Retro-Fitting an Existing Crown Adjacent to a Removable Partial Denture in a Single Visit
Gregg A. Helvey, DDS, MAGD
There is an increasing interest in “digital” restorative dentistry with the recent introduction of new scanning devices for the fabrication of chairside and off-site restorations. The chairside model-free/ impression-free systems include CEREC® (Sirona Dental Systems, Charlotte, NC) and the newly introduced E4D (D4D Technologies, LLC, Richardson, TX). These two technologies allow the clinician to provide one-appointment indirect restorations. There are also chairside scanners, while providing an impression free scenario, that are used to create milled laboratory models on which the restorations are fabricated. These include the Lava™ Chairside Oral Scanner (3M ESPE, St. Paul, MN) and iTero™ (Cadent, Carlstadt, NJ).
The CEREC® and E4D systems can use different programs that can ease the difficulty of certain restorative procedures. One, for instance, is retro-fitting a crown adjacent to an existing removable partial denture (RPD). There are several techniques found in the literature including a previous one from this author that describe chairside and laboratory steps in creating a crown to fit the spatial requirements of a tooth to which a RPD is adapted.1-6
The CEREC software has a correlation mode in which an existing tooth is scanned and used to model the final restoration. In other words, the program can copy the contours of an existing tooth and provide a duplicate crown that will allow the full seating of an existing RPD. This program mode eliminates the numerous steps that were once necessary to provide this restorative procedure.
This article will describe the technique in which the data was acquired and the restorative material used to fabricate the full crown. It will also include the cementation procedure in which the restoration was permanently placed.
Case Study
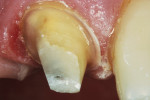
A 50-year-old patient presented with an existing RPD where one of the previously placed crowns on the maxillary right central incisor was broken. Upon examination, it was noted that some of the natural tooth structure had also fractured and separated. It appeared that the remaining tooth structure was insufficient to retain a new crown. Different treatment options were presented to the patient. The patient felt comfortable with the option of performing root canal therapy with subsequent placement of a post and core followed by a new crown designed to fit his existing RPD. The patient was also excited that this could be accomplished in one appointment.
Treatment Sequence
The fractured parts of the existing crown were temporarily replaced on the tooth. The correlation mode was selected in the CEREC program. The two maxillary central incisors were powdered and captured by the hand-held acquisition device. The fractured parts were then removed. Root canal therapy was completed followed by placement of a prefabricated post (Essential Dental Systems, Inc, Hackensack, NJ). A resin-modified glass ionomer was used to create the core. The tooth was then prepared for a full crown. After the initial preparation, it was obvious that the prefabricated post was still visible and could compromise the esthetic appearance of the final restoration. A less light-illuminating material was selected to prevent any of the gray post color from bleeding through an all-ceramic restoration. The clinician should select the restoration type and material before the final preparation of the tooth is completed. Each restorative material has specific preparation requirements that must be met to ensure the success of that restoration.
In this case, IPS e.max CAD LT (Ivoclar Vivadent, Amherst, NY) was selected for the fabrication of the crown. IPS e.max CAD is a lithium disilicate glass-ceramic material that can be used for anterior and posterior full anatomical crowns. The glass-ceramic is provided to the clinician or laboratory technician in a crystalline intermediate phase that must undergo final crystallization to obtain full strength. The material can come in block form that is suitable for computer-aided design/computer-aided manufacturing (CAD/CAM). This restorative material is also provided in an ingot form that can be used in a hot-ceramic pressing procedure. When using the material with the CEREC system, the crown is designed in full contour and then milled. The IPS e.max CAD block is available in medium opacity (MO) and low translucencies (LT), and used for different types of restorations and situations. Low translucency blocks are indicated for full crowns where a staining or cut-back technique will be employed. The medium opacity blocks are used for fabricating frameworks for restoring devitalized or lightly discolored teeth. The MO serves as a framework and involves a more time-consuming layering technique and may not be indicated for a single-appointment procedure. The LT block, which is blue in color, is in a partial crystalline phase (biaxial strength of 130 MPa). At this level of strength the material has good edge stability and can be easily machined with a CAD/CAM system. The restoration can be milled to full contour and stained. Alternatively, a small amount of a cut-back technique can be used with a combination of additional layering and staining.
After milling, the restoration can be brought back to the patient to verify full seating and to adjust the bite. The color of the glasses is produced by polyvalent coloring ions, which exist in a different state of oxidation in the intermediate crystalline phase (blue state). Therefore, after milling, the fit and occlusion can be verified but not the color.
The blue full-contour restoration can either be cut back and layered with the appropriate porcelains or stain and glazed. It is then further crystallized in a porcelain oven where, according to the manufacturer, it reaches its final strength of 360 MPa at 850°C. At this point it can either be placed using adhesive, a combination of self-etching adhesive and resin cement, self-adhesive cement, or conventional cementing.
Tooth Preparation for IPS e.max CAD LT
The posterior and anterior tooth preparation requirements for this type of restorative material include a 360° shoulder with a rounded internal angle and should be 1 mm in depth. The lingual aspect of the preparation should be slightly deeper at 1.2 mm for anterior teeth and 1.5 mm for posterior teeth. Although the manufacturer suggests a minimum of 1.5 mm incisal/occlusal reduction, a 2-mm reduction will allow development of deeper, more natural occlusal anatomy in the posterior6 and more room in the anterior when using the cut-back technique.
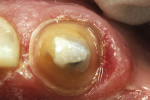
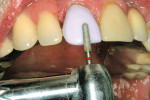
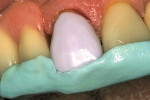
For anterior teeth, the dimension of the incisal edge should be at least 1 mm in thickness to allow the milling bur adequate room to prevent thin areas in the framework. In this case, because of the adaptation of the RPD framework, 2 mm of lingual reduction was provided (Figure 1 and Figure 2).
Virtual Impression
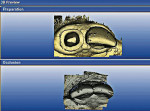
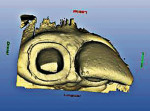
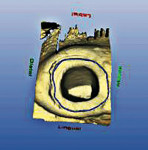
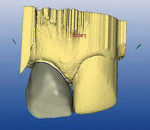
The CEREC program was set in the correlation mode which would allow for the duplication of the preoperative scanned image of the tooth. The cursor was placed in the occlusion box on the screen and a scanned image was saved. After completion of the preparation, the tooth was powdered and then scanned with the CEREC acquisition unit (Figure 3). The data-collection screen was comprised of two images; the preoperative image and the prepared tooth (Figure 4). The left central incisal was also included to facilitate the correlation of the pre-preparation model and the post-preparation model. The program was then advanced to trimming the model and marking the preparation margin (Figure 5 and Figure 6). The restoration was then proposed and final adjustments were made by the author using the tools in the CEREC program (Figure 7). After shade selection, the appropriate block was placed into the CEREC milling machine and milled (Figure 8).
Try-in
Before any laboratory modification or crystallization, the milled CAD LT crown should be thoroughly cleaned by either an ultrasonic bath and/or a steam cleaner. The coolant used during the milling process can leave a residue that can interfere with bonding or cause a discoloration during the crystallization process. After steam cleaning the crown, the remaining sprue was removed using a fine green stone.
There are four variations to the finishing process of the IPS CAD LT crown. There are three variations of the crystallization process and a cut-back technique. In the Variant A processing step, crystallization and glaze firing are performed as one step. If characterization is desired, then application of IPS e.max CAD Crystall./Shades and IPS e.max CAD Crystall./Stains are applied before the crystallization process. In the Variant B processing step, the IPS e.max CAD Crystall./Glaze Spray is used instead of the IPS e.max CAD Crystall./Glaze Paste. If characterization is desired, application of the IPS e.max CAD Crystall./Stains are applied first followed by the IPS e.max CAD Crystall./Glaze Spray. In the Variant C processing step, the IPS CAD restoration is crystallized first without any stains or glaze application. Subsequently, a separate Stain and Glaze firing cycle is used. In the cut-back technique, the blue CAD LT block is milled using the CAD software “reduce” function or is manually cut back before crystallization. After the crystallization step is completed, a wash coat of incisal porcelain is fired followed by addition of the incisal layering porcelain which is then fired subsequently.
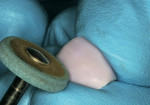
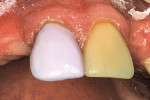
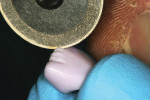
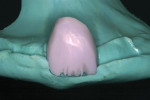
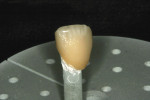
In this case, the crown was polished using CeramiPro™ Dialite wheels (Diamond Ceramic Polishers, Brasseler USA, Savannah, GA), starting with the blue reduction and contouring wheel, followed by the pink pre-polish wheel and finally achieving the final, high gloss with the gray, fine-grit polishing wheel (Figure 9 and Figure 10 ). The restoration was then tried in and evaluated for fit and correct occlusion (Figure 11). The RPD was then placed to confirm full seating. Because the restoration was a copy of the original damaged restoration, the fit of the RPD to the crown was satisfactory (Figure 12).
With the RPD still in place, a silicone index was made to record the incisal edge (Figure 13). In the laboratory, using a cut-back and layering technique without a working model, the clinician needs to know precisely the original incisal edge to prevent over/under layering of porcelain. The silicone index preserves the original incisal edge and provides a backdrop which simplifies the layering procedure.
Laboratory Modification
To create the mamelons, a red diamond-impregnated wheel (Perladia, Chicago, IL) was used (Figure 14). First, the incisal edge was shortened then the developmental grooves were cut. The mesial developmental groove was carried toward the gingival margin the furthest, followed by the mid-body groove and then the distal, which was the shortest. Supplemental grooves were then placed between the major developmental grooves using a double-sided diamond disk (Figure 15 ). The edges of the grooves were kept rounded. The crown was then placed back on the silicone index to evaluate the cut-back (Figure 16). The surrounding area of the cut-back was roughened with a green stone before the incisal porcelain wash coat application. Because cervical stain was to be applied, that area was also roughened.
All IPS e.max Ceram fluoroapatite veneering porcelains are compatible with the CAD LT block material. There are porcelains made specifically for the CAD LT material but they have a higher fusing temperature than the Ceram porcelains. Either type of layering porcelain may be used but they cannot be mixed because of the difference in firing temperatures. A thin incisal porcelain wash coat was first applied to the cut-back area and fired. Then, incisal porcelain was layered over the cutback area using the silicone index as a backdrop. At this point the crown can be fixed to a special firing pin which aids in handling the restoration during the application of the stains and glaze (if used).
The crystallization process involves placing the restoration on an IPS e.max CAD Crystallization Pin using IPS Object Fix Putty. There are several sizes of firing pins and the clinician should choose the pin that best fills the inside of the restoration without touching the internal walls of the crown. The inside of the crown is first filled with IPS Object Fix Putty and then the firing pin is inserted into the crown. The displaced putty is then smoothed with a porcelain or plastic spatula. The crown margins were fully supported with the putty. Excess putty beyond the crown margin was removed with a wet brush.
Once the crown was fixed to the firing peg, Khaki external stain was applied to the cervical area (Figure 17). Alternative finishing techniques bypass the finishing and polishing steps with the CeramiPro™ Dialite wheels (Brasseler USA). A spray-on glaze (IPS e.max CAD Crystall./Glaze Spray) or the IPS e.max CAD Crystall./Glaze Paste can be used to fill in the grounded crown surface. If so desired, then the Glaze Spray must be applied after the incisal layering porcelain and stains. The Glaze Spray is applied in two coats, letting the restoration dry between coats. If the IPS e.max CAD Crystall./Glaze Paste is used, it should be applied first followed by any desired stains.
The crown, secured to the firing peg, was placed on the firing tray (IPS e.max Crystallization Tray). The tray was then placed in the oven (Programat 300) and the two-stage, 21-minute crystallization program was started. From a scheduling aspect, the clinician can perform hygiene checks or short-appointment procedures during the crystallization process.
On completion of the crystallization cycle, the crown was removed from the oven and allowed to bench cool (Figure 18). The firing peg was removed. The IPS Fix Object Putty material was removed from the internal surface of the crown. Using a steam cleaner, the remaining parts of fixing putty material were removed. An ultrasonic cleaner can be used for this step if a steamer is not available. Sandblasting the internal surface is contraindicated because of the damage that can be caused to the lithium disilicate particles.
Cementation Alternatives
The beauty of the CAD LT material is that it can be inserted, as previously stated, using adhesive, self-etching adhesive, or conventional cementing. In this case, it was decided to use a self-etching adhesive with resin cement.
There is an advantage in using a resin-based luting material in that there is an increase in fracture resistance of the ceramic restoration.29,30 Tensile stresses can lead to the propagation of surface flaws resulting in fractures of ceramic materials.31 Salz reported indications that clinical fractures of full ceramic crowns were generally initiated at the internal surface.33 Axisymmetric finite element analysis34 and quantitative fractography35-37 have demonstrated that all-ceramic crown restorations fail from the extension of pre-existing defects resident on the internal surfaces of a restoration under tensile loading.38
Resin-based luting materials can heal surface defects that may reduce crack propagation.32 Load-to-failure in vitro mechanical testing has demonstrated that resin-cement coating increases the flexural strength of ceramic crowns.39,40
There are numerous self-adhesive materials available today that are made up of different components and, therefore, have different bonding strategies. However, a general rule of bonding adhesives is that the more steps involved, the better the bond.7,8 Having said that, with the more steps involved, the greater the technique sensitivity. Therefore, manufacturers have developed simpler, less technique-sensitive adhesive systems to prevent some of the common pitfalls with dental adhesives.
Self-etching adhesive cementing agents eliminate the conditioning, rinsing, and drying steps that are associated with multi-step adhesives. The exact execution of the multi-step adhesive procedures is difficult to standardize and can be critical to the durability of the bond.9 For example, using a self-etching dentin adhesive with resin cement eliminates the concern of a dehydration factor (overdrying) from dentin conditioning with resultant collapse of the collagen fiber network that is associated with the multistep adhesives. This collagen network collapse can result in incomplete resin infiltration leading to postoperative sensitivity.10
Self-etching adhesives can be subdivided by their acidity and the type of functional monomer. The level of acidity (pH) determines the aggressiveness of the self-etching component of the adhesive. Self-adhesives that have a pH of less than 1 are considered to be very aggressive and can produce resin tags and a hybrid layer 3 µm to 5 µm thick.9 As far as bond strength, the hybrid thickness and the presence of resin tags are not contributing factors.11 At this level of acidity, all hydroxyapatite crystals are dissolved within the hybrid layer.9 On the other hand, a self-etch adhesive with a pH greater than 2 is considered to be the least aggressive and produces a submicron hybrid layer with minimal dentin demineralization. With these types of adhesives, the hydroxyapatite crystals remain intact around the collagen fibers.7,12 There is also an intermediate category of self-etching adhesives that have a pH around 1.5 and share some of morphological changes seen in both acidic levels previously described but to a lesser extent.
Functional Monomers
Because mild or intermediate self-etch adhesives only partially demineralize the dentin, leaving hydroxyapatite crystals around the collagen fibrils, Yoshida et al13 examined the bonding potential of three functional monomers, which included: 10-methacryloxydecyl dihydrogen phosphate (10-MDP), 4-methacryloxyethyl trimellitic acid (4-MET), and 2-methacry-loxyethyl phenyl hydrogen phosphate (phenyl-P). Their study concluded that the 10-MDP monomer had the most stable bond of the three monomers. Stability was characterized by the hydrolytic strength of the calcium-monomer bond. They found that specific functional monomers have additional chemical bonding efficacy that is expected to contribute to their adhesive potential to tooth tissue.13 The basis of the bond durability can be evaluated on the hydrolytic stability of the functional monomer.9,14-16
The bond of the self-etching adhesives to enamel is definitely greater with aggressive adhesives (lower pH). In fact, strong self-etching adhesive systems (pH of 1 or lower) demonstrate an acid-etch pattern on enamel resembling that of a phosphoric acid treatment after a total-etch approach.24 Nevertheless, high, stable bond strengths have been achieved with mild or intermediate self-etching adhesives because of the ultra-structural interaction of the functional monomer (10-MDP) with dentin. Mild self-etching adhesive systems induce only a shallow partial demineralization no deeper than 1 µm in dentin.24 Hybridization of the microporous hydroxyapatite-coated collagen network obtains micromechanical interlocking. The thickness of the hybrid layer is much thinner than that with the strong self-etching adhesive systems or the total-etch approach but they have been proven to be as effective with regard to bond strength.22,25,26 In fact, in 2003 Van Meerbeek et al reported bond strengths of mild self-etch adhesives to dentin to be equivalent to three-step, etch-and-rinse adhesives.12 In 2008, Van Meerbeek stated that some mild self-etch adhesives do reach satisfactory bond strength. Additional chemical interaction between the monomers and residual hydroxyapatite must explain the satisfactory performance of the mild self-etch adhesives. He stated, however, that such interaction of self-etch adhesives with tooth substrate is dependent to a great extent on the kind of acidic functional monomer and eventually the overall composition of the adhesive.28 Perdigão reported drawbacks to some self-etch adhesives as a result of their disappointing resistance to thermal and mechanical stresses.21 DeMunck et al reported that when comparing the microtensile bond strength to dentin, only Optibond® FL (Kerr Corporation, Orange, CA) performed significantly better than the one-step, self-etch adhesives.22 This was also confirmed by Van Landuyt et al, where they found one-step adhesives bonding less effectively to enamel/dentin than did their multi-step versions. They accounted for this decrease in bond strength as a result of the entrapment of droplets within the adhesive layer, suggesting that the adhesive monomers separate from water upon evaporation of ethanol/acetone. They found that this could be avoided by strong air-drying of the adhesive, thereby removing interfacial water and thus improving the bonding effectiveness.23 Burrow et al, in their comparative study in determining the durability of tensile bond strengths of conventional three-step bonding systems and self-etching bonding systems, found that the use of a strong acid for demineralizing the dentin showed greater deterioration of the bond to dentin compared with the self-etching priming system.27
In this case, Futurabond DC and Bifix QM resin cement (VOCO America, Inc,) were used for insertion of the crown. At a pH of 1.4, Futurabond DC is a mild or intermediate self-etching adhesive that can be used with light-cure, dual-cure, and self-cure resin systems. The functional monomer in Futurabond is very similar to the 10-MDP monomer. The patented single-dose system prevents solvent evaporation, which can be a problem with one-bottle designs after multiple uses. According to the manufacturer, the self-etching adhesive contains SiO2 nanofillers (less than 20 µm) that improve the bond strength by reinforcement of the adhesive layer. This fortification is accomplished by the nanofillers that can easily penetrate the tubules, spaces in the collagen network, and the micro-retentive etching pattern on the enamel. This nanotechnology also allows for a more even and thinner hybrid layer of 9 µm.
Insertion
Before the restoration is inserted, the internal surface must be prepared no matter what type of cementation protocol will be used. Because the CAD LT is considered a high-strength glass-ceramic (more than double the 160 MPa flexural strength of IPS Empress) it is not mandatory to use adhesive cementation. Conventional cement can be used for final placement. But the manufacturer did find that it is necessary to condition the internal surface with IPS Ceramic Etching Gel (5% hydrofluoric acid) for 20 seconds to create a retentive pattern whether a bonding (composite resin) or cementing (resin-modified glass ionomer) procedure is used. Etching all-ceramic restorations is routine for clinicians when an adhesive bonding technique is employed. However, it is not a routine procedure to etch the internal surface when using resin-modified glass-ionomer cement. The manufacturer did find that there was no measurable bond of the resin-modified glass-ionomer to the lithium disilicate without a retentive pattern on the internal surface. Therefore, no matter what cementing procedure is used, it is necessary to condition the restoration before final placement.
Returning to the patient, the crown was tried in once again for shade confirmation. Upon the patient’s approval, the tooth was prepared for cementation. The intaglio surface of the CAD LT crown was then etched for 20 seconds with IPS Ceramic Etching Gel. The gel was rinsed and air-dried. Monobond-S (Ivoclar Vivadent, Amherst, NY), a silanizing agent, was applied for 1 minute and then air-dried.
Using the Futurabond DC single-dose delivery system, the dual-cure, self-etching adhesive was activated by pressing the package blister that mixes the two components together. The package was opened and the adhesive was applied in a continuous motion. The manufacturer recommends a 35-second application. The Futurabond DC is alcohol-based. Its predecessor, Futurabond NR, was acetone-based. There are studies that address the application time of Futurabond NR and should not be confused with the Futurabond DC dual-cure version. Erhardt et al found an increase in bond strength by doubling the application time.17 Toledano and his group tested the microtensile bond strength of Futurabond NR using five different parameters. These different bonding scenarios included: 1) following the manufacturer’s protocol; 2) using phosphoric acid-etch (36%) for 15 seconds; 3) treating with 10% sodium hypochlorite for 2 minutes after phosphoric acid-etching; 4) doubling the application time; and 5) doubling the number of application coats. They found that doubling the application time attained the highest microtensile bond strength to dentin and that all of the different scenarios did not affect the bond strength to enamel.18 These application times are pointed out so the clinician will not be confused with the self-etching adhesive (not the dual-cure, self-etching version) that was used in those studies.
In this case, the adhesive was applied for 35 seconds and air-dried for 5 seconds. This is a critical step that may be less stressful to clinicians. Van Landuyt et al19 found a lower bond strength with one-step adhesives that entrapped water droplets within the adhesive layer. Once polymerized, the droplets jeopardize the durability of the bond. They found that using strong air-drying of the adhesive would remove the water droplets and improve the bond effectiveness.19 Pooling of the adhesive in any line angles of the preparation has been shown to decrease bond strength because of excessive solvent confined within the adhesive layer.20 Therefore, the air-drying is a critical step and must not be taken lightly.
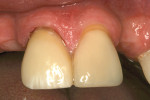
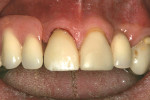
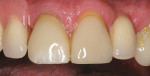
Once the adhesive application was completed, the cement was mixed and the restoration was seated. The RPD was then placed. The facial surface of the restoration was then light-polymerized. Gross removal of the excess cement was performed (Figure 19).The lingual surface was also light-polymerized after removal of the RPD. The remaining excess cement was then removed (Figure 20). The patient returned for a 6-month follow-up (Figure 21 and Figure 22).
Conclusion
Computer technology is finding new ways to become incorporated in dentistry. What was once a laborious procedure of retro-fitting a crown to an existing RPD can now be accomplished at a single appointment with the use of digital technology. Simplified laboratory procedures performed by the clinician can replace the tedious methods often used in a commercial laboratory setting. The patient benefits greatly because the restoration can be completed in a single appointment with excellent results.
Author's Note
All laboratory work was completed by the author. Special thanks to Ruth Egli for her editorial contribution.
References
1. Helvey GA. Retrofitting crowns to an existing removable partial denture clasp: a simple technique. J Prosthet Dent. 2002;87(4):399-402.
2. Marchack BW, Chen LB, Marchack CB, Futatsuki Y. Fabrication of an all-ceramic abutment crown under an existing removable partial denture using CAD/CAM technology. J Prosthet Dent. 2007;98(6):478-482.
3. Hansen CA, Russell MM. Making a crown fit accurately under an existing removable partial denture clasp assembly. J Prosthet Dent. 1994;71(2): 206-208.
4. Carracho JF, Razzoog ME. Removable partial denture abutments restored with all-ceramic surveyed crowns. Quintessence Int. 2006;37(4): 283-288.
5. Burns DR, Unger JW. The construction of crowns for removable partial denture abutment teeth. Quintessence Int. 1994;25(7):471-475.
6. McLaren EA, Hyo L, CAD/CAM update: Technologies and materials and clinical perspectives. Inside Dentistry. 2006;2(10):98-103.
7. Peumans M, Kanumilli PV, DeMunck J, et al. Clinical effectiveness of contemporary adhesives: a systematic review of current clinical trials. Dent Mater. 2005;21:18-25.
8. Shirai K, DeMunck J, Yosida Y, et al. Effect of cavity configuration and aging on the bonding effectiveness of six adhesives to dentin. Dent Mater. 2005;21: 110-124.
9. Van Meerbeek B. Mechanisms of resin adhesion: Dentin and enamel bonding. Functional Esthetics & Restorative Dentistry. 2008;2(1):18-25.
10. Magne P, Douglas WH. Porcelain veneers: Dentin bonding optimization and biomimetic recovery of the crown. Int J Prosthodont. 1999;12:111-121.
11. Yoshiyama M, Carvalho R, Sano H, et al. Interfacial morphology and strength of bonds made to superficial versus deep dentin. Am J Dent. 1995;8:297-302.
12. Van Meerbeek B, DeMunck J, Yosida Y, et al. Buonocore memorial lecture. Adhesion to enamel and dentin: current status and future challenges. Oper Dent. 2003;28:215-235.
13. Yoshida Y, Nagakane K, Fukuda R, et al. Comparative study on adhesive performance of functional monomers. J Dent Res. 2004;83(6):454-458.
14. Inoue S, Koshiro K, Yosida Y, et al. Hydrolytic stability of self-etch adhesives bonded to dentin. J Dent Res. 2005;84:1160-1164.
15. DeMunck J, Van Landuyt K, Peumans M, et al. A critical review of the durability of adhesion to tooth tissue: methods and results. J Dent Res. 2005;84:118-132.
16. Tay FR, Pashley DH. Have dentin adhesives become too hydrophilic? J Can Dent Assoc. 2003;69:726-731.
17. Erhardt MCG, Proenca JP, Osorio E, et al. Influence of application parameters on resin-dentin bonding of self-etch adhesives. The IADR/AADR/CADR 85th General Session and Exhibition. March 21-24, 2007.
18. Toledano M, Proenca JP, Erhardt MCG, et al. Increases in dentin-bond strength if doubling application time of an acetone-containing one-step adhesive. Oper Dent. 2007;32(2):133-137.
19. Van Landuyt KL, De Munck J, Snauwaert J, et al. Monomer-solvent phase separation in one-step self-etch adhesives. J Dent Res. 2005;84(2): 183-188.
20. Zheng L, Pereira PNR, Nakajima M, et al. Relationship between adhesive thickness and microtensile bond strength. Oper Dent. 2001;26:97-104.
21. Perdigão J. New developments in dental adhesion. Dent Clin North Am. 2007;51(2): 333-357.
22. DeMunck J, Van Meerbeek B, Satoshi I, Vargas M, et al. Microtensile bond strengths of one- and two-step self-etch adhesives to bur-cut enamel and dentin. Am J Dent. 2003;16(6):414-420.
23. Van Landuyt KL, DeMunck J, Snauwaert J, et al. Monomer-solvent phase separation in one-step self-etch adhesives. J Dent Res. 2005;84(2):183-188.
24. Türkün LE. The clinical performance of one- and two-step self-etching adhesive systems at one year. J Am Dent Assoc. 2005;136(5):656-664.
25. Perdigão J, May KN Jr, Wilder AD Jr, Lopes M. The effect of depth of dentin demineralization on bond strengths and morphology of the hybrid layer. Oper Dent. 2000;25:186-194.
26. Inoue S, Vargas MA, Abe Y, et al. Microtensile bond strength of eleven modern adhesives to dentin. J Adhes Dent. 2001;3:237-245.
27. Burrow MF, Harada N, Kitasako Y, et al. Seven-year dentin bond strengths of a total- and self-etch system. Eur J Oral Scien. 2005;113(3):265-270.
28. Van Meerbeek B. Mechanisms of resin adhesion: dentin and enamel bonding. Functional Esthetics & Restorative Dentistry. 2008;2(1): 18-25.
29. Malament KA, Socransky SS. Survival of Dicor glass-ceramic dental restoratives over 14 years: Part I. Survival of Dicor complete coverage restorations and effect of internal surface acid etching, tooth position, gender and age. J Prosthet Dent. 1999;81: 23-32.
30. Malament KA, Socransky SS. Survival of Dicor glass-ceramic dental restoratives over 14 years: Part II. Effect of thickness of Dicor material and design on tooth preparation. J Prosthet Dent. 1999;81:662-667.
31. Peterg V, de Vree J, Brekelmans WAM. Distributed crack analysis of ceramic inlays. J Dent Res. 1993;72(11):1537-1542.
32. Marquis PM. The influence of cements on the mechanical performance of dental ceramics. Bioceram. 1993;5:317-324.
33. Salz U. Adhesive cementation of full ceramic restorations. Ivoclar-Vivadent Report No 10. July 1994:9-20.
34. Anusavice KJ, Hojjatie B. Tensile stress in glass-ceramic crowns: effect of flaws and cement voids. Int Prosthodont. 1992;5:351-358.
35. Kelly JR. Clinically relevant approach to failure testing of all-ceramic restorations. J Prosthet Dent. 1999;81:652-661.
36. Kelly JR, Nishimura I, Campbell SD. Ceramics in dentistry: historical roots and current perspectives. J Prosthet Dent. 1996;75:18-32.
37. Quinn JB, Quinn GD, Kelly JR, Scherrer SS. Fractographic analysis of three ceramic whole crown restoration failures. Dent Mater. 2005;21:920-929.
38. Addison O, Marquis PM, Fleming GJP. Quantifying the strength of a resin-coated dental ceramic. J Dent Res. 2008;87(6):542-547.
39. Rosenstiel SF, Gupta PK, van der Sluys RA, Zimmerman MH. Strength of dental glass-ceramic after surface coating. Dent Mater. 1993;9:274-279.
40. Pagniano RP, Seghi RR, Rosenstiel SF, et al. The effect of a layer of resin luting agent on the biaxial flexure strength of two all-ceramic systems. J Prosthet Dent. 2005;93:459-466.
About the Author
Gregg A. Helvey, DDS, MAGD
Adjunct Associate Professor
Virginia Commonwealth University School of Dentistry
Richmond, Virginia
Private Practice
Middleburg, Virginia