Changes in the Demographics of Oral Cancer
Margaret I. Scarlett, DMD
Despite advances in survival rates for all cancers in the United States, 5-year survival rates for oral cancer stubbornly remain under 60% and less than 50% for 10-year survival. Part of the reason is that most oral cancers are diagnosed in the late stages of disease.1 Experts believe that early detection may be one tool to increasing long-term survival rates. Recently, data suggests that more oral cancers can be attributed to increasing rates of oral viral infection with certain types of human papillomavirus (HPV) among people under the age of 40.2 These types, notably HPV 16, and to a lesser degree HPV 18, are involved in squamous-cell carcinomas of the base of the tongue, tonsillar area, and posterior oropharyngeal wall. This is new information for many on the oral healthcare team.
Not all oral cancers can easily be detected visually; however, now that new adjunctive screening and detection methods are available, dentists can provide increased life-saving benefits for patients through more comprehensive oral cancer examinations. This article will review newly available scientific information about oral cancers, evidence gaps, and new techniques to assist the clinician in oral cancer diagnosis.
Last year, more than 35,000 new cases of oral and oropharyngeal cancer were diagnosed, with about 7,600 deaths attributed to the disease.1 This represents an increase of about 15% from the 1990s, and is most probably a result of improved detection by the dental team.2 Oral cancers occur in a variety of oral and perioral sites (Table 1) and account for about 2.5% of all cancers diagnosed last year in the United States.1
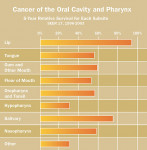
Approximately two thirds of oral cancers occur in the oral cavity, with the remainder occurring in the oropharynx. After the oropharynx (44%), the most common site for oral cancer is the lateral border of the tongue, followed by the floor of the mouth and the soft palate/tonsil/trigone.1 While 5-year survival rates have not improved as much as other cancers, such as colorectal or breast cancer, since the 1970s, oral cancer impacts different segments of the US population differently. For example, mortality from oral cancer is nearly twice as high in African-American men as it is in white men.3 Late detection and delayed care for black men has been implicated as a key reason for these differences. In addition to population differences, gender differences exist, with men about two times more likely to be diagnosed than women.3 About 72% of new cases of oral cancer are estimated to occur among men.3 The highest percentage of new cases is among African-Americans, compared to Hispanics and Caucasians.3
Recent evidence has emerged that the risk factors associated with the oral cancers being detected are changing. Dental team members should know that HPV has been implicated in at least one subset of oropharyngeal cancers, with a subset of these related to the oral cavity. A case control study of HPV and oropharyngeal cancers showed a very high association between HPV high-risk type 16 and oral cancer (odds ratio [OR] of 14.6 at a 95% confidence interval [CI], 6.3 to 36.6).4 Other studies show that at least 15% to 25% of oropharyngeal cancers are associated with HPV 16, one of the high-risk types of HPV.4-8 These high-risk types of HPV are different than low-risk types causing oral warts (ie, HPV 6 and HPV11).
While natural history studies of HPV in the oral cavity are incomplete largely because of sampling site selection and detection difficulty, the percentage of oropharyngeal cancers attributed to HPV has increased. From 1998 to 2003, new cases of potentially HPV-associated cancers of the oropharynx in the tonsilar area and the base of the tongue both increased significantly.5 The annual percentage change of potentially HPV-associated cancers was 3%, which was statistically significant (P < .05). New cases of oral cancer at other comparison sites decreased during the same time.5
The early signs of oral cancer are often painless, with detection occurring through a combination of patient symptoms and a thorough soft tissue head-and-neck examination by a dental or medical professional.A thorough head-and-neck examination includesboth visual inspection and palpation ofthe extraoral head and neck soft tissues, oralcavity, and oropharynx.In the intraoral part of the examination, the clinician should palpate the tongue, floor of the mouth,palate, salivary glands (submandibular and sublingual), lymph nodes (thesealong with the parotid nodes are included in the extraoral palpation), buccal mucosa, and the posterior oropharyngeal wall to checkfor abnormalities.Having the patient lift and move the tongue from side to side confirms functionality; theclinician should grasp the tip of the tongue and retract it to allow for direct visual inspection and palpation of its dorsum, ventral, andlateral areas; visual inspection of the base of the tongue is difficult butit may be palpated.
According to the Centers for Disease Control and Prevention (CDC), the signs and symptoms of oral cancer are:2
- A mouth sore that fails to heal or that bleeds easily
- A white or red patch in the mouth that will not resolve
- A lump, thickening, or soreness in the mouth, throat, or tongue
- Difficulty chewing or swallowing food
Avoiding high-risk behaviors, such as tobacco and alcohol abuse, are critical in preventing oral cancers. Changingoral sexual behaviors (ie, increased frequency with increased multiple partners) among young people may increase HPV acquisition. Risk factors for developing oral cancer are:
- Tobacco use (cigarette, smokeless, pipe smoking, cigars)
- Excessive alcohol consumption
- Viral infections, especially HPV
- Immunodeficiency
- Poor nutrition
- Excessive exposure to ultraviolet light (vermilion and skin of lip cancer)
- Certain occupational exposures, such as excessive sunlight for outdoor workers1-11
Staging describes the clinical size, extent, and/or spread of the cancer at time of diagnosis and, thus,its prognosis. The “TNM” staging system is used to assess the size of the primary tumor (T), absence or presence of regional lymph node involvement (N), and absence or presence of distant metastases (M).2 After the T, N, and M values are determined, suspected lesions are categorized (or assigned) as either Stage I, II, III, or IV, with IV being the most dire prognosis. Generally, Stage I is a lesion of less than 2 mm in diameter, with Stage II, III, and IV being more advanced disease; however, a small Stage I lesion with local or distant metastatic spread is staged with a higher value and thus a lower prognosis.1
Invasive surgical biopsy is the best way to diagnose and, ultimately, stage cancers. Thus, earlier detection of oral cancer in a dental office is associated with a lower stage.15 Some key facts about lip cancer:
- Vermilion and skin of lip cancer is diagnosed two to six times as frequently as intraoral sites and at Stage I more than 80% of the time (Figure 1).
- The 5-year relative survival rate is much better for lip cancer than oral cavity and oropharynx subsites, with hypopharynx being the lowest (Figure 2). 12
- Lip cancer has a better 5-year relative survival rate even when comparing only cases diagnosed at Stage I.12
While the oral biofilm contains more than 700 species of organisms, many of which have not been cultured outside of the mouth, evidence is emerging that disruptions in the oral biofilm occur in the presence of oral cancers.13 Whether this will be useful in the future for detecting oral cancers is not yet known. Elevated levels of three unique bacteria in saliva have been exclusively isolated from patients with oral squamous-cell carcinoma (OSCC) when compared to other patients.14 The sensitivity (disease recognized in diseased individuals) and specificity (no disease recognized in truly healthy people) of the presence of these organisms—Capnocytophaga gingivalis, Prevotella melaninogenica, and Streptococcus mitis—in saliva, compared to OSCC-free subjects, was more than 80%.14 More scientific inquiry is needed.
Even though survival rates are not much better than they were a few years ago, survival after radiation therapy is more commonplace than a decade ago. Johns Hopkins University researchers suggested that recent improvements in survival with radiotherapy could be the result of a shift in more HPV-associated squamous cell carcinoma.15 However, if more dentists used the new adjunctive screening methods to detect oral cancer earlier, it could further contribute to declines in its death rate.
In 2006, a Cochrane Collaboration evidence-based review16 noted that there was insufficient evidence to suggest that oral cancer screening is effective; however, there was only one long-term study which assessed the difference in oral cancer mortality over 10 years between a screened group and an unscreened group. The Cochrane review results mean lack of evidence, not lack of effectiveness. The lack of long-term studies, as well as a lack of comparative studies of different methods, hampers having definitive scientific answers about the effectiveness of oral cancer screening.16
A traditional oral cancer examination with palpation remains the goldstandard for diagnosis of oral cancer lesions. If visualization for suspicious oral mucosal lesions is difficult,diagnostic aids may be useful. Toluidine blue, a blue pheothiazinedye, has been used for years to identify andmark suspicious lesions. ViziLite® Plus with TBlue® (Zila Pharmaceuticals, Inc, Phoenix, AZ) has a chemiluminescent light source used to enhance identification of lesions and marking the lesions with toluidine blue, after an initial acetic acid rinse. Scalpel biopsy with pathology reports provides the most definitive diagnosis, while brush biopsy has been used before scalpel biopsy for suspected lesions with nearly 50% sensitivity.17 VELscope® (LED Dental, Inc, Vancouver, British Columbia, Canada) is another instrument used for oral cancer screening. Recently, a new detection device, Identafi™ 3000 (Trimira™, LLC, Houston, TX) has been introduced that uses multiple spectrums of wavelengths of light to monitor biochemical and tissue changes. While published studies comparing one method to another are limited, each of these methods may beuseful for visualization of lesions in conjunction with traditional oral cancer examinations.
A systematic review of 23 studies assessed the effectiveness of some of these adjunctivetechniques for oral cancer diagnosis.18 Published in 2008, this analysis updated a previous review in 2003.19 The authors reviewed ViziLite Plus with TBlue, Microlux DL (AdDent, Danbury, CN), Orascoptic DK™ (Orascoptic, Middleton, WI), VELscope, and OralCDx® (Oral CDx Laboratories, Suffern, NY) brush biopsy. They concluded that toluidine blue was effective as a diagnostic aid for use in high-risk populations and suspicious mucosal lesions. They concluded that there was insufficient data to assess the effectiveness of the aids reviewed. This affirmed the need for a thorough clinical examination and palpation for detection and diagnosis of oral cancer or suspicious mucosal lesions.18 The American Dental Association (ADA) and the CDC hosted an expert panel in April 2009 to develop evidence-based clinical recommendations for all healthcare practitioners. They addressed key questions, such as whether visual and tactile examination by a dentist reduces morbidity or mortality from premalignant or early malignant oral and oropharyngeal cancer. They also discussed the properties of the diagnostic aids listed above as well as the risk factors and characteristics of populations at highest risk for oral cancer.20 By the end of the year, the ADA and the CDC are expected to release evidence-based recommendations to enhance early detection of oral cancers.
Early detection of oral cancer may provide life-saving benefits to patients, while enhancing treatment outcomes and survival rates, and newadjunctive screening methods for oral cancer detection are available. Thesenewer detection techniques will make oral cancer screening easier to add toa pre-existing standardized examination in thedental practice. Consider advocatingfor increased community and professionalefforts to encourage others to perform life-saving oral cancerscreenings in their practices.21-24
References
1. American Cancer Society. Cancer Facts and Figures. 2008. Available at: www.cancer.org.
2. CDC. Oral Cancer: Deadly to Ignore. Available at: www.cdc.gov/OralHealth/publications/factsheets/oc_facts.htm.
3. Ries LAG, Melbert D, Drapcho M, et al. SEER Cancer Statistics Review, 1975-2005. National Cancer Institute. Bethesda, Md: 2008.
4. D’Souza G, Kreimer AR, Viscidi R, et al. Case control study of human papillomavirus and oropharyngeal cancer. N Engl J Med. 2007;10:356: 1944-1956.
5. Ryerson AB, Peters ES, Coughlin SS, et al. Burden of potentially human papillomavirus-associated cancers of the oropharynx and oral cavity in the US, 1998-2003. Cancer. 2008;113:2901-2909.
6. Benard VB, Johnson CJ, Thompson TD, et al. Examining the association between socioeconomic status and potential human papillomavirus-associated cancers. Cancer. 2008;113(10 Suppl):2910-2918.
7. Kreimer AR, Clifford GM, Boyle P, Franceschi S. Human papillomavirus types in head and neck squamous cell carcinomas worldwide: a systematic review. Cancer Epidemiol Biomarkers Prev. 2005;14:467-475.
8. Anil K, Chaturvedi EA, Engels WF, et al. Gillison incidence trends for human papillomavirus—related and unrelated oral squamous cell carcinomas in the United States. J Clin Oncology. 2008;26:612-619.
9. Kujan O, Glenny AM, Oliver RJ, et al. Screening programmes for the early detection and prevention of oral cancer. Cochrane Database Syst Rev. 2006;3:CD004150.
10. Schwartz SM, Daling JR, Doody DR, et al. Oral cancer risk in relation to sexual history and evidence of human papillomavirus infection. Journal of the National Cancer Institute. 1998;90:1626-1636.
11. Reichman M. National Cancer Institute Summary Data from Surveillance, Epidemiology, and End Results (SEER). Presented to Healthy People 2020 Dental Health Objectives meeting, March 4, 2009.
12. Gillison ML, Koch WM, Capone RB, et al. Evidence for a causal association between human papillomavirus and a subset of head and neck cancers. Journal of the National Cancer Institute. 2000;92: 709-720.
13. Nagy KN, Sonkodi I, Szöke I, et al. The microflora associated with human oral carcinomas. Oral Oncol. 1998;34(4):304-308.
14. Mager DL, Haffajee AD, Devlin PM, et al. The salivary microbiota as a diagnostic indicator of oral cancer: A descriptive, non-randomized study of cancer-free and oral squamous cell carcinoma subjects. J Transl Med. 2007;3:27.
15. Holmes JD, Dierks EJ, Homer LD, Potter BE. Is detection of oral and oropharyngeal squamous cancer by a dental health care provider associated with a lower stage at diagnosis? J Oral Maxillofac Surg. 2003; 61(3): 285-291.
16. Kujan O, Glenny AM, Oliver R, et al. Screening programmes for the early detection and prevention of oral cancer. Cochrane Database of Systematic Reviews. 2006, Issue 3.
17. Poate TW, Buchanan JA, Hodgson TA, et al. An audit of the efficacy of the oral brush biopsy technique in a specialist oral medicine unit. Oral Oncol. 2004;40(8):829-834.
18. Patton LL, Epstein JB, Kerr AR. Adjunctive techniques for oral cancer examination and lesion diagnosis: a systematic review of the literature. J Am Dent Assoc. 2008; 139(7):896-905.
19. Patton LL. The effectiveness of community-based visual screening and utility of adjunctive diagnostic aids in the early detection of oral cancer. Oral Oncol. 2003; 39(7):708-723.
20. American Dental Association Center for Evidence-Based Dentistry. Available at: https://ebd.ada.org/SystematicReviewsCategories.aspx?IndexId=6b78bbdf-3115-49c9-94d4-3f703693cfe9. Accessed May 6, 2009.
21. Centers for Disease Control and Prevention. Preventing and controlling oral and pharyngeal cancer. Recommendations from a national strategic planning conference. MMWR. 1998:47(RR14).
22. Horowitz AM, Nourjah P, Gift HC. US adult knowledge of risk factors and signs of oral cancers: 1990. J Am Dent Assoc. 1995; 126:39-45.
23. Alfano MC, Horowitz AM. Professional and community efforts to prevent morbidity and mortality from oral cancer. J Am Dent Assoc. 2001:(Suppl 132):24S-29S.
24. Centers for Disease Control and Prevention. Examinations for oral cancer, United States, 1992. MMWR. 1994;43:198-200.
About the Author
Margaret I. Scarlett, DMD
President
Scarlett Consulting International
Atlanta, Georgia