EDS Flexi-Post® Fiber
Increasing the success rate for fiber posts.
Allan Deutsch, DMD
Glass-reinforced fiber posts have been in clinical use for over 10 years and the failure rate can be high. However, since the clinical failure does not include tooth fracture, many dentists feel that placing a post will just make it easier to bond everything together and perhaps reinforce the restoration. This is not a preferred philosophy of treatment because when the post fails, so does the restoration. In some cases the restoration can be many units long and quite extensive, leading to both patient dissatisfaction and dentist anxiety.
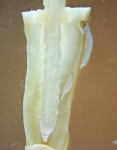
Retention of a fiber post in the root can be dramatically increased with the use of active retention of fiber threads in the root and an anatomical design of the post, which includes two or three tiers, depending on the post type. The threading of the root is achieved using a non-stress-causing, split-shank technology tap. The tap is a specially designed split-shank post machined with a wrench handle (Figure 1). The split of the tap creates the thread line for the fiber posts in the root in an atraumatic fashion, acts as a stress breaker, and lets the legs of the tap collapse as they thread into the root. This creates the thread line in a gradual and low-stress environment, allowing the apical threads to penetrate the least into the dentin and the coronal threads to penetrate the deepest into the dentin. The fiber threads of the post create an extremely retentive (mechanical retention) fiber post restoration. Figure 2 and Figure 3 show the fiber threads embedded in the dentin. Note the thread line is sharp, with no microfractures radiating from the thread line. The fiber post is slightly conical in shape near the apical end to allow the threads to fit into the graduated thread line created by the split-shank tap.
The posts can be cemented in place by etching the walls of the post hole with EDS’ 17% EDTA in water and then using EDS’ self-curing titanium reinforced Flexi-Flow Auto composite cement to lute the post in place. The 17% EDTA removes the smear layer and opens the dentinal tubules while it also etches the intertubular and intratubular dentin. This etching creates fingers in the dentin (a hybrid layer) that facilitates composite bonding. Flexi-Flow cement is self-curing, so it fully cures even at the bottom of the post hole. The combination of etching the dentin using 17% EDTA and Flexi-Flow composite cement provides such high retention that additional bonding with a bonding agent within the canal is not required.
Clinical Technique
Once post-hole preparation is complete, the dentin is conditioned with a 17% aqueous solution of EDTA for 1 minute. While the canal is still wet with EDTA it is threaded with the appropriate split shank tap. The fiber post is then placed on the wrench and trial seated in the canal to ensure proper fit. If the second tier or flange does not fit completely within its preparation, then the post is too long and must be cut at the apical end. Each thread line is approximately 1 mm wide and can be used as a guide when shortening the fiber post. The canal is dried and Flexi-Flow Auto cement is placed down the canal using the micro tip. Next, thread the post into the canal until fully seated. The working time for the cement is approximately 3.5 minutes. Build up the core by first applying bonding agent to the coronal dentin and then placing the core material onto the post and coronal dentin.
The posts are made from a specially formulated uni-directional S-glass to increase their strength under function. They also retain a modulus of elasticity close to that of natural dentin. The modulus is slightly higher than other fiber posts to approach the stiffness of the much larger diameter of the root dentin. All fiber posts are tooth-colored for esthetic restorations. The split-shanked fiber posts are designed to take maximum advantage of all the design and functional features that have been brought to light through research to improve clinical success.
This article was written by Allan Deutsch, DMD.
For more information, contact:
EDS
Phone: 800-22-FLEXI
Web: https://www.edsdental.com
Disclaimer
The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dentistry. The preceding is not a warranty, endorsement, or approval for the aforementioned products or services or their effectiveness, quality, or safety on the part of Inside Dentistry or AEGIS Communications. The publisher disclaims responsibility for any injury to persons or property resulting from any ideas or products referred to in the preceding material.