Achieving a Predictable Outcome with CAD/CAM
James Klim, DDS
Chairside CAD/CAM technology enables the practitioner to virtually design and mill high-strength restorations to fulfill treatment objectives.
Achieving an esthetic and functional outcome in restorative dentistry depends on numerous factors. One of the most important considerations in an esthetic treatment plan is the patient's esthetic expectations and biomechanical factors; having a clear understanding of the steps involved improves the predictability of the proposed restorative treatment. As demonstrated in the following case study, chairside CAD/CAM technology enables the practitioner to virtually design and then mill high-strength restorations to fulfill the objectives set forth preoperatively.
Dentistry is rapidly developing with new products, materials, and laboratory applications for the restorative dentist. The advancements in digital optics, virtual design software, and precise CAD/CAM machining capability is rapidly advancing fabrication options in restorative dentistry.1,2 When applying sound periodontal, biomechanical, and esthetic fundamentals to CAD/CAM dentistry, the practitioner can provide a predictable outcome for functional and esthetic comprehensive restorative treatment.3
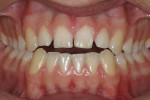
Esthetic restorative care starts with understanding the focus of the patient's objectives and expectations. In this particular case, the patient was very specific about closing the spaces between the front teeth and enhancing the size of the front teeth to close the open space between the upper and lower front teeth.
The initial interview process sets the stage for restorative success. This is where treatment and relationship expectations are established between the dentist and the patient. From the historical material gathered from clinically focused questions and responses, the clinician can determine the best route to achieve patient and clinical expectations.
After the interview, records are achieved to gather the necessary information for a diagnosis and restorative treatment options. The clinical examination consists of a full series of radiographs, periodontal evaluation, digital photographs, study models, and oral/nasal airway assessment.
Treatment Planning with CAD/CAM
The CEREC® Bluecam camera optics and CEREC® MC XL (Sirona Dental Systems, https://www.sirona.com) milling dimensions are now in the 10-μm to 20-μm range.4 Margins, interproximal contacts, and occlusion will rival and can surpass traditional laboratory and impression techniques when applied with detailed precision by the operator.
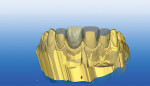
The CEREC software allows the operator to overlay the virtual wax-up model over the virtual preparation model to precisely propose and design restorations dimensionally identical to the wax-up (Figure 1 ). When crossing the midline, the author designs the centrals first. The mesial-cervical embrasure is determined by the mesial margin outline and, to some extent, can be compensated for during the virtual design process when dealing with asymmetrical root trunks. The larger root trunk trumps the emergence profile, so virtual design and shape should be done first.
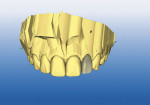
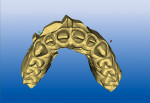
Once the centrals are designed and are in the process of milling, the remaining lateral incisors are designed in tandem sequence for proficient design and milling time from the same virtual die (approximately 7 to 9 minutes per tooth) (Figure 2 ).
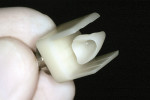
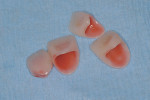
One of the esthetic advantages of CAD/CAM ceramics (such as IPS Empress® CAD Multi, Ivoclar Vivadent, https://www.ivoclarvivadent.us, used in the case presented in this article) is the inherent cervical-incisal gradient zones. The virtual restoration, before milling, can be positioned in the virtual block to reproduce the desired gradient zones to best esthetically blend the restoration (Figure 3 ). In many ways, recreating similar color/transparency transition and optic influences as seen in a natural tooth are being created. The preparation stump shade and margin design plays an intricate part in the final cervical chroma outcome. When applicable to the case, using the dentin optical color shine-through will give vitality and depth to the final restoration.
Pre-mill block selection is determined primarily by the desired brilliance for the incisal half of the restoration. The cervical half can then be controlled by the depth of the preparation (ceramic thickness); margin design (chamfer, shoulder, or feather); virtual block opacity; placement of the virtual restoration positioning in the IPS Empress CAD Multi block relative to block size (12, 14, or 14L); and stain characterizing. During the adhesive period, the bonding resin can be used in the body and cervical zones to increase brilliance or gain warmth in the final desired outcome.
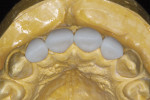
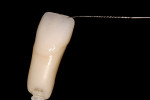
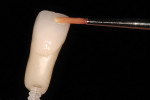
The primary contours and cervical emergence profiles are established in the virtual design process. The surface textural features are defined following after the mill but before stain application (Figure 4 ). Incisal highlights and cervical/interproximal stain characteristics are applied and fired before glazing. In the more visually critical anterior zone, stain firing prior to glaze before glazing will give more optical depth to the applied colors when an independent stain firing is used.
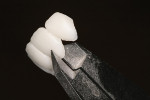
The author prefers a cast model for final shaping and finishing procedures once the machining process is accomplished (Figure 5 ). Finishing techniques are applied to "fingerprint" the desired esthetic presentation. For a more incisal-depth look with the IPS Empress CAD Multi blocks, it is possible to achieve excellent incisal effects without a full cutback. Apply subtle mamelon reduction to only the labial surface, staying 0.5 mm from the incisal or mesial-distal edge. Apply IPS Wash Paste Modifiers (Ivoclar Vivadent), preferably a blue and white combination (Figure 6 ), fire, and then add back a thin layer of medium Incisal Opalescent ceramic. Leaving the incisal edge intact maintains the pure functional strength of the ceramic. Studies affirm that the machined ceramics have inherently better functional properties (less likely to fracture) than traditional laboratory stacked or pressed ceramics because of the industrial manufacturing process.5-7
The ceramic finishing artistic caveat to fooling the eye starts with the tooth profile, which can also be called the tooth figure. In addition, customizing the reflective and deflective surfaces and texturing creates an individuality and uniqueness for each case. But even considering these important artistic tooth principles, the superficial gloss finish is what completes the "fingerprint" act. This is created with glaze-style (Figure 7 ) application and post-glaze polishing.
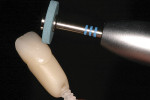
The superficial gloss finish is applied after the glazing process. The labial convex surfaces are smoothed and polished to a higher luster. Medium and high-gloss polishing wheels are used primarily on the mesial and distal line angles. Be careful to avoid polishing away wanted surface texture. Final surface luster also can be controlled with a Robinson wheel and diamond pastes (Figure 8 ).
Case Presentation
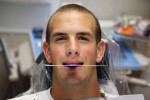
A male teenager presented with a history of airway obstruction via enlarged tonsillar pillars and a deviated nasal condition (Figure 9 and Figure 10 ). The author saw this as a myofunctional contributor to the tongue thrust and future posttreatment retentive factors. A referral was recommended for a sleep study and airway assessment.
After the records data collection, a wax-up proposal was presented to best determine the esthetic characteristics, soft-tissue zenith outline, and functional dynamics for the case. Using the metric golden proportion for central tooth length, the upper central incisor edge was determined.8 The central width/length ratio should be 75% to 85%; in most cases, the centrals are in the 9-mm to 10-mm length zone (Figure 11 and Figure 12 ).
The patient accepted an esthetic treatment proposal of all-ceramic restorations on the upper four incisors to fill space and enhance the esthetic harmony for tooth size. Because he was leaving for college in a few days, the author decided to prepare the teeth, place transitional restorations (provisionals) for functional and phonetic assessment, and then whiten the remaining teeth in the smile zone. Chairside whitening was completed using Zoom!® (Discus Dental, https://www.discus.com) to achieve an overall lighter tooth color. Subtle soft-tissue alignment issues were taken care of at the preparation appointment with a diode laser. Care was taken to protect the 2.5-mm biological width and adequate attached tissue zone.9 It is important to respect the distance of the restorative margin to the bone in order to optimize the natural architecture of the gingival attachment and avoid harmful periodontal consequences.
The secret to achieving the proper final restorative emergence outline, particularly at the midline, is to control the zenith outline first and then prepare to the zenith outline. In cases where the midline root trunks are not the same size, the tooth should be prepared with a larger root trunk first for ideal emergence zenith outline, and the smaller root margin should be dropped another 0.5 mm from mid-tooth to mesial line angle. This will create ceramic clearance for a fuller emergence contour in the cervical one third of the preparation and facilitate flexibility at the design stage to compensate for symmetrical emergence Maxillary midline appeal is best enhanced with adjoining symmetry for the incisal, labial, and cervical embrasures. Identifying this physical symmetry condition in the diagnostic phase will facilitate proper communication for the diagnostic wax-up and lead to a clearer focus during the preparation process.
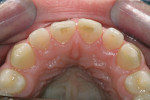
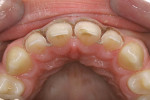
The central and lateral incisors were prepared to retrocline the final restorations and create the ideal interproximal papillae architecture (Figure 13 and Figure 14 ). Interproximal cervical margins were prepared so that the interproximal contacts could be placed 4-mm to 4.5-mm from the bone, facilitating a predictable papillae fill of the cervical embrasures.10 The interproximal margins were feathered to the lingual, leaving the lingual unprepared. The lingual full-coverage restoration margins were established during the virtual design on enamel near the lingual free gingival margin. It is the author's objective to be as minimally invasive as possible with the preparation requirements and still create the most ideal preparation architecture design to maximize all-ceramic engineering for a highly esthetic outcome that honors the functional demands of the mouth.
This case presented an open bite and proclined maxillary incisors. The final tooth position goal was to retrocline the clinical crown to best meet tooth-arch positioning, establish protrusive guidance, and create a positive lingual phonetic morphology. With the MC XL refined margin milling, the clinician was able to honor minimally invasive preparation criteria and design and still mill margins on uncut or minimally prepared enamel. After milling, the ceramic margin was then refined to a "knife" edge with finishing wheels, thereby avoiding over-bulked margins and optimizing cervical tooth/gingival harmony.
Before the final preparation check, the final pre-planned ceramic and shade needed to be reaffirmed. To accomplish preparation reduction verification, the author used a diagnostic wax-up matrix, formed a provisional, removed the provisional, and then measured and assessed the provisional for the proposed labial ceramic thickness. The preparation shade was taken and the final desired shade was finalized for proper ceramic shade and opacity. Preparation design and reduction was primarily controlled by occlusal, functional, and pre-color conditions to achieve final esthetic objectives.11
While it would have been possible to provide same-day restorations using chairside CAD/CAM technology, the author placed transitional restorations to assess tooth size esthetics, functional envelope, and phonetics (Figure 15 and Figure 16 ). The preparations were digitally imaged before provisional placement. Using CEREC® CAD/CAM technology, multiple optical images of the preparation and the adjacent teeth in the opposite arch were taken to build a virtual (Figure 17 ) die.12One advantage of a digital impression is instantaneous preparation and margin assessment. If needed, alterations can be accomplished in the mouth and re-imaged to ensure precise margin outline and preparations that will fulfill the engineering requirements for a successful functional and esthetic outcome.
Once the restorations were milled, texturized, glazed, and superficial gloss polish was completed, the ceramic restorations were prepared for bonding with a hydrofluoric-acid application, rinsed, and dried, and then followed with Monobond Plus (Ivoclar Vivadent) silane application (Figure 18 ).
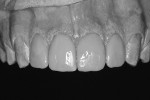
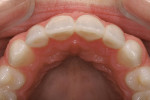
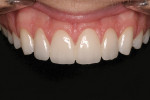
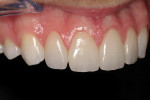
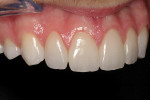
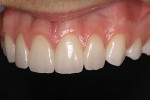
The final restorations illustrate the possibilities with current chairside CAD/CAM dentistry (Figure 19 ). With the proper esthetic planning, it is possible to achieve quality esthetic restorations. The CEREC software has the capability to precisely reproduce the wax-up for tooth proposal, significantly simplifying the virtual design process. With the chairside option to customize texture and ceramic finish, the "fingerprinting" process can be enhanced for optimal ceramic blend (Figure 20 , 21 , 22 ).
Conclusion
Esthetic chairside CAD/CAM will take restorative dentistry to new creative heights as the technology continues to evolve (Figure 23 ). However, the basis of success still relies on the critical elements demanded for sound restorative care: diagnosis, periodontal support, biomechanical application, preparation design, sound optical impressions and bite records, placement protocols, and finishing.
Virtual design and ceramic machining is creating an attractive alternative to investing and pressing or stacking ceramics. The CAD/CAM ceramics have natural tooth gradation/color transitions already designed in the ceramic, so the esthetic result can be very natural without layering and firing ceramic applications.
With so many cement adhesive systems on the market, pay particular attention to the system being used. Apply adhesive steps with a microscopic mindset. Schedule adequate time for this appointment in order to take the necessary time and pace for predictable adhesive results. The secret to adhesive management is to systematize each step for predictability and efficiency. When the CAD/CAM ceramics are bonded with precise clinical technique, they will surpass tooth strength and yet have wear properties that are as biologically compatible as enamel.
Disclosure
The author is a current consultant for Sirona.
References
1. Liu PR. A panorama of dental CAD/CAM restorative systems. Compend Contin Educ Dent. 2005;26(7):507-508, 510, 512 passim; quiz 517, 527.
2. Leinfelder KF, Kurdziolek SM. Contemporary CAD/CAM technologies: the evolution of a restorative system. Pract Proced Aesthet Dent. 2004;16(3):224-226, 228, 231.
3. Klim J. Clinical applications of chairside CAD/CAM dentistry. Compend Contin Educ Dent. 2007;28(11)(Suppl 2):19-26.
4. Schneider W. No compromises the new CEREC MC XL and inLab MC XL milling machines. Int J Comput Dent. 2007;10(1):119-126.
5. McLaren E: CAD/CAM All-Ceramic Restorations Achieving Ultimate Esthetics: Clinical & Laboratory Perspective. ACDNA Presentation. June 2006.
6. Chen HY, Hickel R, Setcos JC, Kunzelmann KH. Effects of surface finish and fatigue testing on the fracture strength of CAD-CAM and pressed-ceramic crowns. J Prosthet Dent. 1999;82(4):468-475.
7. Clinical Research Associates. Newsletter. 2001;25:3-4.
8. Bukhary SM, Gill DS, Tredwin CJ, Moles DR. "Golden proportion" and its application to calculate dentition. Georgian Med News. 2007;(142):87-94.
9. Cunliffe J, Grey N. Crown lengthening surgery-indications and techniques. Dent Update. 2008;35(1):29-30, 32, 34-5.
10. Kois JC. Altering gingival levels. The restorative connection. Part I Biologic variables. J Esthet Dent. 1994;6(1):3-9.
11. Stappert CF, Ozden U, Gerds T, Strub JR. Longevity and failure load of ceramic veneers with different preparation designs after exposure to masticatory simulation. J Prosthet Dent. 2005;94(2):132-139.
12. Dunn M. Biogeneric and user-friendly: the Cerec 3D software upgrade V3.00. Int J Comput Dent. 2007;10(1):109-117.