Smile-Design Case Planning Using Conservative Treatment Modalities
Case selection is critical to the functional and esthetic success of minimal-preparation veneers.
By Jason Olitsky, DMD
Patient demand for conservative cosmetic smile enhancements appears to be on the rise. Much of this demand is driven by the manufacturers and laboratories with consumer-based marketing of “no prep” veneers. With newfound awareness and loaded with marketing propaganda, patients are seeking smile enhancements that avoid the preparation of tooth structure without understanding the potential compromises to the final results. More often, we are encountering patients who share feelings during their consultations about wanting to make improvements to their smile, but are afraid that they will not look like themselves after the treatment. They are also concerned about having their teeth drilled down to “pegs” after hearing about negative experiences from friends and family. Patient and dentist demands have required innovation within laboratories to create thinner, more lifelike restorations to meet these new patient demands without sacrificing ultimate esthetics. To confidently and consistently improve smiles for all types of patients requires that the clinician stay in control of the smile-design process and work with a laboratory that can consistently deliver those results. Using conservative treatment modalities also requires unique skills in case planning.
Case selection is critical to the functional and esthetic success of minimal-preparation veneers. Teeth that are small, have incisal edge wear, small spaces, collapsed buccal corridors, and are slightly deflective make great restorative candidates for minimal- or no-preparation veneers. Teeth that are buccally displaced or in a severely lingualized position, are flared out incisally creating open gingival embrasures, or have obvious rotations or canted axial inclinations make poor candidates for minimal- or no-preparation veneers (Table).1 It is important to remember that not every tooth being restored in a smile needs to be minimal or no-preparation in order to use the treatment modality. For example, when designing a smile, bicuspids make great teeth for minimal- or no-preparation veneers when filling out a deficient buccal corridor, which can be achieved with direct or indirect veneering options, which creates more affordable options for the patient. Also, if teeth are in poor restorative positions for conservative veneers, they can be moved orthodontically into better positions before preparation for the final restorations.2
No-preparation veneers have been in the dental marketplace for more than two decades. The author’s opinion is that the addition of restorative material on a properly contoured natural tooth in proper alignment leads to the overcontouring of the tooth, resulting in a bulky result. This type of treatment leads to an unnatural-looking restoration, and excessive plaque and food accumulation that results in gingivitis. Minimal preparation has a broader range of clinical practicality and requires the clinician to understand the capabilities of ceramic restorations. Smaller amounts of tooth structure can be removed on teeth with proper anatomical contours and replaced with restorative ceramics of the same thickness. The use of an additive-reductive mock-up or wax-up allows the practitioner to set up a case by visualizing the end result.
Having more detailed communication with the laboratory enables the dentist to create provisionals for the patient that are prototypes of their final restorations both esthetically and functionally. The process of fabricating veneer provisionals is often listed as a negative when promoting the two-visit approach to no-preparation veneers, but it can be a very important part of visualizing the end result with the patient. While there are certainly advantages to being “quick and easy,” such as needing less communication with the laboratory when performing minimal- or no-preparation veneers, the practitioner gives up the ability to design the smile. There are several types of patients who are interested in cosmetic dentistry, some are easy to please and some require more time and attention to the smile-design process. Employing techniques that are “quick and easy” may not prepare the practitioner for all types of cosmetically driven patients who request cosmetic dentistry. Proper communication with the laboratory includes impressions, bite records, facebow jigs, a stick bite, a photographic series, shades, and detailed prescriptions on porcelain characteristics.1,3 There are increasingly more options in laboratory selection for the fabrication of minimal- and no-preparation porcelain veneers. There is no one perfect material for all situations. When choosing a material, the laboratory technician’s experience is important as well as the condition and shades of the teeth being restored.4
Pressed leucite-reinforced ceramics have the advantages of strength,5,6 ability to see final contours before fabricating in porcelain, marginal fit,7-10 and wear compatibility.11 Using a laboratory that is capable of cutting back and layering during the fabrication of both traditional and minimal-thickness pressed-ceramic restorations gives the practitioner more options when designing beautiful and natural-looking smiles. In one fabrication process, the laboratory presses the ceramics at a thickness of 0.7 mm, at which time the incisal edges are cut back and layered for effects. The ceramist then thins the restoration with the ability to check the thickness of the restoration throughout the fabrication process. One such technique has been developed by Gold Dust Dental Laboratory in Tempe, Arizona, to create an Emprethin™ veneer (Gold Dust Dental Lab, www.emprethin.com) a polychromatic 0.2-mm thin, cut back, and layered IPS Empress® veneer, which is detailed in this article.
Case Report
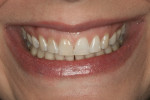
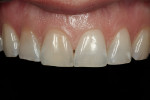
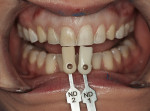
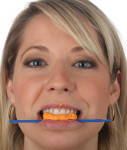
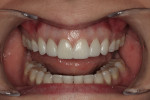
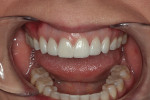
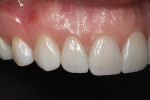
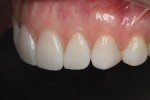
A 32-year-old woman presented to the office for a cosmetic consultation after initiating treatment at another dental office for porcelain veneers. She was in excellent health. She had no caries and good home care. She had moderate posterior wear and incisal wear of the maxillary anterior teeth. Her goal was to add back the length of her front teeth that she had worn off and make all the front teeth match as two of the teeth in her smile had darkened from previous root canal therapy (Figure 1 and Figure 2). She also wanted whiter teeth.
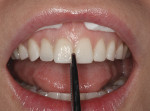
In this particular circumstance, a direct intraoral mock-up made more sense than fabricating a wax-up. When making minor changes to a smile, it can be easier, as well as less time-consuming and cost-effective, to mock up the new smile rather than order a wax-up. The mock-up was created by simply adding additional length to the anterior teeth intraorally with resin material and making some other small changes to the alignment and shape of the teeth.12 Tetric EvoFlow® (Ivoclar Vivadent) shade A1 was used as the mock-up material for this case. The maxillary anterior teeth were dried thoroughly and the resin was added in small increments, then cured for 20 seconds with a bluephase 20i LED curing light (Ivoclar Vivadent) and contoured with fluted carbides and an Enhance® cup (DENTSPLY, www.dentsply.com). Approaching the planning aspect of her new smile from this perspective was in line with the patient’s expectations for her new smile (Figure 3).
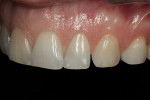
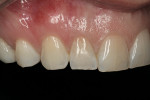
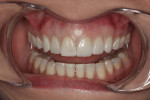
As stated previously, when the patient was seen for her initial consultation with this author, she had already been to another dentist who was unable to make her happy using an intraoral mock-up fabricated from a template of a laboratory wax-up of teeth Nos. 5 through 12. During her initial consultation, a photographic series was taken in the studio where full-face and 1:1 front, left, and right lateral shots were taken to evaluate the smile with the patient on the computer (Figure 4, Figure 5, Figure 6). After her smile was evaluated it was decided what the best treatment would be and what options were available to her to best achieve her goals.
To meet this particular patient’s goals, it was decided that she would be best served with six Emprethin restorations on teeth Nos. 6 through 11 to correct the value discrepancies of the natural teeth, as well as to restore the worn incisal edges and correct the alignment. The first bicuspids would be treated with direct-resin veneers (Renamel Universal and Microfill, www.cosmedent.com) to match the anterior and transition color to the posterior for a natural effect, because she did want whiter teeth. The cost of porcelain restorations are substantially more than direct-resin veneers, and using direct veneers as a conservative treatment modality on her bicuspids helped lower her costs. Her occlusion would also be evaluated and treated for the presence of posterior interferences to centric relation that could be the source for the tooth wear in the anterior as well as working and non-working interferences.13 The patient was hesitant to again pursue veneers, as her last experience with the wax-up was negative; however, the patient allowed the author and his team to do an additive intraoral mock-up using a flowable composite. About 0.75 mm of length to the four upper incisors was added and some of the tooth wear on the tips of the maxillary canines was corrected. The laterals were brought out slightly facially to correct the alignment. No resin was added to the bicuspids at this time and very little resin was added to the facials of the centrals or canines. The patient was allowed to stand up and evaluate the intraoral mock-up in several mirrors for perspective. Her full-face photograph was taken in the studio to compare to her “before” photograph taken at the beginning of her appointment. The intraoral mock-up was effective in building confidence by making an already skeptical patient instantly happy. An impression of the mock-up was taken with a full-arch triple tray. The teeth were lined with fast-setting Virtual® Light Body impression material (Ivoclar Vivadent) and the tray was filled with Clear Bite (Discus Dental, www.discusdental.com) for the maxillary and mandibular teeth. The tray was allowed to sit for 3 minutes, removed, and checked for accuracy, then saved for the patient’s preparation appointment.
At the preparation appointment, the impression taken with the triple tray was then used to transfer the intraoral mock-up to the patient’s mouth. The impression was filled with Luxatemp (DMG America, www.dmg-america.com) in shade BL and seated back into the patient’s mouth. After 2 minutes, the tray was removed and the flash from the transfer of the intraoral mock-up was removed quickly before final set. The new mock-up was used as a definitive goal for the smile. A 0.3-mm reduction bur was used on the incisal, middle, and gingival thirds of the anterior six teeth. The incisal reduction was done using a Brasseler 856L 016 bur (Brasseler USA, www.brasselerusa.com) horizontally removing 1.5 mm of mock-up material and tooth on the anterior six teeth. Because length was added, less than 1 mm of actual incisal edge of the tooth was removed. For the laboratory to cut back and layer incisal effects into the porcelain, appropriate space is required. The teeth were prepared by removing the reduction lines facially and incisally and placing margins. The margins were placed supragingivally and only deep enough to allow the ceramist to read a definitive finish line. Interproximal contacts were not broken during preparation. The color of the preparations was evaluated, and it was determined to prepare slightly more into the facials of teeth Nos. 7 and 8, because they were considerably darker than the other preparations as a result of their previous root canal treatment. They were then opaqued with Renamel A1/B1 opaquer to more closely match the other prepared teeth (Figure 7). This step is crucial in matching the thin-pressed veneers, as the resultant thin-pressed ingots will allow more show-through of the underlying preparation. The teeth were impressed using full-arch impressions using Virtual Heavy Body Fast Set and the teeth were lined with Virtual Light Body Fast Set. The lower teeth were also impressed with heavy body lined with light body, and a bite was taken of the preparations in full occlusion using a polyvinyl impression material.
The provisional restorations were made by again using the triple tray of the intraoral mock-up filled with Luxatemp in BL shade. The patient was allowed to see and approve the look of the provisionals, then an impression was taken of the provisionals for laboratory communication and mounting. A centric occlusion bite was taken using polyvinyl material and a Panadent earless facebow (Panadent, www.panadent.com) was taken in the photography studio as well as a stick bite for reference (Figure 8 and Figure 9).
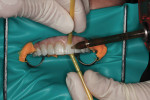
The patient returned for the cementation approximately 3 weeks later. The provisionals were removed with a straight hemostat placed interproximally to fracture the connection between the individual teeth, making them easy to remove (Figure 10). Because the patient really liked her provisionals, only half of them were removed and ceramic restorations were tried on over that half to compare the provisionals and ceramics. The two sides looked nearly identical in length and shape, showing that the laboratory did a great job of following the provisionals (Figure 11). The rest of the provisionals were removed and each veneer was tried on individually as well as two by two to check fit and contacts. It is crucial to evaluate tight contacts at this point no matter how slight, as opposed to when cementing in the restorations, to prevent the unintentional minor underseating of a veneer. This can be observed many times in smiles with two centrals that are not perfectly even at the incisal edge, or a lateral that is unintentionally slightly off in axial inclination. These thin veneers are 0.2-mm to 0.3-mm thick and must be handled even more delicately than traditional veneers. It is important to have good protocols in place for passing veneers between assistants and doctors.
The ceramics were placed with try-in paste and evaluated for shade. Despite the opaquer used over the darker preparations, there was still a slight variation in shades at try-in when one color try-in paste (Variolink® Veneer, Ivoclar Vivadent) was used for all six restorations (Figure 12). Traditionally, when using different color try-in pastes, they tend to have a smaller effect on the final restorations’ color, but when using thin veneers as a restorative option, try-in gels have a much more significant effect on the overall color of the tooth.14,15 The veneers were tried in over the darker teeth with different color try-in gels, first +1, then +2. It was decided that +1 and +2 would be mixed for the most ideal color match (Figure 13). Patients who are the most critical of the final results appreciate this attention to detail.
Teeth Nos. 3 through 14 were isolated using a split rubber-dam technique while the veneers were ebeing prepared by the assistant. The palate was blocked out with polyvinyl bite material and the teeth were cleaned and rinsed thoroughly. The teeth were cleaned with Consepsis® (Ultradent, www.ultradent.com) and rinsed off.16 Sulcular fluid and bleeding were not a concern, the patient had good home care, had followed instructions, and the preparations were all supragingival. Then the teeth were etched for 15 seconds using Ultra-Etch® (Ultradent) three teeth at a time to ensure proper etch time. The etch was rinsed and the teeth were dried with light air until visible drops of moisture were absent.17 The teeth were then coated with two layers of Telio® CS Desensitzer (Ivoclar Vivadent). The excess desensitizer was suctioned off using the high-speed vacuum. Next, ExciTE® Unidose (Ivoclar Vivadent) was applied to each tooth in two layers for about 20 seconds per tooth. The ExciTE was air-dried with a warm air-dryer toward the gum line until there was a shiny surface that did not move when the air hit the tooth. Each tooth was then light-cured for 10 seconds per surface with the bluephase 20i LED curing light.
The veneers were prepared by cleaning with 37% phosphoric etch and rinsing and drying. The internal aspect of the veneers were then coated with silane and allowed to air-dry for 60 seconds. ExciTE was then placed internally and coated evenly, then air-dried with the warm air-dryer until visible moisture was gone and the internal surface was shiny. The six veneers were loaded with the proper color of Variolink Veneer cements, taking care to match the correct cement color into the proper veneer, then the veneers were placed into a light protective box and taken to the treatment room for cementation.
The veneers were placed on the teeth in the same order they were tried in the mouth. First, the centrals were placed and confirmed to be properly seated by standing up and visualizing them from the front of the patient. Next, the laterals were placed, followed by the canines. Careful seating is paramount for the thin veneers. Too much pressure during seating from the facial direction can easily cause a fracture. The author applied pressure from the incisal direction and facial direction using the ends of a microtip brush, while the assistant “tacked” the veneer in the dead center of the tooth with the bluephase 20i LED curing light and a 2-mm tacking light (Figure 14). The assistant then changed lights to one with an 8-mm tip and waved first the facial, then lingual surfaces, for approximately 3 seconds facially and 3 seconds lingually from about 3 inches away. The excess cement was then in a gel state and easily removed using the instrument. The veneers were then flossed to remove interproximal excess cement. The veneers were then final-cured for 40 seconds per surface. After rinsing and cleaning the teeth, instead of removing the rubber dam, the first bicuspids were treated for direct-resin veneers.
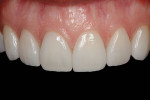
Teeth Nos. 5 and 12 were treated individually. Each were etched for 30 seconds, then rinsed with water. ExciTE bonding agent was placed in two coats and applied for 20 seconds, then air-thinned with the warm air-dryer and cured for 10 seconds. Renamel Universal shade B1 was placed on the incisal edge to build the incisal shape of the resin veneer in the hybrid material. Once the incisal shape was built and cured for 40 seconds, a layer of Renamel Microfil B1 was placed and sculpted into place with IPC instruments. The material was carefully taken back interproximally into the elbows and down to the gum line to completely cover the underlying enamel. Once the final shape was achieved, the resin was light-cured with the bluephase 20i LED curing light for 40 seconds. The microfill was then finished and polished using fluted carbides, then Enhance cups and PoGo® cups (DENTSPLY), then polished with Enamelize (Cosmedent) on a brush.18 The rubber dam was then removed and the final restorations were adjusted for occlusion and polished (Figure 15, Figure 16, Figure 17).
The patient returned one week later for a postoperative appointment. She confirmed how happy she was with the final result. Her studio headshot was taken (Figure 18) prior to being seated in the treatment room where final intraoral photographs where taken and all margins were checked for any excess cement and a final polish. Her bite was evaluated with a T-Scan® III (Tekscan, www.tekscan.com) to confirm that she had balanced occlusion and no prematurities in contact that could potentially harm her new restorations.19
It is common that individual cases requiring variations to typical smile-design protocols enter our offices. Wax-ups are routinely ordered in the office to visualize the end results of smile designs and full-mouth rehabilitations, especially when making considerable changes to the smile and occlusion. Intraoral mock-ups can be a great option for patients who require fewer modifications to their existing smiles to make them happy and still allow for the envisioning of the final results before preparing the teeth. Emprethins are a viable option for patients who require minimal conservative techniques for the best results. Emprethins were shown here in a minimal-preparation technique, but they can also be used in no-preparation techniques when teeth need to be enhanced slightly in size and length for the patient when indicated. Instead of treating this patient with more traditional veneering options, we were able to meet her goals and make her happy with conservative treatment modalities.
References
1. Hornbook D. Prepless and minimal prep veneers. Hornbrook Clinical Excellence Through Education DVD. 2011
2. Smallwood TW. Invisalign and porcelain: the contemporary restorative powerhouse. Alpha Omegan. 2009;102(4):148-151.
3. Terry DA, Moreno C, Geller W, Roberts M. The importance of laboratory communication in modern dental practice: stone models without faces. Pract Periodontics Aesthet Dent. 1999;11(9):1125-1132.
4. Spear F, Holloway J. Which all-ceramic system is optimal for anterior esthetics? J Am Dent Assoc. 2008;139(suppl):19S-24S.
5. Dong JK, Luthy H, Wohlwend A, Scharer P. Heat-pressed ceramics: technology and strength. Int J Prosthodont. 1992;5(1):9-16.
6. Sorensen JA, Choi C, Fanuscu MI, Mito WI. A clinical trial of all-ceramic crown restorations: status, fall 1995. Signature. 1997;4(3 suppl):14-19.
7. Orkin DA, Reddy J, Bradshaw D. The relationship of the position of crown margins to gingival health. J Prosthet Dent. 1987;57(4):421-424.
8. Schatzle M, Land NP, Anerud A, et al. The influence of margins of restorations of the periodontal tissues over 26 years. J Clin Periodontol. 2001;28(1):57-64.
9. Ferrari M, Mannocci F, Mason PN, Kugel G. In vitro leakage of resin-bonded all-porcelain crowns. J Adhes Dent. 1999;1(3):233-242.
10. Celik C, Gemalmaz D. Comparison of marginal integrity of ceramic and composite veneer restorations luted with two different resin agents: an in vitro study. Int J Prosthodont. 2002;15(1):59-64.
11. Fradeani M, Redemagni M, Corrado M. Porcelain laminate veneers: 6- to 12-year clinical evaluation—a retrospective study. Int J Periodontics Restorative Dent. 2005;25(1):9-17.
12. Reshad M, Cascione D, Magne P. Diagnostic mock-ups as an objective tool for predictable outcomes with porcelain laminate veneers in esthetically demanding patients: a clinical report. J Prosthet Dent. 2008;99(5):333-339.
13. Wood WW. A review of masticatory muscle function. J Prosthet Dent. 1987;57(2):222-232.
14. Vichi A, Ferrari M, Davidson CL. Influence of ceramic and cement thickness on the masking of various types of opaque posts. J Prosthet Dent. 2000;83(4):412-417.
15. Probster L, Geis-Gerstorfer J, Kirchner E, Kanjantra P. In vitro evaluation of a glass-ceramic restorative material. J Oral Rehabil. 1997;24(9):636-645.
16. Moon PC, Weaver J, Brooks CN. Review of matrix metalloproteinases’ effect on the hybrid dentin bond layer stability and chlorhexidine clinical use to prevent bond failure. Oper Dent J. 2010;4:147-152.
17. Dunne SM, Millar BJ, Davies B. A survey of dental airlines and an examination of tooth drying techniques. Prim Dent Care. 1996;3(2):61-64.
18. Mopper KW. Contouring, finishing, and polishing anterior composites. Inside Dentistry. 2011;7(3):62-70.
19. Cranham JC. Optimum dental care, Part 3. Case finishing. Dent Today. 2003;22(5):78-83
About the Author
Jason Olitsky, DMD
Clinical Adjunct Faculty
Arizona School of Dentistry and Oral Health
Mesa, Arizona
Faculty Mentor
The Clinical Mastery Series