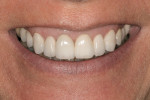
A Multidisciplinary Approach to Improvements in the Esthetic Zone
Gregory R. Gillespie, DDS
Long-term predictable results with zirconia restorations and implants in the esthetic zone can be achieved with a proper understanding of restorative and esthetic principles.
Dental practitioners are inundated with options for esthetic improvement in a patient’s smile. In the past, porcelain-fused-to-metal (PFM) restorations were the standard for esthetic excellence. Today, there are several varieties of esthetic porcelains, lithium-disilicate crowns, and zirconia restorations. When a patient desires a change to their smile, what factors help to decide the optimal type of restoration? How can the clinician be confident that the restorations will remain esthetic 5, 10, or even 20 years after placement? The difficulty of maintaining a high esthetic standard increases exponentially with the addition of missing teeth in the esthetic zone. Single-tooth implants are often the optimal solution for missing teeth, but meticulous planning with surgical placement and soft tissue management is key to long-term esthetics.
The general practitioner charged with creating a new smile for a patient incorporating multiple restorations and implants in the esthetic zone must have a solid understanding of the periodontium and the types of restorative materials that increase the potential of long-term esthetic success. The position of the osseous crest plays a major role in determining marginal placement of the final restorations on natural teeth and implants. The practitioner can be confident that the restorations will maintain a high esthetic standard for many years when appropriate protocols are established and followed.
Case Presentation
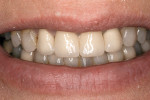
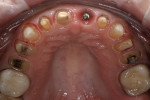
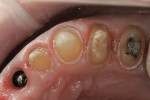
A 47-year-old woman presented with a chief complaint of a “loose” central incisor. Tooth No. 8 had a failing post-and-core build-up under a PFM crown as a result of recurrent decay (Figure 1). The patient was asymptomatic but had noticed increased mobility of the crown over the past few months. Before creating a treatment plan, other complaints the patient had with her smile were explored. She noted that she never liked the look and opacity of the crowns placed on teeth Nos. 7 through 10. The patient added that the discoloration of the posterior teeth appearing in her smile was bothersome, and she desired whiter teeth in both arches.
Clinical Findings
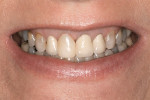
A comprehensive clinical examination found a healthy dentition with no signs of additional decay. The patient had stable occlusion, with no signs of parafunctional habits or excessive occlusal wear. Areas of localized recession were present and mainly limited to the posterior mandible. She presented with an Angle class I molar relationship, with minimal crowding limited to the mandibular anterior teeth. The temporomandibular joint was healthy with no sounds or pain. The periodontal examination revealed healthy tissue in both appearance and probing levels. Bone height was normal throughout the mouth, with no signs of periodontal disease. An esthetic examination of the teeth considered for treatment exhibited the following findings (Figure 2):
- No. 4 had an existing composite restoration with an amalgam lining that gave the tooth a grayish hue.
- No. 5 had undergone root canal therapy through an existing composite restoration, with a temporary filling placed.
- No. 6 had a discolored cervical composite restoration.
- No. 7 had a PFM restoration.
- No. 8 had a PFM restoration with a failing post-and-core build-up.
- No. 9 had a PFM restoration.
- No. 10 had a PFM restoration.
- No. 11 had a discolored cervical composite restoration.
- No. 12 had a discolored cervical composite restoration and distal–occlusal composite restoration with amalgam lining that gave the tooth a grayish hue.
- No. 13 had a mesial–occlusal–distal resin-composite restoration in good repair with an amalgam lining that gave the tooth a grayish hue.
Treatment Planning
The treatment plan was built around the patient’s chief complaint of a failing central incisor, tooth No. 8. That tooth would require extraction due to the limited amount of healthy tooth structure remaining. A 3-dimensional cone beam volumetric tomography revealed sufficient healthy bone for immediate implant placement. Because of the unpredictable quality of bone at placement of the implant, the patient would wear a treatment partial, or “flipper,” for 4 to 6 months during osseointegration of the implant. A provisional crown would then be fabricated to sculpt the tissue to the desired shape and contour.
After 1 to 3 months of sculpting the tissue around tooth No. 8, teeth Nos. 4 through 13 would be prepared for full-coverage porcelain restorations with a zirconia core. The option to use a mixture of veneers and full-coverage restorations was discussed, but the treatment plan again centered around the implant restoration. The implant system did not offer a zirconia abutment, magnifying the need for a restoration that could block out the darkness of a metal abutment while maintaining excellent esthetics. In addition, several teeth had undergone previous root canal therapy, which could vary in color over the coming years. Therefore, in an effort to keep uniformity and maximize esthetics, a zirconia restoration material was chosen for restoring all of the teeth included in the plan.
Treatment
In the first phase, tooth No. 8 was extracted atraumatically and the bone was examined to determine its quality. There were no signs of dehiscence, fenestration, or infection. The buccal plate was completely intact. An osteotomy was performed beyond the apex of the tooth, increasing the degree of primary stability of implant placement. The entire esthetic success of the case would be determined at the following crucial step of implant placement.
It is ideal to place the implant 3 mm apical and 2 mm palatal to the gingival zenith to achieve predictable and stable tissue height.1-4 Tissue esthetics will be compromised if the implant is placed too deep, too shallow, or too facially, resulting in a less than desirable final product. The width and length, platform switching, and collar design of the implant are also important aspects to consider before implant placement in an immediate extraction site.
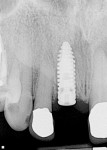
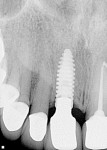
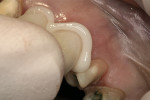
A 4-mm x 13-mm implant was placed in the extraction site after subsequent osteotomy preparation (Figure 3). The implant was initially very stable and a healing cap (at implant level) placed. Primary closure was not achieved. The clot formation inhibits a long junctional epithelial attachment that might invade the implant site if it is completely covered by gingiva through primary closure.5 The treatment partial was fitted to the patient and standard postoperative medications and procedures were completed.
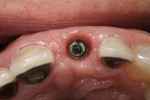
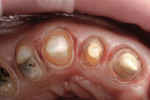
At 4 months, the healing abutment was removed (Figure 4). A composite crown was fabricated on a temporary abutment and screwed into place. After 4 weeks of sculpting the tissue, the temporary was removed and recontoured to improve gingival esthetics and contour. The patient remained in the temporary crown phase for another 6 months.
Marginal Placement
The patient’s osseous crest position, which plays a crucial role in the long-term esthetics of any restoration, was determined during the treatment-planning phase. Patients can be categorized into three osseous crest positions: normal crest (2 mm combined epithelial/connective tissue attachment); high crest (less than 2 mm combined epithelial/connective tissue attachment); or low crest (greater than 2 mm combined epithelial/connective tissue attachment). The osseous crest position is determined through sounding with a periodontal probe. Patients with a normal osseous crest position are usually resistant to recession, even with subgingival marginal placement, as long as the biologic width is not violated.6
Patients with a high osseous crest position are susceptible to periodontal inflammation because the biologic width can be easily compromised if the margin is placed even slightly subgingivally. The bone must be recontoured first to establish a more favorable sulcus depth above the osseous crest if margins necessitate subgingival placement.6
The real danger appears in patients with a low osseous crest position. The instability of the tissue above the bone is high and, if traumatized, it can recede quickly. The clinician should consider placing margins supragingivally, completely avoiding trauma to the tissue, or perform a gingivectomy to establish a shallower, more stable pocket.7
Supragingival or equi-gingival margin placement is ideal, when possible, in esthetic restorations because of their low risk of damaging the periodontium, instigating an inflammatory response, or initiating recession. Porcelain can be used with these margins because it can retain translucency in the cervical region. However, several circumstances necessitate a subgingival margin, including: the need to mask discoloration at the cervical region, caries extending below the gingiva, old restorations with subgingival margins, gaining required resistance and retention form, and improving contours of spaced or misshaped teeth. Understanding the osseous crest position in these circumstances is critical to avoid unsightly results from tissue recession.8
Given a normal osseous crest position, the margins were placed equi-gingivally, or 0.5 mm subgingivally (Figure 5). The previous restorations on teeth Nos. 7 through 10 as well as the previously root canal treated teeth necessitated subgingival margin placement. The placement of the implant abutment margin also was effected by osseous crest position.9The most important factor was the position of the interproximal bone.10 The type of implant placed had a roughened surface to the connection interface, minimizing the amount of interproximal bone loss after placement (Figure 6). The abutment style also mimicked platform switching, allowing for the formation of a natural biologic width. After all of these considerations, the implant abutment margin was placed 1 mm subgingivally, maintaining 2 mm of biologic width and decreasing the concern for future tissue recession.
Impressioning
Proper tissue management is vital to an accurate, detailed impression. The patient was given a chlorhexidine rinse 2 weeks before the preparation date to improve tissue health. The type of retraction necessary is often dictated by marginal placement. Atraumatic cord placement is a technique that requires mastery. Retraction cord can be placed with minimal concern about recession of the tissue in the normal and high osseous crest patient. However, great care must be taken if the patient has a low osseous crest, as any trauma to the tissue when placing cord can lead to recession.11
Retraction paste provides adequate retraction with supra-, equi-, and even slightly subgingival margin placement. Retraction pastes are clay-like materials that contain a hemostatic agent to control bleeding while simultaneously providing a degree of retraction, due to the thickness of the paste.12 Such materials are highly desirable because they provide a favorable tissue response.
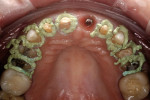
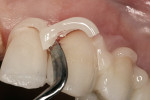
In this case, Expasyl was applied around all of the margins (Figure 7). After 2 minutes, the preparations were completely rinsed, and the tissue was inspected for adequate retraction and hemostatic/moisture control (Figure 8). The impression was then captured with a regular-set polyvinyl siloxane impression material.
Temporization
All too often, temporary restorations are given little attention when in reality they play a very significant role in the long-term success of the treatment. Careful attention must be paid to marginal accuracy. The patient can maintain healthy tissue with accurate temporary margins. Inflammation quickly arises with ill-fitting margins, creating a difficult environment that compromises the final cementation/bonding procedure. The use of a chlorhexidine rinse while the patient is in the temporary phase improves tissue health at the seating appointment.13
Cementation
The patient was anesthetized and the temporaries were removed. Meticulous temporaries coupled with the patient’s compliance during the 4-week temporization phase provided a healthy environment to predictably seat the final restorations (Figure 9).
The implant abutment was seated and torqued according to the manufacturer’s specifications. An x-ray was taken to verify the complete seating of the abutment. The gingival portion of the metal abutment, not covered by the final restoration, was opaqued to lessen the visibility of the metal through the tissue. The final zirconia restorations were tried in and evaluated for marginal fit, occlusal accuracy, and overall appearance. The teeth were isolated and prepared for cementation after proper verification during try-in.
The teeth must be clean to ensure the strongest bond possible. Pumice paste effectively removes any residue left by temporary crowns.14 An additional application of a disinfectant/rewetting agent (eg, Gluma®, Heraeus, www.heraeus-kulzer-us.com; Tublicid Red, Global Dental Products, www.gdpdental.com) has beneficial results. Disinfectants reduce the bacterial contamination to a greater degree than rinsing/drying/acid-etching alone.15 A clean surface and low bacterial count leads to better bond strengths with less chance of sensitivity and leakage, resulting in longer-lasting restorations.16 Additionally, the application of a rewetting agent enhances bond strength by lubricating dentinal tubules to increase the flow of resin deeper into the tubules.17
The teeth were cleansed with pumice and washed. Chlorhexidine was then scrubbed over the teeth and subsequently washed. A disinfectant/rewetting agent (in this case, Tubulicid Red) was applied in two coats, scrubbing continuously for 20 to 40 seconds each, and air-dried.
Zirconia restorations can be cemented successfully with several types of luting agents because they rely primarily on resistance and retention form for long-term success.18 However, recent studies suggest that primers or surface treatments can improve zirconia bond strengths to resin cements.19-20 Regardless, self-adhesive resin cements have distinct advantages in the cementation of zirconia restorations. Clean-up with self-adhesive resin cements is quick and simple. There is extended working time, but a gel phase is quickly achieved with a tack-cure. No separate etching, priming, or bonding steps are required because of the self-adhesive nature of the cement. These features allow the clinician to be more effective in the cementation procedure.
The implant abutment was again torqued and the abutment space was filled with a cotton pellet before final cementation. The zirconia restorations were filled with self-adhesive resin cement (Maxcem Elite™, Kerr Corporation) and seated (Figure 10). Finger pressure was applied while a quick tack-cure was performed. Clean-up of the cement at the margins with a gold knife was done and contacts were flossed (Figure 11). The process was repeated until all of the restorations were positively seated. All margins were cured again for 20 seconds on the buccal and lingual. Consistent pressure was applied for 5 minutes while final curing of the cement was achieved. Occlusion was checked with marking paper and slight occlusal adjustments were made to ensure even centric contacts and excursive movements. All contacts, centric and excursive, were left very light on the implant crown in an effort to minimize forces and overloading the implant.
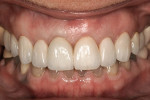
The patient returned 6 weeks later for final evaluation of tissue health around the zirconia and implant restorations (Figure 12 and Figure 13). The patient was very pleased with her smile transformation (Figure 14 and Figure 15) and reported no discomfort or occlusal issues.
Conclusion
Creating long-term esthetics with multiple zirconia restorations and implants in the esthetic zone is challenging. A clear understanding of a patient’s osseous crest position aids in surgical implant placement and marginal placement of the final restoration, increasing the predictability of tissue esthetics over time. The use of retraction paste when possible allows for favorable tissue management. Furthermore, self-adhesive resin cements allow for a more effective cementation procedure. Implementation of these few points enables a long-term, predictable result with zirconia restorations and implants in the esthetic zone.
Disclosure
The author has received financial support from Kerr Corporation.
Acknowledgment
The author would like to thank his ceramist, Mike Archibald, for his teamwork on this difficult case, and acknowledge his unique ability to make all restorations look incredibly beautiful and lifelike.
References
1. De Kok IJ, Chang SS, Moriarty JD, et al. A retrospective analysis of peri-implant tissue responses at immediate load/provisionalized microthreaded implants. Int J Oral Maxillofac Implants. 2006;21(3):405-412.
2. Solakoglu O, Cooper LF. Immediate implant placement and restoration in the anterior maxilla: a tissue-related approach. Observations at 12 months after loading. Int J Periodontics Restorative Dent. 2006;26(6):571-579.
3. Gallucci GO, Belser UC, Bernard JP, et al. Modeling and characterization of the CEJ for optimization of esthetic implant design. Int J Periodontics Restorative Dent. 2004;24(1):19-29.
4. Cooper LF, Ellner S, Moriarty J, et al. Three-year evaluation of single-tooth implants restored 3 weeks after 1-stage surgery. Int J Oral Maxillofac Implants. 2007;22(5):791-800.
5. Tarnow DP. “Extraction Site Micro-gap and Treatment Options in Implant Therapy.” Summit by the Sea Focusing on Tissue Wellness in Implant Dentistry. Ritz-Carlton Hotel, Key Biscayne, Florida. 27 June 2009. Lecture.
6. Spear FM. Using margin placement to achieve the best anterior restorative esthetics. J Am Dent Assoc. 2009;140(7):920-926.
7. Lowe RA. “The Master Impression: The Elusive Pursuit of Perfection!” Lecture. GCA Training. 17 June 2009. Web.
8. Spear FM. “Anterior Esthetic Crown Preparation.” Lecture. Advanced Esthetics & Interdisciplinary Dentistry Education Series.2006. DVD.
9. Kois JC. Predictable single-tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2004;25(11):895-900.
10. Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
11. Lowe RA. The Master Impression: The Elusive Pursuit of Perfection! GCA Training, 2009. Web. 17 June 2009. Lecture.
12. Poss S. An innovative tissue-retraction material. Compend Contin Educ Dent. 2002;23:13-17.
13. Sorensen JA, Doherty FM, Newman MG, et al. Gingival enhancement in fixed prosthodontics. Part I: Clinical findings. J Prosthet Dent. 1991;65(1):100-107.
14. Grasso CA, Caluori DM, Goldstein GR, et al. In vivo evaluation of three cleansing techniques for prepared abutment teeth. J Prosthet Dent. 2002;88(4):437-441.
15. Christensen GJ. Disinfection of tooth preparations—why and how? Clin Rep.2009;2(11):2-3.
16. Saraç D, Bulucu B, Saraç YS, Kulunk S. The effect of dentin-cleaning agents on resin cement bond strength to dentin. J Am Dent Assoc. 2008;139(6):751-758.
17. Ritter AV, Heymann HO, Swift EJ Jr, et al. Effects of different re-wetting techniques on dentin shear bond strengths. J Esthet Dent. 2000;12(2):85-96.
18. Palacios RP, Johnson GH, Phillips KM, et al. Retention of zirconium oxide ceramic crowns with three types of cement. J Prosthet Dent. 2006;96(2):104-114.
19. Magne P, Paranhos MP, Burnett LH Jr. New zirconia primer improves bond strength of resin-based cements. Dent Mater. 2010;26(4):345-352.
20. Cavalcanti AN, Foxton RM, Watson TF, et al. Bond strength of resin cements to a zirconia ceramic with different surface treatments. Oper Dent. 2009;34(3):280-287.
About the Author
Gregory R. Gillespie, DDS
Private Practice
Vancouver, Washington