Patient-Driven Treatment Options
Harry A. Long, DMD
There is almost always more than one treatment that can restore form and function to patients when the need arises.
The practice of dentistry affords its practitioners the opportunity to diagnose and treat many types of dental problems. The treatment modalities dentists select are often the ones with which they feel most comfortable,2 the ones that they feel will provide a solution to the patient's immediate need, and the ones they know will last the longest without a need to revisit the original problem. Dentists seek an evidence-based solution to the problem as presented.
As new materials and techniques become available in the dental marketplace, dentists often must choose between their tried-and-true treatments of choice or challenge themselves with new and improved materials and learning new techniques. Continuing education opportunities provide the possibility of continued growth in a profession where change is constant.
Ideally, when dental problems arise, the preferred treatment is usually the one that is minimally invasive to hard and soft tissues and best preserves healthy hard and soft tissue. As materials and techniques have advanced, so has the dialogue among dentists. Although dentists may not always agree with each other on the needed treatment for individual patients, most do agree that there is more than one treatment that can restore form and function to patients when the need arises.
Further complicating the problem of treatment selection is the desire of the patient. Patient-influenced care many times is not evidence-based, and is often just based on conversations with friends or information gleaned from the Internet, and is often full of misconceptions and misunderstandings.
The wake-up call for all practitioners often comes by just looking at cases that were treated years ago as they come for regular care and realizing how much concepts and treatments have changed over the years. The most difficult aspect of dental care is often deciding which treatment modality is the best for a particular patient.
Healthy Disagreements
The practice of dentistry has been one of constant change and controversy-a healthy disagreement.3 Soft tissue is unimportant. Soft tissue is expendable. Soft tissue is sacrosanct. Dental amalgam is good. Dental amalgam is bad. Tooth whitening is bad. Tooth whitening is good. Full-coverage dental restorations are good. Full-coverage dental restorations are the last choice for tooth restoration.
Controversy in dentistry is nothing new. One day a certain dental treatment is the treatment of choice and the next day it is replaced. Dentists who then continue to use the older method of treatment are said to no longer be providing the "standard of care" for their patients.
There have been many regional differences in care as well. Full-coverage, tooth-colored posterior restorations seem to be the standard of care on both coasts, while in the heartland full-coverage cast-gold restorations have been popular for a long time. For many years, gold-foil restorations were popular on the West Coast. These differences in care do seem to be disappearing as all areas of the country use more and more tooth-colored restorations.4
Many dentists have embraced the digital age with computers and digital radiographs while others still praise the clarity and accuracy of traditional methods. Stim or centric relation? Endodontic care or implant therapy? With so many choices, it is amazing that dentists can agree about anything.
While a highly successful functional and esthetic outcome for the patient is the desire of all who practice dentistry, the selection of the treatment modality is often an individual dentist's preferred treatment. This is the treatment that each dentist finds to be the most successful at treating the dental problem at hand. This may not be a bad rationale for treatment selection, because the dentist is choosing a treatment that has proven to be successful in his or her hands. Ultimately, each practitioner must choose his or her own best way to get to where the profession seeks to go collectively-which is the best possible outcome for the patient.
Patient Concerns and Preferences
The problem of treatment options is further complicated for the dentist by the demands of the patient. Although most patients will accept the dentist's recommendations for treatment, some patients will have preconceived ideas about their care and they will require the dentist to alter his or her treatment plan to accommodate their needs. Patients' needs, such as moving to another state or having a wedding in a few weeks, as well as health issues, phobias, and/or compliance issues, will often influence the treatment modality chosen by the dentist. One of their friends had a problem with a certain procedure so they do not want that procedure. They have done a lot of "research on the Internet" and they know what they want and especially what they do not want.5
Patients may come into the dental office requesting a specific service such as LUMINEERS® (DenMat, https://www.denmat.com), Invisalign® (Align Technology, https://www.invisalign.com), or dental implants. If the dentist is a certified provider of the services requested, and he or she feels the service requested is the proper one to correct the dental problem, treatment can and should proceed. But if the dentist is not certified to provide the services requested or the dentist does not feel the services requested are the proper ones to correct the dental problem, alternative services should be suggested to the patient.
A patient needing smile design services that can only be properly treated with orthodontics and teeth whitening cannot hope to have these services completed 3 weeks before her upcoming wedding. Orthodontic care may give way to porcelain veneers and teeth whitening. The treatment of choice becomes replaced by the treatment of necessity.
The treatment of choice, the standard of care, and evidence-based care may all be altered as a result of patient-dictated circumstances.6 Improper planning by the patient may make it impossible to provide the services required for a complex restoration requiring time for implants, orthodontics, or orthognathic surgery. Alternative services may be substituted because of a lack of time. The substituted services should not be considered lesser services, but rather the proper services considering the time restraints created by the patient.
Often the patient will have or create financial restraints that require an alternative to the ideal treatment. For the patient who is missing a number of posterior teeth, a half dozen implants and nine units of implant-supported crown-and-bridge can cost thousands of dollars more than a removable partial denture. Both treatments restore form and function for the patient in need of posterior support. The clinician's preference may be to do the implants and then restore with fixed dentistry, but when the patient says they have three children in college, the clinician has to be able to provide a suitable treatment option.7
When examining a patient for the first time, it is interesting to ask them about their dental care and why they have had specific restoration types. The answers may be surprising. The restorations in the patient's mouth may not have been the first choice of the providing dentist, but the best treatment available when balancing the needs and wishes of the patient. Fortunately for the profession, clinicians are able to plan a number of treatment options for patients who may require alternatives because of their circumstances.
Creating the Criteria for Treatment Options
A great patient experience begins with a thorough patient interview. Find out why the patient has chosen your office. Make a real effort to understand the care they have had in the past. Finding out how they view dental care and dentistry in general will help to understand what the patient is thinking and, as a result, how to best serve them.8 A thorough patient examination, along with the appropriate radiographs, soft tissue examination, study casts, and digital images of the dentition and the full face of the patient can help the dentist and the patient co-diagnose and develop the ideal treatment plan.
When developing the treatment plan, it is important to first plan the ideal care needed to correct the problems presented by the patient.9 Periodontal needs (such as scaling and root planing), endodontic therapy, correction of all soft and hard tissue disease, and remediation of joint and/or muscle problems establish the baseline for beginning patient care. This care will be needed regardless of the plan chosen by the patient as definitive care needed to restore the patient's mouth to a state of health.
When choosing definitive care, fixed dentistry is usually preferred over removable dentistry. The underlying choices for the ideal treatment plan require that clinicians be conservative both of hard and soft tissue and that the patient is fully involved in the process of developing the final plan.10 It is not enough to bring the patient only one plan for their care. Dentists must develop at least two plans and then describe the needed care. They must talk about the benefits and the disadvantages of each treatment plan and they must help the patient to understand as well as possible the differences of each plan and the limitations of both materials and technique. Patients should understand the need for regularly scheduled follow-up care and the need for structured and vigilant home care.
At this point, patient preferences may indicate a need for the development of different treatment options. Time or budget constraints, fear, or preconceived ideas about some aspect of proposed treatment all may require the ideal treatment plan to be altered to suit the desires of the patient.
When the dentist's ideal treatment plan needs to be changed, the patient needs to be aware of the limitations introduced by the new plan. The new plan may call for a removable denture or for the removal of teeth needing endodontic therapy. The patient needs to fully understand the changes and how they may affect the patient's speech and function during mastication. The patient also needs to know how today's proposed treatment will affect possible future restoration choices.
Case One
Ideal Treatment Plan: Invisalign and Teeth Whitening
Patient-Driven Treatment Option: Ten Porcelain-Laminate Veneers
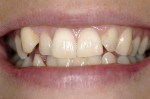
The first case is a 26-year-old woman with a collapsed arch form and classically crowded dentition. A full digital radiography series was taken along with study casts, soft tissue probe readings, and a thorough clinical examination along with a complete medical history. During the new patient interview, the patient suggested she would like to have straighter, whiter teeth.
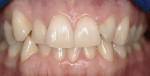
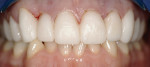
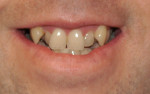
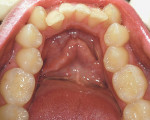
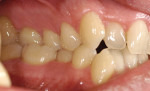
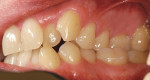
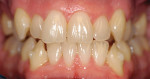
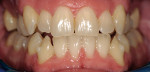
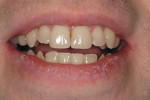
The digital images show the effects of a broken arch form. The full-face image shows anterior crowding and collapse of the buccal corridors (Figure 1). Dark triangles could be seen at the corners of the mouth (Figure 2). This negative space is where the teeth would be positioned if there had not been a collapse of the maxillary dental arch.
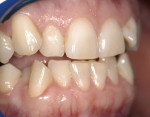
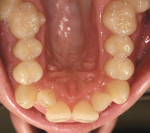
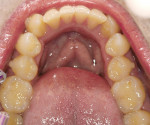
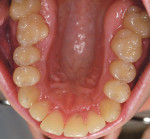
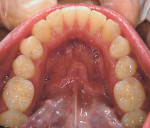
There was irritated gingival tissue that had been squeezed and distorted as the arch collapsed (Figure 3). In this state of collapse, it was difficult for the patient to adequately clean her teeth using just a toothbrush and dental floss. As a dental arch broke and began its collapse, the arch form actually became smaller and more constricted. This case exemplified the classic orthodontic problem seen in adult orthodontics. Adults present with loss of space in the dental arch resulting from collapse of the arch, crowding of the teeth, and gingival irritation due to difficult access to the tissues (Figure 4).11 These cases are easily treated using either classic orthodontic therapy or Invisalign treatment.
The patient and the author participated in an exercise of co-diagnosis where they both looked at a PowerPoint presentation of digital images of her face and various images of her teeth and smile. During this co-diagnosis, the patient described the things she did not like about her smile and the author continued to ask questions to promote a conversation about her concerns and possibilities for remediation.12 The patient expressed the most concern about her crowded and discolored maxillary dentition. She wanted straighter and whiter teeth.
After this discussion, the author felt that the patient would best be treated using either conventional orthodontic therapy or Invisalign treatment. The plan would be to increase size of the arches and, therefore, increase the available space for the teeth in order to provide adequate room for all of the maxillary and all of the mandibular teeth. The goal would be to procline each of the teeth in both of the arches and to use reproximation to gain a couple of millimeters of lost arch length.
The author confidently presented his plan for Invisalign therapy to straighten the patient's crooked teeth and explained how she would be able to whiten her teeth while they were being straightened by using a whitening gel at home. He presented a plan for porcelain-laminate veneers as an alternative treatment. The patient informed the author that she did not want to do orthodontics of any type. She had an upcoming engagement party and she wanted a beautiful smile in less than a month. She wanted porcelain-laminate veneers.
After some discussion about porcelain-laminate veneers, including their benefits and their limitations, she elected to do 10 porcelain-laminate veneer restorations on her maxillary anterior teeth. Her lack of planning and her time constraints left only one option for the care she wanted.
Using porcelain-laminate veneers to correct a collapsed and crowded arch form is just like doing orthodontics. The goal of smile design is to widen the arch to create room to place all of the teeth into the arch form without the appearance of crowding and without the appearance of crushed and crowded interdental papilla.
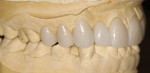
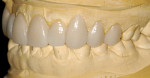
The case was first designed in wax on the study casts. The arch was expanded and the esthetically pleasing natural proportions of the teeth were recaptured in the wax-up. Gingival tissue was altered to create a more ideal gingival architecture (Figure 4 and Figure 5).
The wax-up was used to create a stent, which would be used to fabricate the provisional restorations (Figure 6). This image shows the provisional restorations in place and the result of some gingival alterations using the diode laser. It is important to note how the collapsed arch was widened and space was created for the tooth to be placed back into the arch form and still allow for beautifully proportioned teeth.
The provisional restorations acted as a "test drive" of the final restorations as they were in the same position, length, and size as the proposed final restorations. During this trial phase, adjustments could be made to the length and position of the teeth to ensure a pleasing result for the final restorations. The final restorations showed a very esthetic correction to the problems presented by the patient (Figure 7 and Figure 8).
Case Two
Ideal Treatment Plan: Invisalign and Porcelain- Laminate Veneers
Patient-Driven Treatment Option: Invisalign
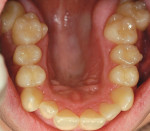
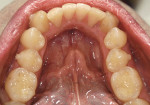
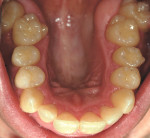
The second case was another classic adult collapsed arch form, loss of arch length, crowded-tooth case. The 30-year-old man presented with collapsed maxillary and mandibular arch forms along with crowded dentition and irritation of the interdental papilla (Figure 9, Figure 10). A close look at the side views shows the crossbite and crowding along with collapse of the arch form (Figure 11 and Figure 12). A full series of dental radiographs were taken along with digital images of the patient's teeth and face, study casts, soft tissue probe readings, a thorough clinical examination, and a complete medical history.
The author engaged the patient in the co-diagnosis exercise using a Power Point presentation. He understood the need for orthodontic care. The author did not want to do this case so he told the patient that he would need to see an orthodontist to have his correction. He went for a consultation, and did nothing for the next few years. On a follow-up visit, the author asked the patient when he was going to begin his orthodontic care. He told the author he still wanted to do it, but that he would not wear conventional metal braces. He asked if the author could do Invisalign to resolve his problem. The author told him he would do a new consultation and try to develop a new plan that would use Invisalign.
The patient ultimately accepted a plan that included 18 months of active Invisalign therapy followed up by 20 porcelain-laminate veneers. The author's goal was to widen the arches and to complete this cosmetic restoration using porcelain-laminate veneers.
As the case began there were remarkable results almost from the start. At 8 months, both arches has begun to widen and room began to open up for the teeth to find their way back into the developing arch form (Figure 13, Figure 14, Figure 15). After 18 months of treatment, the arches looked great and they appeared ready for the next phase of treatment, which included 20 porcelain-laminate restorations (Figure 16, Figure 17, Figure 18).
The patient was very pleased with the results of the Invisalign therapy up to this point, and he said that he would like to continue using Invisalign to finish his cosmetic and functional makeover. After some discussion, the author and the patient agreed to try a mid-course correction and continue to move the teeth to correct what had seemed an impossible, patient-driven treatment option.
The case is still in care and the author continues to see the patient for short visits once every month to monitor his progress (Figure 19, Figure 20, Figure 21, Figure 22). The patient is very happy with the Invisalign therapy and has gained a new confidence as his cosmetic makeover has unfolded.
Discussion
Change seems to be the overlying concept of the dental profession. Materials and techniques change; equipment evolves or seemingly appears out of nowhere. As these changes occur, dentists are forced to look at their treatment plans and make changes as they see fit. When the author began his practice in 1973, acrylic-covered gold crowns had just been replaced by porcelain-fused-to-gold crowns. Today, all-ceramic lithium-disilicate restorations used either as veneers or crowns have replaced the full-coverage porcelain-fused-to-metal (PFM) anterior restorations of the past.13
Changes in materials have afforded the profession the opportunity to do "prepless" veneers and better bonding technology has helped dentists to be minimally invasive and create partial-coverage restorations where once only full-coverage would work.
As materials technology advances, new treatment options will continue to enter the dental arena. Full-coverage porcelain-veneered-to-zirconia restorations have been quite successful for cosmetic posterior restorations, although the strength of porcelain to zirconia is weak and failures can occur under load. Recent advances have produced full-contour zirconia restorations to take the place of porcelain-veneered-to-zirconia and PFM crowns. These full-contour zirconia restorations are very kind to the surrounding soft tissues and can be very esthetic on both molars and premolars. They have the added advantage of being almost impossible to break.
Material choices can also influence treatment options. The strength of lithium disilicate can change many restorations from full-coverage to minimally invasive, partial-coverage restorations. Creating porcelain-laminate veneers using lithium disilicate at a thickness of 0.3 mm has made it possible for "prepless" veneers to replace the conventional tooth preparation for stacked porcelains. Lithium disilicate can also more easily hide discolored underlying tooth structure and dark metal posts than many other all-ceramic restorations.
Changes in treatment options resulting from changes in materials and techniques and technology are constant and manageable. With each new round of materials, the results dentists are able to achieve seem so much better than the previous generation, and the resulting treatment comes closer to replacing what has been destroyed with a more natural appearance and a more biocompatible result.
The changes in treatment options that result from patient preference can be quite interesting but often are much more difficult for the dentist to deal with because the optional treatment plan can, and usually does, deviate quite a bit from the ideal, evidence-based treatment plan. The two most common reasons for patients to request changes to the evidence-based treatment plan developed by their dentist are lack of time to complete the described treatment and needing a less costly treatment option to resolve their dental problems.
Time constraints are often a reason to elect an optional treatment plan for a patient. Patients often are not aware, at least initially, that their ideal treatment plan may take many months to complete. They come to the office requiring dental implants, restorative dentistry, and often think their care can be completed in a matter of weeks. Lack of planning on the patient's part can be the main reason that optional treatment plans have to replace ideal, evidenced-based care. Patients are often unaware of the severity of their dental condition and, therefore, do not plan enough time to complete the complicated treatment plans required for the remediation of their problems. This situation can be frustrating for the patient and the dentist as well. The treatment plans developed for patients who have time constraints are most often compromises of ideal care. Although they may satisfy all of the requirements of restorative dentistry, they may be less comfortable for the patient to wear, more difficult for the patient to clean, and might be an esthetic compromise, and, as a result, they may find less patient compliance in both the patient wearing them regularly and being able to clean them properly.
The need to develop treatment options because of cost is probably the most common reason that dentists need to develop alternative plans for patient care. The ideal, evidence-based treatment plan for patients requiring tooth replacement and periodontal care along with implants and restorative dentistry often costs many thousands of dollars. Patient circumstances may dictate the need for an alternative treatment option that will have to restore form and function, often at thousands of dollars less than the original treatment plan. These cost compromises can severely alter the stability, esthetics, longevity, comfort, and compliance.
Ideal, evidence-based treatment plans have the advantage of being long-lasting, easy to maintain, highly esthetic, and exhibit a high degree of patient comfort. Treatment options developed because of the patient's financial concerns may exhibit all of these features as well, though usually to a lesser degree. It is difficult to capture the stability, comfort, and beauty of fixed dentistry with optional care that often relies on removable dentistry.Conclusion
Treatment options are a way of life in the dental profession. Most dentists develop their treatment plans using the best of evidence-based criteria. Just as often, those plans may be altered by the needs and desires of the patient. Dentists seek to be minimally invasive and to provide long-lasting solutions to often very difficult problems. Circumstances may require the practitioner to alter or even completely change a treatment plan but, ultimately, the best treatment options for the patient will be delivered regardless of the constraints the patient places on the dentist.
The two cases presented here were both patient-driven treatment options. It has been the author's experience that most instances of treatment options tend to be patient-driven. Although other types of treatment options occur as well, such as a fixed dentistry case becoming a fixed/removable case when implant fixtures cannot be placed for any reason, the treatment options cases that are patient-driven because of either time constraints or financial concerns are the most common and have been the most interesting.
References
1. Maslow A. The Psychology of Science: A Reconnaissance. Richmond, CA: Maurice Bassett Publishing; 1966.
2. Summitt JB. Choosing among the wide range of treatment options. In: Summit JB, Robbins JW, Schwartz RS, eds. Fundamentals of Operative Dentistry. A Contemporary Approach. 2nd ed. Hanover Park, IL: Quintessence Publishing; 2008.
3. Kawahata N, MacEntee MI. A measure of agreement between clinicians and a computer-based decision support system for planning dental treatment. J Dent Educ. 2002; 66(9):1031-1037.
4. Christensen GJ. Longevity versus esthetics: the great restorative debate. J Am Dent Assoc. 2007;138(7):1013-1015.
5. Koufos MJ, Lange KW, Rose TS, et al. Future of dentistry: dental practice issues. Interview. J Am Dent Assoc. 2002;133(8):1108-1116.
6. Meyer DM. Evidence-based dentistry: mapping the way from science to clinical guidance. J Am Dent Assoc. 2008;139(11): 1444-1446.
7. Taking the Bite Out of the Cost of Dental Work. US News and World Report Health. Available at: https://health.usnews.com/health-news/articles/2008/02/14/taking-the-cost-out-of-the-bite.html. Accessed September 7, 2010.
8. Homoly P. Importance of stories: the new patient interview - part two. Journal of Cosmetic Dentistry. 2006;22(2):112-116.
9. Hook CR, Corner RW, Trombly RM, et al. Treatment planning process in dental schools. J Dent Educ. 2002;66(1):68-74.
10. Murdoch-Kinch CA, McLean ME. Minimally invasive dentistry. J Am Dent Assoc. 2003;134(1):87-95.
11. Lestrel PE, Takahashi O, Kanazawa E. A quantitative approach for measuring crowding in the dental arch: Fourier descriptors. Am J Orthod Dentofacial Orthop. 2004;125(6): 716-725.
12. Digital documentation: seeing the big picture in guided co-diagnosis. Dental Economics. Available at: https://www.dentaleconomics.com/index/display/article-display/254076/articles/dental-economics/volume-96/issue-4/features/digital-documentation.html. Accessed September 7, 2010.
13. Della Bona A, Kelly JR. The clinical success of all-ceramic restorations. J Am Dent Assoc. 2008;139(Suppl):8S-13S.
About the Author
Harry A. Long, DMD
Private Practice
Wayne, New Jersey