What’s the Buzz?
Question: What’s the buzz about anesthesia? Answer: VibraJect.
Howard S. Glazer, DDS
It has been quite a while since the days of “Painless Parker,” and dental anesthesia has come a long way in being a more comfortable procedure. Key to that advancement has been the use of a vibrational device attached to the anesthetic syringe.
The brain recognizes changes in pressure and temperature and translates that information into pain. Furthermore, the brain can handle only one impulse at a time. To compensate for the puncture the syringe needle makes through tissue (read as pain), many dentist use the “wiggle and jiggle” technique when injecting into the mucobuccal fold, hoping this action distracts the patient. Such distraction causes the nerve endings to sense only the vibrations and not the sensation of the pressure associated with the injection.
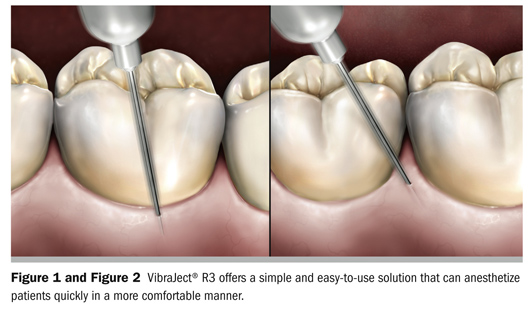
A vibrational device attached to a syringe uses this same concept of tricking the mind to recognize only the sensation caused by the “wiggle and jiggle” vibrations. The VibraJect® R3 (Miltex, Inc, York, PA) offers a simple and easy-to-use solution that can anesthetize patients quickly in a more comfortable manner (Figure 1 and Figure 2). Use of this two-piece device is simple: Just clip the VibraJect motor unit (a small battery-operated unit) onto the barrel of a conventional and/or intraligamentary syringe, turn it on, and use any standard technique for injecting the patient.
Not only is this device ideal for “normal” patients, but even more so for those patients who have a phobia of dental injections. The device also can be used with pediatric patients 5 years of age and older (as recommended by the manufacturer). In almost all cases, the need for topical anesthetic is eliminated, which saves time and money. A key point to remember when attaching the clip is that it must not cover or touch the anesthetic cartridge.
The system is useful with all types of routine dental injections. Typically, the most painful area for the patient to endure an injection is the palate. This, of course, is because the already taut tissue is stretched further when a bolus of anesthetic fluid is introduced, causing a great deal of pressure. The VibraJect enables a less painful palatal injection because it delivers small amounts of anesthetic solution over a period of time.
To anesthetize the mandible, most dentists were taught to use a regional block technique. While this technique is viable, three adverse effects are associated with the procedure: the risk of “missing” the site (ie, the area surrounding the inferior-alveolar canal orifice), second, the risk of paresthesia, and third, the patient’s lip and tongue may remain numb for several hours, thus impeding the ability to speak and function in a work or school environment. This author no longer gives traditional mandibular block injections. Following is a technique for mandibular injections that helps to eliminate these adverse effects and provide a positive experience for patients. The technique can be used for maxillary injections. In both instances, the technique relies on a very slow drip deposition of anesthetic fluid and using vibration, via the VibraJect.
Supplies
- Conventional aspirating syringe (Miltex, Inc) for maxillary injections
- N-Tralig® (Miltex, Inc) syringe for mandibular injections
- VibraJect R3
- Articaine hydrochloride 4% with epinephrine 1:100,000 (Septocaine® Gold, Septodont USA, New Castle, DE)
- 30-gauge, extrashort hypodermic needles (Septodont USA)
Mandibular Technique
Step 1: Approach the midline of the buccal sulcus with an N-Tralig syringe with a 30-gauge extra-short hypodermic needle, loaded with Septocaine Gold. Clip the VibraJect onto the barrel, close to the hub of the syringe. The syringe should be vibrating.
Step 2: With the long aspect of the bevel of the needle parallel to the long axis of the tooth, begin a slow drip (2 to 4 drops) of anesthetic fluid when approaching and entering the buccal sulcus.
Step 3: After entering the sulcus, slowly drip anesthetic fluid until resistance is felt at the periodontal ligament.
Step 4: At the periodontal ligament, deposit another 2 to 4 drops while penetrating slightly beyond the ligament.
Step 5: Next, repeat Step 1 through Step 4 for the mesiobuccal and the distobuccal aspects of the tooth, remembering to inject slowly.
Step 6: Approach the midline of the lingual sulcus. Again, have the long aspect of the bevel of the needle parallel to the long axis of the tooth and slowly drip anesthetic fluid when approaching the sulcus.
Step 7: After reaching the lingual periodontal ligament, slowly deposit another 2 to 4 drops of anesthetic fluid while penetrating slightly beyond it
Step 8: Repeat Steps 1 through 5 for the mesiolingual and distolingual aspects of the tooth, remembering to inject slowly.
Maxillary Technique
Step 1: Attach a 30-gauge extra-short hypodermic needle loaded with Septocaine Gold onto an aspirating syringe. Clip the VibraJect onto the barrel close to the hub end. The syringe should be vibrating.
Step 2: Approach the mucobuccal fold in the apical area of the tooth with the long aspect of the bevel parallel to the long access of the tooth, and slip the tissue over the bevel by elevating the lip and slowly deposit only a few drops of anesthetic fluid.
Step 3: For the palatal injection, again approach the palatal surface near the approximate apical root end of the involved tooth with the long aspect of the bevel parallel to the long access of the tooth.
Step 4: Puncture the tissue, and slowly deposit only a few drops of anesthetic fluid.
Tips
- Recharge the batteries overnight; do not leave the batteries in an unplugged charger.
- Do not autoclave the motor unit; simply wipe it with any cold sterilizing solution.
- The first time a patient says “ouch,” it is time either check the technique and/ or recharge the battery.
- The injection should be a very slow drip technique.
Undoubtedly, an extra benefit is the practice building that will result when patients tell family and friends about their painless injections. This technique also saves time by eliminating the time it takes for topical and block anesthesia to take effect. With this technology, dentists can treat multiple quadrants, often eliminating the need for additional appointments. This time savings also has economic benefits, creating time to treat an additional patient each day and ultimately adding to the practice’s bottom line. After becoming comfortable with this technique, dentists will be not only high-tech, but also making happy, loyal, and referring patients.
For more information, contact:
Miltex, Inc.
Phone: 800-645-8000
Web: www.miltex.com
The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dentistry. The preceding is not a warranty, endorsement, or approval for the aforementioned products or services or their effectiveness, quality, or safety on the part of Inside Dentistry or AEGIS Communications. The publisher disclaims responsibility for any injury to persons or property resulting from any ideas or products referred to in the precedingmaterial.
About the Author
This article was written by Howard S. Glazer, DDS.