Using a Simplified Composite System to Esthetically Restore Non-Carious Class V Lesions
Frank J. Milnar, DDS, AAACD
Class V cervical lesions can be carious or non-carious. When non-carious in nature, they may be classified as abfractions, despite some controversy surrounding this terminology. Their appearance may be characterized by a loss of hard dental structure near the cemento-enamel junction. The shape of the lesion may resemble a wedge with an inward-pointing apex.1
The literature suggests that cervical lesions occur in 85% of the population,1 but anecdotally, the incidence may be significantly higher in individuals with permanent teeth because the aging population is increasing dramatically. At a time when people are maintaining their natural teeth longer, there is an increased likelihood that caries will develop in class V areas.2
The cause of abfractions has been thought to be occlusal stress. This stress produces cervical cracks and subsequently predisposes the surface to the effects of erosion and abrasion.3 However, critical literature reviews suggest that abfraction is a hypothetical component of cervical wear.3 Regardless of the nomenclature used for their classification, it is important to determine possible causative factors for non-carious lesions, as treatments range from eliminating the aggravating agents to specific restorative procedures.4
Among the materials used to treat non-carious class V lesions have been glass-ionomer cements, compomers, and composite resins.1 When the class V lesions have been carious and in areas of esthetic concern, a combination of glass-ionomer restorative materials (eg, for the internal aspect of the restoration) and resin-based composite materials (eg, for the surface of the restoration) has been advocated based on their esthetic results and potential for caries reduction.2
Based on their ability to bond to tooth structure, esthetic potential, and their physical properties, resin composites have been considered by some practitioners as the best materials for restoring cervical defects.4 After 3 years, resin composite restorations that were placed to treat non-carious cervical lesions exhibited no secondary caries, and composite restorations demonstrated less deficiencies in marginal adaptation at 3 years than compomer restorations.5
However, placing composite resin restorations in esthetically sensitive areas of the mouth (eg, anterior teeth) requires an understanding of the composites to be used and their respective optical and physical characteristics.6,7 This will enable their use and placement to replicate the polychromatic effects that are seen in natural teeth. Simultaneously and most importantly, producing outstanding composite resin restorations also necessitates a thorough comprehension of natural tooth morphology and how each component of tooth structure affects esthetics.8,9
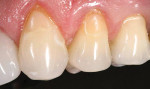
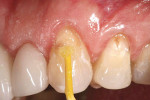
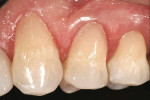
A 45-year-old man presented with non-carious cervicallesions on teeth Nos. 11 through 13 (Figure 1). A complete examination was performed that included radiographs,photographs, and a review of thepatient’s periodontal condition. Occlusal analysis determined that no interferences or contributory factors would require functional and/or occlusal rehabilitation. No pathologies were found that might contraindicate conservative and esthetic treatment using a simplified esthetic composite system (Amaris®, Voco America, Inc, Sunnyside, NY).
The selected composite system is based on a simplified concept of tooth structure and color. In essence, dentin shines through enamel and, combined, these two components define the color and appearance of a natural tooth. Therefore, the chosen composite system requires two steps—the selection and placement of the appropriate opaque dentin composite layer and the selection and placement of a translucent enamel layer that can lighten, darken, or complement the opaque shade. The combination of two composite layers—similar to the combination of two component tooth structures—results in the desired optical effects of the restoration.
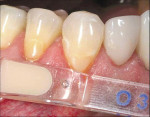
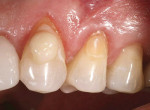
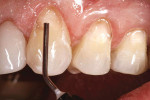
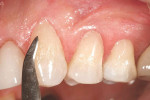
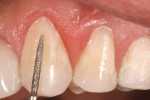
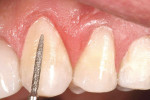
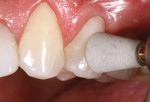
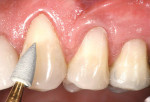
The Voco Amaris® composite shade guide was used to take a preoperative cervical shade of the patient’s teeth (Figure 2). The selected dentin composite shade—Shade 03—was previewed on tooth No. 11 (Figure 3).
In natural teeth, there are areas where the translucent enamel layer will be thinner and the dentin will be closer to the surface. The cervical areas of the teeth—such as in this case—are a good example of this. Therefore, when restoring these non-carious lesions, it was important to re-establish the dentin in these areas using a properly opaque composite and bringing it closer to the surface of the tooth.8 It would then be important to control the value of this dentin shade using the correct translucent enamel layer.8
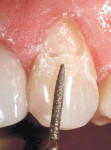
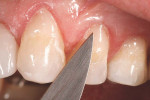
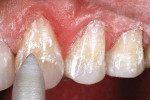
The patient was anesthetized, his lips and cheeks properly retracted, and the immediate surrounding dentition was isolated with cotton rolls. A slight bevel preparation was made on each of the teeth from Nos. 11 through 13 (Figure 4). After the bevel preparations were made, a single-step, self-etching adhesive (Futurabond, Voco America) was placed (Figure 5). This adhesive was placed on the preparations for 20 seconds, lightly air-dried for 5 seconds, and light-cured for 10 seconds. It has been shown that single-step, self-etching adhesives have acceptable clinical retention rates to dentin surfaces when used in non-carious cervical lesions.10
A flowable, high opaque (HO) composite was used for wettability and to mask the dark inner highly saturated color demonstrated on teeth Nos. 11 through 13 (Figure 6). 11 Then, a 2-mm layer of the dentin/opaque material composite in 03 was placed on teeth Nos. 11 through 13 using an esthetic contour placement instrument (Clinician’s Choice, London, Ontario, Canada) (Figure 7). This layer was cured for 20 seconds per tooth.
A 2-mm layer of the translucent shade of the composite was placed on teeth Nos. 11 through 13 (eg, Dark Translucent [DT] on tooth No. 11; Neutral Translucent [NT] on tooth No. 12; and Neutral Translucent [NT] on tooth No. 13) (Figure 8). It was properly sculpted into place and then cured for 20 seconds per tooth.
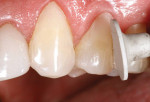
The restorations were assessed after placement of the translucent composite layer and then underwent a 360° polymerization for 60 seconds each (Figure 9). The surface texture of the restorations was then refined using a diamond bur (Brasseler USA, Savannah, GA) (Figure 10).
Subsequently, after the application of polish, heavy pressure was applied to two components of a composite finishing system (Shape and Shine™, Clinician’s Choice) to finish the restorations (Figure 11 and Figure 12). Finally, by applying light pressure, three components (eg, cup, point, and disc, respectively) of an innovative polishing system (Shape and Shine™, Clinician’s Choice) were used to impart a final polish and luster to the restorations (Figure 13, Figure 14, Figure 15).
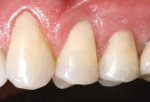
Dentistry is mastering its understanding of tooth structure and also the optical and physicalproperties of futuristic and next-generationrestorative materials. As a result, the clinical protocol for creating life-like and natural-looking restorations is returning to an age ofsimplicity. The final restorativeresults achieved in this case (Figure 16) represent what is possible usingonly two shades of composite—one in opaque dentin and one in translucent enamel—to replicate the form and function of natural tooth structure.
Dr. Milnar has received financial and materials/productsupport from Voco America, Inc.
References
1. Ceruti P, Menicucci G,Mariani GD, et al. Non carious cervicallesions. A review. Minerva Stomatol. 2006;55:43-57.
2. Christensen GJ. The “new” operative dentistry. J Am Dent Assoc. 2006;137:531-533.
3. Bartlett DW, Shah P. A critical review of non-carious cervical (wear) lesions and the role of abfraction, erosion, and abrasion. J Dent Res. 2006;85:306-312.
4. de Melo FV, Belli R, Monteiro S Jr, et al. Esthetic noncarious Class V restorations: a case report. J Esthet Restor Dent. 2005;17:275-284.
5. Pollington S, van Noort R. A clinical evaluation of a resin composite and a compomer in non-carious Class V lesions. A 3-year follow-up. Am J Dent. 2008;21:49-52.
6. Terry DA, Geller W, Tric O, et al. Anatomical form defines color: function, form, and aesthetics. Pract Proced Aesthet Dent. 2002;14:59-67.
7. Terry DA. Dimensions of color: creating high-diffusion layers with composite resin. Compend Contin Educ Dent. 2003;24(2 Suppl):3-13.
8. LeSage B, Milnar F, Wohlberg J. Achieving the epitome of composite art—advanced concepts in shade selection and layering composite. Journal of Cosmetic Dentistry. Accepted July 2008. In press.
9. Milnar FJ. Altering tooth inclination and overall esthetics with direct composite veneers, gingival contouring, and enamelplasty. Inside Dentistry. 2006;2(1):46-49.
10. van Dijken JW, Sunnegårdh-Grönberg K, Sörensson E. Clinical bonding of a single-step self-etching adhesive in noncarious cervical lesions. J Adhes Dent. 2007;9(Suppl 2):241-243.
11. Celik C, Ozgunaltay G, Attar N. Clinical evaluation of flowable resins in non-carious cervical lesions: two-year results. Oper Dent. 2007;32(4):313-321.
About the Author
Frank J. Milnar, DDS, AAACD
Family, Cosmetic and Restorative Dentistry
Saint Paul, Minnesota