Clinical Application of Probiotic Therapy
New adjunctive therapies offer new alternatives for treatment.
Numerous studies have researched the oral biofilm to determine the pathogenicity of specific bacteria.1-3 Now, dental researchers are looking for which bacteria, if present in large quantities, prevents the development of a pathogenic oral biofilm.4 The practitioner may then successfully modify the oral biofilm by targeting specific patients and their specific areas of concern (periodontal disease, dental caries, etc).5 By using the appropriate probiotic, there may be a method of supplementing the oral environment with beneficial bacteria to create a healthy oral biofilm and, ultimately, prevent dental disease.6
The difference between a diseased and a healthy oral condition appears not only to be related to the presence of oral pathogens but also to the level of "healthy" bacteria.4 The oral flora of young children who do not develop pathology contains a number of inhibitory bacteria. Based on this concept, Oragenics, Inc. has introduced EvoraKids™ and Evora Plus™ with a proprietary mixture (ProBiora3™) containing three GRAS (generally recognized as safe) probiotics; Streptococcus rattus JH145, Streptococcus oralis KJ3, and Streptococcus uberis KJ2. These low-acid–producing oral inhabitants quickly colonize the oral cavity to inhibit the growth of the pathogenic streptococci strains.7 Streptococcus oralis KJ3 also produces hydrogen peroxide to inhibit adjacent pathogenic bacteria by oxygenating the plaque. A probiotic mouthwash with ProBiora3, a mixture of the three previously mentioned bacteria strains, has been demonstrated as safe in the laboratory rat model.8,9
The introduction of probiotics into dentistry means that the profession should now consider the entire biofilm complex instead of just the pathogen-specific model of plaque.10 Previous considerations were to mainly focus on the specific pathogens, such as mutans streptococci and the Lactobacillus genus.11 Hence, tests were designed to measure the presence of these two "pathogens" (CRT® bacteria, Ivoclar Vivadent, www.ivoclarvivadent.com). But these bacteria are not the only causative agents; they are perhaps just markers of a pathogenic biofilm.12,13 Focusing on the genesis of the unhealthy oral biofilm will enable the practitioner to prevent or treat a host of oral pathologies and related systemic disorders.10
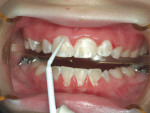
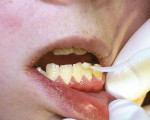
The patient's oral hygiene practices should be thoroughly reviewed, a complete oral prophylaxis should be performed, and Cervitec Plus™ (Ivoclar Vivadent) varnish applied to reduce the level of the oral pathogens.14-16 Then, the presence of any oral disease—either carious lesion or periodontal in nature—should be an indication for the initiation of probiotic therapy (Figure 1, Figure 2, Figure 3 and Figure 4).17-21
Conclusion
Probiotics have been extensively studied in the medical literature and dental reports are very encouraging. Indeed, current research has shown that it is the balance between beneficial and pathogenic bacteria that determines the oral health of the individual. Certain strains of specific species of naturally colonizing oral bacteria greatly inhibit pathogenic bacteria, specifically Streptococcus mutans, and results in either a caries-free condition, or a few arrested caries in caries-prone individuals dependent upon the threshold number of beneficial bacteria.22,23 Previously accepted methods of preventive dentistry may indeed only shift the strains of the more pathogenic bacteria into a greater plurality. Probiotic therapy is becoming more accepted by many in the health professions. Dental professionals should be actively pursuing this potentially very useful therapeutic measure for the benefit of their patients.
References
1. Berkowitz RJ. Acquisition and transmission of mutans streptococci. J Cal Dent Assoc. 2003;31(2):135-138.
2. Featherstone JDB. The caries balance: Contributing factors and early detection. J Cal Dent Assoc. 2003;31(2):129-133.
3. Thenisch NL, Bachmann LM, Imfeld T, et al. Are mutans streptococci detected in preschool children a reliable predictive factor for dental caries risk? A systematic review. Caries Res. 2006; 40(5):366-374.
4. Nunn ME, Tanner ACR, Lu SC, et al. Oral flora of caries-free 1 to 4 year-old children. Phuket, Thailand, 2009 World Congress of Preventive Dentistry.
5. Meurman JH, Stamatova I. Probiotics: contributions to oral health. Oral Dis. 2007;13:443-451.
6. Meurman JH. Probiotics: Do they have a role in oral medicine and dentistry? Eur J Oral Sci. 2005;113:188-196.
7. Hillman JD, McDonell E, Cramm T, et al. A spontaneous lactate dehydrogenase deficient mutant of Streptococcus rattus for use as a probiotic in the prevention of dental caries. J Appl Microbiol. 2009;107(5):1551-1558.
8. Hillman JD, McDonell E, Hillman CH, et al. Safety assessment of ProBiora3, a probiotic mouthwash: subchronic toxicity study in rats. Int J Toxicol. 2009;28(5):357-367.
9. Zahradnik RT, Magnusson I, Walker C, et al. Preliminary assessment of safety and effectiveness in humans of ProBiora3, a probiotic mouthwash. J Appl Microbiol. 2009;107(2):682-690.
10. Lenoir-Wijnkoop I, Sanders ME, Cabana MD, et al. Probiotic and prebiotic influence beyond the intestinal tract. Nutr Rev. 2007;65(11):469-489.
11. Zoitopoulos L, et al. Dental caries and caries-associated micro-organisms in the saliva and plaque of 3- and 4-year-old Afro-Caribbean and Caucasian children in south London. Arch Oral Biol. 1996;41(11):1011-1018.
12. Sánchez-García S, et al. A simplified caries risk test in stimulated saliva from elderly patients. Gerodontology. 2008;25(1):26-33.
13. Sánchez-Pérez L. Clinical, salivary, and bacterial markers for caries risk assessment in schoolchildren: a 4-year follow-up. Int J Paediatr Dent. 2009;19(3):186-192.
14. Haukali G, Poulsen S. Effect of a varnish containing chlorhexidine and thymol (Cervitec) on approximal caries in 13- to 16-year-old schoolchildren in a low caries area. Caries Res. 2003;37(3):185-189.
15. Twetman S, Petersson LG. Interdental caries incidence and progression in relation to mutans streptococci suppression after chlorhexidine-thymol varnish treatments in schoolchildren. Acta Odontol Scand. 1999;57(3):144-148.
16. Araujo AM, Naspitz GM, Chelotti A, Cai S. Effect of Cervitec on mutans streptococci in plaque and on caries formation on occlusal fissures of erupting permanent molars. Caries Res. 2002;36(5):373-376.
17. Caglar E, Cildir SK, Ergeneli S, et al. Salivary mutans streptococci and lactobacilli levels after ingestion of the probiotic bacterium Lactobacillus reuteri ATCC 55730 by straws or tablets. Acta Odontol Scand. 2006;64(5):314-318.
18. Krasse P, Carlsson B, Dahl C, et al. Decreased gum bleeding and reduced gingivitis by the probiotic Lactobacillus reuteri. Swed Dent J. 2006;30(2):55-60.
19. Caglar E, Kuscu OO, Cildir SK, et al. A probiotic lozenge administered medical device and its effect on salivary mutans streptococci and lactobacilli. Int J Paediatr Dent. 2008;18(1):35-39.
20. Twetman S, Derawi B, Keller M, et al. Short-term effect of chewing gums containing probiotic Lactobacillus reuteri on the levels of inflammatory mediators in gingival crevicular fluid. Acta Odontol Scand. 2009;67(1):19-24.
21. Caglar E, Kavaloglu SC, Kuscu OO, et al. Effect of chewing gums containing xylitol or probiotic bacteria on salivary mutans streptococci and lactobacilli. Clin Oral Investig. 2007;11(4):425-429. Epub 2007 Jun 16.
22. Simark-Mattsson C, Jonsson R, Emilson CG, Roos K. Final pH affects the interference capacity of naturally occurring oral Lactobacillus strains against mutans streptococci. Arch Oral Biol. 2009;54(6):602-607.
23. Simark-Mattsson C, Emilson CG, Hakansson E, et al. Lactobacillus-mediated interference of mutans streptococci in caries-free vs. caries-active subject. Eur J Oral Sci. 2007;115(4):308-314.
About the Author
Mark L. Cannon, DDS, MS
Associate Professor
Northwestern University
Feinberg School of Medicine
Chicago, Illinois


 www.carifree.com
www.carifree.com www.carifree.com
www.carifree.com