Esthetic Connective Tissue Grafting of Multiple Recession Sites
An acellular dermal matrix is a valuable tool in the treatment of gingival recession.
By Douglas H. Mahn, DDS
Gingival recession represents a significant problem in the esthetic zone. Autogenous connective tissue grafts have been considered the gold standard, but are limited by the availability of tissue that can be derived from the patient’s palate. Acellular dermal allografts are useful in the treatment of gingival recession defects, and are not as limited in availability as the patient’s own tissue. Reflection of an envelope flap can lead to shrinkage of the interdental papillae, and reduces the esthetic benefits of grafting. Tunnel techniques are one method of protecting the papillae and improving esthetics. The purpose of this article is to demonstrate and discuss the use of the tunnel technique and an acellular dermal matrix in the treatment of multiple adjacent gingival recession sites.
An attractive smile is the result of a harmonious relationship between the teeth and the gingiva. Proper tooth size and tooth-to-tooth proportion are dependent on the gingival architecture.1 Gingival recession represents an important challenge in creating a natural looking smile. Methods to cover root surface must yield results that do not create unintended problems such as blunting of the interdental papillae.
The subepithelial connective tissue graft (CTG) was first described as a method to enhance anterior cosmetics.2,3 Connective tissue grafting with an “envelope” technique was developed to achieve root coverage on a single tooth, without the problems associated with vertical incisions.4 Tunnel techniques were developed to improve the esthetic results for treatment of multiple adjacent recession sites.5-10
The benefits derived from CTGs are limited by the amount that can be harvested from the patient’s palate.11,12 An acellular dermal matrix (ADM) being derived from an organ donor’s skin does not have this limitation.13-15 ADMs have been highly successful in the treatment of gingival recession.16-23 ADMs permit the treatment of multiple teeth in a single visit.16,20,23 Its uniform thickness also makes ADMs simple to use with tunnel techniques.18,19,22,23
Case Report
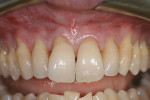
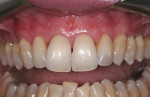
A 48-year-old female non-smoker reported “ugly and long teeth” as a chief concern. Teeth Nos. 5 through 12 were found to have Miller Class III gingival recession. The range of recession was between 2 mm and 4 mm with interdental attachment loss24 (Figure 1). After discussing the findings and treatment plan options, it was agreed to treat these teeth with connective tissue grafting.
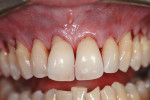
Profound local anesthesia was achieved using approximately 9 cc of 2% lidocaine with 1:100,000 epinephrine. Intrasulcular incisions were made along the facial surfaces of teeth Nos. 4 through 13 using a Bard-Parker #15 blade (Figure 2). Leaving the interdental papillae intact, an Orban knife was used to raise a full-thickness flap. Between teeth Nos. 5 and 6 and 11 and 12 were the only areas in which the facial gingiva detached from the underlying interdental papillary bed. Individual pouches adjacent to each tooth were extended beneath the mucogingival tissues until a continuous tunnel extended from teeth Nos. 5 through 12. Root planing using curettes was performed to reduce root prominences and smooth root surfaces.
An ADM (AlloDerm® Regenerative Tissue Matrix, BioHorizons, www.biohorizons.com) was trimmed to approximately 5 mm in height and 40 mm in length (Figure 3). Using the Orban knife, the ADM was then inserted into the mucogingival tunnel between teeth Nos. 5 and 6, and pushed/pulled through to site No. 12.
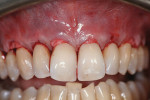
The ADM was secured over the root surfaces using a continuous 4.0 plain-gut suture (Figure 4). The gingiva was then positioned completely over the ADM and secured in a coronal position using a continuous 4.0 chromic-gut suture (Figure 5).
The patient was given postoperative instructions, including the use of ibuprofen (600 mg) for discomfort. The patient was prescribed amoxicillin (875 mg) q12 h for 10 days. The patient was also instructed not to brush or floss the surgical site for 10 days. Instead, she was to rinse twice daily with 0.12% chlorhexidine gluconate (Peridex®, Proctor & Gamble, www.pg.com). After 10 days, the patient was instructed to discontinue the rinse and begin gentle toothbrushing and flossing.
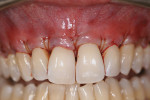
Approximately 12 weeks after surgery, the treatment sites were found to be healing well,with complete root coverage (Figure 6). No additional blunting of the interdental papillae was found. The overall appearance of the soft tissue architecture was natural and healthy; the mucosa exhibited a thicker and pinker appearance.
Discussion
Tunnel techniques represent an important advancement in the esthetic correction of gingival recession. While the anterior gingiva receive their major source of blood perfusion from an apicocoronal direction, circulation is compromised where incisions are made.25,26 Therefore, keeping the interdental papillae intact fosters improved circulation and preservation of esthetics.27,28 In addition, the tunnel technique has been shown to be effective in treating multiple Miller Class III gingival recession sites.29 Some studies show, however, that the tunnel technique may not be as effective in achieving root coverage as with conventional flap designs.30 One explanation for this is that the tunnel procedure is highly technique-sensitive and developing adequate flap mobility is more difficult.
Positioning of the CTG into the mucogingival tunnel can be done using different methods. One method is to use the limited space provided adjacent to an individual tooth.4-6 This can be difficult, however. The interdental papillae or marginal gingiva, having minimal attached keratinized gingiva, can inadvertently tear. Secondly, the gingival flap can be detached from the interdental papillae at a site that is not esthetically critical.8,23 This is typically at the most distal site. Enlarging access space to the tunnel facilitates placement of a graft with increased dimensions. The detached area is sutured into position after graft placement. A third method creates access to the tunnel by making vertical incisions into the mucosa. All of the interdental papillae are left intact.18,19 This vertical access greatly facilitates graft placement. After the graft and gingiva are secured in position, the vertical incisions must then be sutured closed. For this case, the second method was deemed the least invasive, yet adequate for proper graft placement.
CTGs have provided excellent results in the treatment of gingival recession.2-10 However, the amount of palatal tissue that can be harvested from the patient is limited.11-12 This can make treating multiple teeth in a single appointment difficult. The palatal donor site has also been associated with postoperative discomfort.31,32 ADMs are derived from the skin of organ donors.13-15 They have also yielded excellent results in the treatment of gingival recession.16-23 Unlike CTGs, the availability of ADMs is not limited by the palatal anatomy, and is not a source of palatal postoperative pain.
The processing of ADMs removes their cellular component while maintaining the ultrastructural acellular matrix. ADMs are cut into pieces with a uniform thickness between 0.89 mm to 1.65 mm. The undamaged collagen and elastin matrices do not initiate an inflammatory response. Cellular repopulation and revascularization occurs through preserved vascular channels.13-15,17 ADM must be in direct contact with vital tissue in order to revascularize. Therefore, ADM overlying root surfaces must be completely covered by the gingival flap to survive.13-15,21
The successful treatment of gingival recession sites using ADMs has been shown to be predictable.16,17,21,22 Similar results in root coverage have been found when using ADMs and CTGs. A significant advantage of ADMs is that its availability is not limited by palatal anatomy. This makes the treatment of multiple teeth in a single visit practical.16,20,23 It also eliminates the discomfort associated with the palatal wound. Its uniform dimensions make ADMs simple to use with tunnel techniques and, therefore, an excellent choice for use with cosmetic surgical procedures.18,19,22,23
Finally, one study compared the results of ADMs used with a coronally positioned tunnel versus a coronally positioned flap.33 While not statistically significant, the coronally positioned flap procedure had better root coverage. It was also the strong clinical impression among the researchers, however, that the tunnel group patients experienced much less postoperative pain. Therefore, it was concluded that, while modifications were needed to improve predictability, the use of ADM with a coronally positioned tunnel was a valuable treatment option.
Conclusion
Tunnel techniques can be effectively used to esthetically treat gingival recession sites. The use of ADMs permits these techniques to be used on multiple adjacent recession sites in a single visit.
References
1. Ohyma H, Nagai S, Tokutomi H, Ferguson M. Recreating an esthetic smile: A multidisciplinary approach. Int J Periodontics Restorative Dent. 2007;27(1):61-69.
2. Langer B, Calagna L. The subepithelial connective tissue graft: A new approach to the enhancement of anterior cosmetics. Int J Periodont Rest Dent. 1982;2(2):22-33.
3. Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56(12):715-720.
4. Raetzke PB. Covering localized areas of root exposure employing the “envelope” technique. J Periodontal. 1985;56(7):397-402.
5. Allen AL. Use of a supraperiosteal envelope in soft tissue grafting for root coverage. I. Rationale and technique. Int J Periodont Rest Dent. 1994;14(3):216-227.
6. Allen AL. Use of a supraperiosteal envelope in soft tissue grafting for root coverage. II. Clinical results. Int J Periodont Rest Dent. 1994;14(4):302-315.
7. Zaballegui I, Sicilia A, Cambro J, et al. Treatment of multiple adjacent gingival recessions with the tunnel subepithelial connective tissue graft: a clinical report. Int J Periodont Rest Dent.1999;19(2):199-206.
8. Santarelli GA, Ciancaglini R, Campanari F, et al. Connective tissue grafting employing the tunnel technique: a case report of complete root coverage in the anterior maxilla. Int J Periodont Rest Dent. 2001;21(1):77-83.
9. Vergara JA, Caffesse RG. Localized gingival recessions treated with the original envelope technique: a report of 50 consecutive patients. J Periodontol. 2004;75(10):1397-1403.
10. Ribeiro FS, Zandim DL, Pontes AEF, et al. Tunnel technique with a surgical maneuver to increase the graft extension: case report with a 3-year follow-up. J Periodontol. 2008;79(4):753-758.
11. Studor SP, Allen EP, Rees TC, Kouba A. The thickness of masticatory mucosa in the human hard palate and tuberosity as potential donor sites for ridge augmentation procedures. J Periodontol. 1997;68(2):145-151.
12. Monnet-Corti V, Santini A, Glise JM, et al. Connective tissue graft for gingival recession treatment: assessment of the maximum graft dimensions at the palatal vault as a donor site. J Periodontol. 2006;77(5):899-902.
13. Wainwright D, Madden M, Luteman A, et al. Clinical evaluation of an acellular allograft dermal matrix in full-thickness burns. J Burn Care Rehabil. 1996;17(2):124-136.
14. Rhee PH, Friedman CD, Ridge JA, Kusiak J. The use of processed allograft dermal matrix for intraoral resurfacing: An alternative to split-thickness skin grafts. Arch Otolaryngol Head Neck Surg. 1998;124(11):1201-1204.
15. Livesey S, Herndon DN, Hollyoak MA, et al. Transplanted acellular allograft dermal matrix. Potential as a template for the reconstruction of viable dermis. Transplantation. 1995;60(1):1-9.
16. Henderson RD, Greenwell H, Drisko C, et al. Predictable multiple site root coverage using an acellular dermal matrix allograft. J Periodontol. 2001;72(5):571-582.
17. Aichelmann-Reidy ME, Yukna RA, Evans GH, et al. Clinical evaluation of acellular allograft dermis for the treatment of human gingival recession. J Periodontol. 2001;72(8):998-1005.
18. Mahn DH. Treatment of gingival recession with a modified “tunnel” technique and an acellular dermal connective tissue allograft. Pract Proced Aesthet Dent. 2001;13(1):69-74.
19. Mahn DH. Esthetic correction of gingival recession using a modified tunnel technique and an acellular dermal connective tissue allograft. J Esth Rest Dent. 2002;14(1):18-23.
20. Mahn DH. The treatment of multiple sites of gingival recession in a single visit using an acellular dermal connective tissue allograft. A case report. VA Dent J. 2002;79(1):7-10.
21. Felipe ME, Andrade PF, Grisi MF, et al. Comparison of two surgical procedures for the use of the acellular dermal matrix graft in the treatment of gingival recessions: A randomized controlled clinical study. J Periodontal. 2007;78(7):1209-1217.
22. Papageorgakopoulos G, Greenwell H, Hill M, et al. Root coverage using acellular dermal matrix and comparing a coronally positioned tunnel to a coronally positioned flap approach. J Periodontol. 2008;79(6):1022-1030.
23. Mahn DH. The use of the tunnel technique and an acellular dermal matrix in the treatment of multiple adjacent teeth with gingival recession in the esthetic zone. Int J Periodont Rest Dent. 2010;30(6):593-599.
24. Miller PD. A classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985;5(2):8-13.
25 Mormann W, Ciancio SG. Blood supply of human gingival following periodontal surgery—A fluorescein angiographic study. J Periodontal. 1977;48(11):681-692.
26 Mormann W, Meier C, Firesone A. Gingival blood circulation after experimental wounds in man. J Clin Periodontal. 1979;6(6):417-424.
27. Zuhr O, Fickl S, Wachtel H, et al. Covering of gingival recessions with a modified tunnel technique. Case Report. Int J Periodontics Restorative Dent. 2007;27(5):457-463.
28. Salama H, Salama M, Garber D. The tunnel technique in the periodontal plastic treatment of multiple adjacent gingival recession defects: A review. Inside Dentistry. 2008;4(9):78-81.
29. Aroca S, Tibor K, Nikolidakis D, et al. Treatment of class II multiple gingival recessions: A randomized-clinical trial. J Clin Periodontol. 2010;37(1):88-97.
30. Papageorgakapoulos G, Greenwell H, Hill M, et al. Root coverage using acellular dermal matrix and comparing a coronally positioned tunnel to a coronally positioned flap approach. J Periodontol. 2008;79(6):1022-1030.
31. Del Pizzo M, Modica F, Bethaz N, et al. The connective tissue graft: A comparative clinical evaluation of wound healing at the palatal donor site. A preliminary study. J Clin Periodontol. 2002;29(9):848-854.
32. Griffin TJ, Cheung WS, Zavras AI, Damoulis PD. Postoperative complications following gingival augmentation procedures. J Periodontol. 2006;77:2070-2090.
33. Tal H, Moses O, Zohar R, et al. Root coverage of advanced gingival recession: A comparative study between acellular dermal matrix allograft and subepithelial connective tissue grafts. J Periodontol. 2002;73(12):1405-1411.
About the Author
Douglas H. Mahn, DDS
Private Practice
Manassas, Virginia