Successful Application of Total-Etch and Self-Etch Techniques in Adhesive Dentistry
By Stephen D. Poss, DDS
In order to effectively perform adhesive dental procedures, today’s clinician must have a thorough understanding of the proper protocols and restorative materials as they relate to preparation design, surface conditioning, and composite stratification. Selection of the proper adhesive can figure prominently in this decision-making process, as the clinician must have knowledge of moisture control in the intraoral environment, the timing of light activation on the performance of the bonding agent, and the bonding substrate itself. This presentation will demonstrate the characteristics of total-etch (TE) and self-etch (SE) techniques, and highlight their clinical applications.
Direct posterior restorations are more often performed with tooth-colored restoratives than with dental amalgam. Composite resin restorations represent a proven alternative to amalgam restorations, without the issues of expansion, the development of cracks in tooth structure, and mercury-related health concerns.
Composites are an integral component of adhesive dentistry, and provide function, biocompatibility, conservation of tooth structure, and improved esthetics. Adhesive restorations may actually reinforce remaining tooth structure, whereas amalgam restorations can have the opposite effect.
Differences in TE and SE Techniques
To become proficient in adhesive dentistry, clinicians should gain an in-depth understanding of the total-etch and self-etch techniques, and recognize the differences between them.
Performed since the 1950s, enamel acid-etching involves preferentially demineralizing portions of hydroxyapatite crystals to develop a porous surface for micro-mechanical bonding. In the modern era, acid-etching is performed on dentin, and with a total-etch (TE) or self-etch (SE) technique. The operator’s selection of either of these techniques depends on his or her preferences, along with several clinical factors.
In the TE technique, the outer layer of dentin is decalcified, removing the smear layer (approximately 10 µm in thickness) and opening the underlying dentin tubules. This exposes delicate collagen fibers that are subsequently infiltrated with a primer (eg, a hydrophilic resin monomer), followed by the application of a resin adhesive. Primer and adhesive are applied simultaneously in many systems. In this procedure, it is critical that the clinician completely seals dentin tubules to avoid bacterial invasion and/or sensitivity. The author generally uses the TE technique for larger direct restorations and for indirect restorations.
Rather than removing the smear layer, the SE approach involves the application of an acidic primer that will promote micro-mechanical bonding of the adhesive to the smear layer and the underlying dentin. This technique minimizes the potential for postoperative sensitivity by preventing the collapse of the collagen fibers that can occur after conditioning and drying in the TE process. The SE technique has less clinical history, but the author has had excellent results with this technique for less invasive procedures such as shallow Class I or Class II restorations.
Total-Etch Technique
Isolation and Cleaning
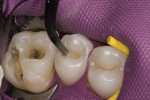
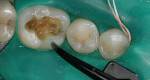
Isolation is critical for preventing contamination, and cleaning with a chlorhexidine rinse promotes disinfection (Figure 1).
Etching the Cavity Site
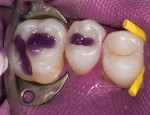
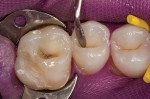
Acid etchant is applied to enamel for 15 seconds, and then to dentin for 10 to 15 seconds before rinsing with water (Figure 2). Care should be taken not to over-wet or over-dry the tooth; a matte surface is desired. A microbrush, evacuator, or cotton pellet can be used to remove pooled water. If multiple teeth will be conditioned for adhesive bonding, the clinician should etch in groups of one to three teeth, to ensure no surfaces are etched for more than 15 seconds. Once the etchant is removed, the site is lightly air-dried, with care taken not to desiccate the tooth. Once the structure is dry with a matte appearance, the author prefers to apply a wetting agent. To provide a uniform dentin surface for adhesive application, the clinician should be careful to avoid pooling.
Activation and Application of the Primer/Adhesive
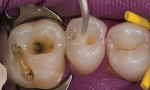
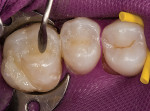
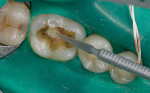
A generous coat of adhesive should be applied to the conditioned tooth surface (Figure 3). Excess solvent is evaporated with a gentle stream of air, and the adhesive is then light-cured. If a fourth-generation adhesive is used, the primer should be light-cured prior to application of the resin.
Buildup of Composite Resin
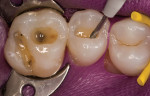
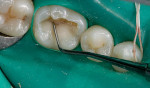
To aid in adaptation of the composite resin, flowable resin is applied in an increment of approximately 1 mm to cover the floor of the preparation and flow beneath any undercuts (Figure 4). After the flowable resin is light-cured, a microhybrid composite resin is added to the buccal and then the lingual walls (Figure 5 and Figure 6). The resin is sculpted to avoid prolonged finishing, and then light-cured.
Finishing of the Restoration
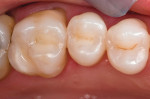
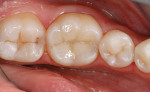
Carbide finishing burs are used for minor finishing. To achieve a final luster, the author prefers a polishing regimen of rubber cups, points, or disks (Figure 7).
Self-Etch Technique
Isolation and cleaning are the same as with TE (Figure 8).
Etching the Cavity
The acidic primer (sixth generation) or all-in-one (seventh generation) SE is applied and left in place for approximately 20 seconds (Figure 9). Light air-drying will evaporate the solvent. The dentist should take care not to desiccate the dentin. This process is repeated, and the SE adhesive is light-cured for 10 seconds.
Buildup of Composite Resin
Flowable resin (1 mm) may first be applied to cover the cavity floor. A microhybrid composite resin is then incrementally applied to the lingual and the buccal walls of the restoration, and sculpted (Figure 10).
Finishing the Restoration
Carbide finishing burs are used to perform minor finishing, followed by the author’s polishing regimen (rubber cups, points, or disks) to achieve the final luster (Figure 11).
While the SE approach may appear to be faster than the TE procedure, the need for repeat applications of the SE material can make for a nearly equal time investment. It is important for the clinician to allow sufficient time for the SE to remain on the tooth prior to removal, so that its acidic components create the proper retentive pattern.
iscussion
In adhesive dentistry, there are numerous clinical factors that may contribute to postoperative sensitivity, such as failing to apply a rubber dam, over-drying or over-etching the dentin, incomplete caries removal, and inadequate curing of the adhesive. Some clinicians claim that a failure to apply an antibacterial agent prior to etching can also cause sensitivity. Inadequately cured resin can result in postoperative sensitivity as well. Therefore, the curing light must have sufficient power to cure resin in the deepest portions of cavities greater than 6 mm in depth. The use of a wetting agent after etching with a TE technique is not included in the directions for most adhesives, but the author has found this step to be helpful in reducing the risk of postoperative sensitivity. Pooling of the wetting agent should be avoided.
Relatively speaking, SE restorations have only recently become a part of adhesive dentistry, and less data is available regarding their longevity. However, their use can eliminate the aforementioned technique sensitivities. The SE approach does not necessarily save a great deal of time, but reduces the potential for postoperative sensitivity by eliminating the possibility of over-etching, and the need for antibacterial or wetting agents employed in the TE procedure.
Conclusion
This article reviewed the fundamental characteristics of total and self-etching from a practical clinical perspective, and used several instructional cases to demonstrate the application of both techniques. Restoring damaged teeth or replacing amalgam restorations with direct composite resin restorations is a viable treatment modality. Additionally, adhesive dentistry also provides numerous clinical benefits such as function, biocompatibility, esthetics, and conservation of tooth structure.
About the Author
Stephen D. Poss, DDS
Poss Dental Designs
Brentwood, Tennessee