Immediate Dentin Sealing (IDS)
Optimizing adhesive performance for indirect restoratives.
Protecting the pulp is of utmost concern to the restorative dentist. Esthetic and restorative excellence can take a back seat to sensitivity for any patient. Understanding the biology of sensitivity has led clinicians to look for progressive protocols that improve clinical outcomes and prevent patients’ sensitivity and pain.
Immediate dentin sealing (IDS) is the application of a dentin bonding agent to freshly cut dentin when it is exposed during tooth preparation for indirect restorations (inlays/onlays, crowns). IDS is a progressive protocol designed to address the challenges of preparation, temporization, and final cementation of indirect restorative procedures, and offers several distinct advantages.
Biological Advantages
Effectively sealing dentin and bonding to enamel is at the core of clinical success. A clean dentin surface is mandatory for optimal seal and adhesion. Freshly cut dentin is uncontaminated and clean, thus more easily capable of resin infiltration. Immediately sealing dentin protects it from contamination from bacterial leakage or remnants of temporary cements.1,2
Creating a hybrid layer that both mimics the dentino-enamel junction (DEJ) and promotes proper adaptation and adherence of the final restoration is the basis of minimal intervention dentistry. Creating a hybrid layer by precuring a dentin bonding agent before impression taking provides a significant thickness to reduce the collagen collapse that may occur during the impression taking and cementation process.3-8 Allowing the hybrid layer to mature while temporized, void of the shrinkage stresses and strain from cement polymerization, helps to create a stress-free dentin bond development.9,10
Additionally, effective sealing of dentin addresses the challenges of hydrodynamic water movement in dentinal tubules which has been shown to induce sensitivity.11 Using a layer of low-viscosity resin (liner) may help to protect the underlying hybrid layer, and will better preserve the dentin seal.12 Alternatively, a filled resin liner (low-elastic modulus liner) has also been shown to facilitate the clinical and technical aspects of IDS.13
Clinical Advantages
Patient comfort with reduced postoperative sensitivity is a compelling clinical advantage. Water movement within cut tubules is the most widely accepted physiological mechanism leading to sensitivity (hydrodynamic theory).14 Effective sealing of dentin with low-viscosity polymerizable adhesive resins results in physical obturation of cut tubules.15 The authors report sealing dentin immediately after preparation has resulted in significantly less interim sensitivity by patients and, in many cases, limits the need for anesthesia at cementation.
Creating the hybrid layer before impression taking eliminates the concern about the thickness of the adhesive layer affecting the fit of the final restoration.16 Capturing the hybrid layer into the impression will eliminate the concern for gap formation and ill-fitting restorations. Upon final cementation, a single layer of bonding agent is placed and light-cured in conjunction with the resin cement, eliminating film thickness as a concern.17-19
IDS allows the clinician to address the importance of dentin sealing and desensitization during the preparation appointment, and establish a durable bond to enamel at the cementation appointment. Standardizing these protocols will lead to optimized clinical outcomes. IDS does not compromise bonding16 and helps to optimize dentin bonding in indirect restorations.13
Case Presentation
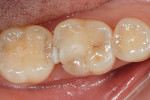
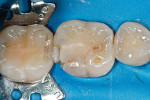
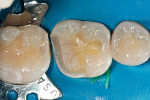
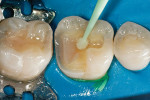
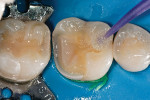
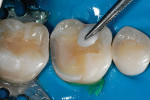
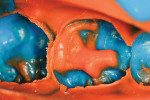
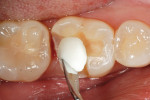
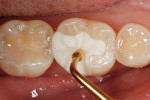
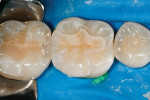
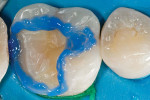
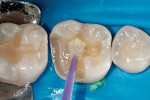
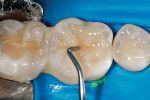
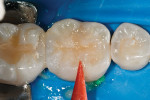
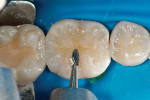
The defective restoration on the first lower molar was removed and a rubber dam was placed (Figure 1 and Figure 2) prior to preparation for an indirect onlay restoration. After removal of the restoration and decay, the dentin was built up and undercuts were eliminated using a self-etch adhesive (All-Bond SE, Bisco, https://www.bisco.com) followed by a flowable composite (Aelite Flow A3, Bisco). The tooth was then prepared for an indirect onlay restoration (Figure 3). The dentin was conditioned using All Bond SE (A and B mixed)for 20 seconds with a gentle scrubbing motion (Figure 4). Excess solvent was evaporated using an air syringe, leaving the preparation visibly shiny. The preparation was then light-cured for 20 seconds.
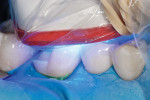
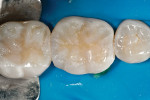
All-Bond 3 Resin (filled) was applied to the preparation and light-cured for 10 seconds. It is postulated that a layer of low-viscosity resin (liner) may help to protect the underlying hybrid layer and would be better to preserve the dentin seal12 (Figure 5 and Figure 6). The enamel of the preparation was redefined and margins were re-beveled. The oxygen-inhibited layer was removed with an alcohol swab, leaving the preparation with a visible matte finish (Figure 7). The final impression was taken with a PVS impression material (Figure 8).
After the impression was taken, one to two coats of Pro-V Coat (a hydro-gel separating agent, Bisco) were applied to the entire preparation and air-dried for 10 to 15 seconds. The water-soluble Pro-V Coat allows a clinician to utilize the benefits of IDS without the risk of the provisional material bonding to the tooth structure. It also serves to protect the dentin surface from contamination and is designed to clean up easily without any residue.
A temporary restoration was created using Bisco’s Pro-V Fill, a packable composite for use in onlay restorations (Figure 9). Pro-V Fill has excellent handling and sculpting properties offering matrix-free modeling directly in the mouth (Figure 10). One coat of Biscover LV, a low-viscosity, light-cured resin liquid polish (Bisco), was applied and light-cured for 30 seconds.
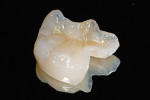
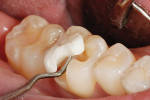
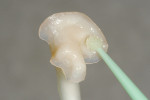
The patient returned for the cementation of the final Tescera indirect composite restoration (Bisco) (Figure 11). The provisional was removed using a sharp instrument (Figure 12). The preparation was cleaned using a slurry of pumice, and the restoration was tried in for proper fit. Note the distal contact was initially too tight and required adjustment (Figure 13). Next, the enamel of the preparation was etched with 32% Uni-Etch with BAC (Bisco) for 15 seconds, rinsed, and dried (Figure 14). Equal parts of All-Bond 3 (A & B mixed) were applied to the entire preparation, air-dried, and light-cured (Figure 15). The internal surface of the onlay restoration was cleaned and prepared with one to two coats of All-Bond 3 (A & B mixed) and thoroughly air-dried and light-cured (Figure 16). The restoration was seated using Bisco’s Duo-Link dual-cured resin cement (Figure 17). Excess material was immediately removed with a rubber tip and the margin was light-cured for 3 seconds to a gel state (Figure 18). The margins and interproximal areas were cleaned and the entire restoration was light-cured for 60 seconds. Adjustments were made to the occlusal surface initially with an egg-shaped carbide bur on high dry (Figure 19). Before final polishing, the lower right second molar was restored with an occlusal composite using Aelite enamel A1 (Bisco) (Figure 20). Both restorations were then finished sequentially and polished (Figure 21).
Disclosure
Dr. Morgan has received honorarium from Bisco Inc.
References
1. Cagidiaco MC, Ferrari M, Garberoglio R, Davidson CL. Dentin contamination protection after mechanical preparation for veneering. Am J Dent. 1996;9(2):57-60.
2.Pashley EL, Comer RW, Simpson MD, et al. Dentin permeability: sealing the dentin in crown preparations. Oper Dent. 1992;17(1):13-20.
3.Dietschi D, Herzfeld D. In vitro evaluation of marginal and internal adaptation of class II resin composite restorations after thermal and occlusal stressing. Eur J Oral Sci. 1998;106(6):1033-1042.
4.Dietschi D, Magne P, Holz J. Bonded to tooth ceramic restorations: in vitro evaluation of the efficiency and failure mode of two modern adhesives. Schweiz Monatsschr Zahnmed. 1995;105(3):299-305.
5.Frankenberger R, Sindel J Krämer N, Petschelt A. Dentin bond strength and marginal adaptation: direct composite resins vs ceramic inlays. Oper Dent. 1999;24(3):147-155.
6.Magne P, Douglas WH. Porcelain veneers: dentin bonding optimization and biomimetic recovery of the crown. Int J Prosthodont. 1999;12(2):111-121.
7.McCabe JF, Rusby S. Dentine bonding—the effect of pre-curing the bonding resin. Br Dent J. 1994;176(9):333-336.
8.Tay FR, Gwinnett AJ, Pang KM, Wei SH. Variability in microleakage observed in a total-etch wet-bonding technique under different handling conditions. J Dent Res. 1995;74(5):1168-1178.
9.Dietschi D, Monasevic M, Krejci I, Davidson C. Marginal and internal adaptation of class II restorations after immediate or delayed composite placement. J Dent. 2002;30(5-6):259-269.
10.Reis A, Rocha de Oliveira Carrilho M, Schroeder M, et al. The influence of storage time and cutting speed on microtensile bond strength. J Adhes Dent. 2004;6(1):7-11.
11. Drisko CL, et al. Dentin Hypersensitivity: Consensus-Based Recommendations for the Diagnosis and Management of Dentin Hypersensitivity. Inside Dentistry. 2008;4(9 Special Issue).
12.Duarte RM, de Goes MF, Montes MA. Effect of time on tensile bond strength of resin cement bonded to dentine and low-viscosity composite. J Dent. 2006;34(1):52-61.
13. Magne P. Immediate dentin sealing: a fundamental procedure for indirect bonded restorations. J Esthet Restor Dent. 2005;17(3):144-155.
14. Brannstrom M. Sensitivity of dentine. Oral Surg Oral Med Oral Pathol. 1966;21(4):517-526.
15. Trowbridge HO, Silver DR. A review of current approaches to in-office management of tooth hypersensitivity. Dent Clin North Am. 1990;34(3):561-581.
16.Magne P, Kim TH, Cascione D, Donovan TE. Immediate dentin sealing improves bond strength of indirect restorations. J Prosthet Dent. 2005;94(6):511-519.
17.Paul SJ, Scharer P. Factors in dentin bonding. Part II: A review of the morphology and physiology of human dentin. J Esthet Dent. 1993;5(2):51-54.
16.Paul SJ, Scharer P. Intrapulpal pressure and thermal cycling: effect on shear bond strength of eleven modern dentin bonding agents. J Esthet Dent. 1993;5(4):179-185.
17.Stavridakis MM, Krejci I, Magne P. Immediate dentin sealing of onlay preparations: thickness of pre-cured Dentin Bonding Agent and effect of surface cleaning. Oper Dent. 2005;30(6):747-757.
About the Authors
Michael J. Morgan, DDS
Private Practice
Hinsdale, Illinois
Douglas J. Brown, DDS
Senior Manager, Clinical Affairs
BISCO Inc
Schaumburg, Illinois
Byoung In Suh, PhD
President
BISCO Inc
Schaumburg, Illinois