Individual Tooth Selection Process
Clinical and laboratory-based evaluation tools facilitate communication between the dentist and laboratory ceramist for the best possible case outcome.
The phrase “the best dentistry is no dentistry,” is one that anyone who works in dentistry is familiar with and can appreciate.The reality today, however, is that we live in a world of instant gratification. Patients go to their dentist not just for care, but also with demands for instant transformations. These transformations oftentimes involve elective dentistry. The goal of restorative dentistry—elective dentistry specifically—should involve the least amount of teeth as possible to reach the outcome that should satisfy the patient’s desires.
In dentistry, dentists and laboratory ceramists should discuss the issue of preparation design, full coverage, three-quarter preparations, or facial veneers. These discussions should consider factors that tend to determine the success of the outcome, such as the minimal number of teeth to be surgically included to accomplish the desired goal. Therefore, it is important to consider every aspect of the dentition, before preparation, to provide ideal esthetics. This must be accomplished while maintaining as much natural tooth structure as possible to meet the goals of the patient and the goals of restorative dentistry, which are minimal dentistry and esthetic excellence. However, of paramount importance to the entire process is the collaborative and ongoing dialogue that occurs between the dentist and laboratory ceramist regarding how to best deliver the patient’s anticipated results. With a shared understanding of the patient’s condition, his or her expectations, and what can be done and with what impact to the dentition, the restorative team can realize success in providing the least invasive treatment possible. This article presents the clinical and laboratory-based evaluation tools that facilitate communication between the dentist and laboratory ceramist in order to properly treatment plan and restore a patient who desires an esthetic smile enhancement.
Evaluation Process for Tooth Consideration
There are many theories or slogans in dentistry that are used to determine the number of teeth to be veneered in order to create ideal esthetics. All too often these tend to be based on faulty biases. “Two, four, eight, or more,” is one of the most rehearsed slogans and often stands in the way of making a decision based on minimal dentistry. Each patient must be evaluated on individual needs. It is imperative to not only carefully evaluate the patient’s individual pre-existing condition, tooth position, and color, but their functional envelope, phonetic components, and perceived goals for outcome as well, before selecting the possible treatment modalities.1-3 In doing so, it is necessary to complete a comprehensive examination with a complete set of records and photographs. These records should be obtained to evaluate how the functional and esthetic results desired may be accomplished. A mounted model is another tool that should be considered and compared with facial photographs to analyze the desired modifications.
Three Modalities to Consider for Optimal Esthetics
The functional and esthetic components of restoring teeth include planning the ideal alignment, shape and contour, surface morphology, incisal edge positions, and the opposing functional surfaces.4 The existing teeth can be moved orthodontically into position, or the tooth contours can be modified by subtraction or addition dentistry. Addition dentistry involves minimal or no preparation of hard tissue to correct esthetic concerns.5 Subtraction dentistry is the most invasive and can require significant hard tissue removal to achieve the desired results.5 Orthodontically repositioning teeth can also be very conservative, but requires significant time to accomplish, so the issue of retention becomes a concern.6 It is important to note that one modality is not necessarily better than the other, but that they all have their benefits and limitations.
Tools Needed for Proper Individual Tooth Selection Criteria
The patient’s models and photographs are used to evaluate any repositioning of the teeth beyond orthodontics that is necessary to achieve the treatment goals. Two types of laboratory wax-ups are essential for adequate assessment of treatment goals.7 An additive-reductive wax-up is accomplished by adding contour in wax to the existing dentition without removing any tooth structure.8 However, most cases will require reductive changes to be made to reach the ideal tooth position. This full-contour wax-up requires reducing hard tissue areas on the model to accomplish ideal contour goals. Both wax-ups are essential in making decisions regarding each individual tooth to be considered for restoration.9
Evaluation of Mock-Up
An intraoral mock-up, using a silicone matrix made from the additive wax-up or direct bonding, can be tested in the patient’s mouth by placing it over the existing dentition to create an intraoral mock-up.10 If the mock-up results are esthetically pleasing, then a phonetic evaluation should be undertaken. Evaluation of “f,” “v,” and “s,” sounds should be done to assess the overall form of the teeth. Most esthetic changes in the anterior incisors will have functional consequences. Protrusive, crossover, and canine guidance must be evaluated while the patient is wearing the mock-up.10
Minimal Teeth Philosophy
There are many reasons why a practitioner would want to involve the least number of teeth in a treatment plan in order to accomplish the desired goals. These reasons are directly parallel to the minimal preparation philosophy. This philosophy involves less preparation time, less anesthetics, fewer provisional restorations, and less potential for postoperative discomfort. There are also many reasons why the patient seeking care would want the least number of teeth included. These reasons often include decreased cost, shorter appointment times, and less potential for discomfort, to name a few.
Case Study
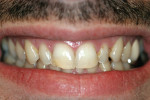
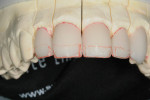
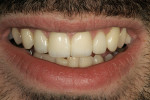
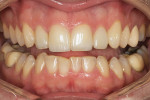
The following case is an example of how a minimally invasive philosophy was applied to the treatment of a 29-year-old man who desired a better smile and whiter anterior teeth (Figure 1). A comprehensive examination was performed, and a complete set of records and photographs was taken. Then, preliminary impressions and habitual bite registrations were taken. The models were mounted and compared with the facial photographs.
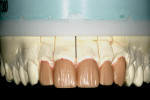
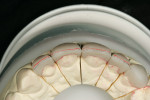
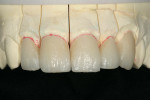
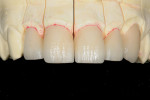
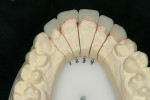
It was determined based on the diagnostic wax-up, the patient’s desires, and financial constraints that only four teeth would be included in the treatment plan to accomplish the desired goals. Laboratory additive and full-contour wax-ups were performed on teeth Nos. 7 through 10 (Figure 2 and Figure 3). This particular patient was not a candidate for minimal preparation veneers because of large failing composite restorations in the teeth in question.
Teeth Nos. 7 through 10 were subsequently prepared for veneers, and provisional restorations were fabricated from a shade B1 provisional material (PERFECTemp, Discus Dental, https://www.discusdental.com). The patient loved the new temporaries and did not want to change any contours or colors. However, within 2 weeks, he had broken off tooth No. 10 twice.
These breakages indicated that there was an obvious functional issue with the provisional restorations that needed to be analyzed. Upon examination, it was determined that the patient had minor prematurities in his posterior teeth and lack of canine guidance on his left side due to the thickness of the lingual surface of tooth No. 10. It then was determined that tooth No. 11 required preparation and restoration to regain canine guidance.
The patient was in the provisional restorations for another week with no other complications. To fabricate the final restorations, the ceramist poured a model from the impressions received from the dentist. Then, a full-contour wax-up of the veneer restorations was performed, and this was sprued onto the ring former. The wax-up was invested, burned out, and the appropriately colored IPS e.max Press ingot (Ivoclar Vivadent, https://www.ivoclarvivadent.us) was pressed onto the wax-up to produce the full-contour veneer restorations.
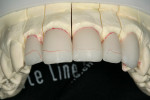
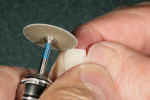
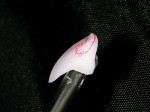
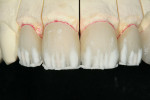
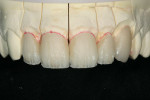
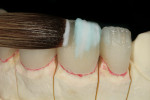
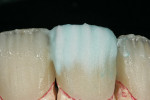
After pressing, the units were fit to the original dies, de-sprued, and ready for cutbacks. For this case, a 0.5-mm facial–incisal bevel cutback from the full contour was made, after which a trough was cut around the incisal half, preserving the silhouette edge. To accomplish this, the facial–incisal edge was outlined using a red pencil, and a 0.3-mm lead pencil line was placed 0.5 mm lingually (Figure 3). A contour stone (Komet 9001, Komet USA, https://www.kometusa.com) was used to bevel the facial–incisal edge back 0.5 mm (Figure 4). The value was drawn in, and a centered diamond disc (Komet K6974) was used to carefully cut in the value area, making certain that a halo effect was established (Figures 5, Figure 6, Figure 7).
Once the cutback was completed, the incisal–facial area was smoothed out to create a canvas for the internal effects. To create the internal effects, Gray, Salmon, and A3 stains were applied and fired (Figure 8). To shape the internal lobe structures, a mixture of internal powders was used (eg, for the mesial and distal lobes, a 50/50 mixture of OE4 and MM light; for the inner lobe, straight MM light and MM salmon) (Figure 9). Once the internal lobes had been formed, they were feathered out. After a thorough and careful evaluation, the eternal effects were fired (Figure 10).
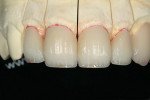
The segments of IPS e.max OE1 (Opal Clear Blue color tagged) and TI1 (incisal 1) were built to 0.5 mm, which was the exact thickness of the initial facial cutback, making it faster and easier to return to the original full contour (Figure 11). IPS e.max OE1 was fired to ensure that the high-value segments mimicked the enamel optics found in the natural teeth, after which the IPS e.max Opal Clear (color tagged blue) filled in the mesial and distal incisal grooves (Figure 12). The restorations were bisque-baked (Figure 13). Then, after using a diamond bur (Komet 842R) to cut in surface lobes in preparation for glazing (Figure 14), a coarse rubber wheel (Komet 9472C) was used to reestablish the deflective zones and redefine the line angles. The facial lobes were recreated with a diamond bur (Komet 842R) after the desired amount of perikymata was added with a diamond bur (Komet 850 016). The restorations were then glazed and polished (Figure 15). The final restorations then were seated and included teeth Nos. 7 through 11 (Figure 16, Figure 17, Figure 18).
Conclusion
In this particular case, the patient was extremely happy with his new smile and, 3 years postoperatively, has demonstrated no complications. How often can five anterior teeth be included to accomplish the desired goals, all while leaving one canine? This case may not be as rare as it appears. However, evaluating each tooth and aligning the desired goals with the minimal tooth philosophy can create a win-win for not only the patient, but also for the clinician and the laboratory ceramist.
References
1. Strassler HE. Minimally invasive porcelain veneers: indications for a conservative esthetic dentistry treatment modality. Gen Dent. 2007;55(7):686-694.
2. Panossian AJ, Block MS. Evaluation of the smile: facial and dental considerations. J Oral Maxillofac Surg. 2010;68(3):547-554.
3. Gross MD. Occlusion in implant dentistry. a review of the literature of prosthetic determinants and current concepts. Aust Dent J. 2008;53(Suppl 1):S60-S68.
4. Koczarski M. Smile makeover utilizing direct composite resin veneers. Dent Today. 2008;27(12):76-79.
5. Christensen GJ. Has tooth structure been replaced? J Am Dent Assoc. 2002;133(4):408-410.
6. Smallwood TW. Invisalign and porcelain: the contemporary restorative powerhouse. Alpha Omegan. 2009;102(4):148-151.
7. Rosenthal L. Preparation guidelines for less-invasive cosmetic restorations. Gen Dent. 2007;55(7):624-630.
8. Magne P, Douglas WH. Additive contour of porcelain veneers: a key element in enamel preservation, adhesion, and esthetics for aging dentition. J Adhes Dent. 1999;1(1):81-92.
9. Small BW. Pretreatment wax-ups and provisionals for restorative dentistry. Gen Dent. 2005;53(2):98-100.
10. Reshad M, Cascione D, Magne P. Diagnostic mock-ups as an objective tool for predictable outcomes with porcelain laminate veneers in esthetically demanding patients: a clinical report. J Prosthet Dent. 2008;99(5): 333-339.
About the Authors
Tim Huff, DDS
Private Practice
Boise, Idaho
Brad Jones, FAACD
Professional Dental Arts
Boise, Idaho