Complete Marginal Seating of Indirect Restorations
A consistent clinical procedure for seating indirect restorations with ideal proximal contacts.
Traditionally, adjustments of proximal contacts of indirect restorations are performed by the clinician holding the restoration between their fingers, using an indicating medium such as very thin articulating paper or colored pencils, and reducing the contact with a rotary instrument. Small restorations such as inlays or onlays are not only difficult to hold but they are also difficult to see and frequently get twisted into the folds of the glove material or end up on the floor somewhere. In addition, incremental adjustments with this method require multiple trials of placing the restoration in and out of the preparation which can be quite difficult, tedious, and time-consuming for the clinician as well as uncomfortable for the patient.
There is very little information given in the dental school curriculum about adjusting tight proximal contacts. In fact, very little is written in the literature about this subject. It has been empirical to do proximal contact adjustment of indirect restorations (crowns, veneers, inlays, and onlays) clinically.
Dorfer et al1 concluded that proximal contact is a manifestation of location, tooth type, chewing, and time of day. Newell et al2 found that although food impaction is generally associated with open contacts, food impaction also can occur in interproximal sites when contacts are tight. Kim et al3 described proper proximal contact as microscopic clearance or passive contact to relieve pressure between the proximal contact surfaces of indirect restorations and adjacent teeth and the relief of pressure was referred to as interproximal relief (IR). By properly restoring interproximal relief, food impaction is prevented, complete marginal seating of indirect restorations is achieved, and occlusal interferences are prevented.
Here, the authors are presenting a consistent clinical procedure for seating indirect restorations with ideal proximal contacts. Determining and adjusting the proximal contact strength of indirect restorations will be achieved using ultra-thin abrasive diamond dental strips coordinated from evaluation and adjustment of proximal contacts to definitive cementation in the patient’s mouth.
Case Report
A 33-year-old woman presented with an old amalgam restoration with recurrent decay on tooth No. 3. The recommended treatment was an all-ceramic CAD/CAM inlay restoration (Vitablocs, VITA, https://www.vitablocs.com). The patient consented to the treatment.
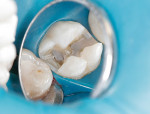
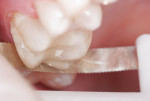
The old amalgam and dental decay were removed and a mesial-occlusal-distal inlay preparation was prepared (Figure 1). Disclosing solution was applied to the preparation to determine if any decay remained. A primer and bond (Touch & Bond, Parkell, www.parkell.com) was applied to the preparation and light-cured before the optical impression. An optical impression was taken of the preparation and a ceramic inlay (CEREC®, Sirona Dental Systems, https://www.sirona.com) was designed and fabricated. The sprue and elevated surround on the inlay body was removed. The inlay was then placed into the preparation. The inlay did not seat completely because of excessive heavy mesial and distal proximal contacts.
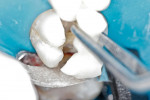
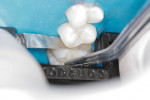
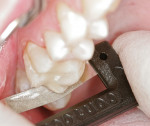
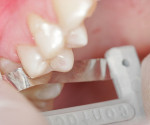
An ultra-thin abrasive diamond dental strip (ContacEZ® Diamond Dental Strip, ContacEZ,https://www.contacez.com) was inserted into the distal interproximal space, abrasive side facing the cavity preparation. The inlay was then placed into the preparation (Figure 2). The strip was passed with a horizontal motion two to three times (Figure 3). The procedure was repeated on the mesial interproximal contact area. The distal proximal contact was tighter against the strip than the mesial proximal contact, indicating that the distal proximal contact was heavier and needed further adjustment with the strip.
The inlay restoration was passively placed into the preparation and held in place with light pressure. The diamond dental strip was passed with a horizontal motion five to six times. The strip was then moved to the mesial interproximal area and the same motion was repeated. This protocol was repeated distally and mesially until the proximal contacts felt light pressure and equal on both sides when the strip was in place (Figure 3). The restoration was now able to be fully seated with appropriate proximal contact pressure.
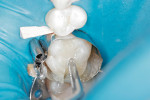
While the restoration was etched and primed (Touch & Bond), a matrix band (Automatrix, DENTSPLY Caulk, https://www.caulk.com) and wooden wedges were placed around the tooth. The cavity preparation was cleaned with etchant and water, and the primer and bonding agent were applied. An auto-mixed, dual-cure resin cement (DUO-LINK Composite Luting Cement, BISCO, https://www.bisco.com) was mixed and placed into the preparation and the restoration was seated into the preparation (Figure 3). The restoration was light-cured from the occlusal surface for 20 seconds. The matrix band was removed and the excess resin cement was removed gently with a composite knife. The restoration was light-cured from the buccal and lingual surfaces, and then the mesial and distal interproximal spaces, each for 20 seconds. The restoration was reshaped and refined using stones and flame-shaped, small, fine-diamond points. The rubber dam was removed and the occlusion was checked with articulating paper. The occlusion was adjusted using a fine round diamond point and a rubber point. The interproximal spaces were cleaned using an ultra-thin serrated dental strip (ContacEZ Serrated Dental Strip) (Figure 5). The diamond dental strip was placed at a 45° angle and the proximal contour of the tooth was further refined (Figure 6). The proximal surfaces were polished with an ultra-fine abrasive diamond strip (ContacEZ Final Polishing Strip) and interproximal relief was confirmed (Figure 7) ensuring ideal proximal contacts. The entire occlusal surface and all proximal surfaces of the tooth were then etched, glazed, and light-cured.
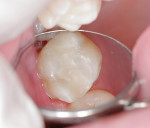
The serrated dental strip was then placed interproximally to remove any retained excess resin cement or to break any bonding between the restoration and adjacent teeth. A waxed dental floss was passed interproximally to clean and confirm the ideal proximal contact pressure. The dental floss snapped in and out of the interproximal space firmly. The finished restoration was polished with a polishing brush. The tooth and restoration were polished using a rubber cup with paste. The finished inlay restoration shows the smooth transition from the tooth surface on proximal contours and complete marginal seating (Figure 8).
Conclusion
When clinicians get their restorations from the milling machines, they need to determine which side has heavier proximal contact. Using an ultra-thin diamond dental strip (0.04 mm to 0.06 mm), the heavier contact side is easily detected and reduced. Using this ultra-thin diamond dental strip method prevents clinicians from opening the wrong proximal contacts mistakenly, but ensuring ideal proximal contact each and every time consistently, which ultimately results in enhanced patient comfort and functionality immediately after definitive cementation.
Disclosure
Neither Dr. Kim nor Dr. Rothchild have any financial interest in or received compensation from any company for the writing of this article.
References
1. Dörfer CE, von Bethlenfalvy ER, Staehle HJ, Pioch T. Factors influencing proximal dental contact strengths. Eur J Oral Sci. 2000;108(5):368-377.
2. Newell DH, John V, Kim SJ. A technique of occlusal adjustment for food impaction in the presence of tight proximal contacts. Oper Dent. 2002;27(1):95-100.
3. Kim DS, Suh KW. A proximal contact adjustment and interproximal relief method. J Prosthet Dent. 2007;97(4):244-245.
About the Authors
Daniel S. Kim, DDS
Private Practice
Vancouver, Washington
John A. Rothchild, DDS
Private Practice
Chicago, Illinois and Durango, Colorado
Assistant Professor of Surgery
Rush University Medical School
Chicago, Illinois
Associate Professor of Dental Medicine Emeritus
Capital University of Integrative Medicine
Washington, DC