Simplified Protocol for a Failed Zirconia Restoration
Careful removal and replacement of failed restorations is a critical aspect of successful treatment.
Andrew Shannon, DDS
Like all things modern, esthetic dentistry evolves to remain in step with the times. Methods, materials, and expectations each play a part in that evolution, changing over time to improve the practice of dentistry. One dramatic change seen over the last several years has been in restorative materials, which now provide more esthetic options than ever before.
Patients and practitioners expect esthetic and functional success from the restorative materials available today. To ensure long-term function of esthetic restorations, clinicians must continue alert watchfulness during restorative preparation, including the careful removal of obsolete or failed restorations.
Case Study
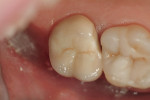
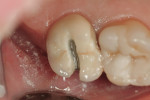
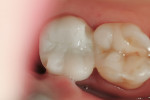
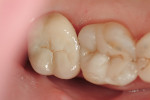
The female patient in this case presented with a failed zirconia restoration on the upper right second molar (Figure 1 and Figure 2). While disappointed in the life span of the failed crown, which had been less than 2 years, the patient requested a metal-free replacement restoration. The author reviewed the patient’s restorative options and the clinical procedures involved in removing the failed restoration. After this discussion, the patient confirmed that she wanted to replace it with another tooth-colored, metal-free zirconia restoration. A preoperative shade was taken with the digital VITA Easyshade® (VITA, https://www.vita-zahnfabrik.com) to get as close to a perfect match as possible.1
The clinical cause of the failure could not be definitively ascertained. There were no occlusal or immediately obvious clinical reasons; one hypothesis was porcelain failure resulting from a possible failure in the laboratory to adhere to the proper crown-building protocol. The patient was assured that extra careful attention would be put into the building of her next restoration to ensure a failure would not happen again. There are many clinical studies to support the everyday clinical use of metal-free zirconia restorations with the peace of mind that clinicians are delivering a very strong durable restoration to their patients.2-6
Removal of the Failed Restoration
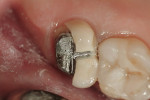
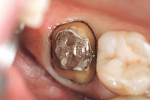
Removal of non-serviceable or obsolete restorations is frequently a time-consuming step in the preparation sequence. Choosing instruments designed and adapted for the removal of specific materials saves chair time, reduces risk of pulpal insult, and minimizes operator fatigue. A zirconia-based coping may demonstrate fracture strengths greater than 1,000 MPa; therefore, care is given to minimize and mitigate the heat generated during the sectioning process. In this case, task-specific Great White® Z Diamond instruments (SS White Burs, Inc, https://www.sswhiteburs.com) were used. Placing the Great White Z 801-014 round diamond at the buccal gingival margin, the facial aspect of the crown was sectioned through to the lingual just shy of the lingual margin (Figure 3 and Figure 4). Using a crown-spreader hand instrument or a small slot-head screwdriver placed in the separation groove, the instrument was gently rotated in the mesial distal direction. The crown separated, loosened, and came off (Figure 5). The author continued making separation slots until the entire failed restoration was removed. Upon removal, caries finder solution was applied to ensure the absence of clinical decay.
Preparation
Today’s all-ceramic restorations have high esthetic and functional survival rates. The failures that do occur are predominately failures related to inappropriate attention paid to the occlusal scheme, tooth preparation, improper restoration choice, or structural defects within the porcelain itself as sent from the laboratory.
The following step-by-step guidelines for full-coverage restorations were used to alter the existing preparation in the study case. The Great White Ultra 856-018 (SS White) carbide bur was used circumferentially to prepare the tooth for the full-coverage restoration. Correct axial reduction is a critical step in the preparation procedure. The round-end tapered carbide was used to create a clear, crisp chamfer margin and ensure reduction and angulations to provide a naturally emerging and functionally accurate restoration.
The main preparation parameterswere as follows: To ensurethe needed space for the technician to design the ideal soft tissue emergence profile,three planes of tooth structure were reduced, starting with a 1.5-mm reduction at the gingival level. The gingival margins should undulate in harmony with the contours of the gingival tissues through the interproximal areas for the establishment of equi-gingival or slightly supra-gingival position. Reduction would include a slight taper toward the occlusal surface.
Mid-body reduction of 1.5 mm would allow the ceramist to create mid-body chroma as needed. The cusp tip was reduced 1.5 mm to 2 mm with the lingual angulations, which allowed the ceramist to ideally place the cusp tips in the proper arch form while maximizing the esthetic outcome. The Great White Ultra 379-023 (SS White) football-shape carbide was used to accentuate occlusal reduction.
Essentially complete, the preparation was now evaluated in reference to the adjacent teeth and compared to their structural orientations. The patient was guided into functional movements to verify that adequate space had been created to meet all of the factors essential to a well-designed restoration. The use of a reduction guide made from the patient’s pre-cast models or from a diagnostic wax-up is a useful tool for three-dimensional evaluation. Fine-grit diamonds or finishing carbides idealize the preparation by eliminating irregularities and creating a clear and distinct margin. Additionally, all line angles were rounded and the taper of the preparation was finalized. To properly mount the models for good centric occlusion, the bite was registered using vinyl polysiloxane.
The soft tissue interface was managed by placing a 00 cord (Ultradent Products, Inc, https://www.ultradent.com) and using Expasyl™ (Kerr Corporation, https://www.kerrdental.com). When expressed into the sulcus, the clay-like aluminum-chloride impregnated material provided both adequate hemostasis and sulcular expansion.7 This method facilitated moisture control and 360° marginal visibility, which is key to obtaining an accurate final impression7,8 (Figure 6).
A vinyl polysiloxane light-body impression material, Flexitime® (Heraeus Kulzer, https://www.heraeus-kulzer-us.com) will define and impress the details of the preparation. A metal impression triple tray was loaded with heavy-body tray material and the impression was taken. It is the author’s choice not to use plastic triple trays because of possible flexing upon biting into the tray. After removal, the impression was checked for clarity (Figure 7).
Temporization
Creating a temporary comes at the end of a focused session of completing the needed prosthetic steps and clinicians would like nothing better than to make temporaries in a quick, simple, predictable manner. In this case, the preoperative bite was used and a self-cure resin was loaded into the tray. Once set, a finished temporary restoration was complete. A properly fitting provisional is important to the ultimate success of the case. It maintains contact points, occlusal stability, and also creates an ideal soft tissue response environment.8 The margins were trimmed with a Jazz P3S knife-edge disk (SS White) and finished with Sof-Lex™ finishing strips (3M ESPE, https://www.3mespe.com). The temporary restoration was secured using a non-eugenol temporary cement (Figure 8).
Laboratory Communication
Recognizing the quality of the communication between the clinician and the technician is a crucial factor in the indirect restorative process, a detailed prescription was sent to the laboratory. The prescription identified the chroma and values, indicating a rich chroma in the central fossa and high value or brightness up the cusp incline. In addition, intraoral photographs were sent with the prescription to assist the technician in matching characterizations.
Restoration Verification
It is the author’s preference to check for color, fit, contact points, and overall esthetic appearance when the completed restorations arrived from the laboratory. This saves rescheduling of the patient’s seating appointment should the restoration need to be sent back to the laboratory.
Seating the Restoration
The restoration was seated using RelyX™ Luting Plus (3M ESPE) (Figure 9). One way to maximize the opportunity for success is to pay close attention to occlusion. Correct anatomical occlusion helps a restoration to withstand the functional load placed on it, thereby eliminating one of the primary culprits in restorative failure.
In spite of pre-appointment inspection of restorations, some adjustments to contact surfaces and/or occlusal adjustments may be necessary. With the zirconia-based restorations, the author commonly uses the Great White Ultra 379-023 football-shape carbide for occlusal/lingual adjustments. Before cementation, the author polishes adjusted surfaces and gingival margins using Jazz P3S polishers. The use of diamond-impregnated polishers to finish the gingival margins improves tissue response and polishing the occlusal surface minimizes the abrasion of opposing dentition.
Conclusion
With the seemingly daily advances being made in esthetic and restorative materials, today’s dental patients have a menu of esthetic options from which to choose. Given the ever-increasing esthetic demands of society as a whole, it is not surprising that more and more patients select metal-free restorations.
The clinical predictability of zirconia has been developed to meet a broad range of clinical needs in reconstructive dentistry. But failures still happen and clinicians must be able to quickly rectify the situation for their patients in an efficient and timely manner. It is for this reason that careful attention to detail in all the steps—removal of obsolete restorations, preparation, and adjusting of all-ceramic restorations—improves the predictability of a restoration that is both esthetic and long-lasting. The use of rotary instruments specifically task-designed provides valuable tools that assist the clinician and ensure patient comfort and satisfaction.
References
1. Baltzer A, Kaufmann-Jinoian V. Shading of ceramic crowns using digital tooth shade matching devices. Int J Comput Dent. 2005;8(2):129-152.
2. Snyder MD, Hogg KD. Load to fracture value of different all-ceramic crown systems. J Contemp Dent Pract. 2005;6(4):54-63.
3. Blatz MB. Long term clinical success of all-ceramic posterior restorations. Quintessence Int. 2002;33:415-426.
4. Sorensen JA. The Lava all ceramic system: CAD/CAM zirconia prosthodontics for the 21st century. Contemporary Esthetics and Restorative Practice. 2003:2(1):3-6.
5. Tinschert J, Natt G, Mautsch W, et al. Fracture resistance of lithium disilicate, alumina, and zirconia based 3 unit fixed partial dentures; a laboratory study. Int J Prosthodont. 2001;14(3):231-238.
6. Piwowarczyk A, Ottl P, Lauer HC, Kuretzky T. A clinical report and overview of scientific studies and clinical procedures conducted on 3M ESPE Lava All-Ceramic System. J Prosthodont. 2005;14(1):39-45.
7.Shannon A. Expanded uses of a novel tissue retraction material. Compend Contin Educ Dent. 2002;(Suppl 1):3-6.
8. The periodontal-restorative interface in fixed prosthodontic tooth preparation, provisionalization, and biologic final impression. Part II. Prac Periodont Aesthet Dent. 1994;6(3):49-60.
About the Author
Andrew Shannon, DDS
Private Practice
Aesthetic Restorative Dentistry
Vancouver, British Columbia