Prosthetic Management of Compromised Implant Positioning
Secondary splinting of individual implants addresses the need for a common path of insertion with minimal compromises to esthetic, biologic, and mechanical concerns.
Increasing awareness and acceptance of dental implant-based treatment options along with advances in surgical and prosthetic options and techniques must allow for predictable restoration of various (and often less than ideal) situations. In the restoration of the largely or fully edentulous arch, removable prostheses have proven to provide outstanding benefits for patients, including increased comfort, an improved emotional state, and better nutritional and systemic health.1,2
Historically, removable implant-retained prostheses have relied either on a bar of various designs or individual (non-splinted) attachments, such as a ball or, more recently, locator abutments, for retention of the prosthesis.3 Each of these options presents distinct benefits and limitations.4 In a general sense, both attachment options (bars and individual attachments) offer retention to the appliance to provide resistance to vertical and horizontal displacement. These options differ in that non-splinted attachments primarily offer limited support to the occlusal load, making the appliance primarily tissue-supported. On the other hand, splinted or bar-type reconstructions offer the benefit of load-sharing, occlusal support, and greater ability to correct for misaligned implants.5-8 The laboratory can restore misaligned implants by casting, soldering, or welding attachments or milling the bar substructure in order to obtain a common path of insertion with the final prosthesis. However, a bar reconstruction frequently has limitations, including: lack of adequate space under the denture; limited access for hygiene; lack of passive fit; and higher cost of components, metal, and laboratory labor.6 Lack of adequate space for the bar often causes a significant compromise in the bulk of acrylic, leading to a higher rate of fracture and tooth loss with the appliance, compromised esthetics caused by less than ideal positioning of denture teeth, and less than ideal occlusal schemes. Also, the lack of vertical space or close proximity of implants often hinders the patient's ability to maintain ideal hygiene. With the loss of a critical implant, other longer-term complications can potentially arise with bar reconstructions. Individual or non-splinted attachments have limitations as well, including: inability to correct for extreme divergence of implants (generally greater than 40°) around the arch; limited ability to provide ideal retention with poor implant distribution or number; and inability to provide for rigid load-sharing when splinting is indicated.
Presented below is an alternative technique to traditional bar reconstruction. It provides rigid splinting of individual implants for load-sharing and cross-arch stabilization, an implant-supported appliance, and a simple solution should the loss of an implant or need for an additional implant arise during the course of treatment without having to alter or re-fabricate a bar.7 This technique allows for extreme angulation correction with a common path of insertion, ease of hygiene access, and passivity of fit while requiring a minimal amount of space within the denture base to minimize potential fracture or esthetic and occlusal compromise of the final prosthesis.
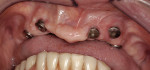
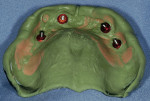
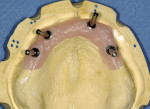
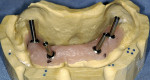
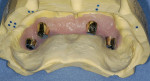
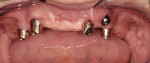
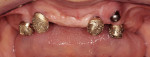
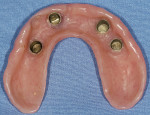
This prosthetic option can be viewed as "secondary splinting" as opposed to unsplinted abutments or the "primary splinting" provided by a traditional bar. In this technique, the splinting of individual implants is accomplished by the supra-structure (denture) upon its insertion over the abutments (Figure 1 and Figure 2). This is not a new technique, although there has been a scarcity of literature about it over the past 15 years. This is reminiscent of the periodontal prosthesis, better known as a telescopic coping or Konus crown technique, whereby individually milled abutments are fabricated for each implant to a common path of insertion. They most often have a 6° taper (there are case reports in the literature of varying tapers), with a continuous taper to the base and no chamfer or shoulder. Each custom-milled abutment can be fabricated by traditional milling procedures or with CAD/CAM and is made parallel to all the abutments in the arch to provide a common path of insertion for even the most divergent implants (Figure 3, Figure 4, Figure 5).
On top of each "primary" abutment, the laboratory fabricates an individual coping with precise tolerances by means of waxing/casting, electroformation, or milling. Each individual abutment, with its corresponding coping, provides a retentive element through the intimacy of fit and conical configuration. Through the curing of the copings into the denture base with acrylic, the individual implants become splinted together by virtue of the denture's "secondary splinting." The combination of ideal fit tolerances of each milled abutment and coping and a common path of draw culminate to provide a retentive appliance with rigid splinting of the implants (Figure 6, Figure 7, Figure 8, Figure 9). This allows for unimpeded hygiene access and a minimal space requirement inside the denture to achieve maximal bulk and strength of prosthetic materials with ideal tooth position and occlusion.
Technical Notes
A 6° taper provides ideal "tension" between the abutment and coping, with minimal friction that would lead to wear. The abutment design with a continuous taper as opposed to a chamfer or shoulder is ideal for continued seating of the coping on the abutment with no apical stop. If there is wear and associated loosening of the abutment/coping unit, polishing of the occlusal aspect of the abutment will allow the coping to sit further down on the abutment and regain retention. If an individual implant is lost, the coping can easily be removed from the denture and the space filled with acrylic. However, if additional implants are placed, then a new coping can easily be incorporated into the prosthesis with no need to alter the additional abutments or copings.
Besimo 7 has reported outstanding retention with as little as 4 mm of abutment height and a coping thickness as slight as 0.4 mm, which provides an ideal solution where there is limited interarch restorative space or significant buccal angulation of implants that would otherwise encroach on the teeth or flange of the denture.
An additional application of this technique is the ability to combine teeth and implants in one prosthesis through the cementation of a milled coping on the prepared tooth and a corresponding (secondary) coping, which gets incorporated into the prosthesis. In situations where a denture base and flange are not indicated, as is found in a traditional "fixed" restoration, this technique can be employed by incorporating the copings into a fixed-bridge framework. This permits the patient to remove the traditional bridge (no cementation) for access to hygiene in even the most ridge-lapped situation. It also enables prosthetic replacement of significant ridge defects with facial support while keeping the ability to maintain hygiene unimpeded.
Conclusion
Increasing awareness and access to dental implant-based treatment for partially and fully edentulous patients has given rise to a growth in both surgical and prosthetic techniques and procedures to simplify clinical care. Restoration of implants with significant misalignment not only presents a challenge to the laboratory but also leads to increased complications and potential failure. Presented is a technique to address the need for a common path of insertion while providing "secondary" splinting of individual implants with minimal compromise to esthetic, biologic, and mechanical concerns. The use of custom-milled abutments with telescopic copings can be employed to accomplish this.
References
1. Morais JA, Heydecke G, Pawliuk J, et al. The effects of two implant overdentures on nutrition in elderly edentulous individuals. J Dent Res. 2003;82(1):53-58.
2. Feine JS, Carlsson GE, eds. Implant Overdentures: The Standard of Care For Edentulous Patients . Hanover Park, Ill: Quintessence Publishing; 2003.
3. Krennmair G, Weinlander M, Krainhofner M, et al. Implant-supported mandibular overdentures retained with ball or telescopic crown attachments: a 3-year prospective study. Int J Prosthodont . 2006;19(2):164-170.
4. Vogel RC. Implant overdentures: a new standard of care for edentulous patients current concepts and techniques. Compend Cont Educ Dent . 2008;29(5) 270-276.
5. Kim Y, Oh TJ, Misch CE, et al. Occlusal considerations in implant therapy: clinical guidelines with biomechanical rationale. Clin Oral Implants Res . 2005;16(1):26-35.
6. Phillips K, Wong KM. Space requirements for implant-retained bar-and-clip overdentures. Compend Contin Educ Dent . 2001;22(6):516-518,520,522.
7. Besimo C. Removable Partial Dentures on Osseointegrated Implants . Hanover Park, Ill: Quintessence Publishing; 1998.
8. Gulizio MP, Agar JR, Kelly JR, et al. Effect of implant angulation upon retention of overdenture attachments. J Prosthodont . 2005;14(1):3-11.
About the Author
Robert C. Vogel, DDS
Private Practice
Palm Beach Gardens, Florida