Boosting Patient Esteem and Satisfaction with Whitening
Using a combination of in-office and take-home whitening treatments enables dentists to offer their patients superior whitening results.
Minimally invasive smile enhancements are increasingly requested in many dental practices today, and the most common and conservative method for quickly altering someone’s smile is the combination of in-office tooth whitening followed by take-home tray bleaching. Whether to lighten and enhance the smile or to remove noticeable and severe stains, vital tooth bleaching is a viable and realistic option for many patients as a means to improve the appearance of their teeth.1,2
Tooth discoloration may be the result of aging, disease, or exposure to medications, foods, and beverages. Intrinsic stains occur as a product of tooth development, fluorosis, or the use of tetracycline.3 Extrinsic stains form in the pellicle of the teeth and are produced by the reaction that occurs between sugars and amino acids or result from the retention of exogenous chromophores in the pellicle.3
Overall, the potential causes of tooth discoloration and stains may be varied and complex.4 Further, the tooth discoloration itself can vary in appearance, location, and severity in a tooth or across multiple teeth.5 The intensity of discoloration may be worse in the presence of enamel surface defects.5
Whitening regimens of various durations using peroxide agents have been described in the literature for treating intrinsic and extrinsic stains.6- 9 To remove intrinsic stains and alter the inherent tooth color, dentist-monitored tooth-whitening products that rely on proven technologies—such as 35% hydrogen peroxide for in-office power bleaching or 10% to 15% carbamide peroxide for at-home bleaching—have been used most often.3 However, a 38% hydrogen peroxide whitening gel for in-office bleaching treatment—followed by the use of a 10% carbamide peroxide at-home bleaching kit—has also been shown to produce significant tooth lightening.9
Depending upon the degree of tooth discoloration, take-home, patient-controlled but dentist-monitored vital tooth bleaching may be deemed adequate to effect the necessary color change in the teeth that will result in a significantly different smile appearance.10 In other cases, the take-home treatment may be preceded by in-office power bleaching. Using a combination of in-office and take-home whitening enables dental professionals to offer patients superior results.
Case Presentation
A 40-year-old female esthetician presented with a request for whiter teeth. Given the nature of her profession and her interaction with clients, she was acutely aware of the importance of an esthetic smile, and she felt that her teeth did not look “sparkling” or as “clean” as they could be. She specifically requested to avoid any procedure in which removal of tooth structure would be required.
A thorough examination was performed that included radiographs and intraoral digital photographs. No pathologies were found that would contraindicate vital tooth bleaching, whether in-office or take-home systems. The nature of the patient’s tooth discoloration was a dentin-influenced, deeper hue to the teeth. This was especially true in the canines, teeth Nos. 6 and 11, where a more yellow color was observed.
The patient was instructed about the variety of tooth-bleaching alternatives available, including light-activated, in-office bleaching followed by home bleaching using prefilled disposable whitening trays. The patient elected to whiten her teeth through a combination of in-office and take-home products.
Specifically, the patient would undergo in-office power bleaching using a chemically activated whitening gel (Opalescence® Boost™, Ultradent Products, Inc, www.ultradent.com). This 38% hydrogen peroxide power-bleaching gel represents a conservative alternative for treating discolored teeth. Additionally, to further enhance the whitening effects, a 10% hydrogen peroxide take-home system (Opalescence® Trèswhite ™ Supreme) featuring preloaded, preformed trays and fluoride would be dispensed for use for 10 days.
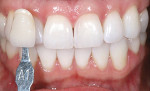
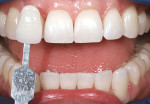
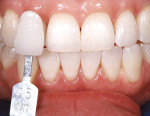
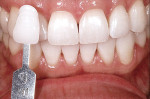
The shade of the patient’s teeth was evaluated against the classic Vita shade tabs and determined to be A1 (Figure 4). However, according to the Vita 3-D Master Shade Guide, the patient’s prebleaching shade was M1.5 (Figure 5). The goal of the whitening procedures was to achieve a higher value for the patient’s teeth.
Preparation for In-Office Bleaching
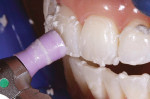
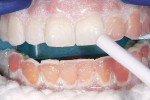
Before initiating the in-office whitening procedure, the tooth surfaces were cleansed to remove any calculus or extrinsic stains (Figure 6). While performing the prophylaxis, care was taken not to exceed 5,000 RPM.
Cheek and lip retractors were used, and cotton rolls and a facial mask were also used to prevent the whitening gel from contacting the patient’s skin. A generous amount of lip balm was applied to prevent the patient’s lips from drying out during the whitening procedure. The patient was also provided with suitable eye protection.
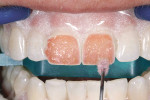
The teeth to be whitened were isolated using a unique, light-reflective and passively adhesive (sealing) light-cured resin (OpalDam®, Ultradent ). This was applied in a 1.5-mm to 2-mm thickness covering 4 mm to 6 mm apically from the gingival margin (Figure 7). Approximately 0.5 mm of protector was placed on the tooth surface adjacent to the gingival margin. After application, the gingival protector was cured for 20 seconds per light guide width using a quality curing light.
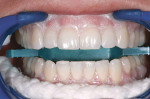
The surfaces of the teeth were then carefully cleaned with prophy paste to remove any excess resin film, taking care not to dislodge the cured barrier. Then, to facilitate the full-arch bleaching, a tongue/bite block (Figure 8) was placed in the molar region and held in place with gentle but firm biting pressure.
Application of In-Office Bleaching Agents
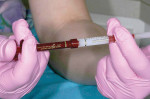
The activator and bleaching agent were thoroughly mixed using the syringe-to-syringe process (Figure 9), ultimately reaching the desired viscosity. The 38% hydrogen peroxide power-whitening gel was syringed onto the labial surface of each tooth to be whitened in a thickness of between 0.5 mm and 1 mm; the gel was extended slightly onto the incisal/occlusal edges.
The whitening gel remained on the teeth for 15 minutes. For optimum effectiveness, it was stirred or agitated on each tooth every 5 minutes (Figure 10).
The gel was removed from each tooth 15 minutes after application using suction only (Figure 11). A surgical aspiration tip worked well for this purpose, and water was not used during the initial suction. Once all visible gel was removed, the teeth were thoroughly rinsed, with the water directed toward the incisal edges of the teeth and high-volume suction used.
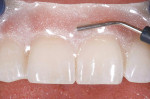
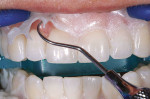
The teeth were then air-dried, after which the gingival barrier was lifted off using an explorer (Figure 12). Any gingival protector that remained interproximally was removed using floss or an explorer.
Take-Home Vital Tooth Bleaching
Before demonstrating and dispensing the selected take-home vital tooth-bleaching system (Opalescence Trèswhite Supreme), a subjective shade analysis of the patient’s teeth was performed. Her postbleaching shade was determined to be 0.5 M1 (Figure 13).
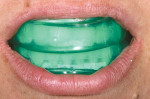
The patient was provided with a demonstration of the easy-to-use, pre-loaded maxillary and mandibular trays for the take-home vital tooth-bleaching system (Figure 14 and Figure 15). This bleaching system was selected based on the concentration of the active ingredient (ie, 10% hydrogen peroxide for faster whitening results), a more comfortable and conveniently pre-loaded tray/membrane design to help ensure patient compliance, and its fluoridated formula to reduce sensitivity, rebuild enamel, and prevent caries.11-14
The patient used the take-home regimen for 10 days for between 30 minutes and 1 hour each day. It is important to note that regardless of changes in formulations and delivery systems, the literature states that the efficacy of vital tooth-bleaching remains dependent upon tooth surfaces being in direct contact with the appropriate concentration of active whitening agents for a specific period of time.10
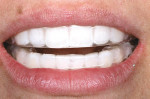
Ten days after the completion of at-home bleaching, the color change of the patient’s teeth was assessed. It was determined that the postbleaching shade that was achieved was 0.0 M1 (Figure 16).
Conclusion
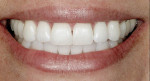
It benefits clinicians and their patients when conservative methods for enhancing the appearance of discolored teeth are considered and appropriately treatment planned (Figure 17). Effective combinations of in-office and take-home bleaching systems can accelerate the whitening process and make it more comfortable and convenient are welcome additions to the practitioner’s armamentarium. By enabling the patient to control and determine when the desired whitening effect had been achieved, her satisfaction with the final outcome was ensured.
Disclosure
Dr. Milnar has received financial and materials/product support from Ultradent Products, Inc.
References
1. Kihn PW. Vital tooth whitening. Dent Clin North Am. 2007;51:319-331.
2. Sarrett DC. Tooth whitening today. J Am Dent Assoc. 2002;133:1535-1538.
3. Viscio D, Gaffar A, Fakhry-Smith S, Xu T. Present and future technologies of tooth whitening. Compend Contin Educ Dent. 2000;28(Suppl):S36-S43.
4. Sulieman M. An overview of tooth discoloration: extrinsic, intrinsic and internalized stains. Dent Update. 2005;32:463-468.
5. Hattab FN, Qudeimat MA, al-Rimawi HS. Dental discoloration: an overview. J Esthet Dent. 1999;11:291-310.
6. Sulieman M, Addy M, Macdonald E, Rees JS. The bleaching depth of a 35% hydrogen peroxide based in-office product: a study in vitro. J Dent. 2005;33:33-40.
7. Leonard RH Jr, Bentley C, Eagle JC, et al. Nightguard vital bleaching: a long-term study on efficacy, shade retention. side effects, and patients’ perceptions. J Esthet Restor Dent. 2001;13:357-369.
8. Auschill TM, Hellwig E, Schmidale S, et al. Efficacy, side-effects and patients’ acceptance of different bleaching techniques (OTC, in-office, at-home). Oper Dent. 2005;30:156-163.
9. Deliperi S, Bardwell DN, Papathanasiou A. Clinical evaluation of a combined in-office and take-home bleaching system. J Am Dent Assoc. 2004;135:628-634.
10. Matis BA. Tray whitening: what the evidence shows. Compend Contin Educ Dent. 2003;24:354-362.
11. Basting RT, Rodrigues AL Jr, Serra MC. The effects of seven carbamide peroxide bleaching agents on enamel microhardness over time. J Am Dent Assoc. 2003;134:1335-1342.
12. Al-Qunaian TA. The effect of whitening agents on caries susceptibility of human enamel. Oper Dent. 2005;30:265-270.
13. Clark LM, Barghi N, Summitt JB, Amaechi BT. Influence of fluoridated carbamide peroxide bleaching gel on enamel demineralization. ADEA/AADR/CADR Meeting & Exposition; March 8-11, 2006: Abstract #0497.
14. Amaechi BT, Clark LM, Barghi N, Summitt JB. Enamel fluoride uptake from fluoridated carbamide peroxide bleaching gel. ADEA/AADR/CADR Meeting & Exposition; March 8-11, 2006; Abstract #0498.
About the Author
Frank J. Milnar, DDS, AAACD
Family, Cosmetic, and Restorative Dentistry
Saint Paul, Minnesota