The PreXion3D Cone Beam Imaging System
Technology offers clinical and diagnostic advantages for use in endodontics.
For the past century, dentists have relied on 2-dimensional (2-D) radiographic imaging for diagnosis and treatment planning. With the introduction of cone-beam computed tomography (CBCT) and the subsequent growth of the industry, all dentists now have tools available for more accurate diagnosis and treatment.1 The ability to look at a tooth in any direction and orientation as well as in three dimensions (3-D) eliminates much of the guesswork commonly experienced with 2-D radiographs. Dentistry has been limited, in most cases, to only a buccal–lingual view provided by periapical, bitewing, and panoramic radiographs with the occasional axial view of an occlusal film. Medical CT scans and images began in the early 1970s, and were sometimes used by dentists, offering the first multi-plane views, more commonly known as “slices.”2 Distortion of CBCT is minimal based on the geometry of the 3-D pixels known as voxels. These voxels are cube-shaped and isometric-shaped, with the X, Y, and Z axes all equal in length. The voxel is one important factor in determining the resolution of an image. High-resolution scanners offer voxel sizes between 76 µm to 125 µm. Minute structures are not as clearly visible above 125-µm. CBCT scanner resolution varies depending on which model and manufacturer is chosen, with ranges from a very small 76-µm to a fairly large 500-µm (½ mm) voxel size. For endodontic purposes, the resolution should be near the smallest voxel size to get the highest-quality information.1-7
The adoption of 3-D cone-beam imaging is appropriate and has important advantages for all modalities of dentistry. From every specialist to the general dentist, the increased amount of radiographic information, as well as increased accuracy, will aid in the most definitive diagnosis possible. With the high demands patients place on their dental professionals, CBCT will certainly help to achieve these levels of dentistry.
CBCT and Endodontics
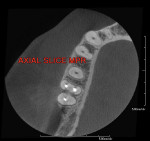
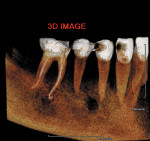
Endodontics is a field that is rapidly adopting the use of high-resolution, high-quality images generated by systems such as the PreXion 3D CBCT (PreXion, Inc, https://www.prexion.com/dental), and for good reason. The inherent geometric deficiencies and limitations of 2-D radiographs make the CBCT scan a valuable adjunct to investigate the root morphology in both 3-D and multiplanar reformation (MPR) images. The typical periapical radiograph will show superimposed canals in the anteriors, bicuspids, and molars as well as unwanted bone densities both buccal and lingual to the affected tooth, rendering many of the images to be of poor quality. The ability to view 3-D and MPR slices in cross-section, long axis, and oblique directions gives the ability to follow all canals in any direction and show their relationship and measurements from other known structures. This virtual tour of the root morphology is a great benefit to the diagnosis and the final treatment outcome (Figure 1, Figure 2, Figure 3, Figure 4).
Case Presentation
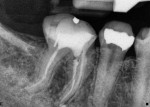
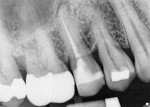
A 54-year-old woman presented several months after endodontic treatment with pain on both palpation and pressure; she was avoiding normal function on the side of the mouth that was painful. The patient’s chief complaints were sensitivity to biting, pressure, and chronic low-grade pain in the lower right quadrant. Visual soft tissue evaluation showed no redness or swelling and no obvious disease. Teeth Nos. 28 through 30 had no mobility and percussion tests resulted in a negative reaction only on tooth No. 30. A digital periapical radiograph showed minimal pathology, with only a slight widening of the periodontal ligament space around the mesial roots of tooth No. 30 (Figure 5). In the digital periapical radiograph, the roots appeared to be completely obturated, and a small puff of sealer extended through the apex of the mesial roots. The distal root structure showed no pathology and obturation appeared to be complete. There was very little indication of periapical radiolucency in either of the root apecies.
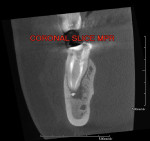
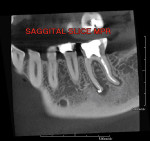
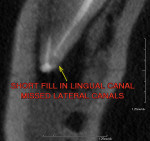
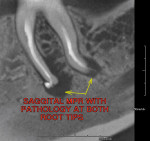
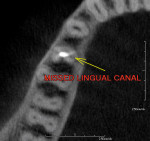
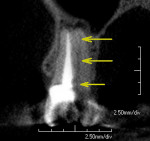
A PreXion 3D CBCT scan was taken to aid in the diagnosis and revealed a completely different picture. The coronal MPR image (mesial to distal) revealed a short fill near the apex and the presence of lateral canals at the mesial–lingual root (Figure 6) and a moderately large radiolucency that was not visible on the periapical radiograph (see Figure 2). Another view from the sagittal MPR shows a moderate radiolucency that was not visible at all in the digital periapical radiograph (Figure 7). Diagnosis and treatment based on the CBCT imaging was very different when compared to the 2-D periapical radiograph that did not show the short fill or the radiolucencies. The referring dentist had not committed to a final restoration and had indicated the possibility of a vertical root fracture to the patient.
With the detailed high-quality 3-D CBCT images, the identification of the actual problem was clearly apparent, and could be properly diagnosed with appropriate treatment recommended to the patient. Three different treatment plans were presented to the patient. The first option was re-treatment of the root canal to obtain complete obturation of the canals. The second treatment offered was an apicoectomy to remove the infected root tips and granulation tissue. The third option was tooth extraction and placement of an implant fixture.
When reviewing 2-D radiographs, the untrained patient has difficulty understanding what they are looking at. Another important advantage of high-quality CBCT images is patient education and case presentation. The CBCT 3-D and MPR images were used to help the patient better comprehend the endodontic issues involved and make an educated treatment decision. The patient elected to have an apicoectomy done on the mesial and distal roots and the cyst and granulation tissue were removed. One more advantage for the dentist and the patient using CBCT is that surgery can be easily accomplished because bone thickness and exact dimensions and location of the lesions can be accurately determined prior to surgery. In this case, minimally invasive protocols were used because both 3-D data and MPR images were available during surgery. The patient appreciated the reduced trauma and the minimal sized surgical site using the CBCT information. Postoperatively, the patient had no symptoms and healed normally.
As noted earlier, the identification of missed canals is difficult to see in a buccal–lingual projection of the periapical radiograph because one canal is superimposed over the other (Figure 8). Looking at this radiograph, periapical pathology can be seen in an apparent normally obturated canal. Digital 2-D radiography with the ability to enhance shading, color, and other parameters has improved diagnostic capabilities but cannot show what CBCT scans allow dentists to see. A CBCT scan allows clinicians to look for pathology in MPR slices to identify the actual problem before invasive procedures are performed. The axial view (top to bottom) (Figure 9) shows that a lingual canal was left untreated. The coronal view confirms the diagnosis (Figure 10), allowing treatment to be initiated and completed. The CBCT scans allow for accurate measurements to find the canal with minimal access through the crown.
Conclusion
Today, endodontists as well as general dentists are benefiting from the diagnostic capabilities of the high-resolution CBCT scanners available over conventional 2-D periapical radiography. The diagnostic capabilities of 3-D CBCT should be apparent from the cases shown in this article. CBCT has many other advantages and will assist the diagnosis and treatment planning processes with dental implants, periodontal evaluation, bone grafting and sinus augmentation, oral surgery, orthodontics, and supernumery and impacted teeth, and give patients a better understanding of the treatments that are offered to them. The author’s own experience is one of greater patient acceptance, not only of treatment plans, but an ownership and understanding of the dental diseases from which they suffer. The author would encourage all dentists to seriously evaluate the advantages of CBCT for the most complete diagnosis and treatment planning possible.
References
1. Zinman E, White SC, Tetradis S. Legal Considerations in the use of cone beam computer tomography imaging. Calif Dent Assoc J. 2010;138:49-56.
2. No author listed. For the patient (history of x-ray). J Am Dent Assoc. 2004;135:1643.
3. Patel S, Dawood A, Whaites E, PittFord T. New dimension in endodontic imaging: Part 1. conventional and alternative radiograpic systems. Int Endodont J. 2009;1-16.
4. Leuzingera I, Dudicb A, Giannopoulouc C, Kiliaridisd S. Root contact evaluation by panoramic radiography and cone-beam computed tomography of super high resolution. Am J Orthod Dentofacial Orthop. 2010; 137:389-392.
5. Hilgers ML, Scarfe WC, Sheetz JP, Farman AG. Accuracy of linear temporomandibular joint measurements with cone beam computed tomography and digital cephalometric radiography. Am J Orthod Dentofacial Orthop. 2005;128:803-811.
6. Stavropoulos A, Wenzel A. Accuracy of cone beam dental CT, intraoral digital and conventional film radiography for the detection of periapical lesions. An ex vivo study in pig jaws. Clin Oral Investig. 2007;11:101-106.
7. Scarfe WC, Levin MD, Gane D, Farman AG. Use of cone beam computed tomography in endodontics. Int J Dent. 2009;2009:634567.
About the Author
Dan C. McEowen, DDS
Private Practice
Hagerstown, Maryland