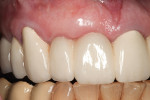
Examination and Treatment of the Complex Perio-Esthetic Patient
Dentists must pay attention to all of the minute details in order to render a successful esthetic outcome to periodontal treatment.
The saying, “the devil is in the details” is certainly one of the truisms of life, applicable in many arenas, including dentistry. Patients with complex treatment needs may only be properly served if those details are ferreted out and addressed. The ability of the dentist to properly identify and manage these details is dictated by training, including postgraduate and continuing education, experience, personal preference for certain dental disciplines, a dedicated amount of intellectual energy devoted to the analysis of the patient from many perspectives, as well as introspection of previous treatment results. Many of these patients may only be successfully treated with an interdisciplinary approach. Ignoring one or more factors contributing to the esthetic condition will lead to a less than optimum result and a dissatisfied patient. The purpose of this article is to present a comprehensive esthetic examination and the treatment of two patients with complex esthetic needs.
The Esthetic Examination
Over the years, many authors have presented their ideas for the evaluation of the esthetic patient. One comprehensive esthetic examination, originally presented by Dr. Leonard Abrams in the 1980s, with minor modifications since, continues to serve as a useful guide.1 His examination follows that of a good physical examination, starting with the more general and external findings and then progressing to the intraoral conditions. One critical part of the examination is questioning the patient and really listening to the responses. Very often, many healthcare professionals (including dentists) have been guilty of speaking too much and listening too little.
Meet the Patient
Meeting the patient is more than shaking hands and exchanging pleasantries. The first few moments of an appointment can yield very valuable information, such as the unprompted patient history, non-verbal clues in how the patient acts, and how the patient answers direct questions from the first staff members he or she encounters. Staff members such as the dental hygienist or dental assistant can be invaluable because the patient may not be as comfortable being completely forthright with the dentist. Patient comments may be prompted by having a “before and after” reference guide or a book such as Change Your Smile2 in the reception area. Patients often peruse these books looking for conditions similar to their own.
Some of the issues to be vigilant about in this initial interview are a history of esthetic changes, and whether there is any periodontal disease or trauma involved. Patient desires must be realistic and achievable. This is a key step, as a patient with unrealistic expectations will never be satisfied. It will be very helpful if there are previous records, photographs, models, and radiographs. Being able to review any available documentation will allow proper understanding of the esthetic change, especially related to the movement of teeth and periodontal disease.
Meet the Face
“Meeting the face allows the clinician to put the smile and oral structures into proper context. First, the relationship of the interpupillary line to the mid-sagittal plane is checked for squareness. If the intersection of these two lines is not a 90o angle, it will be important to have the maxillary incisal edge line follow the interpupillary line. Other features to consider are facial symmetry (seeing if the patient has an imbalance of one side to the other, either developmental or due to trauma), lip symmetry, movement symmetry in various motions (including a smile, a grimace, and while speaking) that will give clues to the amount of gingiva and teeth visible with various functions, and the relationship of the philtrum to the mid-sagittal plane and dental maxillary and mandibular midlines. Check the intersection of the interpupillary line and mid-sagittal plane for squareness. If the intersection is not at a 90o angle, it will be important to have the incisal-edge line follow the interpupillary line.
Meet the Mouth
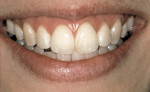
Smile Line Once the facial relationships have been studied, it is time to “meet the mouth,” the center of dental activities. The upper lip line must be examined to see if it is in an average location, is low, or high in function. The patient with a high smile line presents a significant challenge to the esthetic dentist (Figure 1). Be sure to have the patient smile or laugh spontaneously. This will give the true measure of how much of the dentition and gingival is visible. Many times when just asked to smile, patients will not reveal the complete extent of their smile. Patients who will not smile, smile tersely, or cover their smile with their hand may be giving non-verbal cues of their opinion of their smile.
Tooth-lower lip position may affect both esthetics and phonetics depending on the degree of overlap. Patients who predominantly show their mandibular anterior teeth in function may have additional challenges based on the small size of these teeth. The incisal edge lower lip relationship should be noted at the same time.
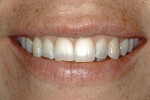
Three features that are interrelated are tooth prominence, horizontal tooth display, and vestibular appearance. In many cases, prominent teeth are also associated with a high smile line. Prominent teeth also may indicate a thin gingival – alveolar bone biotype, susceptible to gingival recession over time. It is imperative that the restorative dentist handles prominent teeth with a thin biotype very cautiously so as not to cause trauma-induced recession from tooth preparation or impression techniques. Horizontal tooth display may indicate the type of restorative material that should be used, even on maxillary first or second molars that may be visible when a patient smiles (Figure 2). This display is directly related to the vestibular appearance — wide or narrow — the existence of the “buccal corridor.”
Continuing to meet the mouth, inspect the tooth midlines to ensure that the midlines are lined up with the nose and philtrum along the mid-sagittal plane. Asymmetry may be indicative of a developmental problem or as a result of trauma, such as mid-face fracture or loss of a tooth with subsequent tooth drift.
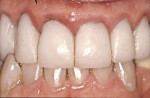
While cosmetic dentistry has traditionally focused on the color, contour, and texture of teeth and their restorations, gingival characteristics contribute significantly to the esthetic smile. Contour and thickness, or soft tissue biotype, will give some indication of the resistance of the gingival margins to recession. Gingiva with a thin biotype must be managed very delicately with any restorative procedure. These tissues are also more susceptible to recession resulting from toothbrush trauma or factitial habit. Adjacent gingival margin heights in the maxillary esthetic zone must also be considered. The gingival margins of the maxillary incisors and canines on one side should either all touch on a straight line or the margin of the lateral incisor should be slightly (about 1 mm) coronal to this line (Figure 3).3 When the gingival margin of the lateral incisor is apical to this line, the viewer’s eye is automatically drawn to this irregularity.
Open embrasures, otherwise known as the dreaded “black triangles,” also add or detract from the esthetic zone. Generally, the embrasure space of the maxillary central incisors will be filled with the interdental papillae if the distance between the crest of the bone and the interdental contact is < 5 mm. Patients who present with attachment/bone loss in the esthetic zone must be cautioned that there may be some embrasure exposure after periodontal therapy is completed.
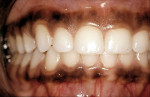
Altered passive eruption (APE) is the disruption of the migration of the gingival margin to the cervical area of the tooth during growth. This condition, whereby an excessive amount of the anatomic crown is covered with gingiva, is most often seen with a thick gingival/alveolar bone biotype, resulting in the “gummy smile.” In general, the width of the maxillary central incisor should be 75% to 80% of the height of this tooth. While the width of the tooth may be seen, the height of the anatomic crown can be determined using a periapical radiograph or estimated using a Chu Aesthetic Gauge (Hu-Friedy, https://www.hu-friedy.com), which is designed for the width-to-height ratio to be 78%. The location of the gingival attachment and amount of attached gingiva must be determined (Figure 4, Figure 5, Figure 6).4,5
Excessive gingival display may not be related to altered passive eruption. It could be the result of a skeletal condition known as vertical maxillary excess. Distinguishing the cause of excessive gingival display is critical. While APE may be managed with esthetic crown lengthening, vertical maxillary excess must be managed with orthodontics and/or orthognathic surgery.
As teeth are lost, the alveolar bone resorbs and may result in a collapsed edentulous ridge. The ridge loss may be classified as horizontal, vertical, or a combination of the two.6 The type of restorative treatment will dictate how the ridge is reconstructed. Implant placement may require bone augmentation procedures while soft tissue augmentation can accommodate an ovate pontic. There may also be isolated gingival defects (recession, Stillman’s clefts) that may be managed with periodontal plastic surgery procedures.
Most dentists focus on tooth characteristics when formulating an esthetic treatment plan. Several features to be mindful of are diastemas, overlapped/malpositioned teeth, discolored teeth, attrition, and tooth contours. These characteristics may require additional treatment considerations such as orthodontics, including forced eruption, bleaching before restorations, reestablishment of the vertical dimension of occlusion when severe occlusal attrition has occurred, or esthetic odontoplasty for teeth not receiving restorations. Transitional line angle position, contact point/area, and tooth surface texture should also be noted.
The final segment of the esthetic exam is evaluating phonetics. Both the labio-palatal dimension and location of the teeth and incisal edge length will affect the tongue and/or lips in the F-V position (making these sounds), the S position, and in swallowing. Patients with an anterior open bite or diastemas may have developed a visceral (infantile) swallowing pattern while a dentition in a normal position will allow for a somatic (mature) swallowing pattern. These features should all be analyzed while the patient is wearing provisional restorations, and the appropriate adjustments made and transmitted to the laboratory technician.
Case Presentation 1
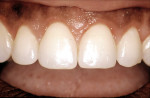
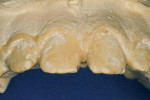
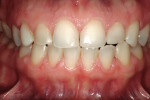
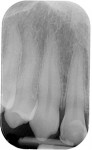
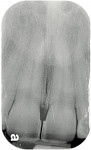
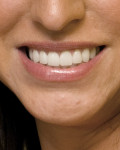
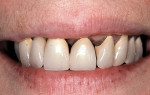
This patient was almost the victim of a monolithic examination and treatment plan. She presented to a “cosmetic dentist” for new veneers. She originally had natural diastemas (Figure 7 and Figure 8) that had been closed with composite veneers several years previously. Without considering the dimensions of the anatomic crowns, the 80% rule, or the relationship of the gingival margins to the teeth, the dentist had proposed ceramic veneers for the maxillary incisors, canines, and premolars. Had the treatment plan been executed as proposed, this patient would have had either boxy teeth or teeth too long for her lip positions. Periapical radiographs (Figure 9 and Figure 10) revealed the true dimensions of the crowns of the maxillary teeth. After esthetic crown lengthening7 (Figure 11), properly sized veneers were placed (Figure 12).
Case Presentation 2
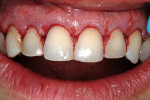
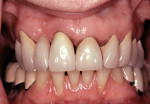
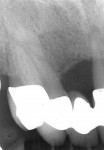
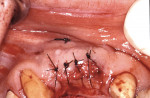
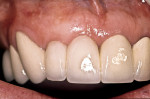
This esthetically demanding patient had undergone several plastic surgery procedures over the previous years, including facial rejuvenation, a tummy tuck, and breast augmentation. She had resective periodontal surgery after her previous reconstruction left her with minimal pocketing but she was extremely dissatisfied with the appearance of her teeth (Figure 13 and Figure 14). Note the Seibert Class 1 ridge defect in the maxillary right lateral incisor area and the unevenness of the gingival margins. The examination and treatment considerations included forced orthodontic eruption8 of the right central incisor as a means of leveling the gingival margins, as well as periodontal ridge augmentation for an ovate pontic in the lateral incisor area, and a new maxillary fixed reconstruction. Because of the loss of bone around the right central incisor (Figure 15), it was decided to sacrifice this tooth and reconstruct the ridge dimensions using autogenous connective tissue—a combination of submucosal9 and onlay connective tissue grafts.10 Despite the patient’s desire to accomplish all of these surgical procedures at once, at times it may be necessary to stage reconstruction procedures to achieve the best results (Figure 16, Figure 17, Figure 18). The reconstructed ridge has held its dimension for 15 years after treatment, with the patient being very satisfied with the result. Some practitioners may consider an implant option here. This would require some guided bone regeneration and may lead to some soft tissue challenges to achieve an acceptable outcome.
Conclusion
The treatment of the complex periodontal-esthetic patient begins with a comprehensive esthetic examination. Once the details of the current conditions have been identified, an interdisciplinary approach to treatment considerations is critical to formulating a staged treatment plan that will ensure the best result with patient satisfaction.11
References
1. Abrams L. The Esthetic Evaluation. 1986. Personal communication.
2. Goldstein RE. Change Your Smile: Discover How a New Smile Can Transform Your Life. 4th ed. 2009; Quintessence: Chicago, Ill.
3. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. 1994; Quintessence: Chicago, Ill. Figure 9-7.
4. Coslet JG, Vanarsdall R, Weisgold A. Diagnosis and classification of delayed passive eruption of the dentogingival junction in the adult. Alpha Omegan. 1977;70:24-28.
5. Ash MM, Nelson S. Wheeler’s Dental Anatomy, Physiology, and Occlusion. 8th edition. 2002; Saunders: Philadelphia, Pa.
6. Seibert JS. Reconstruction of deformed, partially edentulous ridges, using full thickness onlay grafts. I. Technique and wound healing. Compendium. 1983;4:437-453.
7. Jorgensen MG, Nowzari H. Aesthetic crown lengthening. Periodontol 2000. 2001;27:45-58.
8. Ingber JS. Forced eruption: alteration of soft tissue cosmetic deformities. Int J Periodontics Restorative Dent. 1989;9:416-425.
9. Langer B, Calagna L. The subepithelial connective tissue graft. J Prosthet Dent. 1980;44:363-367.
10. Seibert JS, Salama H. Alveolar ridge preservation and reconstruction. Periodontol 2000. 1996;11:69-84.
11. Serio FG, Strassler HE. Perio-aesthetic troubleshooting: Solutions for the unexpected. J Esthet Dent. 1997;9:317-326.
About the Author
Francis G. Serio, DMD, MS, MBA
Professor and Associate Dean for Clinical Affairs
East Carolina University School of Dentistry
Greenville, North Carolina