be accomplished with a sound union of proper restorative material selection, adequate tooth preparation, and biologically acceptable soft-tissue treatment.3,4 The result will be achieving a maximum level of stable esthetics.5
Thorough planning and adherence to biologic principles are the keys to predictable treatment.6 Performing careless, hasty treatment creates the potential for chronic soft tissue irritation, which can lead to compromised treatment, despite more favorable tooth proportions.7 Anatomical and functional challenges must be incorporated into a thorough treatment plan, taking soft tissue position, tooth preparation design, and idealized tooth positioning into consideration, all while meeting patient expectations.8,9
Before soft-tissue preparation, the clinician should take the following steps:
- Record patient expectations
- Radiographic evaluation
- Photographic “blueprint” of ideal contours
- Sulcus measurement
- Marking of sulcus depth on tissue
- Probe to alveolar crest (bone sounding)
Case Report
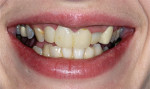
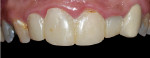
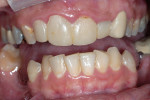
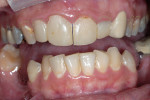
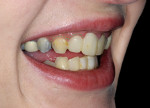
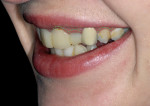
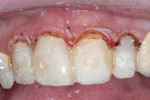
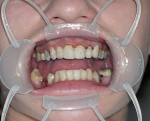
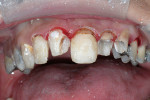
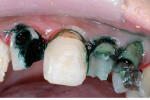
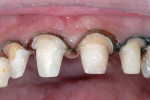
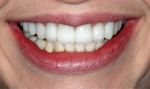
A young woman presented requesting cosmetic dental procedures, with the main goal of re-doing the bonding on her front teeth. She wanted her front teeth to be whiter and straighter, and for less gum tissue to show when she smiled (Figure 1 and Figure 2). She also experienced cold and spontaneous pain in several teeth, as a result of bleeding gums, food packing, and poor hygiene. A clinical examination revealed chronic gingivitis associated with poor restoration contours, recurrent decay, and minor attachment loss (Figure 3). Irreversible pulpitis was present on several teeth. She had no history of parafunctional habits, despite missing lower posterior teeth and exhibiting worn incisal tips on the upper cuspids.
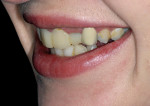
A natural side view revealed the extent of the cosmetic units needed to fulfill her esthetic desires (Figure 4). Review of the pretreatment images convinced her of the need for treating five teeth from the midline, in order to make a seamless transition between treated and non-treated teeth. Her “heightened sense of cosmetic need” led to her acceptance of a treatment plan that included fixing all of the porcelain crowns on teeth Nos. 4 through 13, multiple endodontic therapies, various direct composites, and a lower removable prosthesis. These images also dramatically reinforced the need for improved oral hygiene.
A thorough periodontal debridement along with low-wattage laser pocket microbe reduction was done during the preparation appointment. Gingival recontouring was also planned, with the presumption that only a closed, soft-tissue remodeling would be done. Because of the biologic limitations of closed diode laser reshaping, open-flap techniques were considered. The patient’s choice, however, is the ultimate deciding factor, as long as esthetic compromises are accepted by the patient and documented by the staff.10
Photographic uses during a cosmetic case should include the following:
- Case documentation
- Patient education and increased treatment awareness
- Case planning
- Soft and hard tissue preparation blueprint
- Lab communication
- Marketing
Planning for Tissue Preparation
Lasers have become a critical component of smile rehabilitations. If done with respect to periodontal tissues and biologic width, the results can be a great enhancement to cosmetic treatment.11,12 A variety of lasers and techniques have been widely reported on in the literature, with diode, erbium, and carbon-dioxide lasers capable of predictable results with esthetic recontouring. The 810-nm soft-tissue laser offers excellent control of tissue sculpting with very predictable healing and tissue tolerance.13 However, their ease of use must not tempt the clinician to disregard sound biologic principles.14
Biologic width is the sum of the two widths of connective tissue attachment and junctional epithelium superior to the alveolar boney crest. This length, the biologic width, is the zone of gingival attachment to the root surface of the tooth, and is about 2 mm on average. Superior to this is the gingival sulcus, which is on average 1 mm in healthy tissue. This total of 2-mm biologic width plus 1-mm sulcus depth results in about 3 mm needed for restoration margins to be away from the crest of bone.15 These principles must be understood during treatment in order to prevent possible chronic periodontal inflammation and unwanted gingival responses such as redness, bleeding, and irritation.16,17
Once the patient was clear on treatment limitations and expectations, digital photographs were studied in detail on a large monitor in a private area of the office. Treatment notes were made, with green marks placed for desired soft tissue changes, and blue lines drawn to denote the desired hard-tissue corrections (Figure 5, Figure 6, Figure 7, Figure 8 and Figure 9). These marks were “ideal,” and would be modified according to biologic principles.18
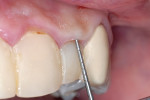
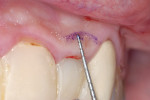
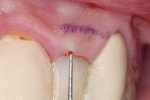
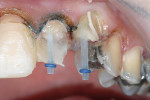
After local anesthetic was administered, the sulcus depths were measured. Great care was taken to record a firm measurement without violating the attachment to the tooth (Figure 10). These measurements were transferred to the gingival and marked with an indelible pen, so that the sulcus depth was easily identified from the facial view (Figure 11). The anatomy can be more accurately evaluated by probing through the periodontal attachment with a sharpened instrument—bone sounding—in order to locate the height of bone crest.19 The periodontal probe was then pushed through the attached tissue to the height of the buccal crest of alveolar bone, which measured about 5 mm (Figure 12).
In this case, about 3 mm of clinical crown length was needed on the facial of tooth No. 10 when looking at the photographs and preoperative measurements of the gummy smile. A probe to the bone revealed 5 mm from the gingival crest, with a sulcular depth of about 3 mm. Therefore, 2 mm of gingival tissue could be safely taken away for this tooth while keeping the restoration margin about 3 mm from the boney crest for uneventful healing. The patient’s decision to do conservative, non-boney lengthening—which was discussed before treatment to prevent postoperative disappointments—slightly compromised the final tissue position.
Tissue Preparation
For quick reference during preparation, the marked images were loaded onto the operatory computer at the preparation appointment. Doing so helps to keep the author on task and organized as tissue changes are made. After measuring sulcus depths, probing to the bone, and marking tissues according to ideal photographic changes, an 810-nm diode laser (Odyssey®, Ivoclar Vivadent, www.ivoclarvivadent.us) was used on a relatively low wattage (2W) to sculpt the tissues.20
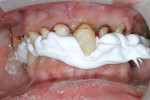
A direct composite mock-up was done freehanded with composite, with a height-to-width ratio of about 75%; an impression was done for laboratory consultation and temporization (Figure 13).21,22 The patient was sat upright in the chair and checked for midline and cant correction (Figure 14). Tissue charring was then cleaned up with hydrogen peroxide and gentle scrubbing with a microbrush. Preparations were then initiated, leaving one central unprepared tooth (Figure 15). This unprepared tooth allowed a positive anterior stop to be maintained while all of the other teeth were prepared and the bite registration was taken.
Old composite was removed and endodontic therapy was completed on four teeth. A caries indicator (Sable Seek®, Ultradent, www.ultradent.com) was used to verify caries removal (Figure 16). The teeth were etched and bonded, and tooth-colored posts (D.T. Light-Post®, BISCO, Inc, www.bisco.com) were luted into place. Build-ups were then done with a dual-cure composite material (Build-It® FR™, Pentron Clinical Technologies, www.pentron.com) (Figure 17). The remaining teeth were then finished with a minimum reduction of 1.5 mm and clear rounded shoulders, with the absence of sharp preparation corners.23 The extent of the finish lines for all of the restorations left at least 3 mm to the boney crest and a 1-mm sulcus in all areas. A bite registration was then taken (Figure 18).
The remaining central incisor was then prepared and restored. A retraction putty (Expasyl®, Kerr Corporation, www.kerrdental.com) was injected along the gingival margins, allowed to sit for 5 minutes, and then rinsed well (Figure 19). Two impressions were taken of the prepared teeth, using a polyvinyl impression material in a full-arch tray, and midline and occlusal plane guide sticks were used to take a polyvinyl bite registration. A self-curing automix composite was used to make temporaries in the patient’s desired shade for a transitional smile preview, and an impression was taken for laboratory communication. The patient was scheduled for follow up in 1 week.
The impressions, models, and bite registration were sent to the laboratory, along with all photographs taken before and during treatment, including preparation and accepted temporary shades.24 The images included shade tabs next to the preparations, which showed the final shade of the prepared teeth that the laboratory had to mask, in this case A2-A3. Pressed ceramic with a cutback and moderate irregular translucency was requested for its strength, beauty, and fit.25,26
Tissue Response
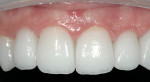
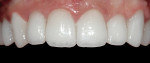
The crowns were tried in and cemented 3 weeks after tooth preparation. Four days after cementation, the patient returned for final clean-up and a postoperative check (Figure 20). Despite slight papilla blunting and redness, the tissues healed very well. The patient reported slight discomfort on the first day after preparation, but experienced no other pain afterwards. Excellent healing of the tissues was shown 3 weeks after cementation, and 6 weeks after tissue preparation showed great improvement in tissue color, bleeding, and adaptation to the restorations with improved hygiene (Figure 21). A lower removable prosthesis was also inserted to stabilize the occlusion.
As a result of proper patient care and adherence to fundamental tissue handling principles (Figure 22), the tissues responded very positively to the restorations, and the tissue improvements remained stable at more than 2 years postoperatively. An open-flap procedure could have improved the result by giving another 1 mm to 2 mm of length to tooth No. 10. The patient’s desires, however, prohibited that procedure (Figure 23). The violated biologic width could have been ignored, and the additional tissue could have been removed, but doing so could create chronic tissue problems in that area. Instead, a healthy and predictable result was achieved, which led to a very satisfied patient (Figure 24).
Disclosure
Jack D Griffin, Jr., DMD, has no financial interest in, or affiliation with, the products, materials, or suppliers used in this article.
Acknowledgment
The author would like to thank Adrium Jurim at Jurim Dental Studio for his cosmetic work.
References
1. Swift EJ Jr, Friedman MJ. Porcelain veneer outcomes, part II. J Esthet Restor Dent 2006;18:110-113.
2. Lee E. Laser-assisted gingival tissue procedures in esthetic dentistry. Prac Proced Asthet Dent. 2006;18(9 suppl):2-6.
3. Tipton, PA. Aesthetic tooth alignment using etched porcelain restorations. Pract Proced Asthet Dent. 2001;13:551-555.
4. Dumfahrt H. Porcelain laminate veneers. A retrospective evaluation after 1 to 10 years of service: Part 1—Clinical procedure. Int J Prosthodont. 1999;12:505-513.
5. Rossmann JA, Cobb CM. Lasers in periodontal therapy. Periodontol 2000. 1995;150-164.
6. Bittner RN. The periodontal factor in esthetic smile design-altering gingival display. Gen Dent. 2007;55(7):616-622.
7. Sadan A, Adar P. Esthetic proportions versus biologic width considerations: a clinical dilemma. J Esthet Dent. 1998;10(4):175-181.
8. Peumans M, Wan Meerbeek B, Lambrecht P, Vanherle G. Porcelain veneers: a review of the literature. J Dent. 2000;28:163-177.
9. Bassett JL. Replacement of missing mandibular lateral incisors with a single pontic all-ceramic prosthesis: A case report. Prac Peridodontics Aesthet Dent. 1997;9(4):455-461.
10. Sonick M. Esthetic crown lengthening for maxillary anterior teeth. Compend Contin Educ Dent. 1997;18(8):807-819.
11. Adams TC, Pang PK. Lasers in aesthetic dentistry. Dent Clin North Am. 2004;48(4):833-860.
12. Rice JH. Laser use in fixed, removable, and implant dentistry. Dent Clin North Am. 2000;44(4):767-777.
13. Coluzzi DJ. Fundamentals of dental lasers: science and instruments. Dent Clin North Am. 2004;48:751-770.
14. Kokich VG, et al. Gingival contour and clinical crown length: their effect on the esthetic appearance of maxillary anterior teeth. Amer J Orthod. 1994;86(2):89-94.
15. Yeh S, Andreana S. Crown lengthening: basic principles, indications, techniques and clinical case reports. NY State Dental J. 2004;70(8):30-36.
16. Padbury A Jr, Eber R, Wang HL. Interactions between the gingival and the margin of restorations. J Clin Peridontol. 2003;30(5):379-385.
17. Nemcovsky CE, Artzi Z, Moses O. Preprosthetic clinical crown lengthening procedures in the anterior maxilla. Prac Proced Aesthetic Dent. 2001;13(7):581-588.
18. Cunliffe J, Grey N. Crown lengthening surgery—indications and techniques. Dent Update. 2008;35(1):29-35.
19. Robbins JW. Esthetic gingival recontouring—a plea for honesty. Quintessence Int. 2000;31(8):553-556.
20. Press J. Effective use of the 810 nm diode laser within the wellness model. Prac Proced Asthet Dent, 2006;18(9 suppl):l8-21.
21. Blitz N, Steel C, Wilhite C. Principles of proportion and central dominance. Diagnosis and treatment evaluation in cosmetic dentistry. A guide to Accreditation Criteria. American Academy of Cosmetic Dentistry. 2000:16-17.
22. Mizrahi B. Visualization before finalization: A predictable procedure for porcelain laminate veneers. Prac Proced Aesthet Dent. 2005;17(8):513-518.
23. Sim C, Ibbetson R. Comparison of fit of porcelain veneers fabricated using different techniques. Int J Prosthod. 1993;6(1):36-42.
24. Griffin JG. How to build a great relationship with the laboratory technician: simplified and effective laboratory communications. Contemporary Esthetics and Restorative Practice. 2006;10(7):26-34.
25. Meijering AC, Roetas FJ, Mulder J, et al. Patient’s satisfaction with different types of veneer restorations. J Dent. 1997;25(6):493-497.
26. Hornbrook D. Invisible beauty: The ultimate in esthetic restorations. Contemporary Esthetics and Restorative Practice. 2005;9(12):14-23.
About the Author
Jack D. Griffin, Jr, DMD
Private Practice
Eureka, Missouri