The Injection-Molded Technique for Strong, Esthetic Class II Restorations
The traditional technique for preparing and filling Class II restorations ultimately leads to higher failure rates.
David J. Clark, DDS
Class II restorations present several challenges to the clinician. The traditional technique for preparing and filling these restorations leaves them prone to leaking, chipping, wholesale fracture, recurrent decay, and ultimately, higher failure rates when compared to amalgam.1-3The classic cavity preparation designs first created by G.V. Black represented a significant advance during his day; however, that day was in the 19th century. We are now seeing evidence that these shapes can weaken the dentition by contributing to tooth fracturing, in spite of the belief that composites will always strengthen the tooth. Furthermore, the practice of applying several separately cured layers of composite in a deep and boxy preparation creates risks for voids, gaps, and seaming between layers. Residual stress can build in the tooth and restoration as the composite is layered and, in spite of careful layering, the composite often shrinks as the stress builds to eventually create marginal gapping or enamel microfracturing.
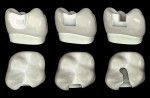
To counter the problems often associated with Class II composite restorations, the author has developed a technique for injection-molded composite dentistry, which reduces the potential for voids and fault lines while maintaining the structural integrity of the tooth. This technique involves the use of a redesigned cavity preparation, a translucent matrix system, and the proper combination of paste and flowable composites to create strong and esthetic restorations. The self-called “Clark Class II” is an evolved version of previous modifications of the original G.V. Black preparation, such as the slot preparation (Figure 1).
Evidence shows that the incorporation of flowable composites is now becoming increasingly common, with one survey finding that more than 90% of dentists reported using them in the past year.4 This popularity, though, comes without any clear consensus on the specific usages, techniques, and percentages of flowable composite that should be employed in Class II restorations. Additionally, the available research does not necessarily support the use of flowable composite, with no proof of improvement in internal adaptation or a difference in restorative performance.3,5,6 However, by the end of this article, the reader will be confident in a disciplined use of flowable composite in a manner that has been shown in the research to provide a superior outcome.
Modified Preparations
The configuration of the cavity plays an important role in the durability of the restoration. The traditional boxy shape of a Class II preparation creates sharp internal line angles, promotes crack initiation,7 and leaves dentin vulnerable to fracture. Moreover, this shape of preparation makes the restoration prone to unfavorable composite shrinkage, as the composite shrinks away from opposing walls of the preparation and creates gapping and/or stress. An additional consideration is that the G.V. Black, or slot, preparation maximizes bondable dentin surfaces while minimizing the bondable enamel surface area.
However, with a redesigned preparation that is flat and shallow, the typical C-factor problems are eliminated or mitigated. A saucer-shaped preparation with feather edges avoids the sharp angles of the traditional preparation, and also allows the composite to act in a new way on the tooth—sitting on the tooth instead of in it. With this shallower preparation, the composite can be injected in one phase instead of increments, which saves time and, more importantly, eliminates the risk of gapping between layers.
Translucent Matrix System
Injection-molded composite dentistry requires the use of a new kind of matrix system, which uses translucent matrices (Bioclear; https://www.bioclearmatrix.com). These matrices make it possible to perform buccal lingual curing, and also facilitate single-load filling. While traditional metal matrices allow curing only from the occlusal surface, a translucent matrix allows the composite to be cured from both buccal and lingual angles. The two sides can be cured simultaneously with two lights, and even a 7-mm preparation can be cured in a single load.
Balanced Use of Paste and Flowable Composites
With a minimally invasive cavity shape, the resultant space is difficult to fill strictly with paste composite. The preparation in this technique is shaped like a saucer instead of a hole, and because paste composite is so heavy, it does not easily flow into deep areas. To address this issue, practitioners often make the mistake of relying too heavily on flowable composites, which have inherent weaknesses. First, flowable composites are more prone to shrinkage than are paste composites. Additionally, flowables are typically not as strong as pastes, and flowable composite near the occlusal surface is more prone to wear than paste composite. However, flowable composites can be extremely useful when applied in moderation. By marrying flowable composite with paste, the practitioner is able to mitigate the shortcomings of flowable while maximizing its superior handling characteristics.
Recently, the Professional Products Review from the ADA presented a comprehensive review of the science of and the clinical application for flowable composites.7 The publication featured a panel of experts weighing in on their opinion of flowable composites, and many questioned the use of flowable as a liner beneath Class II restorations. When used as a liner, the flowable composite is placed and cured separately. However, other researchers describe a different method, referred to as the “snowplow technique,” in which the flowable is placed first and not cured separately, followed with a paste composite injected into the flowable, which is then “squeegeed” out of the sides of the restoration. These researchers have found that this technique can improve adaptation and also lessen the chance of marginal leakage, versus separate layers of flowable.8,9
The Injection-Molded Technique
Before beginning the technique, if a significant amount of dentin is present, that dentin is either covered with glass ionomer or dentin bonding agents. The injection-molded composite dentistry technique (Table 1) calls for first applying a bonding resin to both the previously treated dentin and freshly etched enamel inside the matrix, then injecting a flowable composite into the pool of bonding resin, and then finally injecting the paste composite. The resin-flowable-paste mass is polymerized together in a single light-cure. In the author’s technique, he aims for the paste composite to make up 80% to 90% of the overall volume of the filling, while flowable should account for 10% to 20%. With traditionally boxy preparations, it is common to see restorations with 50% to 70% of the overall volume made up by flowable composite. That amount (greater than 25%) of flowable can be a liability for the dentist and patient, as our studies have shown that these volumes can contribute to unacceptably high rates of marginal ridge fracture and complete filling dislodgement.
Properties of Paste and Flowable Composite
Choosing the appropriate composite is another important component of this technique. 3M ESPE (https://www.3mespe.com) has developed both a paste, Filtek™ Supreme Plus Universal Restorative, and a flowable composite, Filtek™ Supreme Plus Flowable Restorative, that lend themselves well to this technique. The Filtek line of composites has a unique formulation of lightly sintered zirconia particles. It has the polishability of a microfill and the strength of a microhybrid, which discourages marginal ditching and loss of surface luster. Also, 3M ESPE designed both the flowable and the universal with the same color targets, which helps to ensure an esthetic blend of flowable and universal in this technique.
Many composites are still indicated for only anterior or posterior use, and force a choice to be made between strength and esthetics. However, Filtek Supreme Plus can be used for both anterior and posterior indications with full confidence. Its chemistry allows it to be used universally, further adding to the simplification achieved with injection-molded composite dentistry.
Case Presentation
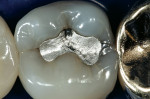
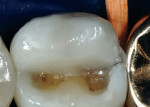
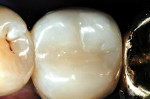
The featured case will serve as an introduction to injection-molded composite dentistry. The patient, a 42-year-old woman, presented with recurrent decay beneath a failing occlusal amalgam on tooth No. 29. There also was an early incomplete fracture crossing the distal marginal ridge, and some secondary caries in the dentin near the crack (Figure 2). The two treatment options discussed were a porcelain onlay, or a direct distal-occlusal-buccal-lingual composite restoration. The patient opted for the composite treatment as it was less invasive, less costly, and more expedient.
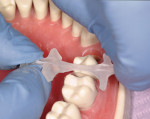
To begin the treatment, a “pre-wedge” was placed between teeth Nos. 28, 29, and 30. The purpose for the pre-wedge is to gently separate the teeth, compress the papilla, and to protect the rubber dam. It is a simple but vital step for bonded restorations. The pre-wedge technique should be used for every Class II injection-molded restoration.
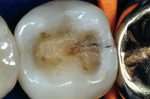
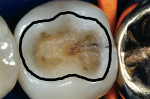
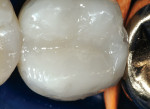
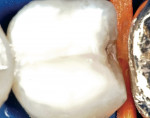
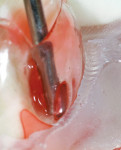
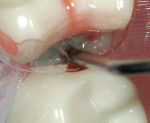
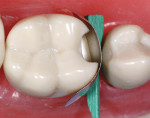
To simplify the procedure and to control shrinkage and C-factor problems, the occlusal portion was restored first (Figure 3 and Figure 4). The lingual half of the tooth was restored with strictly paste composite (Figure 5). The buccal cusp was then restored with paste to finish covering the entire occlusal surface (Figure 6). To mitigate shrinkage, composite was first applied to the lingual cusps, and the buccal cusp incline was built subsequently. After completion of the occlusal portion of the composite, the author moved on to treatment of the fracture across the distal marginal ridge and the caries associated with the crack.
Following those steps, a brand new original Fissurotomy® bur (SS White; https://www.sswhiteburs.com) was used to prepare the interproximal portion of the tooth. To “chase” the fracture, the smaller Fissurotomy NTF bur was used. Note the final saucer shape of the preparation with feather-edge or infinity-edge margins (Figure 7). The final infinity edge of the interproximal was prepared with a fine diamond. As a final step, the pre-wedges were removed, and the external areas near the margins were cleansed and abraded with a lightning strip.
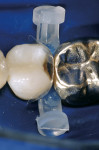
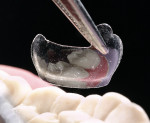
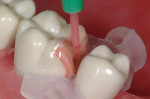
The injection molding step is the final portion of the procedure. The proper Bioclear matrix and Interproximator were selected and placed (Figure 8). A 37% phosphoric acid was placed for 20 seconds interproximally and on the freshly cut composite, then rinsed and dried. Two coats of Adper™ Single Bond Plus Adhesive (3M ESPE) were applied to the dentin with a microapplicator, air-thinned, and individually light-cured. Once the dentin was covered with two coats of bonding resin, the area was ready for injection molding. (Before the advent of the IMC technique, enamel areas needed to be bonded and light-cured before flowables or pastes were applied. The injection-molding technique, however, streamlines these steps: once the dentin is covered, there is no need to cure the bonding resin separately. The pool of bonding resin allows the composite to flow seamlessly into the delicate areas of the matrix.)
The flowable composite was injected into the pool of bonding resin, filling the matrix to approximately one third full. After injection of the flowable composite, the paste was injected, which acted to drive out the bulk of the bonding resin and flowable composite. The materials were displaced laterally as the paste was injected at the mid-interproximal. Pressure was maintained on the syringe as the injection was finished to avoid the paste pulling out of the interproximal area as the syringe was withdrawn. The syringe was swiped against the occlusal on removal to avoid pullback. The excess composite was quickly removed with an explorer and burnisher, and the marginal ridge was rounded. Using a high intensity (5-second) curing light, the composite was cured for 10 seconds with dual lights on both buccal and lingual sides, then cured for 10 seconds on the occlusal portion, and 10 seconds again with dual lights from both buccal and lingual sides. The matrix was removed, and the Interproximator was cut and removed laterally. Pre-polishing was done with coarse pumice and a rubber cup, and final shaping and polishing was performed with a combination of Sof-Lex™ Extra Thin Finishing and Polishing Discs (3M ESPE) and carbide burs on the occlusal surface. The final polish was achieved with new Jazz Supreme Polisher by SS White.
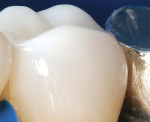
After the procedure was completed, the patient, who was able to watch the entire procedure broadcast on chairside TV, was ecstatic and commented that the restoration looked more natural than some of her existing porcelain crowns (Figure 9 and Figure 10).
Discussion
The concept of injection-molded composite dentistry can be compared to impressioning, in which the low-viscosity, light-body material is syringed into subgingival areas, and then followed and partially displaced by a heavier, high-viscosity impression material that has appropriate physical characteristics. In this technique, successively higher-viscosity materials are applied in sequence, and the bonding resin and flowable composite act as wetting agents, which are subsequently displaced by the heavier paste-composite material.
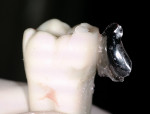
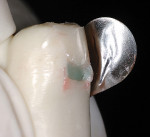
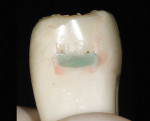
To demonstrate the stark contrast between traditional incremental loading with a metal matrix and the injection-molding process, the author restored two ivorine teeth (Figure 11, Figure 12, Figure 13, Figure 14, Figure 15, Figure 16, Figure 17, Figure 18, Figure 19, Figure 20, Figure 21, Figure 22, Figure 23 and Figure 24). It is very interesting to note that for the injection-molding technique, the author purposely placed excessive bonding agent (dyed orange) and excess flowable composite (dyed green), and yet the final view demonstrates how effectively the paste composite displaces nearly all of the lesser-filled resins. The best way to describe the technique is to compare it to seating a porcelain onlay, where the bonding resin is not cured separately and the resin cement is squeezed laterally, the excess cement cleared away, then the complex (porcelain, resin cement, bonding resin) is cured all at once. In the traditional preparation, four problems are evident (Figure 21). First, the excessive flowable composite (green) has significantly more polymerization shrinkage than the paste, and less strength. Second, there is a seam between the flowable and the paste. Third, the finish is not as smooth as the injection-molded method because metal matrices have a much rougher surface than does the Mylar surface. Fourth, air-thinning the resin drives it past the margins, leaving a gingival margin that is not light-cured, and is prone to dissolution and an eventual void.
The patient’s case presents a common dilemma, in which a conservative occlusal amalgam has been in place for decades and is accompanied by significant incomplete fracturing. Placing a traditional intracoronal restoration has not been shown to predictably protect the tooth from further fracturing. A porcelain onlay or crown treatment has been shown to protect against fracturing, but for this particular case, that amount of tooth reduction would have mutilated an essentially intact tooth.
The modified preparation in this particular instance provided several benefits. First, it created a favorable C-factor to allow injection molding. Second, the interproximal saucer preparation allowed the composite to engage a significantly higher portion of the overall interproximal enamel, which further enabled the composite to splint the tooth. Thus, the unique preparation allows the composite to act as a splint without having to resort to a crown or onlay. If the old preparation model had been followed and the filling was placed in the tooth, there would not have been sufficient enamel to splint the tooth. By redesigning both the occlusal and interproximal preparations, the tooth has been essentially swept around and a significant portion has been covered with composite. In essence, the restoration becomes a composite onlay without having to “shoe” the cusps.
Additionally, the combination of a “calla lily”-shaped occlusal preparation and a flaring Clark Class II interproximal cavity preparation extends the preparation to cuspal areas, allowing for significant coverage of the occlusal surface. This will give the clinician confidence that the tooth will be protected from further fracturing. These “infinity-edge” or feather-edge margin preparations on the occlusal surface of posterior teeth were studied in over 100 teeth followed at 5 to 7 years. The teeth were studied with SEM and clinical evaluation. The Filtek Supreme Plus Universal Restorative samples demonstrated wearing patterns that were similar to surrounding enamel.
This data gives us confidence in treatments where the composite is used to cover significant portions of posterior teeth. Our current perceptions of the inadequacies of composite when compared with porcelain may be unfounded. The author’s own observation using constant microscope visualization for treatment and follow-up is that the true problems of composite are in inappropriate cavity designs and archaic filling protocols and matrices, and not the physical properties of the top-performing composites.
The paste composites can have such an outstanding ability to withstand wear, and studies have shown that a feather-edge margin on the posterior has ideal resistance to both wear and fracture. This technique gives the practitioner confidence in performing a procedure that is both minimally invasive and maximally esthetic, and could potentially service the patient for decades.
Disclosure
Dr. Clark developed the Bioclear system and continues to receive financial compensation for the product. He has a majority interest in the company. Injection-molding technique is patent pending.
References
1. Van Nieuwenhuysen JP, D’Hoore W, Carvalho J, Qvist V. Long-term evaluation of extensive restorations in permanent teeth. J Dent. 2003;31:395-405.
2. Sjogren P, Halling A. Survival time of class II molar restorations in relation to patient and dental health insurance costs for treatment. Swed Dent J. 2002;26:59-66.
3. Mjor IA, Dahl JE, Moorhead JE. Placement and replacement of restorations in primary teeth. Acta Odontol Scand. 2002;60:25-28.
4. Flowable Composites. ADA Professional Product Review. Spring 2009. Volume 4. Issue 2.
5. Lindberg A, van Dijken JW, Horstedt P. In vivo interfacial adaptation of class II resin composite restorations with and without a flowable resin composite liner. Clin Oral Investig. 2005;9(2):77-83.
6. Ernst CP, Canbek K, Aksogan K, Willershausen B. Two-year clinical performance of a packable posterior composite with and without a flowable composite liner. Clin Oral Investig. 2003;7(3):129-134.
7. Clark DJ, Sheets CG, Paquette JM. Definitive diagnosis of early enamel and dentinal cracks based on microscopic evaluation. J Esthet Rest Dent. 2003;15(Special Issue):7:391-401.
8. Hilton TJ, Quinn R. Marginal leakage of Class 2 composite/flowable restorations with varied cure technique. J Dent Res. 2001;80(Special Issue):Abstract No. 0502.
9. Opdam NJ, Roetersi JJ, Deboeri T, et al. Voids inside restored micropreparations using various resin composites and application techniques. J Dent Res. 2002;81 (Special Issue A):Abstract No. 3132.
About the Author
David J. Clark, DDS
Founder
Academy of Microscope Enhanced Dentistry
Fort Wayne, Indiana
Course Director
Newport Coast Oral Facial Institute
Newport Beach, California
drclark@bioclearmatrix.com