Increased Efficiency with Modern Technology and Restorative Materials
Composite restorations have been improving over the past 10 years but still require a few steps to achieve adequate bond strengths and longevity. This often results in a second appointment after a cavity is diagnosed at hygiene or examination appointments. However, a new generation of self-adhesive composite restorative material is available that reduces the time it takes for simple restorations. This will allow for increased office efficiency and patient satisfaction.
Case Report
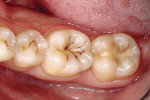
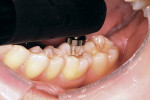
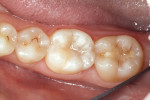
A 34-year-old woman came to the office for a routine hygiene visit. Her teeth were photographed with a high-resolution digital camera to evaluate them for pathology (Figure 1). After her cleaning was complete, a laser cavity detector (DIAGNOdent, KaVo Dental Corporation, Lake Zurich, IL) was used to evaluate all suspicious grooves for decay. The DIAGNOdent recorded a 33 score for the occlusal of tooth No. 19 (Figure 2).
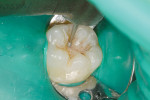
The decay was then confirmed with a digital radiograph. It is interesting to note that the traditional method of plunging an explorer tip into the groove to check for a “stick” did not reveal any decay as the tip did not stick in the groove. Dental loupes with LED illumination and rubber dam isolation were used to improve vision while restoring the tooth (Figure 3).
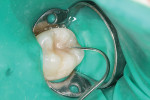
Because of the small size of the cavity, no anesthetic was given. Topical anesthetic was applied to the gum tissue to reduce discomfort from the rubber dam clamp. The decay was removed using an electric high-speed drill (Ti-Max Ti95L/NSK, Brasseler USA, Savannah, GA) and nano-preparation diamond burs (N379 009 Nano diamond bur, Axis Dental, Coppell, TX). Note the amount of decay clearly visible within each groove after the groove was opened. The enamel was lightly roughened slightly past the edge of each groove (Figure 4). The self-adhesive composite will have a stronger bond to cuIncreased Efficiency with Modern Technology and Restorative Materialst enamel as compared to uncut enamel.
After the remaining decay was removed from each groove, a first layer of A1 self-adhesive flowable composite (Fusio Liquid Dentin, Pentron Clinical Technologies, Wallingford, CT) was placed in the floor of the preparation. By using an A1 shade, the small amount of dentin that was removed was replicated. A 0.5-mm layer was applied just to the floor of the preparation. The self-adhesive flowable composite was allowed to sit in the tooth for 20 seconds to condition the enamel and dentin. While sitting in the preparation, the composite was agitated slowly with an explorer and dragged into each grove. (If the composite layer is too thick, air bubbles can be incorporated into the restoration by the explorer.) The first layer was cured for 10 seconds with an LED curing light (Demi LED Light Curing System, Kerr Corporation, Orange, CA). A second layer of B1 self-adhesive flowable composite was applied to the middle of the preparation and dragged to the extent of each groove to simulate any enamel that was removed (Figure 5). By applying such a small amount of composite to simply replace the amount of tooth structure removed with the nano-diamond bur, no occlusal adjustment was needed (Figure 6).
Conclusion
With the use of modern dental technology such as digital cameras, digital radiography, and laser cavity detectors, patients can have cavities diagnosed and restored at a very early stage and usually with no anesthetic. With the use of micro burs and dental loupes, the cavity preparation can be kept extremely conservative. The use of self-adhesive flowable composites allows the restorations to be completed in a very short period of time, with confidence that the restoration will be of high quality. In this case, each layer of composite took no more than 40 seconds to apply, sit for 20 seconds, and cure. The entire restoration took 10 to 15 minutes and was completed in the hygiene operatory. The use of modern restorative materials allowed for greater efficiency, patient comfort, and office production while deceasing overhead and stress.
For more information, contact:
Pentron Clinical Technologies
Phone: 800-551-0283
Web: www.pentron.com
Disclaimer
The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dentistry. The preceding is not a warranty, endorsement, or approval for the aforementioned products or services or their effectiveness, quality, or safety on the part of Inside Dentistry or AEGIS Communications. The publisher disclaims responsibility for any injury to persons or property resulting from any ideas or products referred to in the preceding material.