Esthetic and Functional Provisional Restorations
When properly planned for and fabricated, provisional restorations provide the dentist, patient, and laboratory technician an accurate working concept from which to construct the final restorations.
With proper planning and execution, dentistry is able to provide very dramatic results under almost any circumstances. In many cases, these results are made even more exciting for both the patient and dentist because they can be achieved quickly and painlessly. One of the most important steps in any esthetic case is the creation of the provisional restorations. Provisionalization not only protects the prepared teeth, but allows an opportunity to work out the nuances of esthetics and occlusion before the fabrication of the final restorations. It is the fabrication of highly esthetic and functional provisionals that creates the template from which the laboratory can create beautiful porcelain. Without the knowledge gained from these provisionals, the high degree of predictability that we now enjoy would suffer dramatically.
Technique
At the Aesthetic Advantage where the author is a clinical instructor, there are two primary methods used to fabricate provisionals. Every case begins with a diagnostic wax-up made by an excellent laboratory. This wax-up reflects the initial treatment plan, and is based on preoperative models, photographs, and input from both dentists and patient. With either method, a Sil-Tec matrix (Ivoclar Vivadent) is made from the wax-up, and will be used as the template. In the first technique, the prepared teeth are spot-etched and bonded before seating the matrix, which has been filled with the temporary material, Luxatemp® (DMG). The material is allowed to set for approximately 3 minutes, and will then be locked onto the preparations. When the matrix is removed, the provisional material is left on the teeth, and the restoration is finished and polished intraorally. With the second method, the teeth are not etched or bonded, and the matrix is removed from the mouth in 1 minute with the material still inside. The material is then allowed to set, and can be finished in the operator’s hands. Once this is completed, the teeth are then spot-etched, bonding agent is placed, and the provisional is seated after flowing Luxaflow® (DMG) onto the inner aspect of the restoration. The material is then light-cured and final finishing and polishing is done.
The decision as to which method to use is determined by several factors. If there is concern as to whether or not there was sufficient reduction in the preparations, it is helpful to be able to remove the provisional before taking an impression. By visualizing the thickness of material, the dentist can judge whether or not the preparation was adequate. Another factor is the operator’s comfort level with trimming the material intraorally. A provisional involving crowns and/or onlays is much more difficult to establish accurate margins and contours in the mouth than is a provisional consisting primarily of veneers.
Case 1
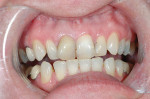
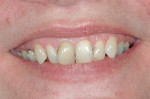
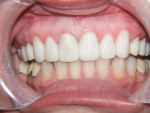
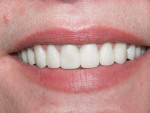
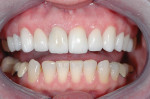
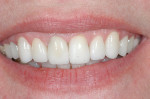
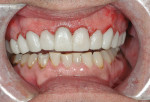
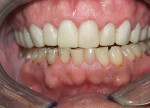
The first case demonstrates the value of a well-made provisional in determining tooth size, shape, and position. The patient was unhappy with every aspect of her smile (Figure 1 and Figure 2), and had very specific ideas as to how she wanted her appearance to change. The goal of the provisional was to make the changes, and give the patient and dentist the opportunity to evaluate them. The arch form was corrected, gingival contours were made symmetrical, incisal edge position was established, incisal embrasures were created and the edges softened, and the shade was lightened (Figure 3 and Figure 4). The patient was advised that the temporary material would appear more opaque and monochromatic than the final porcelain restorations. Both the dentist and patient were totally satisfied with the provisionals, and impressions, photographs, and careful measurements with a digital caliper were taken to ensure correct communication with the laboratory. The final restorations (Figure 5 and Figure 6) closely approximated the provisionals, and the patient was thrilled with the results.
Case 2
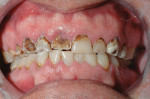
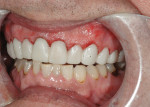
The second case is still in treatment, but shows how dramatically a well-made provisional can change a patient’s appearance and set up the case. This patient had suffered severe destruction of his maxillary teeth as a result of sucking on hard candies while attempting to stop smoking (Figure 7). He understood that a full-mouth reconstruction would be needed, but because of financial constraints, phased treatment would be necessary. In one 4-hour appointment, the upper arch was anesthetized, all decay was removed, endodontics were performed on tooth No. 6 and tooth No. 8, and posts and cores were placed on these teeth. All teeth were then prepared for full-coverage crowns and proper gingival contours were established with the extensive use of a diode laser. Provisional restorations were then fabricated using a putty matrix from the diagnostic wax-up. As seen in the photographs, a rather dramatic result was seen immediately, and the patient was stunned. Figure 8 and Figure 9 show the provisionals immediately after treatment, and the result of the soft tissue recontouring is evident. It can be seen how the vertical dimension of occlusion was recreated, and canine guidance was established. Figure 10 shows the provisionals 3 days later, with excellent soft tissue healing present, and the patient with a happy, healthy smile. This provisional was created in three units so that the final restorations could be completed in sections if the patient’s finances allow.
Conclusion
As can be seen in the above cases, the provisional restoration is an essential aspect of the esthetic and functional case. Properly planned out and fabricated, it provides the dentist, patient, and laboratory technician an accurate working concept from which to construct the final restorations. It behooves the restorative dentist to take as much time and effort as possible to ensure that all components of a successful case are first created in the provisionals.
Acknowledgment
The author would like to thank all of the instructors at the Aesthetic Advantage for their guidance and wisdom, and especially Dr. Larry Rosenthal for his contributions to the field of esthetic dentistry.
About the Author
Marc Schlenoff, DDS
Attending Physician
Morristown Memorial Hospital
Morristown, New Jersey
Clinical Instructor
Aesthetic Advantage
New York, New York
Private Practice
McAfee, New Jersey